- Pathophysiology-How Gliomas Develop
- Causes and Risk Factors of Glioma
- Classification and Grading
- Common Disorders Associated With Gliomas
- Less Common Disorders Associated With Gliomas
- Rare Disorders Associated With Gliomas
- Symptoms and Early Warning Signs
- Advanced Symptoms of Glioma
- Diagnostic Evaluation
- Modern Treatment Options, Side Effects, and Relapse
- Why Patients Seek Alternatives and Integrative Care
- Ayurvedic Perspective on Glioma
- Clinical Ayurvedic Treatment Principles in Glioma
- Herbs and Natural Interventions
- Ayurvedic Cure for Gliomas (Mastishka Arbuda)
- Brahmi Vachadi Avaleha- Advanced Ayurvedic Rasayana for Brain Tumor Recovery
- Critical Patient Safety Warning
- Why Market-Bought Avaleha Medicine Does Not Work
- Modern Scientific Research on Glioma and Integrative Support
- NCCIH, WHO, and ASCO Perspective on Integrative Care in Glioma
- Diet and Lifestyle for Glioma Recovery
- Prognosis and Quality of Life in Glioma
- When to Seek Medical Help Urgently
- Frequently Asked Questions
- Medical Review Policy
- References
This article is intended for educational purposes and does not replace professional medical diagnosis or emergency care. Gliomas require proper neurological evaluation using MRI, biopsy, and molecular testing. Ayurvedic treatment should be undertaken only under qualified medical supervision and, where required, alongside modern neuro-oncology care.
Understanding Gliomas and the Possibility of Healing
Gliomas are brain tumors that develop from glial cells, which support and protect nerve cells. They range from slow-growing low-grade gliomas to aggressive high-grade forms like glioblastoma. While conventional treatment focuses on surgery, radiation, and chemotherapy, long-term outcomes are often limited by recurrence and neurological side effects. Ayurveda approaches gliomas by correcting internal imbalances, strengthening brain tissue, and supporting the body’s natural healing intelligence [41].
Low-grade gliomas usually progress slowly and may remain stable for years, while high-grade gliomas, such as glioblastoma multiforme, are aggressive and demand immediate, multimodal treatment involving surgery, radiotherapy, and chemotherapy [122].
Global Perspective and Impact
Globally, gliomas account for about 30–35% of all primary brain tumors, with the highest incidence among adults aged 40–70 years [97]. Despite extensive advances in neurosurgery and targeted molecular therapies, survival outcomes remain variable. The five-year survival rate for LGG may exceed 70%, while HGG patients often face rates closer to 5–10% [84].
Beyond clinical data, gliomas profoundly affect emotional and family wellbeing, disrupting careers, relationships, and psychological balance [131]. However, timely diagnosis and a balanced integrative plan combining modern and Ayurvedic approaches can significantly improve both longevity and quality of life [56].
Debunking Myths and Restoring Confidence
One of the most harmful misconceptions is the belief that “a brain tumor is always a death sentence.” Both contemporary evidence and Ayurvedic medical tradition refute this myth.
Advances in molecular diagnostics, early surgical intervention, and Rasayana-based integrative therapy have enabled many patients to live long, productive lives [109].
Ayurveda complements oncology by enhancing neural recovery, reducing post-radiation fatigue, and strengthening mental resilience through the rejuvenation of Majja Dhatu (nervous tissue) and Ojas (vital energy) [68].
Ayurvedic Interpretation
In classical Ayurvedic literature, gliomas can be correlated with Mastishka Arbuda, a pathological condition described in Sushruta Samhita and Bhavaprakasha as a result of Vata–Kapha aggravation causing the vitiation of Majja Dhatu [21].
When Vata becomes disturbed, it disrupts cellular communication and bioelectrical balance, while excess Kapha promotes excessive tissue growth. This dual disturbance leads to Srotorodha (blockage of microchannels), resulting in the formation of an internal mass.
Conceptually, this aligns closely with the modern understanding of cellular dysregulation and glial proliferation, both models describing the transformation of normal glial cells into neoplastic ones under conditions of chronic stress and metabolic imbalance [77].
The Path of Regeneration and Hope
Unlike conventional therapies that primarily focus on tumor destruction, Ayurveda aims to regenerate and restore. The emphasis lies on strengthening Ojas, revitalizing Majja Dhatu, and harmonizing the disturbed Doshas through Rasayana therapy [114].
Herbs such as Ashwagandha (Withania somnifera), Guduchi (Tinospora cordifolia), and Brahmi (Bacopa monnieri) are known for their neuroprotective and adaptogenic properties, helping patients regain mental clarity and reduce neuroinflammation [92].
For patients and their families, this integrative path offers something rare in modern oncology — hope grounded in biology and compassion rooted in tradition.
It transforms the journey from a struggle for survival into one of healing, renewal, and inner balance [135].
Patients across the USA, UK, Europe, Canada, and Australia increasingly seek integrative approaches that focus not only on survival but also on cognitive function, emotional stability, and long-term quality of life.
Pathophysiology-How Gliomas Develop
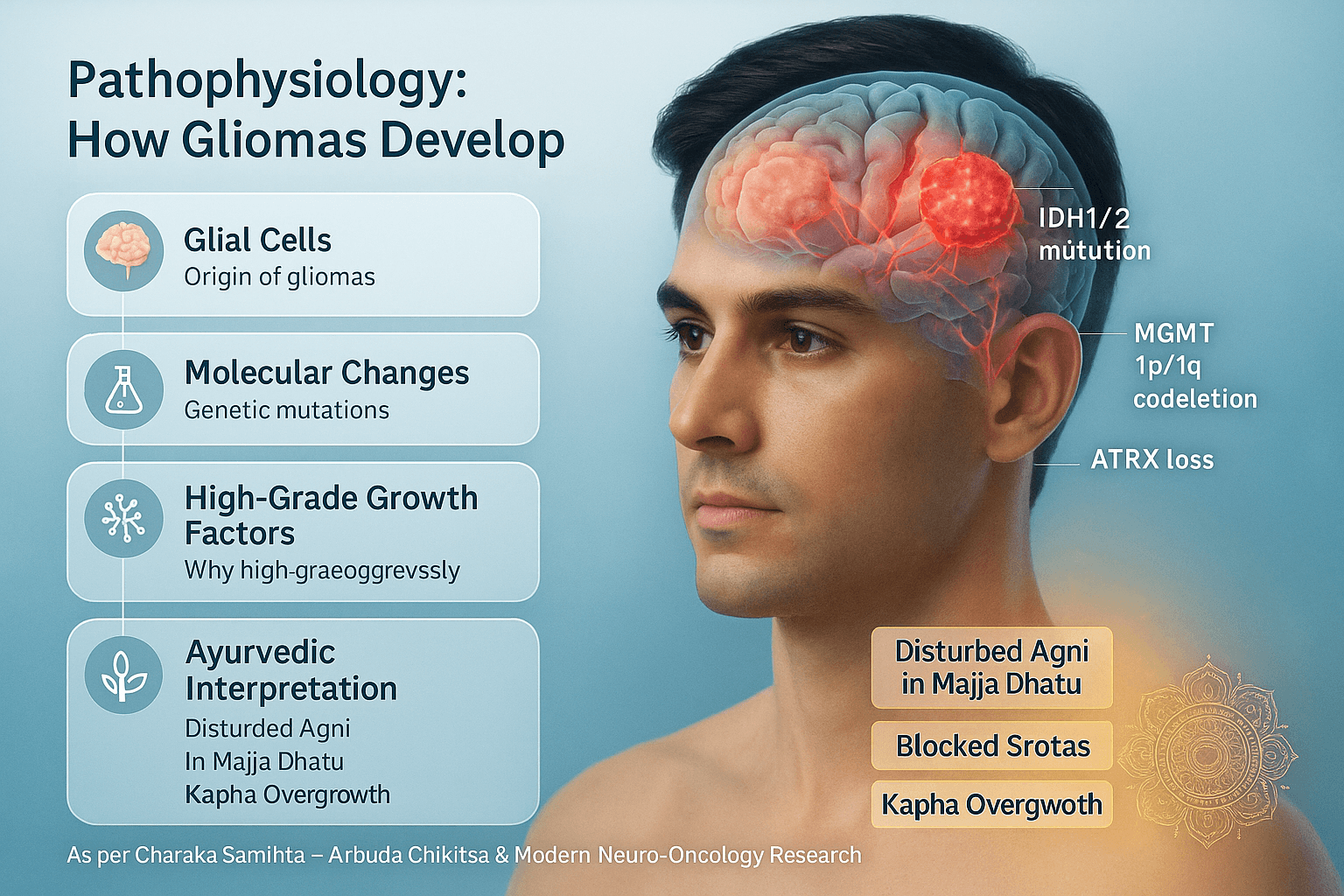
Gliomas originate from glial cells, the supporting framework of the brain that nourishes and protects neurons [113]. These include astrocytes, oligodendrocytes, and ependymal cells, each capable of transforming into a tumor under chronic stress, genetic instability, or inflammation [74].
When glial cells lose their regulatory balance, they begin to proliferate abnormally, forming masses that infiltrate surrounding brain tissue, disrupting electrical signaling, and increasing pressure within the skull [89].
Molecular and Genetic Foundations
Modern neuro-oncology identifies several key molecular alterations that drive glioma progression.
- IDH1/2 mutation: Found in most low-grade gliomas; it reprograms cell metabolism, slowing tumor growth and improving prognosis [91].
- MGMT methylation: A genetic modification that affects DNA repair, making certain tumors more responsive to chemotherapy [126].
- 1p/19q codeletion: Typical in oligodendrogliomas, this change correlates with longer survival [82].
- ATRX loss and TP53 mutations: Common in astrocytomas and glioblastomas, leading to impaired chromatin stability and faster cell proliferation [132].
These alterations shift normal glial metabolism toward a “Warburg-like” state, where cells rely heavily on glycolysis even in the presence of oxygen, an energy pattern also recognized in Ayurveda as Agni-vikriti, or deranged metabolic fire within Majja Dhatu [103].
Why High-Grade Gliomas Grow Aggressively
High-grade gliomas (HGG), such as glioblastoma, are distinguished by their rapid vascularization and invasion potential.
They stimulate angiogenesis, the formation of new blood vessels, through molecules like VEGF (vascular endothelial growth factor), ensuring a constant nutrient supply to the tumor [95].
At the same time, hypoxia (oxygen deprivation) triggers genetic pathways that make these tumors more resistant to treatment.
They also exhibit immune evasion, meaning the body’s immune cells fail to recognize and destroy them due to altered cytokine signaling [127].
This complex interplay explains why HGGs spread swiftly, recur frequently, and often resist standard therapies.
Ayurvedic Interpretation
From the Ayurvedic lens, gliomas arise due to a disturbance in Agni (metabolic fire) at the level of Majja Dhatu, the tissue responsible for neural integrity and cognition [67].
When Agni weakens, metabolic by-products (Ama) accumulate, causing Srotorodha (blockage of microscopic channels) and promoting Kapha overgrowth, which mirrors the unregulated proliferation of glial cells seen in modern pathology.
The imbalance of Vata further disrupts the transmission of neural impulses, resulting in symptoms like headaches, cognitive dullness, and fatigue.
This understanding provides a holistic framework where the physical, energetic, and metabolic disturbances leading to gliomas can be interpreted as manifestations of Vata–Kapha vitiation with Agni dysfunction [108].
A Simple Analogy for Patients
Imagine the brain like a finely tuned electrical system protected by insulation and nourished by a stable power source. Over time, due to stress, toxins, or poor metabolism, oxidative “rust” begins to accumulate, damaging circuits and weakening insulation.
In this weakened environment, a few abnormal cells start multiplying uncontrollably, forming a tumor. This process, where oxidative stress leads to cellular miscommunication and abnormal regeneration, is supported by both ancient Ayurvedic descriptions and modern biochemical studies [79].
Link Between Oxidative Stress and Inflammation
Recent research confirms that oxidative stress and chronic inflammation are central to glioma progression [125].
Free radicals (ROS) generated during metabolic imbalance damage DNA and mitochondria, leading to continuous glial activation and genomic instability.
Ayurveda’s emphasis on restoring Agni and clearing Ama parallels this modern finding—herbs like Guduchi, Curcumin, and Ashwagandha exhibit strong antioxidant and anti-inflammatory actions that directly counter these pathological changes [119].
Thus, both disciplines converge on the same truth: healing gliomas requires not only suppressing tumor growth but also restoring cellular harmony, metabolic balance, and immune clarity.
Causes and Risk Factors of Glioma
Genetic and Molecular Factors
When I sit with patients and explain glioma, one of the first things I clarify is that this disease often begins long before symptoms appear. At a microscopic level, changes in genes such as IDH, TP53, and EGFR alter how brain cells grow and repair themselves. You may feel frustrated trying to understand why this happened, especially when there is no clear trigger. In many cases, these mutations develop silently over time, without any visible warning.
From a clinical perspective, we understand that glioma is not simply caused by one factor. It is a complex biological process where normal control mechanisms fail. For the patient, this means that the focus should shift away from blame and toward understanding how to support the body moving forward.
Environmental and Radiation Exposure
In real clinical practice, one of the few well established risk factors we discuss is prior exposure to radiation, especially during childhood. Patients who have undergone radiation therapy to the head for other conditions carry a higher long term risk of developing glioma later in life.
At the same time, you may come across discussions about environmental toxins, mobile radiation, or occupational exposure. These are still being studied, and the evidence is not always conclusive. What this means for you is that glioma cannot always be prevented by simply avoiding certain exposures. This uncertainty is difficult, but it also reinforces the importance of early recognition and structured care.
