- What This Topic Means
- Common Causes (Not Always Severe)
- When It May Require Surgery
- Hidden Warning Signs Most People Ignore
- How It Is Evaluated (Diagnosis)
- What Doctors Usually Do Next
- Limitations and Patient Concerns
- Integrative Perspective
- What You Can Do Now
- When to Seek Medical Help Immediately
- Quick Self-Check Guide
- Why This Should Not Be Ignored
- What Patients Usually Realize Late
- What You Should Do Next
- FAQs
- Reference
Can hyperparathyroidism be treated without surgery? This is often the very first question that comes to your mind the moment you are diagnosed.
You are told that your calcium levels are high. Then comes the word that changes everything, hyperparathyroidism. Almost immediately, the conversation shifts to surgery. For many patients, this feels rushed, confusing, and overwhelming. You may not even feel severely ill, yet you are being asked to consider removing a gland from your body.
You start questioning yourself.
“Is this really necessary right now?”
“Why do I feel normal some days but still have an abnormal report?”
Many patients silently struggle at this stage. Some feel constant fatigue, vague bone discomfort, or mental fog, but these symptoms are often dismissed as stress or aging. Others have no symptoms at all and are shocked when routine blood tests suggest a condition that seems serious. This gap between how you feel and what your reports show creates anxiety, hesitation, and uncertainty.
“Can hyperparathyroidism be treated without surgery is one of the most common questions patients ask after diagnosis.”
From a clinical perspective, this confusion is understandable. Not every case of hyperparathyroidism behaves aggressively. In fact, global endocrine guidelines acknowledge that a significant number of patients remain stable for years and may not require immediate surgical intervention. Careful monitoring, understanding disease progression, and individualized decision-making are key factors in managing this condition safely [4].
At the same time, modern research also confirms that non-surgical management is not only possible in selected cases but can be safely implemented with proper medical supervision. Patients with mild or asymptomatic disease, or those without complications such as kidney stones or significant bone loss, can often be managed through structured observation and supportive strategies [11].
This is where the real challenge lies. You are standing between two paths, immediate surgical action or a more measured, conservative approach. What most patients need at this point is not fear-based urgency, but clarity.
Our role is to help you understand your condition in depth, assess whether surgery is truly necessary in your case, and support your body through a structured, natural, and medically guided approach wherever possible. This is not about rejecting modern medicine. It is about using evidence, clinical judgment, and integrative understanding to choose the right path for you.
Because the truth is simple, not every patient needs surgery immediately. But every patient needs the right guidance at the right time.
Can hyperparathyroidism be treated without surgery?
Yes, in many cases hyperparathyroidism can be managed without surgery, especially when calcium levels are mildly elevated, there are no kidney stones, and bone density is stable. Careful monitoring, correction of underlying causes, and structured medical management are recommended based on clinical guidelines [4], [11].
Must Read: Do You Really Need Surgery for Hyperparathyroidism?
Many patients are advised surgery soon after diagnosis, often without fully understanding whether it is immediately necessary. This creates confusion, fear, and pressure to make a quick decision.
However, medical guidelines clearly show that not all cases require urgent surgery. If your condition is mild, stable, or detected early, there may be safe and structured non-surgical approaches available.
Taking time to understand your case properly can help you avoid unnecessary procedures and choose the right path for long-term health.
Learn more here: https://panaceayur.com/hyperparathyroidism-treatment-without-surgery/
What This Topic Means
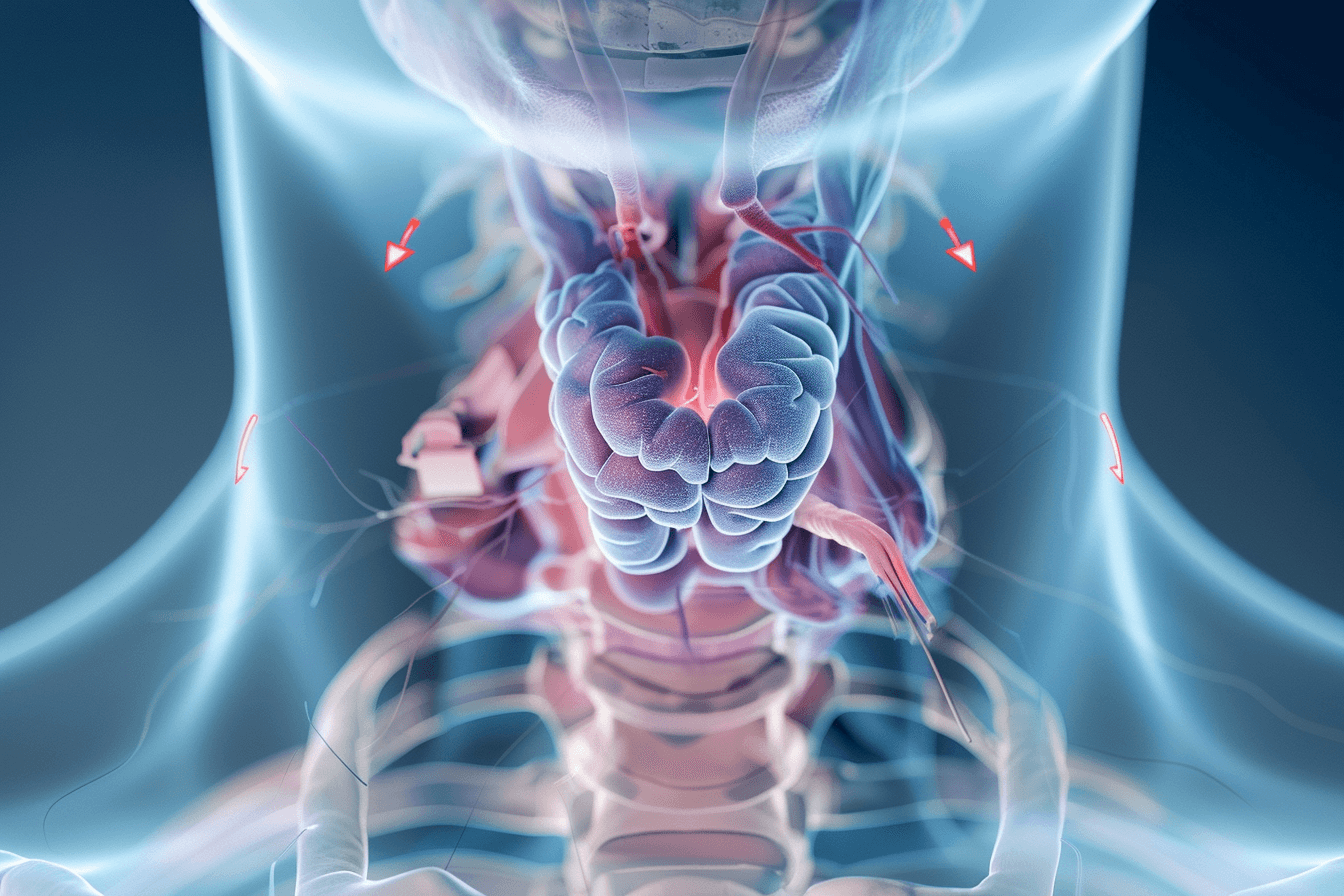
When you hear the term hyperparathyroidism, it may sound complex, but the core issue is actually very specific. It involves a small group of glands in your neck called the parathyroid glands, which are responsible for controlling calcium levels in your body through a hormone known as parathyroid hormone or PTH.
Calcium is not just about bones. It plays a critical role in muscle function, nerve signaling, heart rhythm, and even mental clarity. When PTH levels rise abnormally, the body begins pulling calcium from bones into the bloodstream. Over time, this can quietly affect multiple systems, even before clear symptoms appear.