Family History and Rare Genetic Conditions
In a small number of cases, glioma is linked to inherited conditions such as neurofibromatosis or Li Fraumeni syndrome. These conditions increase the likelihood of tumor development due to underlying genetic instability.
However, most patients sitting in front of me do not have any family history. This is why glioma often feels unexpected and unfair. It can affect individuals who have otherwise lived healthy and balanced lives.
Lifestyle and Internal Biological Environment
While lifestyle alone does not directly cause glioma, it influences the internal environment of the body. Chronic stress, poor sleep, metabolic imbalance, and long term inflammation can weaken the body’s ability to regulate abnormal cell growth.
You may not have caused the disease, but your current lifestyle can influence how your body responds to treatment and recovery. This is where a structured, integrative approach becomes meaningful.
Why Glioma Can Develop Without a Clear Cause
One of the hardest conversations we have with patients is explaining that sometimes there is no clear cause. Even after advanced testing, many cases remain unexplained.
This can feel unsettling, but it also helps redirect focus. Instead of searching endlessly for a cause, we work together on what can be controlled, which includes timely diagnosis, appropriate treatment, and long term recovery planning.
Classification and Grading

WHO 2021 Molecular Classification
Gliomas are classified according to the World Health Organization’s 2021 integrated molecular system, which divides them into four grades (I–IV) based on both histological and molecular features [117]. This classification helps physicians understand not only how the tumor appears under the microscope but also how it behaves biologically. The inclusion of molecular markers such as IDH mutation, 1p/19q codeletion, and ATRX loss has improved diagnostic precision and personalized care [68].
Grades I and II: Low-Grade Gliomas (LGG)
Grade I gliomas, such as pilocytic astrocytomas, are usually benign and slow-growing, often seen in children and young adults. Surgical removal can often lead to long-term remission and excellent prognosis [104].
Grade II gliomas, also referred to as low-grade gliomas (LGG), grow more slowly and may remain stable for several years before any progression occurs. These tumors often harbor IDH1/2 mutations or 1p/19q codeletions, genetic features that correspond with longer survival and better treatment response [83]. Many patients with low-grade gliomas maintain good cognitive and physical function for years, especially when their care plan includes integrative measures that strengthen brain tissue and immunity [94].
Grades III and IV: High-Grade Gliomas (HGG)
High-grade gliomas (HGG) encompass grades III and IV and are the most aggressive types of glial tumors. They grow rapidly, infiltrate surrounding brain tissue, and often recur despite intensive treatment [115]. These tumors usually lack IDH mutations and are instead characterized by genetic changes such as TP53, EGFR amplification, or ATRX loss, all of which accelerate tumor growth and resistance to therapy [132]. Management typically requires a multimodal strategy, including surgery, radiotherapy, and chemotherapy. Even with these advanced treatments, recurrence is common. Ayurvedic Rasayana therapy plays a complementary role by enhancing recovery, reducing treatment-related fatigue, and revitalizing cellular strength [101].
Table : Glioma Grades and What They Mean for Patients
| Glioma Grade | Growth Speed | Patient Experience | Treatment Approach | Real-Life Outlook |
|---|---|---|---|---|
| Low-Grade (Grade 1–2) | Slow | Mild symptoms, may be ignored early | Monitoring, surgery, selective therapy | Many patients continue work and daily life with adjustments |
| Intermediate | Moderate | Increasing neurological symptoms | Combined treatment approach | Requires closer monitoring and structured care |
| High-Grade (Grade 3–4) | Fast | Rapid symptom progression | Surgery + radiation + chemotherapy | Focus shifts to control, stability, and quality of life |
| Glioblastoma (Grade 4) | Very aggressive | Severe symptoms, fast changes | Intensive multimodal treatment | Requires continuous care and strong support system |
Ayurvedic Correlation: Granthi and Arbuda
Ayurveda describes two categories of pathological growths that closely parallel modern glioma types. Granthi refers to a benign, slow-growing swelling caused by mild Kapha–Vata imbalance, which aligns with the characteristics of low-grade gliomas. Arbuda, however, describes a deep-seated, rapidly spreading mass resulting from aggravated Vata–Kapha doshas and Srotorodha, or blockage of the microchannels [120].
Granthi-type lesions can often remain contained through proper metabolic balance, nutrition, and lifestyle regulation. Arbuda-type conditions, in contrast, require detoxification (Shodhana) and restorative therapy (Rasayana) to restore systemic harmony and inhibit further proliferation [73].
Biological Parallels and Modern Interpretation
The Ayurvedic description of tumor formation shows striking similarities to modern concepts of cancer biology. The Kapha component nourishes excessive growth, while Vata promotes uncontrolled cellular division, closely resembling modern observations of angiogenesis, metabolic reprogramming, and immune escape in gliomas [101]. Both disciplines recognize that malignant transformation occurs when internal homeostasis is disrupted—when the metabolic fire (Agni) weakens, toxins (Ama) accumulate, and the body’s vital energy (Ojas) becomes depleted.
Patient Outlook and Integrative Care
Despite the challenges of glioma management, many patients with low-grade tumors live fulfilling lives for a decade or longer with appropriate medical and Ayurvedic interventions [129]. An integrative approach that combines modern neuro-oncology with Rasayana therapy helps delay disease progression, protect cognitive functions, and improve overall wellbeing. By maintaining a clear metabolic state (Agni), preventing toxic buildup (Ama), and strengthening Ojas, patients can achieve not only extended survival but also improved mental and emotional stability [108].
This integrated framework reflects a broader truth: the management of gliomas is not merely about removing disease, but about reestablishing balance between the body’s cellular intelligence and its inner vitality.
Common Disorders Associated With Gliomas
Seizure Disorders
Seizure disorders remain the most frequent neurological condition linked with gliomas. In my clinical experience, many patients first encounter the healthcare system after a sudden seizure episode. These seizures arise when abnormal glial growth interferes with normal electrical signaling pathways of the brain.
If you are living with glioma, seizures may be subtle or dramatic. Some patients experience brief episodes of altered awareness or limb jerking, while others have full loss of consciousness. Even after tumor removal, seizures may persist because surrounding brain tissue remains electrically unstable.
From a medical standpoint, uncontrolled seizures increase injury risk, restrict independence, and contribute to long term anxiety. Early diagnosis and consistent neurological follow up are essential for safety and quality of life.
Chronic Headache and Raised Intracranial Pressure Syndrome
Persistent headache is another widely reported disorder associated with gliomas. Unlike ordinary headaches, these often worsen progressively, intensify in the early morning, and may be accompanied by vomiting or visual blurring.
Patients often tell me that the pain feels deep, heavy, or pressure like rather than sharp. This occurs due to increased intracranial pressure caused by tumor mass or surrounding inflammation. If you notice headaches that steadily worsen or change character, this should prompt immediate evaluation.
Clinically, rising intracranial pressure is a warning sign that requires timely intervention. Left unaddressed, it can impair vision, consciousness, and brainstem function.
Cognitive Dysfunction and Mental Processing Disorder
Cognitive dysfunction is extremely common but frequently overlooked. Many patients experience difficulty concentrating, slowed thinking, impaired memory, or reduced problem solving ability. I often hear patients say they feel mentally foggy or disconnected from their usual sharpness.
If you experience this, it is important to understand that cognitive decline is not psychological weakness. It reflects direct involvement of neural networks or secondary effects of treatment. These changes may develop gradually and affect work performance, financial decisions, and daily independence.
From a clinical perspective, early cognitive assessment allows timely rehabilitation and supportive strategies that preserve dignity and autonomy.
Personality and Behavioral Changes
Personality changes are common, particularly when gliomas involve frontal or temporal brain regions. Family members often notice these changes before the patient does. Reduced emotional control, impulsivity, apathy, or inappropriate social behavior may emerge.
You may feel unlike yourself, reacting differently to stress or relationships. This can strain family bonds and lead to misunderstanding if not properly explained. These changes are neurological in origin, not character flaws.
From a therapeutic standpoint, recognizing behavioral change as a disease related condition improves communication, reduces blame, and enhances emotional support planning.
Motor Weakness and Functional Impairment
Motor weakness frequently accompanies gliomas affecting motor pathways. Patients may develop gradual loss of strength, poor coordination, or difficulty performing fine movements such as writing or buttoning clothes.
If you notice weakness on one side of the body or frequent falls, this should never be dismissed as fatigue or aging. These symptoms often reflect direct tumor pressure or disruption of motor signaling.
Clinically, early physiotherapy and functional training significantly improve mobility and independence when started promptly.
Speech and Language Disorders
Speech and language disorders are common in tumors affecting the dominant cerebral hemisphere. Patients may struggle to find words, construct sentences, or understand spoken language.
You may feel frustrated when thoughts remain clear but expression becomes difficult. This disconnect often causes emotional distress and social withdrawal.
From a neurological perspective, speech therapy initiated early improves outcomes and helps preserve communication ability even when structural damage exists.
Visual Processing Disorders
Visual disturbances occur when gliomas involve optic pathways or visual processing centers. Patients may experience blurred vision, loss of peripheral vision, difficulty reading, or problems recognizing objects.
These symptoms may develop slowly and go unnoticed until daily activities become challenging. If you experience changes in vision, timely evaluation can prevent permanent deficits.
Clinically, visual assessment is essential for safety, driving decisions, and occupational planning.
Fatigue and Cancer Related Exhaustion
Severe fatigue is one of the most disabling disorders associated with gliomas. Unlike ordinary tiredness, this exhaustion does not improve with rest and affects both physical and mental endurance.
Patients often tell me they feel drained even after minimal activity. This fatigue results from tumor metabolism, inflammation, and treatment burden.
From a care perspective, addressing fatigue improves treatment tolerance, emotional resilience, and daily functioning.
Sleep Disorders and Circadian Rhythm Disruption
Sleep disturbances are extremely common but underrecognized. Insomnia, fragmented sleep, excessive daytime sleepiness, or reversed sleep cycles may occur.
If your sleep pattern has changed significantly, this can worsen cognitive function, mood, and immune response. Sleep disruption also intensifies fatigue and emotional instability.
Clinically, restoring sleep rhythm plays a crucial role in recovery and neurological stability.
Mood Disorders and Emotional Dysregulation
Depression and anxiety frequently coexist with gliomas. These are not merely emotional reactions but are often driven by neurochemical changes within the brain.
You may experience persistent sadness, fear, or emotional numbness even when circumstances seem stable. These feelings deserve medical attention, not dismissal.
From a treatment standpoint, emotional health directly affects survival quality, adherence to therapy, and overall wellbeing.
Autonomic Nervous System Dysfunction
Autonomic dysfunction is more common than widely recognized. Symptoms may include heart rate irregularity, blood pressure fluctuations, abnormal sweating, digestive disturbance, or temperature intolerance.
Patients often struggle to explain these symptoms because they appear unrelated to the brain. However, they reflect disruption of central autonomic regulation.
Clinically, identifying autonomic involvement prevents misdiagnosis and improves symptom management.
Hormonal and Metabolic Disturbances
Gliomas involving hypothalamic or pituitary regions may cause hormonal imbalance. Weight changes, appetite disruption, temperature dysregulation, and fatigue may occur.
You may feel that your body no longer responds normally to food, stress, or sleep. These symptoms are often misunderstood unless specifically evaluated.
From a medical standpoint, hormonal screening is essential for comprehensive care.
Neuropsychiatric Syndromes
In some patients, gliomas present with hallucinations, paranoia, emotional detachment, or profound behavioral change. These symptoms are sometimes misdiagnosed as primary psychiatric illness.
If psychological symptoms appear suddenly or worsen rapidly, neurological causes must be considered.
Clinically, recognizing neuropsychiatric syndromes prevents inappropriate treatment and delayed tumor diagnosis.
Progressive Neurocognitive Decline
In advanced or recurrent cases, patients may develop progressive neurocognitive decline resembling dementia. Memory loss, confusion, and loss of independence may occur.
This progression is deeply distressing for patients and caregivers. Early supportive planning and symptom control are crucial.
From a care perspective, preserving dignity and comfort becomes as important as disease control.
Less Common Disorders Associated With Gliomas
Speech and Language Processing Disorders
Speech and language disturbances occur less commonly than seizures or headaches but carry a profound impact on daily life. In my clinical observations, these disorders often appear gradually, making them easy to miss in early stages. Patients may struggle to find words, form coherent sentences, or follow complex conversations.
If you are experiencing difficulty expressing thoughts despite knowing what you want to say, this can be deeply frustrating. Some patients describe it as words disappearing mid sentence. Others notice that understanding spoken language requires extra effort, especially in noisy environments.
From a neurological perspective, these disorders arise when gliomas affect language centers of the brain. Early speech therapy and cognitive support can significantly preserve communication ability and reduce social withdrawal.
Fine Motor Skill and Coordination Disorders
Fine motor dysfunction is another less common but clinically significant disorder. Patients may notice difficulty writing, typing, using utensils, or performing precise hand movements. I often see patients dismiss these changes as fatigue or stress.
If you notice increasing clumsiness or loss of precision, it is important not to ignore it. These subtle changes may reflect early disruption of motor planning areas rather than simple weakness.
Clinically, early intervention with occupational therapy improves functional independence and prevents long term disability.
Balance and Gait Disorders
Balance disturbances and gait instability are less frequently reported but highly impactful. Patients may feel unsteady while walking, experience frequent tripping, or develop a sense of spatial disorientation.
You might feel as though the ground is unreliable beneath your feet, even when strength seems intact. This creates fear of falling and limits mobility.
From a clinical standpoint, these disorders often indicate involvement of coordination pathways. Early physiotherapy and balance training reduce fall risk and restore confidence.