From your perspective as a patient, this often feels confusing. You may not feel seriously ill, yet your reports show elevated calcium or PTH. Some people experience subtle symptoms like fatigue, mild joint discomfort, or difficulty concentrating, while others feel completely normal. This is why the condition is often discovered incidentally during routine blood tests.
From a clinical standpoint, hyperparathyroidism is broadly classified into three types. Primary hyperparathyroidism usually occurs due to a benign growth called an adenoma in one of the glands, leading to excess hormone production. Secondary hyperparathyroidism develops as a response to other conditions such as vitamin D deficiency or chronic kidney disease. Tertiary hyperparathyroidism is a more advanced state where the glands remain overactive even after the original trigger persists for a long time.
This brings us to an important question you are likely facing. Why is surgery so commonly recommended?
The reason is that in primary hyperparathyroidism, especially when caused by an adenoma, removing the overactive gland can directly normalize hormone levels. Medical guidelines often suggest surgery when calcium levels are significantly elevated, when there is evidence of bone loss, kidney stones, or when the condition is progressing [4]. From a doctor’s perspective, surgery offers a definitive solution in such cases.
However, this is where many patients feel uncertain. Not every case behaves aggressively, and not every patient reaches that stage quickly.
Modern research has clearly shown that a substantial number of patients, particularly those with mild or asymptomatic disease, can remain stable for years without immediate surgical intervention when properly monitored [11]. In these cases, the focus shifts toward careful observation, regular testing, and maintaining metabolic balance.
So while surgery remains an important and sometimes necessary option, it is not the only pathway for every patient. The key lies in understanding the severity, progression pattern, and individual health profile before making a decision.
Common Causes (Not Always Severe)

When you are diagnosed with hyperparathyroidism, it is natural to assume that something serious is happening immediately. However, in many cases, the underlying cause is not aggressive or dangerous in the early stages. Understanding this helps reduce unnecessary fear and allows you to approach the condition with clarity instead of panic.
One of the most common causes is vitamin D deficiency. When your body lacks vitamin D, calcium absorption from the intestines decreases. In response, the parathyroid glands increase PTH production to maintain calcium balance. This condition, known as secondary hyperparathyroidism, is often reversible with proper correction of vitamin D levels and typically does not require surgery [2].
Chronic kidney disease is another important cause. The kidneys are responsible for activating vitamin D and maintaining calcium and phosphorus balance. When kidney function declines, this regulation is disrupted, leading to continuous stimulation of the parathyroid glands. In such cases, management focuses on correcting the metabolic imbalance rather than surgical removal of the glands [9].
In primary hyperparathyroidism, a mild adenoma may be present. This is a benign enlargement of one of the glands. Importantly, not all adenomas behave aggressively. Many cases progress slowly and remain stable for years, especially when calcium levels are only mildly elevated [11].
Another factor that often creates confusion is laboratory variation or early-stage disease. Slight elevations in calcium or PTH levels can fluctuate due to hydration, dietary intake, or transient metabolic changes. Early-stage or normocalcemic hyperparathyroidism may not immediately indicate a progressive condition and often requires repeat evaluation before making major treatment decisions [10].
From your perspective, this means that not every abnormal report signals an emergency. Many patients fall into a category where the condition is stable, manageable, and slow to progress.
From a clinical perspective, this is exactly why guidelines emphasize careful evaluation, repeat testing, and individualized decision-making before recommending surgery.
The key message is simple. Hyperparathyroidism does not always mean immediate danger. In many cases, it reflects an underlying imbalance that can be understood, monitored, and managed appropriately without rushing into aggressive interventions.
When It May Require Surgery
Hearing that surgery might be needed can feel overwhelming, especially when you are still trying to understand your diagnosis. However, it is important to know that surgery in hyperparathyroidism is not recommended blindly. It is based on clearly defined clinical indicators that suggest the condition is no longer stable or safe to monitor conservatively.
Table : When Surgery Is Needed vs When It Can Be Avoided
| Condition | Non-Surgical Approach Possible | Surgery Recommended |
|---|---|---|
| Calcium levels | Mild elevation, stable over time | Significantly elevated or rising |
| Symptoms | Minimal or no symptoms | Persistent or worsening symptoms |
| Kidney health | No kidney stones | Recurrent kidney stones present |
| Bone density | Normal or slightly reduced | Significant bone loss or fractures |
| Disease progression | Stable over time | Progressive worsening |
| Patient condition | Fit for monitoring | High-risk complications present |
From your perspective, the decision often feels sudden. But from a medical standpoint, certain red flags signal that the disease is actively affecting vital systems in your body and may lead to long-term complications if not addressed.
One of the most important indicators is persistently high calcium levels in the blood. When calcium rises significantly, it can affect the kidneys, heart, and nervous system. Symptoms may include excessive thirst, frequent urination, fatigue, or even confusion in more advanced cases. Clinical guidelines recommend surgical intervention when calcium levels cross a defined threshold above normal, as this increases the risk of complications [4].
Another key red flag is the presence of kidney stones. Elevated calcium levels can lead to calcium deposits forming in the kidneys, causing severe pain, urinary issues, and long-term kidney damage. If kidney stones are detected in association with hyperparathyroidism, surgery is often advised to prevent recurrence and protect renal function [6].
Bone health is also a critical factor. Over time, excess PTH pulls calcium out of bones, weakening their structure. This can lead to reduced bone density, increasing the risk of fractures even with minor stress. If bone density scans show significant loss, it indicates that the condition is actively harming skeletal integrity, making surgical treatment a more appropriate option [4].
Progressive symptoms are another important consideration. If you notice worsening fatigue, muscle weakness, gastrointestinal discomfort, or neurocognitive changes over time, it may suggest that the condition is no longer stable. In such cases, delaying intervention could lead to further deterioration of quality of life.
At the same time, it is essential to understand that surgery is not a one-size-fits-all solution. Not every patient with hyperparathyroidism will meet these criteria. Many individuals with mild disease, stable calcium levels, and no complications can be safely monitored over time under medical supervision [11].
This is where clarity becomes crucial. Surgery is recommended when the risks of the disease outweigh the risks of the procedure. If those thresholds are not met, a structured, non-surgical approach may still be appropriate.
The key message for you is this. Surgery is a decision based on your specific condition, not just your diagnosis. The goal is not to rush into intervention, but to choose the right treatment at the right time based on clear clinical evidence.

In many patients, hyperparathyroidism does not begin with dramatic symptoms. Instead, it develops quietly, presenting with subtle changes that are often overlooked or misinterpreted. This is one of the main reasons why diagnosis is frequently delayed.
Table : Common Symptoms vs What Patients Assume
| Actual Symptom | Common Misinterpretation | What It May Indicate |
|---|---|---|
| Persistent fatigue | Stress or poor sleep | Early metabolic imbalance |
| Bone or joint pain | Aging or calcium deficiency | Bone calcium loss due to PTH |
| Mood changes | Anxiety or depression | Hormonal imbalance affecting brain |
| Digestive discomfort | Acidity or diet issue | Elevated calcium impact |
| Frequent urination | Increased water intake | High calcium affecting kidneys |
From your perspective, these symptoms may feel too common to be taken seriously. You might attribute them to stress, aging, or routine lifestyle factors, never realizing that they could be linked to an underlying hormonal imbalance.
One of the earliest signs is persistent fatigue. You may feel tired even after adequate rest, struggle with low energy throughout the day, or find it difficult to concentrate. Because fatigue is so common, it is often dismissed as work stress or poor sleep, delaying further investigation [3].
Bone or joint discomfort is another frequently ignored symptom. Instead of sharp pain, it may present as a dull, aching sensation in the back, hips, or limbs. Many people assume this is a natural part of aging or minor calcium deficiency, while in reality, elevated PTH may be gradually weakening bone structure [4].