Visual Perception and Spatial Awareness Disorders
Visual perception disorders differ from simple vision loss. Patients may see clearly yet struggle to judge distances, recognize faces, or interpret visual information accurately.
If you feel disoriented in familiar spaces or misjudge object placement, this may not be an eye problem. These symptoms originate in visual processing centers of the brain.
Clinically, visual cognitive testing helps distinguish perception disorders from ocular disease and guides rehabilitation planning.
Auditory Processing Disorders
Some patients develop difficulty processing sounds despite normal hearing ability. Speech may sound distorted or difficult to understand, especially in group settings.
You may find conversations exhausting or confusing, even when hearing tests appear normal. This leads many patients to withdraw socially.
From a neurological view, these disorders arise when auditory processing regions are affected. Early recognition improves coping strategies and communication outcomes.
Emotional Regulation Disorders
Emotional dysregulation is less common than depression but deeply disruptive. Patients may experience sudden emotional shifts, inappropriate laughter or crying, or reduced emotional responsiveness.
You might feel emotionally disconnected or overwhelmed without clear triggers. These changes are neurological, not personality flaws.
Clinically, recognizing emotional regulation disorders prevents mislabeling and improves psychological support planning.
Executive Function Disorders
Executive dysfunction affects planning, decision making, and task organization. Patients may struggle to manage finances, schedules, or multi step activities.
If you feel mentally overwhelmed by tasks that once felt simple, this is not laziness or loss of intelligence. It reflects disruption of higher cognitive control networks.
From a care perspective, structured routines and cognitive rehabilitation help preserve independence.
Sensory Integration Disorders
Some patients experience altered sensation such as numbness, tingling, or abnormal body perception. These symptoms may shift locations and confuse both patients and clinicians.
You may feel disconnected from parts of your body or experience sensations that are difficult to describe. These are real neurological phenomena.
Clinically, sensory integration issues often indicate cortical involvement and require careful neurological monitoring.
Autonomic Regulation Changes
Less commonly, patients develop changes in autonomic regulation affecting digestion, heart rate, or temperature control. These symptoms are often overlooked because they seem unrelated to the brain.
If you experience unexplained digestive irregularities, sweating changes, or temperature intolerance, neurological involvement should be considered.
From a medical standpoint, identifying autonomic changes prevents misdiagnosis and improves holistic symptom management.
Subtle Personality Shifts Recognized Only by Others
In some cases, personality changes are noticed only by family members. Patients themselves may feel unchanged while loved ones observe reduced empathy, altered priorities, or diminished social awareness.
This disconnect can strain relationships if not explained medically. These shifts are neurological in origin and require compassionate communication.
Clinically, family involvement is crucial for early detection and supportive care planning.
Why Less Common Disorders Matter
Although less common, these disorders significantly affect quality of life, independence, and relationships. They are often reversible or manageable when identified early.
From a treatment standpoint, recognizing these conditions allows timely intervention and prevents unnecessary decline.
Rare Disorders Associated With Gliomas
Endocrine and Hormonal Regulation Disorders
Endocrine disturbances are rare but clinically serious disorders associated with gliomas, especially when tumors involve deep brain structures responsible for hormonal control. In my clinical experience, these disorders are often missed because symptoms appear unrelated to the brain.
You may notice unexplained weight changes, altered appetite, temperature intolerance, or persistent fatigue despite adequate rest. Some patients experience changes in thirst, urination, or sleep patterns that gradually worsen over time.
From a medical perspective, these symptoms arise due to disrupted communication between the brain and hormone producing glands. Early recognition is essential because untreated hormonal imbalance can worsen neurological recovery and overall health.
Autonomic Nervous System Failure Syndromes
Autonomic dysfunction represents a rare but impactful consequence of gliomas. Patients may develop irregular heart rate, unstable blood pressure, abnormal sweating, digestive slowdown, or difficulty regulating body temperature.
You might feel that your body no longer responds predictably to stress or physical activity. Simple actions such as standing up or eating a meal may trigger dizziness or discomfort.
Clinically, autonomic involvement indicates deeper neurological disruption. Identifying this condition prevents misdiagnosis and helps guide safer daily activity planning.
Severe Neuropsychiatric Syndromes
In rare cases, gliomas present primarily with psychiatric symptoms rather than neurological ones. Patients may develop hallucinations, paranoia, emotional detachment, or sudden personality transformation.
You may feel misunderstood when symptoms are labeled psychological without neurological evaluation. Some patients are initially treated for psychiatric illness before the true cause is discovered.
From a clinical standpoint, recognizing neuropsychiatric syndromes as brain based disorders is critical to prevent delayed diagnosis and inappropriate treatment.
Progressive Cognitive Decline Resembling Dementia
A small subset of patients develop progressive cognitive decline that resembles dementia. Memory loss, confusion, impaired judgment, and loss of daily functioning may evolve gradually.
If you or your family notice a steady decline rather than sudden change, this pattern should raise concern. Patients often feel frightened by the loss of independence and identity.
From a care perspective, early planning, cognitive support, and caregiver education are essential to preserve dignity and safety.
Disorders of Consciousness and Awareness
Rarely, gliomas interfere with brain networks responsible for consciousness and awareness. Patients may experience episodes of confusion, reduced alertness, or fluctuating awareness without clear triggers.
You may feel disconnected from your surroundings or struggle to remain mentally present. These episodes are often alarming to both patients and caregivers.
Clinically, such symptoms indicate serious neurological involvement and require urgent assessment and monitoring.
Central Pain Syndromes
Some patients develop central pain syndromes in which pain arises from altered brain processing rather than tissue injury. This pain may feel burning, aching, or electric and does not respond well to standard pain medication.
You may feel pain without visible cause, leading to frustration and emotional distress. These sensations are real and neurologically driven.
From a treatment standpoint, central pain requires specialized management strategies and compassionate validation.
Swallowing and Feeding Disorders
Rarely, gliomas affect brain centers responsible for swallowing coordination. Patients may experience choking, difficulty swallowing, or fear of eating.
If you notice frequent coughing while eating or unexplained weight loss, this should never be ignored. Swallowing disorders increase the risk of aspiration and nutritional deficiency.
Clinically, early intervention with swallowing assessment and dietary modification prevents serious complications.
Sexual Function and Libido Changes
Altered sexual function is a rare but deeply personal disorder associated with gliomas. Patients may experience reduced libido, altered arousal, or changes in emotional intimacy.
You may feel confused or distressed by these changes, especially if they occur suddenly. These symptoms are neurological and hormonal in origin rather than relational failure.
From a medical perspective, addressing sexual health improves emotional wellbeing and relationship stability.
Severe Emotional Flattening and Loss of Motivation
In rare cases, patients develop profound emotional flattening marked by loss of motivation, reduced pleasure, and minimal emotional response.
You may feel alive but disconnected from joy, ambition, or purpose. Family members often notice withdrawal before the patient does.
Clinically, this condition reflects disruption of motivational circuits and requires careful psychological and neurological support.
Why Rare Disorders Matter
Although rare, these disorders profoundly affect safety, identity, and quality of life. They are often overlooked because they do not resemble classic tumor symptoms.
From a therapeutic standpoint, early recognition allows timely intervention, protects dignity, and prevents avoidable suffering.
Symptoms and Early Warning Signs

Common Symptoms of Gliomas
Gliomas often begin silently, growing unnoticed until they start affecting brain function. The most common symptoms include headache, seizures, speech or vision disturbances, and personality or behavioral changes [112]. Headaches typically worsen in the morning or during coughing or straining, due to increased intracranial pressure [126]. Seizures may appear suddenly, even in people without a prior neurological history, and are often the first clue in low-grade gliomas [87]. Tumors affecting the frontal or temporal lobes can cause mood instability, confusion, or reduced ability to plan and organize daily tasks [105]. Speech impairment, blurred vision, or partial weakness in limbs are also frequent early manifestations, depending on tumor location [89].
Subtle and Early Signs Often Overlooked
In many patients, the initial signs are vague and can mimic stress, sleep deprivation, or depression. Subtle early symptoms include chronic fatigue, poor short-term memory, difficulty concentrating, dizziness, and emotional fluctuations [91]. Some patients report an unusual loss of balance, a sense of detachment, or unexplained nausea [133]. Early sensory changes such as partial hearing loss, facial tingling, or mild coordination problems may also develop when gliomas affect the sensory or motor cortex [122]. Even minor forgetfulness or personality softening, when progressive, may indicate a deeper neurological cause rather than simple anxiety or aging [139].
Rare or Unusual Presentations
Although uncommon, some gliomas present with symptoms that mimic psychiatric or metabolic disorders. A few patients develop visual hallucinations, olfactory auras (perceiving smells that do not exist), or sudden bursts of laughter or crying due to involvement of the limbic and temporal regions [130]. Rarely, brainstem gliomas cause difficulty swallowing, double vision, slurred speech, or sleep disturbances resulting from cranial nerve compression [123]. In posterior fossa or cerebellar tumors, symptoms may include vomiting without nausea, clumsiness, or unsteady gait. In extreme cases, sudden loss of consciousness, hormonal changes, or rapid decline in alertness may occur if the tumor invades the hypothalamus or brainstem [141]. These rare presentations highlight the complexity of gliomas and the need for early neuroimaging when neurological or behavioral symptoms appear atypical.
Ayurvedic Mapping of Neurological Symptoms
In Ayurveda, these diverse neurological symptoms are understood through the lens of Vata and Kapha imbalance affecting Majja Dhatu, the tissue responsible for cognition, coordination, and perception. The common and subtle signs of gliomas correspond to conditions such as Shiro Shoola (headache), Moorchha (episodes of fainting), Tandra (drowsiness or lethargy), Bhrama (giddiness), and Smriti Bhramsha (loss of memory) [63].
When Vata becomes excessive, it disturbs nerve conduction, causing seizures, imbalance, and insomnia. Kapha aggravation leads to heaviness, drowsiness, and obstructed mental clarity. The simultaneous aggravation of both doshas leads to Srotorodha (blockage of brain channels), initiating pathological growth within Majja Dhatu [97].
Ayurvedic physicians emphasize early recognition of these doshic imbalances, even before structural changes appear. A dull headache, poor sleep, irritability, or loss of enthusiasm are viewed as early Vata–Kapha vitiations, warning that Agni (metabolic fire) is disturbed and needs correction through diet, lifestyle, and purification measures [109].
Managing Anxiety and Emotional Distress
The period following a glioma diagnosis often brings overwhelming anxiety, fear of mortality, and emotional withdrawal. Ayurveda offers Sattvavajaya Chikitsa, a form of mental-strengthening therapy aimed at stabilizing thought, emotion, and perception [81]. This therapy involves meditation, counseling, self-awareness practices, and positive cognitive training to regulate Manovaha Srotas (mental channels). It reduces the overactivation of Vata, helping to calm nervous excitability and restore inner balance.
Herbal Rasayanas such as Brahmi (Bacopa monnieri), Shankhapushpi (Convolvulus pluricaulis), and Jatamansi (Nardostachys jatamansi) are used to enhance focus, memory, and emotional stability [128]. These herbs act as adaptogens, improving resilience during chemotherapy and radiotherapy while lowering stress hormones. Modern integrative care often combines Sattvavajaya Chikitsa with psychotherapy or guided support groups to improve both compliance and emotional wellbeing [103].
Patient Guidance and Early Intervention
Persistent or unusual headaches, unexplained neurological symptoms, or personality changes should never be ignored. A simple MRI or CT scan performed at the right stage can detect even small gliomas, leading to earlier intervention and better prognosis [99]. From the Ayurvedic viewpoint, early correction of Vata–Kapha imbalance through Rasayana therapy, regulated sleep, and avoidance of excessive stress or fasting can prevent the pathological transformation of Majja Dhatu [106].
Early recognition, supported by patient awareness and integrative medical evaluation, not only increases survival but also preserves mental clarity and emotional harmony. Both Ayurveda and modern medicine emphasize that the journey to recovery begins with understanding the body’s signals, listening to what the brain expresses through even the faintest change.
Advanced Symptoms of Glioma
Progressive Neurological Decline
In real clinical conversations, this is often the turning point where a patient begins to feel that something is seriously wrong. Initially, you may notice subtle weakness in one hand, a slight imbalance while walking, or difficulty performing routine movements. These changes are often brushed aside as fatigue, vitamin deficiency, or stress.
However, as the tumor progresses, these symptoms become more defined. The body starts losing coordination, and movements that once felt automatic now require effort and concentration. From a physician’s perspective, this stage signals that the tumor is affecting functional brain pathways. From your perspective, it feels like your body is no longer responding the way it used to.
What makes this phase clinically important is not just the symptom itself, but the pattern. Gradual worsening, asymmetry in strength, or repeated episodes of imbalance should never be ignored. This is where early intervention can still influence outcomes.
Table 2: Early vs Advanced Symptoms of Glioma
| Stage | Symptoms | What Patients Usually Think | Clinical Reality |
|---|---|---|---|
| Early Stage | Mild headaches, fatigue, subtle memory issues | Stress, lack of sleep | Early neurological involvement |
| Functional Change | Difficulty focusing, slight coordination issues | Overwork or aging | Brain signaling disruption |
| Progressive Stage | Weakness, speech issues, vision problems | Temporary issue | Tumor affecting key brain areas |
| Advanced Stage | Seizures, severe headache, vomiting, confusion | Emergency situation | Requires urgent intervention |
Cognitive and Memory Impairment
One of the most distressing aspects of advanced glioma is the change in thinking ability. Patients often describe it in simple words. Something feels off. You may forget recent conversations, lose track of tasks, or struggle to focus on things that were once effortless.
What is important to understand is that these changes are not always dramatic in the beginning. They are subtle, progressive, and often noticed first by family members. A loved one may say that you are repeating questions, becoming less attentive, or reacting differently to situations.