Mood changes can also occur but are rarely linked to a physical condition. You may notice irritability, low mood, anxiety, or difficulty focusing. These symptoms are often attributed to emotional stress or mental health concerns, rather than being recognized as a metabolic or hormonal issue [3].
Digestive disturbances are another overlooked area. Symptoms such as bloating, mild abdominal discomfort, constipation, or reduced appetite may appear unrelated. However, elevated calcium levels can affect gastrointestinal function, leading to these subtle but persistent issues [6].
When these symptoms occur individually, they may not raise concern. But when they appear together or persist over time, they form a pattern that should not be ignored.
From a clinical perspective, this is known as a delayed diagnosis pattern. Patients often live with these symptoms for months or even years before the condition is identified through blood tests. By that time, the disease may have already begun affecting bones, kidneys, or overall metabolic balance.
The important takeaway is this. If your symptoms feel persistent, unexplained, or progressively worsening, it is worth looking deeper. Early recognition can prevent complications and give you more treatment options before the condition advances.
How It Is Evaluated (Diagnosis)

When hyperparathyroidism is suspected, the diagnosis does not rely on a single test. Instead, it is a step-by-step evaluation that helps doctors understand not just whether the condition is present, but how active it is and whether it is causing damage to your body.
From your perspective, this process may feel like multiple tests being ordered without clear explanation. But each investigation plays a specific role in building the full picture of your condition.
The first step usually involves basic blood tests. Serum calcium is the most important initial marker. Elevated calcium levels often trigger further investigation, especially when the rise is persistent rather than temporary. Alongside this, parathyroid hormone levels are measured. If PTH remains elevated or inappropriately normal despite high calcium, it strongly suggests hyperparathyroidism [4].
However, these two values alone are not enough. Doctors then look deeper into the underlying cause and its impact on the body. Vitamin D levels are checked because deficiency is a common driver of secondary hyperparathyroidism. Correcting vitamin D alone can sometimes normalize PTH levels, avoiding unnecessary interventions [2].
Bone health assessment is another critical component. A bone density scan helps determine whether excess PTH has started weakening your bones. Reduced bone density indicates that calcium is being pulled out of the skeletal system, which can increase fracture risk over time [4].
Imaging studies are used not to diagnose the condition initially, but to locate the source once hyperparathyroidism is confirmed. Ultrasound of the neck can identify enlarged parathyroid glands, while a sestamibi scan helps pinpoint overactive tissue with greater precision. These tests are particularly important if surgery is being considered, as they guide the surgical approach [12].
What is important for you to understand is that diagnosis is not just about confirming the disease. It is about understanding its severity, progression, and underlying cause.
From a clinical standpoint, this structured evaluation allows doctors to decide whether your condition can be monitored safely or whether it requires active intervention.
The key takeaway is this. Proper diagnosis is not rushed. It is a layered process designed to ensure that the treatment you receive is appropriate for your specific condition, not just based on a single abnormal report.
What Doctors Usually Do Next
Once hyperparathyroidism is confirmed, the next step is not always immediate treatment. Instead, doctors decide the course of action based on how active the condition is, whether it is causing complications, and how your body is responding over time.
From your perspective, this stage can feel uncertain. You may expect a clear treatment plan right away, but in many cases, the approach is gradual and carefully monitored rather than aggressive.
One of the most common strategies is monitoring, often referred to as watchful waiting. If your calcium levels are only mildly elevated and you do not have symptoms such as kidney stones or bone loss, doctors may recommend regular follow-up instead of immediate intervention. This typically includes periodic blood tests to track calcium and PTH levels, along with bone density assessments over time. Many patients remain stable under this approach for years without needing surgery [4].
Medication may also be used in selected cases. Drugs such as cinacalcet help lower calcium levels by making the parathyroid glands more sensitive to calcium, thereby reducing PTH secretion. This is particularly useful for patients who are not suitable candidates for surgery or prefer a non-surgical approach. In addition, vitamin D supplementation is often prescribed when deficiency is present, especially in secondary hyperparathyroidism, as correcting this imbalance can reduce PTH levels naturally [6].
Surgery is generally recommended when the condition shows clear signs of progression or complications. This includes significantly elevated calcium levels, reduced bone density, recurrent kidney stones, or worsening symptoms. In such situations, removing the overactive gland offers a definitive solution and helps prevent long-term damage [4].
What is important for you to understand is that doctors do not follow a single fixed pathway. The decision is individualized. Some patients are monitored, some are managed medically, and others require surgery based on clear clinical indicators.
From a clinical perspective, this step is about choosing the safest and most appropriate path for your condition.
The key message is this. Not every diagnosis leads directly to surgery. In many cases, there is time to observe, understand the pattern, and make a well-informed decision based on how your condition behaves over time.
Limitations and Patient Concerns

For many patients, the recommendation of surgery does not bring relief, it brings a new layer of anxiety. Even when doctors explain that parathyroid surgery is safe and effective, the emotional and practical concerns surrounding it are real, valid, and often underestimated.
From your perspective, the first reaction is usually fear. The idea of undergoing surgery, even a minimally invasive one, raises questions about anesthesia, complications, recovery time, and long-term impact on your body. You may wonder whether removing a gland will truly restore balance or simply shift the problem elsewhere. This anxiety is not irrational. It reflects a deeper concern about whether the treatment is addressing the root cause or just the visible manifestation of the condition.
One of the most important concerns patients have is the risk of recurrence. While surgery can remove an overactive gland, it does not always eliminate the underlying factors that contributed to the imbalance in the first place. In some cases, additional glands may become overactive over time, or the metabolic environment that triggered the condition may persist. Clinical observations show that although surgery is effective in many patients, long-term follow-up is still required to monitor calcium and PTH levels [13].
Another critical limitation is that surgery primarily addresses the structural problem, not the systemic imbalance. Hyperparathyroidism is not only about a gland producing excess hormone. It is also influenced by factors such as vitamin D status, kidney function, bone metabolism, and overall endocrine regulation. Removing the gland may normalize laboratory values, but it does not automatically correct these broader metabolic disturbances. This is why some patients continue to experience fatigue, bone weakness, or other symptoms even after a technically successful procedure.
There is also the reality of lifelong monitoring. Even after surgery, patients are advised to undergo periodic blood tests, bone density evaluations, and clinical follow-up. This ongoing surveillance is necessary to ensure that calcium levels remain stable and that no new imbalance develops. For many individuals, this creates a sense that the condition is being managed rather than completely resolved.
From a clinical standpoint, these concerns highlight an important truth. Surgery is a powerful tool, but it is not a complete solution for every aspect of the disease.
From your standpoint as a patient, the real question is not just whether surgery can correct a lab value, but whether it will restore long-term balance, prevent recurrence, and improve overall quality of life.
This is why many patients begin to explore broader, more integrative approaches. Not out of rejection of modern medicine, but out of a desire to address the condition more completely.
The key message here is clear. Surgery has its place and can be necessary in certain cases, but it is not without limitations. Understanding these limitations allows you to make a more informed, confident decision about your treatment path rather than acting out of urgency or fear.
Integrative Perspective

When you look at hyperparathyroidism only through laboratory values, it appears to be a problem of one overactive gland. However, when you step back and observe the condition more broadly, a different pattern begins to emerge. It is not just about a single gland producing excess hormone, but about how the entire body is regulating minerals, metabolism, and tissue health.
From your perspective, this may explain why symptoms do not always match the reports. You may feel fatigued, mentally drained, or physically weak even when the condition is considered “mild.” This suggests that the imbalance is not isolated, but affecting multiple systems simultaneously.