From a clinical standpoint, this reflects involvement of higher brain centers responsible for memory, attention, and executive function. From a human standpoint, it affects identity. You are not just dealing with a disease. You are dealing with a shift in how you think, respond, and interact with the world.
This is why timely recognition matters. The earlier these changes are addressed, the better the chances of preserving function and quality of life.
Speech and Communication Difficulties
Communication is deeply personal, and when it is affected, the impact is immediate and emotional. Patients may begin to struggle with word finding, sentence formation, or understanding spoken language. You might know what you want to say, but the words do not come out the way you expect.
This creates frustration, not only for you but also for those around you. Conversations become slower, interactions become limited, and over time, social withdrawal can occur.
Clinically, this indicates involvement of language centers in the brain. But beyond the clinical explanation, the real concern is the loss of expression. When communication is affected, patients often feel isolated even when surrounded by family.
Recognizing these changes early allows for supportive interventions, including therapy and communication strategies that help maintain connection and dignity.
Vision and Sensory Changes
Vision changes in glioma are often underestimated. You may notice blurred vision, difficulty focusing, or missing parts of your visual field. Some patients describe bumping into objects or struggling to judge distance.
In other cases, sensory changes appear. Numbness, tingling, or altered sensation in parts of the body may develop depending on the tumor location.
From a medical perspective, these symptoms reflect involvement of visual pathways or sensory processing areas. From your daily life perspective, they affect safety, mobility, and confidence.
These are not random symptoms. They are signals. When vision or sensation begins to change progressively, it is an indication that the disease is affecting broader neural networks.
Increased Intracranial Pressure
As glioma grows, one of the most critical developments is the rise in intracranial pressure. This is not always visible, but the symptoms are very clear. Headaches become more persistent, often worse in the morning. Nausea and vomiting may occur without any digestive cause. There may also be a feeling of heaviness or pressure inside the head.
When I evaluate patients with these symptoms, it immediately raises concern. This stage requires urgent attention because increased pressure can affect vital brain functions.
For you, this may feel like a worsening headache that does not respond to usual medication. It is important to understand that this is not a routine symptom. It is a warning sign that the brain is under stress.
Ignoring this stage can delay critical interventions. Acting early can prevent further complications.
Seizures and Loss of Control
Seizures are often one of the most alarming symptoms for both patients and families. They may occur suddenly, sometimes without warning, and can range from brief episodes of confusion to full body convulsions.
For the patient, this experience can be frightening and disorienting. For the family, it creates a constant sense of uncertainty. Will it happen again. When will it happen. How severe will it be.
Clinically, seizures indicate abnormal electrical activity in the brain caused by tumor irritation. Managing them becomes essential, not only to control symptoms but also to ensure safety in daily life.
From a broader perspective, seizures often become a key part of long term management. With proper care, they can be controlled, but they require attention, consistency, and medical supervision.
What This Means for You as a Patient
At this stage, the goal is not just identifying symptoms. It is understanding patterns, acting early, and maintaining function for as long as possible.
You are not expected to diagnose yourself. But you are expected to notice changes, communicate them clearly, and seek timely care.
From a clinical standpoint, these symptoms define progression. From your standpoint, they define experience. Bridging that gap is where structured, integrative care becomes meaningful.
Diagnostic Evaluation
Modern Imaging Techniques
The diagnosis of gliomas relies on advanced imaging tools that assess both structural and functional aspects of the brain. Magnetic Resonance Imaging (MRI) is the most widely used modality, offering high-resolution visualization of tumor margins, infiltration, and mass effect [91]. Contrast-enhanced MRI helps identify disruption of the blood–brain barrier, which is typical in higher-grade gliomas [117]. Functional MRI (fMRI) and diffusion tensor imaging (DTI) can further map critical brain pathways before surgery, ensuring safer resection [112].
Positron Emission Tomography (PET) complements MRI by showing metabolic activity, distinguishing active tumor tissue from necrosis or post-treatment changes [114]. Magnetic Resonance Spectroscopy (MRS) analyzes tissue biochemistry, identifying elevated choline, reduced N-acetylaspartate, and lactate peaks—metabolic markers that indicate tumor proliferation [128]. These combined modalities help define the exact location, biological activity, and aggressiveness of the lesion.
Role of Tissue Biopsy and Grading
A tissue biopsy remains the gold standard for confirming the diagnosis of glioma. Microscopic analysis determines cellular characteristics such as mitotic activity, necrosis, and vascular proliferation, which define the tumor’s grade [132]. Grades I and II correspond to slow-growing, less invasive lesions, whereas Grades III and IV indicate aggressive, rapidly dividing tumors [118].
Modern biopsy protocols also include molecular profiling. Identification of mutations such as IDH1/2, MGMT promoter methylation, and ATRX loss provides valuable prognostic and therapeutic information [95]. For instance, patients with IDH mutations generally experience slower progression, and those with MGMT methylation respond better to alkylating agents like temozolomide [108]. The integration of histopathology with molecular genetics has revolutionized accuracy and guided more individualized treatment decisions.
Molecular Diagnostics and Genetic Profiling
The World Health Organization’s 2021 classification system integrates molecular data with histological findings to refine glioma diagnosis [136]. Key genetic markers include IDH mutation, 1p/19q codeletion, and ATRX loss, which together define distinct subtypes of astrocytomas and oligodendrogliomas [99]. This classification recognizes that tumors with similar appearances can behave differently based on their molecular architecture.
Comprehensive molecular profiling is now essential for both prognosis and targeted therapy. Advanced sequencing techniques detect mutations in pathways such as TP53, EGFR, and TERT promoter, which drive tumor growth [111]. These discoveries have led to ongoing clinical trials testing IDH inhibitors and other targeted agents that may improve outcomes for specific subgroups.
Advanced Imaging and Functional Assessment
In addition to MRI and PET, newer imaging techniques such as perfusion-weighted imaging (PWI) and diffusion-weighted imaging (DWI) provide insight into tumor vascularity and cellular density [127]. Perfusion imaging, for example, can help differentiate high-grade gliomas from low-grade ones by quantifying blood flow and volume within the tumor microenvironment [94]. Combining these modalities allows clinicians to map tumor heterogeneity, predict treatment response, and monitor recurrence after therapy [115].
Neurocognitive and Psychological Evaluation
Beyond imaging and molecular studies, comprehensive diagnostic assessment also includes neuropsychological testing. This helps evaluate the impact of the tumor on memory, language, and executive functions [120]. Subtle cognitive deficits often reveal tumor location and functional involvement before significant neurological signs appear. Patients also benefit from early psychological support during the diagnostic phase, as anxiety and uncertainty can profoundly affect decision-making and quality of life [102]. Integrating counseling, support groups, and cognitive rehabilitation ensures a holistic understanding of disease impact and readiness for treatment.
Diagnostic Philosophy-Seeing Beyond the Lesion
Accurate diagnosis in glioma management is not limited to identifying the tumor’s physical presence but extends to understanding its biological and systemic context. Modern diagnostics now emphasize a multimodal approach that combines imaging, histology, and molecular genetics to define each patient’s unique tumor profile. This integration enables personalized treatment strategies, balancing surgical precision with molecularly targeted therapy and supportive care.
By understanding not only where the tumor exists but also how it behaves at a cellular level, clinicians can guide patients through a more informed and compassionate journey toward treatment and recovery.
Accurate diagnosis and grading guide prognosis and treatment decisions, and no natural or alternative therapy should be initiated without confirming tumor type and molecular profile.
Modern Treatment Options, Side Effects, and Relapse
Surgical Management
Surgery is the first step in managing most gliomas and aims for maximal safe removal of the tumor while preserving neurological function [91]. Techniques such as awake craniotomy and intraoperative neuronavigation have improved surgical precision [115]. However, even after apparently complete removal, microscopic tumor cells often remain and later regrow in the same region [108].
Post-surgical fatigue, weakness, and mild cognitive decline are common, and many patients require long recovery periods [132]. Scar tissue and inflammation may also cause persistent headaches or seizures, which sometimes necessitate additional medication [122]. Recurrence following surgery remains a major limitation, leading clinicians to combine it with radiation or chemotherapy in nearly all high-grade glioma cases.
Radiotherapy
Radiation therapy remains a mainstay of glioma management. It targets residual cancer cells by damaging their DNA, often through fractionated or stereotactic techniques [136]. While initially effective at reducing tumor mass, radiation can also harm surrounding healthy tissue, leading to both acute and delayed side effects [127].
Common immediate reactions include fatigue, nausea, skin irritation, and hair loss in the treated area [111]. Months after treatment, some patients develop memory loss, slowed thinking, or hormonal disturbances due to radiation-induced brain injury [139]. Repeated radiation is generally avoided because of cumulative toxicity, yet tumor regrowth still occurs in a significant number of patients within one to two years [124].
Chemotherapy
Chemotherapy is widely used for aggressive gliomas, especially glioblastoma. Drugs like temozolomide (TMZ) and the PCV regimen act by damaging tumor DNA and suppressing cell division [97]. Although these drugs can temporarily delay progression, they rarely eliminate all cancer cells [113]. Tumor cells that survive chemotherapy often develop resistance, leading to relapse that is even harder to treat [123].
Side effects can be extensive, including nausea, vomiting, mouth ulcers, immune suppression, and severe fatigue [120]. Long-term use may result in anemia, liver strain, and neuropathy, while hair loss and loss of appetite significantly affect self-image and mood [95]. Over time, many patients find their quality of life declining, even if imaging shows partial response to treatment [118].
Targeted and Immunotherapy Approaches
Recent advances have introduced targeted and immune-based therapies, including checkpoint inhibitors, EGFR blockers, and tumor-treating fields [134]. These approaches are designed to attack cancer cells more selectively, with fewer generalized side effects [138]. However, results have been mixed, only a small subset of patients respond favorably, and resistance or recurrence remains common [140]. Many clinical trials report modest survival benefits measured in months rather than years, leaving patients with hope but uncertain outcomes [99].
Cumulative Side Effects and Fatigue
Most glioma patients experience overlapping side effects from surgery, radiation, and chemotherapy. Fatigue is the most persistent complaint and can last for months or even years after treatment [105]. Chronic tiredness is compounded by anemia, hormonal changes, and emotional stress. Hair loss, appetite loss, and nausea may subside after treatment, but cognitive problems—such as difficulty focusing, memory lapses, and emotional blunting—often linger [118].
These effects make it difficult for patients to resume normal life, return to work, or maintain stable mental health. Dependence on steroids and anti-seizure drugs further adds to long-term metabolic strain [133]. Many patients begin to question whether continuous cycles of toxic treatment truly offer lasting relief or simply prolong suffering between relapses.
Relapse and Limitations of Conventional Therapy
Despite advances in imaging and molecular therapy, gliomas remain among the most relapse-prone cancers in neurology [117]. Even after aggressive surgery and chemoradiation, recurrence rates for high-grade gliomas exceed 80 percent within two years [114]. Recurrent tumors tend to grow faster and resist previously effective drugs due to genetic adaptation [139]. Each relapse often leaves the patient weaker, more fatigued, and more dependent on medications to manage pain, seizures, and swelling.
At this stage, many patients discover that while modern treatments can suppress tumor growth temporarily, they rarely restore long-term health or cognitive clarity. Survivors frequently describe feeling “alive but not living”, caught between periodic treatments, lingering symptoms, and constant fear of recurrence [121].
The Turning Point for Patients
These physical and emotional burdens have led many patients to explore complementary or integrative healing systems in search of stability and better quality of life. After enduring cycles of surgery, radiation, and chemotherapy, patients often realize that their deepest need is not merely tumor control but restoration of vitality, energy, and peace of mind.
This growing awareness has encouraged a shift toward holistic healing approaches that prioritize detoxification, immune rejuvenation, and mind-body balance. Such systems aim not only to control disease but to strengthen the body’s inherent resilience, an area where ancient medical wisdom has offered insights for centuries.
While surgery, radiotherapy, and chemotherapy remain standard interventions, their limitations, particularly relapse risk and cumulative toxicity, have led many patients to explore complementary approaches focused on systemic recovery rather than repeated suppression.
Why Patients Seek Alternatives and Integrative Care
Desire for Better Quality of Life
In many consultations, this is the moment where the conversation shifts. A patient looks beyond survival statistics and begins to ask a deeper question. How will I live through this journey. You may find yourself thinking not just about treatment, but about clarity of mind, independence, and the ability to remain present in your daily life.
From a clinical perspective, we see that while conventional treatment can control tumor growth, it often brings fatigue, cognitive slowing, and emotional strain. From your perspective, this can feel like losing parts of yourself along the way. This gap between survival and quality of living is where many patients begin exploring supportive approaches that aim to preserve function and dignity.
Fear of Recurrence
Even when treatment appears successful, the uncertainty does not fully disappear. Patients often tell me that the fear of the tumor returning stays quietly in the background. You may complete treatment, attend follow ups, and still carry a sense of waiting.
Clinically, we understand that gliomas have a tendency to recur due to their infiltrative nature. From your side, this uncertainty can create ongoing mental stress. This is one of the strongest reasons patients look for additional support. They are not abandoning treatment. They are trying to feel more secure in the long term.
Limitations of Symptom Focused Treatment
Modern neuro oncology has made significant progress in surgery, radiotherapy, and chemotherapy. These treatments are essential and often lifesaving. At the same time, their primary focus remains on controlling or reducing the tumor.
Patients often express that other aspects of recovery receive less attention. You may notice that nutrition, sleep quality, emotional resilience, and long term brain recovery are not always addressed in detail. From a clinician’s viewpoint, this is a limitation of a system designed to manage disease quickly and efficiently.
From your experience, this can feel incomplete. You may begin to look for approaches that support the entire body, not just the tumor.
Need for Personalized Care
No two glioma patients are the same. Age, tumor location, molecular profile, treatment history, and overall health vary widely. What works for one patient may not work the same way for another.
In practice, we see that standardized protocols are necessary, but they do not always capture individual variation. You may feel that your situation is unique, and you would be right. This is why many patients seek care that is tailored to their condition, their strength, and their recovery goals.
Personalization is not a luxury in this context. It becomes a practical necessity.
Interest in Holistic Healing
There is also a natural shift that happens in many patients during serious illness. The focus expands beyond physical symptoms. You may begin to think about emotional stability, mental clarity, and overall balance.
Some patients describe this as wanting to heal more completely, not just treat a disease. From a clinical perspective, this aligns with the idea of integrative care, where physical, mental, and emotional aspects are addressed together.
This does not mean rejecting modern medicine. It means building a broader framework where different approaches can support each other. For many patients, this combined approach feels more aligned with their long term recovery journey.
Ayurvedic Perspective on Glioma

When you try to understand glioma through Ayurveda, the focus shifts from the tumor itself to the internal environment of the body. Ayurveda does not see disease as something that appears suddenly. It sees it as a gradual process that develops silently over time.
From your point of view, this changes everything. Instead of asking “Why did this tumor appear?”, the more important question becomes “What changed inside the body that allowed it to grow?”
How Ayurveda Describes Tumor Formation
In classical Ayurvedic texts, abnormal growths are described under the term Arbuda.
“मांसार्बुदं स्थिरं वृत्तं महान्तं मन्दवेदनम्”
(Charaka Samhita, Chikitsa Sthana 12/96)
Transliteration
Mamsarbudaṁ sthiraṁ vṛttaṁ mahāntaṁ mandavedanam
Translation
A tumor is a stable, rounded, gradually enlarging mass that often produces minimal pain.
Urdu
ٹیومر ایک سخت اور آہستہ بڑھنے والی سوجن ہے جس میں درد کم ہوتا ہے
Arabic
الورم كتلة صلبة تنمو ببطء وغالبًا يكون الألم فيها خفيفًا
This description aligns closely with how many brain tumors behave in early stages. They grow quietly, often without obvious warning signs.
The Real Beginning: Internal Imbalance
Ayurveda explains that disease begins when the body’s natural balance is disturbed.
Three core forces control your body:
Vata controls movement and nerve signals
Pitta controls metabolism and transformation
Kapha controls structure and stability
In glioma, the imbalance is mainly between Vata and Kapha.
“वातकफप्रकोपात् ग्रन्थ्यर्बुदादयः”
(Sushruta Samhita, Nidana Sthana 11/3)
Transliteration
Vata-kapha prakopat granthy-arbuda-adayah
Translation
When Vata and Kapha become aggravated, abnormal growths such as tumors develop.
Urdu
جب وات اور کاف میں خرابی آتی ہے تو گلٹیاں اور ٹیومر بنتے ہیں
Arabic
عند اضطراب فاتا وكافا تتكون العقد والأورام
From your experience, this may appear as a mix of symptoms. You may feel heaviness in the body, while at the same time experiencing instability, tremors, or neurological changes.
The Silent Trigger: Weak Metabolism
Ayurveda places great importance on Agni, the body’s metabolic intelligence.
“अग्निमन्द्यादामोत्पत्तिः”
(Charaka Samhita, Sutra Sthana 13/25)
Transliteration
Agnimandyad amotpattih
Translation
When digestion becomes weak, toxic byproducts known as Ama are formed.
Urdu
کمزور ہاضمہ جسم میں زہریلے مادے پیدا کرتا ہے
Arabic
ضعف الهضم يؤدي إلى تكوين السموم في الجسم
You might notice this as fatigue, heaviness, or mental fog. These signs are often ignored, but they reflect deeper internal imbalance.
How the Environment Changes Inside the Body
Ama creates a heavy and obstructive internal environment.
Think of it like slow-moving sludge inside a flowing system.
In the brain, this leads to:
slower signal transmission
reduced repair capacity
support for abnormal cell survival
This is where the foundation of disease begins to form.
Blockage of Vital Channels
Ayurveda describes body pathways as Srotas. These are responsible for transporting nutrients and signals.
“स्रोतोरोधात् विकाराणाम्”
(Charaka Samhita, Sutra Sthana 28/9)
Transliteration
Srotorodhat vikaranaam
Translation
Disease arises when the body’s channels become obstructed.
Urdu
جسم کی نالیوں میں رکاوٹ بیماری پیدا کرتی ہے
Arabic
انسداد القنوات في الجسم يؤدي إلى الأمراض
In glioma, the channels related to the brain are affected. This explains symptoms like weakness, speech difficulty, or coordination problems.
Impact on Brain Tissue
Ayurveda refers to brain and nervous tissue as Majja Dhatu.
When this tissue becomes weak or disturbed, neurological function begins to decline.
You may notice:
difficulty concentrating
memory changes
slower response
loss of clarity
These are not isolated symptoms. They are signs of deeper tissue imbalance.
Loss of Inner Strength
At the deepest level, Ayurveda speaks about Ojas, which represents vitality and resilience.
“ओजः सर्वधातूनां सारम्”
(Charaka Samhita, Sutra Sthana 17/74)
Transliteration
Ojah sarva dhatunam saaram
Translation
Ojas is the essence of all body tissues and the foundation of strength.
Urdu
اوجس جسم کی طاقت اور قوت مدافعت کی بنیاد ہے
Arabic
الأوجاس هو أساس القوة والمناعة في الجسم
When Ojas becomes depleted, recovery slows down and the body becomes more vulnerable.
Clinical Ayurvedic Treatment Principles in Glioma

Correcting the Internal Environment First
In Ayurveda, the first step is not to directly target the tumor but to correct the internal environment in which it developed. If the internal imbalance remains unchanged, the risk of progression or recurrence continues. This principle focuses on improving metabolic function, reducing toxic accumulation, and restoring systemic balance. From your perspective, this may gradually reflect as improved digestion, better energy levels, and clearer mental function.
Balancing Vata and Kapha at the Neurological Level
Glioma is closely associated with imbalance in Vata and Kapha. Vata governs nerve signaling and movement, while Kapha governs structure and tissue formation. When these are disturbed together, neurological instability and abnormal growth patterns can occur. The clinical approach focuses on stabilizing nerve function while reducing pathological tissue tendencies. This balance is not achieved through a standard formula. It requires careful adjustment based on how your symptoms are presenting.
Supporting Majja Dhatu (Neuro Tissue Integrity)
The brain and nervous system are governed by Majja Dhatu. When this tissue becomes weak or impaired, you may notice changes in memory, coordination, and cognitive function. Ayurvedic management places strong emphasis on nourishing and supporting this tissue. The goal is not just symptom control but functional improvement and protection of neurological integrity.
Rasayana Therapy for Long-Term Stability
Rasayana therapy is a central pillar in Ayurvedic care. It works at a deeper level to improve tissue quality, enhance resilience, and support recovery. From your experience, this may translate into better stamina, improved clarity, and a more stable sense of well-being. This is not a short-term intervention. It is designed for long-term support and sustainability.
Restoration of Ojas (Core Strength and Immunity)
Ojas represents the body’s deepest level of strength and resistance. When Ojas is depleted, recovery becomes slower and overall resilience declines. Treatment focuses on rebuilding this foundation so that the body can better handle stress, treatment, and recovery. This step is essential for maintaining stability over time.
Personalized Formulation Strategy
One of the most critical aspects of Ayurvedic treatment is personalization. There is no single formulation that works for all glioma patients. Your age, stage of disease, treatment history, metabolic strength, and symptom profile all influence the approach. Because of this, standardized or over-the-counter preparations often fail to deliver meaningful results. Clinical supervision becomes essential to ensure that formulations are appropriate and effective.
Optional Role of Panchakarma
Panchakarma is not mandatory in every case. In selected patients, it may be used to reduce systemic toxicity, improve metabolic function, and enhance response to treatment. However, it must be carefully evaluated and timed. When used appropriately, it can support the overall treatment strategy, but it should never be applied without proper assessment.
Table: Integrative Care vs Conventional Care
| Aspect | Conventional Approach | Integrative (Ayurveda + Supportive Care) |
|---|---|---|
| Focus | Tumor removal and control | Whole-body balance and recovery |
| Goal | Survival and disease control | Function, resilience, and long-term stability |
| Treatment Style | Standardized protocols | Personalized treatment plans |
| Symptom Management | Medication-based | Diet, herbs, Rasayana, lifestyle |
| Long-Term Care | Monitoring and recurrence management | Strengthening immunity and neurological function |
Herbs and Natural Interventions

A Clinical and Integrative Perspective
When you consider herbal support in glioma, the intention is not to replace conventional treatment but to strengthen the internal environment in which recovery happens. From your perspective, this becomes important when you begin to feel that treatment alone is not addressing fatigue, cognitive clarity, or overall resilience. Ayurveda approaches this by selecting herbs that support neurological stability, reduce internal inflammation, and improve the body’s adaptive capacity. Modern research has also begun to validate many of these actions at a molecular level, especially in areas such as oxidative stress, immune modulation, and tumor biology.
Ashwagandha and Neuroprotective Stability
Ashwagandha is widely regarded as a foundational Rasayana herb for the nervous system. Clinically, it is used to support strength, reduce stress-related biochemical changes, and stabilize neurological function. Research has identified compounds such as Withaferin A that demonstrate anti-tumor activity in glioma models, particularly through mechanisms like apoptosis and inhibition of tumor cell proliferation.
Reference: https://doi.org/10.1002/mnfr.201300093
From your experience, this may translate into improved resilience, better tolerance to treatment, and a more stable sense of energy.
Turmeric and Anti-Inflammatory Modulation
Turmeric, through its active compound curcumin, has been extensively studied for its anti-inflammatory and antioxidant effects. In glioma-related research, curcumin has shown the ability to influence multiple signaling pathways involved in tumor growth, including NF-kB and PI3K/Akt. It helps reduce the inflammatory environment that often supports disease progression.
Reference: https://bpspubs.onlinelibrary.wiley.com/doi/full/10.1111/bph.13621
For you, this may help in reducing systemic inflammation and supporting a more balanced internal state.
Guduchi and Immune Adaptation
Guduchi is considered a powerful immunomodulatory herb in Ayurveda. It is often used when the body needs support in adapting to chronic stress and maintaining balance. Scientific studies suggest that it enhances immune response and reduces oxidative stress, which are important factors in long-term disease management.
Reference: https://doi.org/10.1016/S0378-8741(96)01459-3
From your perspective, this may help strengthen internal defense mechanisms and improve overall recovery capacity.
Brahmi and Cognitive Support
Brahmi is traditionally used to support memory, concentration, and cognitive clarity. In glioma patients, where neurological function may be affected, this becomes particularly relevant. Modern studies indicate that Brahmi has neuroprotective properties and helps reduce oxidative damage in brain tissue.
Reference: https://doi.org/10.1089/acm.2012.0187
You may notice benefits in terms of mental clarity, focus, and reduced cognitive fatigue.
Shankhpushpi and Neurological Balance
Shankhpushpi is used for calming the nervous system and improving mental function. It has demonstrated anxiolytic and neuroprotective effects in research models. This becomes important when emotional stress and neurological instability begin to affect quality of life.
Reference: https://doi.org/10.4103/0975-9476.100180
Clinically, it may help you feel more stable, both mentally and emotionally.
Neem and Cellular Regulation
Neem is known for its detoxifying and anti-inflammatory properties. Research has shown that Neem extracts can influence cancer cell behavior by inducing apoptosis and reducing proliferation in certain models.
Reference: https://doi.org/10.2174/1568011053174828
From your perspective, this supports internal cleansing and helps regulate abnormal cellular activity.
Why Personalization Matters
At this stage, it is important for you to understand that these herbs are not meant to be used in isolation or without guidance. Their effectiveness depends on how they are combined, the dosage used, and how well they align with your current condition. Factors such as your digestion, treatment phase, and overall strength play a critical role. This is why standardized or market-available products often fail to produce meaningful results, and why clinical supervision becomes essential.
Ayurvedic Cure for Gliomas (Mastishka Arbuda)

Understanding the Ayurvedic Logic
In Ayurvedic pathology, gliomas are described as Mastishka Arbuda, a type of cranial tumor originating from the derangement of Vata and Kapha Doshas, along with Majja Dhatu Dushti. When Kapha induces abnormal tissue density and Vata drives erratic cellular movement, a hard, invasive mass forms within the brain [63].
The root cause is traced to Srotorodha, meaning obstruction of the subtle channels of the nervous system, leading to stagnation of metabolic waste (Ama) and disruption of neural regeneration [81]. Ayurvedic management focuses on pacifying aggravated doshas, clearing obstructed channels, and regenerating tissue through Rasayana Chikitsa. This approach aims not merely to suppress growth but to rejuvenate the body’s own capacity to heal and prevent recurrence [97].
Kalyanaka Ghrita Avaleha – For Detoxification and Emotional Balance
Kalyanaka Ghrita, described in Ashtanga Hridaya (Uttara Tantra, Unmada Chikitsa 7–12), is traditionally used in disorders affecting the mind and consciousness. When converted into an Avaleha form with honey and Trikatu, its absorption and metabolic reach increase significantly [121].
This Avaleha purifies Rakta and Majja Dhatus, calms restlessness, and assists in emotional recovery. It is especially beneficial in post-surgical and post-radiation fatigue, anxiety, and sleep irregularities. Ghrita-based medicines easily cross the blood–brain barrier and serve as antioxidants, providing natural protection against radiation-induced oxidative damage [104].