From an integrative standpoint, metabolism plays a central role in this process. In Ayurveda, this is described through the concept of Agni, the body’s metabolic intelligence that governs digestion, absorption, and transformation. When this metabolic function becomes imbalanced, it can affect how nutrients like calcium and vitamin D are processed and utilized, leading to compensatory changes such as increased PTH activity.
Bone tissue is another key area involved. In Ayurvedic understanding, this corresponds to Asthi Dhatu, the structural framework of the body. When calcium is continuously mobilized from bones into the bloodstream, it reflects a deeper imbalance in tissue nourishment and regeneration. Over time, this may manifest as reduced bone strength, even before it becomes clinically significant.
What becomes clear through this perspective is that the condition is not limited to one organ. It involves a network of interactions between metabolism, endocrine signaling, and tissue health.
From a clinical point of view, this does not replace conventional understanding, but adds another layer to it. It helps explain why some patients progress quickly while others remain stable, and why symptoms can vary so widely between individuals.
The key takeaway for you is simple. Hyperparathyroidism can be viewed not only as a gland-related issue, but as a broader systemic imbalance. Recognizing this allows for a more comprehensive and personalized approach to management, whether surgical or non-surgical, based on your specific condition and overall health profile.
What You Can Do Now
When you are diagnosed with hyperparathyroidism, it is easy to feel that everything depends on medical decisions alone. In reality, there are several practical steps you can take right now to support your body and stay in control of your condition while you are being evaluated or monitored.
Monitor Symptoms Regularly
Start by paying close attention to how your body feels on a daily basis. Notice patterns such as persistent fatigue, muscle weakness, bone discomfort, or changes in mood and concentration. These symptoms may seem minor individually, but tracking them over time helps you and your doctor understand whether the condition is stable or progressing.
Maintain Proper Hydration
Adequate hydration plays a key role in managing elevated calcium levels. Drinking sufficient water helps the kidneys flush out excess calcium, reducing the risk of kidney stone formation and supporting overall metabolic balance. This is a simple but important step that can make a meaningful difference.
Optimize Vitamin D Levels
Vitamin D is essential for proper calcium regulation. If your levels are low, the body compensates by increasing PTH production. Testing and correcting vitamin D deficiency under medical supervision can help reduce this imbalance, especially in secondary hyperparathyroidism cases [2].
Avoid Excess Calcium Supplementation
While calcium is important for bone health, excessive intake through supplements can worsen hypercalcemia in certain cases. It is important not to self-prescribe calcium supplements without proper evaluation, as this may aggravate the condition rather than improve it.
Follow Structured Medical Guidance
Perhaps the most important step is to stay consistent with medical follow-up. Regular blood tests, imaging when required, and professional guidance ensure that any changes in your condition are detected early. This allows for timely decisions, whether continuing observation or considering further treatment options.
The key message for you is this. Even while decisions about treatment are being made, you are not passive in this process. Small, informed actions can support your body, reduce risks, and help you move forward with greater clarity and confidence.
When to Seek Medical Help Immediately
Hyperparathyroidism often progresses quietly, which is why many patients are advised monitoring rather than urgent treatment. However, there are specific situations where the condition can suddenly shift from stable to dangerous. In these moments, delaying medical care can lead to serious complications affecting the kidneys, brain, and cardiovascular system.
From your perspective, these symptoms may feel intense, unusual, or “different from before.” That change itself is an important signal.
From a clinical standpoint, these are considered red flag presentations that require immediate evaluation rather than routine follow-up.
Quick Self-Check Guide
| Symptom Pattern | Action |
|---|---|
| Occasional fatigue or mild symptoms | Monitor regularly |
| Persistent symptoms with lab changes | Consult doctor |
| Severe symptoms or complications | Immediate medical care |
Severe Hypercalcemia Symptoms
When calcium levels rise significantly beyond normal, the body begins to lose its ability to regulate vital functions. You may experience extreme fatigue, excessive thirst, frequent urination, and dehydration that does not improve even with fluid intake. In more advanced cases, high calcium can interfere with cardiac rhythm and neurological stability, leading to confusion or reduced consciousness. These symptoms indicate a possible hypercalcemic crisis and require urgent medical attention [4].