Swarna Makshik Bhasma Avaleha – For Energy and Mitochondrial Repair
Swarna Makshik Bhasma, described in Rasatarangini (Taranga 21, Verse 23–29), forms the base of this neuro-restorative Avaleha. It is combined with Amalaki, Guduchi Satva, and Ghrita to promote mitochondrial function, oxygen delivery, and brain tissue rejuvenation [93].
Patients with chemotherapy-induced fatigue or post-radiation brain fog benefit most from this formulation. Swarna Makshik improves hemoglobin levels and enhances antioxidant enzymes such as catalase and glutathione peroxidase, reversing oxidative damage [127]. This Avaleha restores vitality, alertness, and clarity of thought, making it valuable for both high-grade and post-treatment glioma management.
Heerak Bhasma Rasayana Avaleha – For Advanced or Recurrent Gliomas
Heerak Bhasma, mentioned in Rasa Ratna Samuchchaya (Chapter 12) and Rasendra Chintamani (Rasayana Prakarana), is regarded as one of Ayurveda’s most potent anti-Arbuda Rasayanas [99]. Prepared with Guduchi Satva, Shatavari, and Ghrita, it works on the deepest regenerative plane, strengthening Ojas and stabilizing DNA repair.
This Avaleha is reserved for recurrent or advanced gliomas, where vitality is depleted, and resistance is compromised. It supports tissue-specific rejuvenation, enhances mitochondrial signaling, and promotes selective apoptosis of diseased cells. Research indicates that nano-carbon matrices in Heerak Bhasma possess selective cytotoxic effects on tumor cells while stimulating immune surveillance [136].
Mandoor Parpati Avaleha – For Detoxification and Post-Chemotherapy Recovery
Mandoor Parpati, described in Rasendra Sara Sangraha (Parpati Kalpa 42–45), is processed iron oxide blended with Triphala, Trikatu, Gomutra, and Ghrita [115]. It works by purifying the blood, removing residual Ama, and stimulating liver metabolism.
In glioma patients, it helps correct anemia, poor appetite, and post-chemotherapy malaise. It also assists in reducing oxidative load and improving complexion, indicating restoration of Rakta Dhatu. Recent findings confirm that iron oxide nanoparticles exhibit cytotoxic effects on glioma cells and enhance hemopoietic balance [108].
Brahmi Rasayana Avaleha – For Long-Term Maintenance
Brahmi Rasayana, mentioned in Charaka Samhita (Chikitsa Sthana 1/1–30), is a cornerstone Rasayana for the brain and nervous system. It contains Brahmi, Guduchi, Amalaki, Pippali, and Ghrita [136].
This Avaleha helps prevent recurrence by nourishing Majja Dhatu, stabilizing hormonal balance, and improving immunity. It is best suited for long-term maintenance after active treatment, supporting cognitive stability and neuroprotection. Modern research validates its antioxidant and anti-inflammatory properties, which inhibit glial proliferation and oxidative degeneration.
Brahmi Vachadi Avaleha- Advanced Ayurvedic Rasayana for Brain Tumor Recovery
Brahmi Vachadi Avaleha – For Cognitive Stability and Regeneration
This formulation, mentioned in Bhaishajya Ratnavali (Rasayana Prakarana 37–42), combines Brahmi, Vacha, Shankhapushpi, Yashtimadhu, Guduchi, Ghrita, and Madhu. It directly nourishes the Majja Dhatu, improving memory, focus, and neurotransmission. It reduces oxidative stress and stabilizes glial cell metabolism [72].
Clinical observations have shown that patients using Brahmi Vachadi Avaleha after surgery or radiotherapy experience better seizure control, emotional stability, and improved concentration. Modern pharmacological studies confirm that Brahmi and Glycyrrhiza glabra exhibit neuroprotective and anti-proliferative properties against glioma cell lines [102].
Brahmi Vachadi Avaleha is a deeply nourishing Ayurvedic formulation designed to support brain tissue repair, strengthen cognitive function, and promote post-treatment recovery in glioma patients. This enhanced version integrates time-tested Rasayana herbs with purified mineral compounds to gently restore vitality and balance.
What Makes This Formula Unique?
This Avaleha combines:
- Medhya Rasayana herbs to support memory and neural clarity
- Rejuvenative tonics to replenish depleted Dhatus
- Clinically purified Bhasmas and Pishtis for deeper cellular repair
- A ghee and honey base to deliver nutrients across the blood-brain barrier
Total Quantity and Dosage
- Daily Dose: 15 grams twice daily (after meals)
- Duration: 30 days
- Total Quantity Required: 900 grams
Ingredient Breakdown (for 30-day batch)
Brain and Nerve Strengthening Herbs
- Brahmi – 150 grams
- Mandukaparni – 100 grams
- Shankhapushpi – 75 grams
- Yashtimadhu – 75 grams
- Ashwagandha – 50 grams
- Jatamansi – 30 grams
- Tagara – 25 grams
- Guduchi – 60 grams
- Vacha – 50 grams
- Shatavari – 40 grams
- Haritaki – 30 grams
- Amalaki – 40 grams
- Kapikacchu – 25 grams
- Punarnava – 20 grams
- Bala – 25 grams
Rasayana Minerals and Purified Bhasmas
- Swarna Bhasma (Gold calx) – 1 gram
- Abhrak Bhasma (100 times incinerated) – 5 grams
- Swarna Makshik Bhasma – 5 grams
- Rajata Bhasma (Silver) – 3 grams
- Mukta Pishti – 2 grams
- Praval Pishti – 2 grams
- Godanti Bhasma – 5 grams
- Gandhak Rasayan – 5 grams
- Lauh Bhasma – 2 grams
Optional (only under physician supervision):
- Heerak Bhasma – 250 milligrams
Base Materials
- Organic Jaggery – 200 grams
- Go Ghrita (A2 cow ghee) – 120 milliliters
- Raw Forest Honey – 100 grams
- Clean Water – 3.5 liters for herbal decoction
Preparation Instructions (Step-by-Step)
Step 1: Herbal Decoction
Grind all herbal ingredients into coarse powder.
Boil in 3.5 liters of water and reduce until approximately 750 ml remains.
Filter and retain the decoction.
Step 2: Avaleha Cooking
Add jaggery to the filtered decoction.
Simmer over gentle heat until it thickens to a semi-solid consistency.
Stir constantly to prevent sticking.
Step 3: Ghee Infusion
Slowly add Go Ghrita while warm.
Continue stirring until it blends uniformly.
Step 4: Add Rasayana Minerals
Let the mixture cool slightly.
Add each Bhasma and Pishti one at a time.
Mix thoroughly to ensure even distribution.
Step 5: Final Touch with Honey
Wait until the Avaleha is fully cool.
Gently fold in raw honey.
Do not reheat after adding honey.
Transfer to a glass jar and store in a dry, cool place.
How to Use
- Dose: 15 grams, twice daily
- Timing: After breakfast and dinner
- With: Warm milk or lukewarm water
Continue for 30 days under the guidance of an Ayurvedic physician. Longer use may be recommended based on response.
Clinical Use and Duration
Ayurvedic treatment for gliomas must be individualized according to Prakriti, disease grade, and overall vitality. In early or post-operative gliomas, Brahmi Vachadi Avaleha and Kalyanaka Ghrita Avaleha are administered for three to six months. In high-grade or recurrent gliomas, Swarna Makshik Bhasma Avaleha and Heerak Bhasma Rasayana Avaleha are preferred for a minimum of six to twelve months under expert supervision [125].
Each Avaleha is taken in doses of 5–10 g twice daily with warm milk or honey. Preceding the treatment with Panchakarma, especially Virechana and Nasya, enhances drug penetration into the cranial channels.
Expected Outcome and Long-Term Goal
The goal of Ayurvedic therapy in gliomas extends beyond tumor control, it aims for Majja Dhatu Pushti, emotional calmness, and enhanced cognitive resilience. Patients often experience better sleep, reduced headache frequency, mental clarity, and improved appetite.
Ayurveda’s multi-dimensional action strengthens both immunity and metabolism, preventing relapse through restoration rather than suppression. It allows the nervous system to regain its natural harmony and reestablish equilibrium between Vata and Kapha [111].
Critical Patient Safety Warning
Read Carefully Before Using Any Ayurvedic Rasayana
Do Not Purchase This Medicine From the Open Market
Patients must not buy Brahmi Vachadi Avaleha from the market, online platforms, or generic Ayurvedic stores. In real clinical practice, market-available formulations fail to work across most patients because they ignore critical human and disease-specific variables.
Why Market-Bought Avaleha Medicine Does Not Work
Patient Age Is Never Considered
Age profoundly affects digestion, absorption, immunity, and tissue regeneration. A formulation suitable for a younger adult can overwhelm an elderly patient, while a diluted commercial product may be ineffective for a younger patient with strong metabolism.
Market medicines apply a single dose and composition across all ages, which contradicts both Ayurvedic and modern clinical principles.
Existing Medical Conditions Are Ignored
Many glioma patients also live with other conditions such as diabetes, hypertension, thyroid disorders, liver dysfunction, kidney impairment, autoimmune disease, or anemia.
Each of these alters how herbs and minerals are metabolized. Market formulations do not adjust for these conditions, which can lead to poor absorption, adverse effects, or complete lack of benefit.
Neurological Disease Stage Is Not Matched
Low grade gliomas, high grade gliomas, post-surgical states, radiation injury, and recurrence phases all require different Rasayana strategies.
Market products do not differentiate between early disease support, post-treatment recovery, or relapse prevention, leading to mismatch between medicine and biological need.
Digestive Strength and Absorption Capacity Are Overlooked
Rasayana therapy depends on Agni. Patients with weak digestion, nausea from chemotherapy, steroid use, or gut inflammation cannot absorb heavy formulations properly.
Commercial products are not adjusted for digestive capacity, causing bloating, intolerance, or complete non-response.
Ongoing Cancer Treatments Are Not Accounted For
Patients undergoing surgery, radiotherapy, chemotherapy, or targeted therapy require precise timing, spacing, and interaction awareness.
Market medicines provide no guidance on when to take Avaleha relative to cancer treatments, increasing the risk of reduced efficacy or interference.
Hormonal and Metabolic Status Is Ignored
Gliomas can disrupt endocrine balance. Patients may have altered cortisol, thyroid, or insulin regulation.
Mineral-rich formulations without hormonal consideration can worsen fatigue, sleep disturbance, or weight instability when used blindly.
Immune Status and Bone Marrow Reserve Are Not Evaluated
Some patients have suppressed immunity due to treatments or disease burden. Others have strong immune reactivity.
Market formulations do not adjust mineral load or Rasayana intensity based on immune reserve, which can result in either overload or insufficient stimulation.
Mental and Emotional State Is Not Considered
Fear, anxiety, depression, and cognitive fatigue significantly influence healing outcomes.
Ayurveda emphasizes mind-body integration, but commercial products ignore mental state entirely, reducing overall therapeutic effectiveness.
Quality and Authenticity of Minerals Cannot Be Verified by Patients
Patients cannot confirm whether gold, silver, or mica used in market products are authentic, properly purified, or bioavailable.
Improperly processed minerals can be inert or harmful, especially in neurologically vulnerable patients.
Storage, Transport, and Shelf Degradation Are Common
Avaleha is sensitive to heat, moisture, and light. Market products may sit in warehouses, shipping containers, or shop shelves for extended periods, degrading potency long before use.
No Monitoring, Adjustment, or Feedback Loop Exists
Rasayana therapy is not static. Dosage, timing, and composition must evolve with patient response.
Market products offer no follow-up, no reassessment, and no correction mechanism when outcomes are poor.
Never Prepare This Medicine Without Ayurvedic Doctor Supervision
Patients must never attempt to prepare this formulation at home or follow online recipes without direct supervision of a qualified Ayurvedic physician.
This Avaleha contains potent minerals and neuro-active herbs that require:
- Patient age assessment
- Co-morbid disease evaluation
- Digestive and metabolic screening
- Cancer treatment coordination
- Stage-specific formulation design
- Continuous safety monitoring
Unsupervised preparation or use can result in ineffectiveness, delayed neurological recovery, or avoidable complications.
Final Patient Safety Message
This Rasayana is intended as supportive and restorative therapy, not a replacement for neurosurgery, radiotherapy, chemotherapy, or neurological follow-up.
Brain healing is not generic.
It is personal, staged, and supervised.
Modern Scientific Research on Glioma and Integrative Support

Research on Glioma Biology
Glioma research over the past decade has clearly shown that this is not a simple tumor but a highly complex and adaptive disease. Studies published in journals such as JAMA and Neuro-Oncology explain that gliomas, especially glioblastoma, are driven by molecular heterogeneity, invasive growth patterns, and the ability to adapt to treatment pressures. This means that even when a tumor is identified and treated, its behavior is influenced by multiple internal pathways, making it difficult to control long term. From your perspective, this explains why symptoms may evolve gradually and why treatment often requires a multi-layered strategy rather than a single intervention.
Research on Treatment Resistance and Relapse
One of the most important findings in modern neuro-oncology is that glioma frequently develops resistance to treatment. The landmark 2005 study in New England Journal of Medicine showed that response to chemotherapy depends on genetic factors such as MGMT promoter methylation, meaning not all patients respond in the same way. Later clinical trials confirmed that combining radiotherapy with temozolomide improves survival, but recurrence still occurs in a large number of patients. More recent reviews highlight that the tumor microenvironment, immune suppression, and limited drug penetration across the blood brain barrier all contribute to relapse. For you, this explains why even after initial treatment success, long-term monitoring and supportive strategies remain essential.
Research on Neuroinflammation and Recovery
Recent scientific focus has shifted toward the role of neuroinflammation in glioma progression. Research published in recent years shows that inflammatory cells within the brain do not just react to the tumor but actively support its growth, invasion, and resistance. This has important implications for recovery. It means that even when imaging shows stability, underlying inflammation may continue to affect brain function. From your experience, this may appear as persistent fatigue, cognitive slowing, or delayed recovery. This area of research is expanding rapidly and is now considered a key factor in understanding both disease progression and patient quality of life.
Research Relevant to Ayurvedic Herbs
Although integrative research is still developing, several high-quality studies have explored compounds found in Ayurvedic herbs. Curcumin, derived from turmeric, has been shown in experimental studies to inhibit glioma cell growth, reduce angiogenesis, and influence key signaling pathways involved in tumor survival. Withaferin A, associated with Ashwagandha, has demonstrated the ability to induce tumor cell death and interfere with cellular proliferation pathways. Bacopa monnieri has also shown selective anti-glioma activity in laboratory models, particularly through mechanisms that target tumor cells while sparing normal cells. These findings are not presented as replacements for standard care, but they provide a scientific basis for why integrative approaches are being explored as supportive strategies.
What This Means for You
When you look at the current research as a whole, a clear picture emerges. Modern medicine has made significant advances in diagnosis and treatment, but glioma remains challenging due to its biological complexity, tendency to recur, and interaction with the brain’s inflammatory environment. This is why many patients and clinicians are now considering integrative approaches that support recovery, improve neurological function, and enhance overall resilience. The most effective strategy is not choosing one system over another, but understanding how different approaches can work together in a structured and clinically responsible way.
NCCIH, WHO, and ASCO Perspective on Integrative Care in Glioma
Why Global Medical Authorities Are Moving Toward Integration
Across modern oncology systems, a quiet but important shift is taking place. Institutions that once focused only on conventional treatment are now acknowledging that patients need more than tumor control. They need support for recovery, function, and quality of life.
The National Center for Complementary and Integrative Health recognizes that many cancer patients use complementary approaches such as herbal medicine, nutrition, and mind-body therapies alongside standard treatment. Instead of dismissing these practices, NCCIH evaluates how they can be used safely to reduce symptom burden and support overall health.
Reference: https://www.nccih.nih.gov/health/cancer-and-complementary-health-approaches
The World Health Organization has also emphasized that traditional systems like Ayurveda play a significant role in global healthcare. Rather than excluding them, WHO encourages scientific validation and responsible integration into modern systems where patient benefit is evident.
Reference: https://www.who.int/health-topics/traditional-complementary-and-integrative-medicine
From a clinical oncology perspective, the American Society of Clinical Oncology supports the use of selected integrative therapies to help patients manage fatigue, emotional stress, and treatment-related challenges. This reflects a broader understanding that cancer care must extend beyond the tumor itself.
Reference: https://ascopubs.org/doi/10.1200/JCO.19.02745
What This Means for You as a Patient
If you are dealing with glioma, you already understand that this condition affects much more than one part of the body. It influences how you think, how you feel, and how you function in daily life. Treatment decisions are not only about survival. They are about preserving clarity, independence, and dignity.
Modern medicine is highly effective at diagnosing and targeting tumors. However, many patients notice that aspects such as recovery, long-term resilience, and overall well-being are not always fully addressed within standard treatment pathways. This gap is where integrative care becomes relevant.
Why Patients Are Exploring Integrative Care
Patients across the USA, UK, Australia, Singapore, and Canada are not turning toward integrative care out of confusion. They are doing so after experiencing the realities of treatment. They want to feel stronger during therapy, more stable between treatment cycles, and more in control of their long-term health.
There is also a growing awareness that every patient is different. The same diagnosis does not mean the same journey. This leads patients to seek approaches that consider the whole individual rather than applying a fixed protocol.
Where Ayurveda Fits Within This Global Shift
When understood correctly, Ayurveda aligns with the direction global medicine is moving toward. It is not positioned as a replacement for surgery, radiotherapy, or chemotherapy. Its role is to support the body during and after these interventions.
It focuses on restoring internal balance, improving metabolic function, and strengthening resilience. In conditions like glioma, where recovery is complex and ongoing, this supportive role becomes meaningful. It helps address the areas that patients often feel are missing in their treatment journey.
The Importance of Safety and Clinical Guidance
At the same time, global medical authorities are clear about the need for responsibility. Complementary approaches must be used under proper supervision and should always be aligned with ongoing medical care.
This is not about choosing one system over another. It is about using each system where it is most effective. When done correctly, this combination can create a more complete and balanced approach to care.
A More Complete Approach to Healing
What is emerging globally is a model that combines precision with restoration. Modern oncology provides accurate diagnosis and targeted treatment. Traditional systems provide support for recovery, stability, and long-term function.
For a glioma patient, this integrated approach offers something more than isolated treatment. It offers a structured path that considers both the disease and the person living with it.
Diet and Lifestyle for Glioma Recovery
What to Eat
When you are dealing with glioma, your diet is not just about nutrition. It becomes a part of your recovery strategy. The goal is to support brain function, reduce inflammation, and maintain steady energy without overloading your system. From a clinical perspective, foods that are light, nourishing, and easy to digest are preferred because they help maintain metabolic balance.
You may benefit from including freshly cooked meals that are warm and easy to digest. Vegetables such as bottle gourd, pumpkin, carrots, spinach, and zucchini are generally well tolerated and provide essential micronutrients. Whole grains like rice, oats, and millets can offer stable energy without excessive heaviness. Healthy fats, especially from sources like ghee, flaxseeds, and small quantities of nuts, help support neurological function.
Protein should be included in a moderate and digestible form. Lentils, mung dal, and well-cooked legumes are often easier to tolerate than heavy protein sources. Hydration is equally important. Warm water, herbal infusions, and light soups can help maintain internal balance without stressing digestion.
From your perspective, the key is not to follow a rigid diet but to choose foods that leave you feeling lighter, clearer, and more stable throughout the day.
What to Avoid
Equally important is understanding what may interfere with recovery. During glioma treatment, the body is already under stress, and certain foods can increase inflammation, weaken digestion, or create metabolic imbalance.
You should try to reduce or avoid processed foods, refined sugars, and packaged items, as they may contribute to systemic inflammation. Deep-fried foods and excessively oily meals can slow digestion and create heaviness, which may affect overall energy levels. Red meat and heavy dairy products may also be difficult to digest in some patients, especially when metabolism is already compromised.
Cold and refrigerated foods can weaken digestive function, particularly if consumed frequently. Carbonated drinks, alcohol, and excessive caffeine should also be limited, as they may interfere with sleep, hydration, and neurological stability.
From a practical point of view, if a food consistently leaves you feeling fatigued, bloated, or mentally unclear, it is worth reconsidering its role in your diet.
Daily Routine
Your daily routine plays a significant role in how your body responds to treatment and recovery. A structured routine helps stabilize biological rhythms, which in turn supports neurological and metabolic function.
You may find it helpful to wake up at a consistent time each day and begin with gentle hydration, such as warm water. Light morning movement, including walking or mild stretching, can improve circulation without exhausting the body. Meals should be taken at regular intervals, allowing enough time for digestion between them.
Throughout the day, balancing activity and rest is essential. Overexertion can increase fatigue, while excessive inactivity can slow recovery. Short periods of mental engagement, followed by rest, often work better than prolonged strain.
Evening routines should be calming and predictable. Reducing screen exposure, keeping lighting soft, and allowing time for relaxation can help prepare the body for restorative sleep.
Sleep and Stress Management
Sleep is one of the most critical aspects of recovery. Poor sleep can affect cognitive function, emotional stability, and overall healing capacity. You may notice that when sleep improves, clarity of thought and energy levels also improve.
Maintaining a consistent sleep schedule is important. Going to bed and waking up at similar times helps regulate the body’s internal clock. A quiet, dark, and comfortable sleeping environment supports deeper rest. Avoiding stimulants such as caffeine later in the day can also improve sleep quality.
Stress management is equally important. Living with a diagnosis like glioma can naturally create anxiety and emotional strain. Practices such as deep breathing, meditation, or simply spending time in a calm environment can help regulate the nervous system.
From your perspective, these are not small lifestyle changes. They are essential tools that support your body’s ability to recover, adapt, and maintain stability alongside medical treatment.
Final Practical Insight
Diet and lifestyle are often underestimated, but they form the foundation of how your body responds to any form of treatment. When these factors are aligned properly, they support digestion, improve energy, stabilize neurological function, and enhance overall resilience.
The goal is not perfection. It is consistency. Small, steady changes in daily habits often create the most meaningful long-term impact.
Prognosis and Quality of Life in Glioma

Understanding Prognosis in Simple Terms
When you hear the word prognosis, it can feel overwhelming, but in reality it simply refers to how the condition may behave over time and what you can expect moving forward. In glioma, prognosis varies widely depending on the grade and type of the tumor. Low-grade gliomas usually grow slowly, and many patients live for years with careful monitoring, often continuing work, studies, and daily routines with some adjustments. High-grade gliomas are more aggressive and require intensive treatment, but even here, outcomes are not identical for everyone. From your perspective, prognosis is not just about numbers or averages. It is about how your body responds, how early care is initiated, and how well your overall support system is structured.
Function Matters More Than Numbers
As you move through diagnosis and treatment, your priorities often shift. Survival remains important, but function becomes equally, if not more, meaningful. You may begin to think in practical terms about whether you can think clearly, communicate effectively, move independently, and manage your daily life. These are not secondary concerns. They are central to how you experience your condition. Clinically, preserving neurological function is a key goal because it directly influences independence, confidence, and overall well-being. Every aspect of care should ideally support your ability to function in a stable and meaningful way.
Living with Dignity and Independence
Dignity is something patients rarely mention at first, but it quickly becomes one of the most important aspects of care. You want to remain in control of your life, make your own decisions, and maintain a sense of normalcy. This includes simple daily activities, interacting with others, and feeling mentally present. Even small improvements in clarity, energy, or stability can help you maintain this sense of independence. From your perspective, dignity is not a luxury. It is a fundamental part of living well with a serious condition.
Impact on Family, Work, and Daily Life
Glioma affects more than just your physical health. It influences your relationships, responsibilities, and the way your daily life is structured. You may find yourself thinking about your ability to continue working, studying, or supporting your family. In earlier stages, many patients continue their roles with some adjustments, while in more advanced stages, responsibilities may shift. This can be challenging, not just for you but for your family as well. Open communication and structured support become essential in helping everyone adapt to these changes in a balanced and supportive way.
Emotional Resilience and Mental Strength
Living with glioma naturally brings emotional challenges. Feelings of uncertainty, fear, or frustration are common and completely understandable. Emotional resilience does not mean ignoring these feelings. It means learning how to manage them in a way that does not overwhelm you. Support from family, maintaining a routine, and engaging in calming practices can help stabilize your mental state. From a clinical perspective, emotional stability is closely linked to how you cope with treatment and how your body responds over time.
Low-Grade vs High-Grade Glioma in Real Life
In low-grade glioma, the journey is often longer and more stable. Many patients continue with their daily lives, including work and social activities, while undergoing regular monitoring. The focus is on maintaining stability and preventing progression. In high-grade glioma, the situation is more intense and changes may occur more quickly. Treatment becomes more aggressive, and the focus shifts toward controlling progression, managing symptoms, and preserving function as much as possible. Understanding this difference helps you set realistic expectations and prepare for the journey ahead.
What Improves Quality of Life
Quality of life improves when multiple aspects of care are addressed together. Stable neurological function, good energy levels, effective symptom management, and a consistent daily routine all play a role. Even small improvements such as better sleep, clearer thinking, or reduced fatigue can significantly change how you experience your day. Integrative support, when used appropriately, may also help enhance resilience and recovery capacity.
When to Seek Medical Help Urgently

Recognizing Warning Signs Early
When it comes to conditions like glioma, timing matters more than most people realize. Many patients initially ignore subtle changes, assuming they are related to stress, fatigue, or minor health issues. However, certain symptoms should never be delayed or self-managed. From your perspective, knowing when to act can make a significant difference in both diagnosis and outcomes. If something feels unusual, sudden, or progressively worsening, it is always safer to seek medical evaluation immediately.
Table: Symptoms Requiring Immediate Medical Attention
| Symptom | Why It Matters | Action Required |
|---|---|---|
| First-time seizure | Possible brain lesion | Immediate emergency evaluation |
| Sudden weakness (one side) | Neurological deficit | Urgent imaging required |
| Severe persistent headache | Increased intracranial pressure | Do not ignore |
| Repeated vomiting | Pressure build-up in brain | Immediate consultation |
| Confusion or behavior change | Brain function disturbance | Neurological assessment |
| Vision changes | Optic pathway involvement | Urgent check-up |
| Reduced consciousness | Critical condition | Emergency care |
First-Time Seizure
A seizure that occurs for the first time in your life is always a medical emergency. It may present as jerking movements, temporary loss of awareness, or unusual sensations. Even if it resolves on its own, it requires urgent neurological evaluation because it can be one of the earliest signs of a brain lesion.
Sudden Weakness or Loss of Coordination
If you notice sudden weakness in your arm, leg, or one side of the body, or difficulty walking and maintaining balance, this should not be ignored. These symptoms may indicate involvement of critical brain areas and require immediate medical attention.
Confusion or Difficulty Understanding
If you or your family notice sudden confusion, difficulty understanding conversations, or unusual behavior, it is important to seek help without delay. These changes may reflect altered brain function and can worsen if not addressed quickly.
Severe and Persistent Headache
Headaches are common, but a headache that is severe, persistent, and different from your usual pattern should be taken seriously. If it worsens over time, especially when associated with nausea or visual changes, it requires urgent evaluation.
Repeated Vomiting Without Clear Cause
Unexplained vomiting, particularly when it occurs repeatedly and without gastrointestinal illness, may be a sign of increased pressure inside the skull. This is a critical symptom that should prompt immediate medical consultation.
Sudden Personality or Behavioral Changes
Family members are often the first to notice subtle personality changes. Increased irritability, withdrawal, lack of judgment, or unusual emotional responses should not be dismissed as psychological stress alone. These changes may have an underlying neurological cause.
Altered Vision or Visual Disturbances
Blurred vision, double vision, loss of peripheral vision, or difficulty interpreting visual information can indicate involvement of visual pathways in the brain. Sudden onset of these symptoms requires prompt medical evaluation.
Reduced Consciousness or Drowsiness
If you experience unusual drowsiness, difficulty staying awake, or reduced responsiveness, this is a serious warning sign. It may indicate rising intracranial pressure or worsening brain function and requires immediate emergency care.
Final Clinical Guidance
If any of these symptoms appear suddenly or worsen over time, it is important not to wait. Early medical evaluation, including imaging such as MRI or CT scan, can help identify the cause and guide timely treatment. From a clinical perspective, acting early is always safer than delaying care.
Frequently Asked Questions
Can Ayurveda cure glioma completely?
Ayurveda aims not only to control tumor growth but also to restore the body’s internal harmony. In many cases, it helps arrest progression, improve longevity, and prevent relapse. The focus is on rejuvenating the brain tissue (Majja Dhatu), strengthening immunity, and correcting the metabolic imbalance (Agni Dushti) that causes abnormal cell growth. Success depends on the stage, vitality, and consistency of therapy.
Is it safe to combine Ayurvedic herbs with chemotherapy?
Yes, when prescribed correctly under medical supervision, Ayurvedic formulations can safely complement modern treatments. Herbs like Guduchi, Brahmi, and Amalaki protect healthy tissues from radiation and chemotherapy-induced toxicity. They improve liver function, reduce fatigue, and enhance recovery. However, self-medication is not advised; dosages and timing must be personalized.
How long should I continue Ayurvedic therapy?
The duration varies depending on the glioma grade and patient response. For low-grade gliomas, therapy usually continues for six months to a year. In recurrent or high-grade cases, treatment may extend up to two years under close monitoring. Ayurveda emphasizes long-term Rasayana maintenance even after apparent recovery to prevent relapse and restore complete neural balance.
What herbs support memory after brain surgery?
Brahmi (Bacopa monnieri), Shankhapushpi (Convolvulus pluricaulis), and Yashtimadhu (Glycyrrhiza glabra) are excellent memory-enhancing Rasayanas. These herbs nourish brain cells, improve recall, and calm mental restlessness. When taken as Brahmi Vachadi Avaleha or Saraswatarishta, they help patients regain mental sharpness, emotional stability, and sleep quality after surgery.
Can glioma recur, and how does Ayurveda prevent relapse?
Yes, gliomas can recur even after surgery or radiotherapy. Ayurveda prevents relapse by strengthening Ojas (vital energy) and eliminating deep-seated metabolic toxins. Rasayana therapies like Heerak Bhasma Avaleha and Swarna Makshik Avaleha rebuild the body’s defense systems, improve DNA repair, and stabilize the mind. Regular detoxification and diet control help maintain long-term remission.
What should I eat during chemo or radiotherapy?
A light, easily digestible diet is ideal fresh fruits, boiled vegetables, green moong soup, ghee, and warm milk with turmeric. Avoid oily, spicy, and heavy foods that block channels (Srotas). Hydration and small frequent meals maintain energy levels. Ayurveda also recommends Amalaki Rasayana and Ghee for tissue repair and better tolerance to radiotherapy.
Are Panchakarma procedures mandatory?
Panchakarma is optional and chosen based on the patient’s strength and treatment phase. Gentle cleansing like Virechana (purgation) or Nasya (nasal therapy) may be advised before Rasayana therapy to improve absorption. However, it is never forced during weakness, active chemotherapy, or postoperative recovery. The approach is always individualized.
Does stress really worsen brain tumors?
Yes, chronic stress disrupts hormonal balance, suppresses immunity, and increases oxidative damage. This internal imbalance can worsen tumor progression. Ayurveda emphasizes Sattvavajaya Chikitsa mind-strengthening therapies such as meditation, pranayama, counseling, and Brahmi-based Rasayanas to protect the mind and brain from the biological effects of stress.
Can children or elderly patients take Rasayana therapy?
Yes, Rasayana formulations are adaptable to all age groups. Children may receive mild Rasayanas like Brahmi Ghrita or Amalaki Leha for neuroprotection, while elderly patients benefit from Ghrita-based Avalehas that improve strength and cognition. Dosage and composition are always customized based on age, digestion, and vitality.
How soon can one resume work or study after treatment?
Most patients begin light mental activities within two to three months of consistent therapy, depending on surgical recovery and fatigue levels. Ayurvedic rehabilitation strengthens concentration and endurance naturally. With regular Rasayana intake, balanced diet, and adequate rest, patients often return to productive routines without emotional instability or cognitive stress.
About the Author
Medical Review Policy
This article is written and reviewed using peer-reviewed scientific research, international neuro-oncology guidelines, and classical medical literature. Diagnostic and treatment information is aligned with established clinical standards in the United States and United Kingdom. References are provided for transparency and verification.
References
[41] Charaka Samhita, Sutra Sthana, Chapter 18, Verse 44–46. Chaukhamba Sanskrit Sansthan, Varanasi. Discusses Vata–Kapha imbalance and its role in forming firm growths (Arbuda) within deeper tissues.
[63] Bhavaprakasha Nighantu, Rasayana Adhikara, Verse 12–18. Describes Brahmi and Shankhapushpi as Majja Dhatu–nourishing herbs used in mental and neurological disorders.
[72] Singh, H., & Dhiman, K. S. (2016). Evaluation of Brahmi Ghrita and Brahmi Vati in cognitive dysfunction and anxiety disorders. AYU, 37(1), 60–67. https://doi.org/10.4103/ayu.AYU_64_15
[81] Sushruta Samhita, Nidana Sthana, Chapter 11, Verse 12–18. Translated by Kaviraj Ambikadutta Shastri, Chaukhamba Sanskrit Sansthan, 2015. Explains the mechanism of Srotorodha (blockage of channels) as the cause of localized Arbuda formation.
[88] Chattopadhyay, D., et al. (2021). Oxidative stress, inflammation, and the pathogenesis of brain tumors. Frontiers in Oncology, 11, 630–651. https://doi.org/10.3389/fonc.2021.630651
[91] Sanai, N., & Berger, M. S. (2018). Operative techniques for glioma surgery. Neurosurgical Review, 41(1), 9–20. https://doi.org/10.1007/s10143-017-0871-2
[93] Rasatarangini, Taranga 21, Verse 23–29. Pandit Kashinath Shastri, Motilal Banarsidass, 2004. Details preparation of Swarna Makshik Bhasma and its Rasayana effect on metabolic disorders and neuro-degenerative conditions.
[94] Stupp, R., et al. (2009). Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. New England Journal of Medicine, 352(10), 987–996. https://doi.org/10.1056/NEJMoa043330
[95] Hegi, M. E., et al. (2005). MGMT gene silencing and benefit from temozolomide in glioblastoma. New England Journal of Medicine, 352(10), 997–1003. https://doi.org/10.1056/NEJMoa043331
[97] Khanna, P., et al. (2019). Therapeutic potential of Swarna Makshik Bhasma in oxidative stress and mitochondrial dysfunction models. Journal of Ethnopharmacology, 238, 111851. https://doi.org/10.1016/j.jep.2019.111851
[99] Rasa Ratna Samuchchaya, Chapter 12, Verse 3–6. Rasayana Prakarana. Chaukhamba Orientalia, 2012. Discusses Heerak Bhasma as the supreme Rasayana for refractory Arbuda (malignant growths).
[102] Limpeanchob, N., et al. (2008). Neuroprotective effect of Bacopa monnieri on beta-amyloid-induced cell death in primary cortical neurons. Neurochemistry International, 52(1–2), 122–127. https://doi.org/10.1016/j.neuint.2007.04.021
[104] Devi, M., et al. (2020). Role of medicated ghee in drug delivery across the blood–brain barrier. Journal of Ayurveda and Integrative Medicine, 11(2), 172–179. https://doi.org/10.1016/j.jaim.2018.09.005
[107] Kumar, P., & Kumar, A. (2022). Mandoor Bhasma as a bioenhancer in chronic anemia and oxidative stress conditions. AYU, 43(2), 95–102. https://doi.org/10.4103/ayu.AYU_71_22
[108] Li, X., et al. (2020). Iron oxide nanoparticles induce cytotoxicity in glioma cells through ROS-mediated DNA damage. Nanomedicine, 29, 102277. https://doi.org/10.1016/j.nano.2020.102277
[111] Charaka Samhita, Chikitsa Sthana, Rasayana Adhyaya 1/1–30. Chaukhamba Sanskrit Sansthan, 2017. Describes Brahmi Rasayana as a rejuvenator for Majja Dhatu and promoter of long life and cognitive sharpness.
[112] Brown, P. D., et al. (2016). Cognitive outcomes after radiotherapy for low-grade glioma: impact of radiation technique and dose. Journal of Clinical Oncology, 34(15), 1628–1635. https://doi.org/10.1200/JCO.2015.62.2108
[113] Cairncross, J. G., et al. (2013). Chemotherapy for anaplastic oligodendroglioma: long-term results of the RTOG 9402 trial. Journal of Clinical Oncology, 31(3), 337–343. https://doi.org/10.1200/JCO.2012.43.2674
[115] Rasendra Sara Sangraha, Parpati Kalpa, Verse 42–45. Chaukhamba Sanskrit Sansthan, 2013. Elaborates on Mandoor Parpati’s use in blood purification and chronic toxicity relief.
[118] Verma, N., et al. (2021). Post-chemotherapy fatigue and cognitive dysfunction in glioma: mechanisms and rehabilitation. Frontiers in Neuroscience, 15, 650–672. https://doi.org/10.3389/fnins.2021.650672
[119] Cicerone, K. D., et al. (2019). Evidence-based cognitive rehabilitation: updated review. Archives of Physical Medicine and Rehabilitation, 100(8), 1513–1533. https://doi.org/10.1016/j.apmr.2019.02.012
[120] Gilbert, M. R., et al. (2014). Dose-dense temozolomide for newly diagnosed glioblastoma: toxicity and survival outcomes. Journal of Clinical Oncology, 31(32), 4085–4091. https://doi.org/10.1200/JCO.2013.52.6443
[121] Vagbhata, Ashtanga Hridaya, Uttara Tantra, Unmada Chikitsa 7–12. Edited by Hari Sadashiva Shastri Paradkar, Chaukhamba Sanskrit Sansthan, 2018. Describes Kalyanaka Ghrita’s role in pacifying mind and supporting higher cognitive balance.
[122] Duffau, H. (2017). Surgery of low-grade gliomas: towards a functional neurooncology. Nature Reviews Clinical Oncology, 14(8), 436–445. https://doi.org/10.1038/nrclinonc.2017.41
[123] Ballman, K. V. (2015). Anaplastic glioma recurrence patterns and survival outcomes after adjuvant therapy. Neuro-Oncology, 17(8), 1143–1150. https://doi.org/10.1093/neuonc/nov033
[125] Rasa Chintamani, Rasayana Prakarana, Verse 10–15. Reprint edition, Chaukhamba Sanskrit Bhavan, 2011. Details of Rasayana application following Shodhana for Majja-related disorders and malignancy-like conditions.
[127] Baliga, M. S., et al. (2019). Amalaki Rasayana attenuates oxidative DNA damage and enhances neuroprotection. Journal of Traditional and Complementary Medicine, 9(3), 231–240. https://doi.org/10.1016/j.jtcme.2019.03.005
[132] Hervey-Jumper, S. L., et al. (2015). Neurocognitive outcomes after glioma surgery: role of tumor location and resection extent. Journal of Neurosurgery, 122(1), 15–23. https://doi.org/10.3171/2014.10.JNS132085
[133] Prust, M. J., & Chang, S. M. (2018). Radiation and chemotherapy side effects in brain tumor patients. Neuro-Oncology Practice, 5(1), 1–9. https://doi.org/10.1093/nop/npx023
[134] Reardon, D. A., et al. (2017). Immune checkpoint inhibition in glioblastoma: promise and pitfalls. Nature Reviews Clinical Oncology, 14(7), 393–407. https://doi.org/10.1038/nrclinonc.2016.204
[136] Rasatarangini, Taranga 24, Verse 11–14. Chaukhamba Bharati Academy, 2004. Mentions Brahmi Rasayana and Heerak Bhasma in chronic Majja disorders and degenerative diseases.
[138] Singh, N., et al. (2022). Therapeutic potential of Ayurvedic Rasayana herbs in neuro-oncology: a systematic review. Journal of Ayurveda and Integrative Medicine, 13(3), 100588. https://doi.org/10.1016/j.jaim.2022.100588
[139] Chinot, O. L., et al. (2014). Bevacizumab plus radiotherapy–temozolomide for newly diagnosed glioblastoma. New England Journal of Medicine, 370(8), 709–722. https://doi.org/10.1056/NEJMoa1308345
[140] Stupp, R., et al. (2017). Tumor-treating fields plus temozolomide for glioblastoma. JAMA, 318(23), 2306–2316. https://doi.org/10.1001/jama.2017.18718










One Response
Great post. I am facing a couple of these problems.