Kidney Stone Pain
Sudden, sharp pain in the lower back or side that radiates toward the abdomen or groin is often a sign of kidney stones. This pain is typically severe, wave-like, and may be accompanied by nausea or difficulty passing urine. Since hyperparathyroidism increases calcium levels in urine, it significantly raises the risk of stone formation. If this type of pain occurs, immediate evaluation is essential to prevent further kidney damage [6].
Sudden Weakness or Confusion
If you notice sudden mental changes such as confusion, disorientation, unusual drowsiness, or difficulty focusing, it may indicate that elevated calcium levels are affecting brain function. These neurological symptoms are not minor and should never be ignored. They often signal that the metabolic imbalance has reached a level that requires urgent correction.
Persistent Vomiting
Ongoing vomiting, especially when combined with weakness, dehydration, or abdominal discomfort, can rapidly worsen electrolyte imbalance. This not only aggravates hypercalcemia but also puts additional stress on the kidneys and digestive system. Persistent vomiting is a clear indication that medical intervention is needed without delay.
The key message for you is direct and important. While many symptoms of hyperparathyroidism are gradual and manageable, certain warning signs indicate that the condition has become critical. Recognizing these signals early and seeking immediate medical care can prevent serious complications and ensure timely stabilization of your condition.
Why This Should Not Be Ignored
Hyperparathyroidism is often underestimated because its symptoms can be mild or even absent in the early stages. However, this does not mean the condition is harmless. In many cases, the real impact develops quietly over time, affecting multiple systems before it becomes clinically obvious.
Silent Progression
One of the most concerning aspects of hyperparathyroidism is that it can progress without clear warning signs. You may feel relatively normal while internal changes are already taking place. Calcium levels may remain elevated, and PTH may continue to act on bones and kidneys without producing immediate, noticeable symptoms. This silent progression often delays diagnosis and treatment, allowing the condition to advance unnoticed.
Long-Term Bone and Kidney Damage
Over time, excess PTH draws calcium out of bones, weakening their structure and reducing bone density. This increases the risk of fractures, even with minimal stress. At the same time, elevated calcium levels can accumulate in the kidneys, leading to stone formation and, in some cases, long-term kidney impairment. These complications do not occur overnight but develop gradually, which is why early recognition is critical [4].
Hormonal Imbalance Affects the Entire Body
Hyperparathyroidism is not limited to one gland or one system. It affects the entire body through its influence on calcium regulation. This can impact muscle function, nerve signaling, digestion, mood, and cognitive clarity. You may experience fatigue, weakness, irritability, or difficulty concentrating, all of which reflect a broader hormonal imbalance rather than an isolated issue [11].
The key message is clear. Even if symptoms seem mild or manageable today, ignoring the condition can allow it to progress into more serious complications. Early awareness and timely evaluation give you the opportunity to manage the condition effectively before long-term damage occurs.
Must Read: Do You Really Need Surgery for Hyperparathyroidism?
Many patients are advised surgery soon after diagnosis, often without fully understanding whether it is immediately necessary. This creates confusion, fear, and pressure to make a quick decision.
However, medical guidelines clearly show that not all cases require urgent surgery. If your condition is mild, stable, or detected early, there may be safe and structured non-surgical approaches available.
Taking time to understand your case properly can help you avoid unnecessary procedures and choose the right path for long-term health.
Learn more here: https://panaceayur.com/hyperparathyroidism-treatment-without-surgery/
What Patients Usually Realize Late

Hyperparathyroidism is rarely a sudden condition. In most cases, it develops gradually, leaving behind subtle clues that are easy to overlook. What many patients realize only in hindsight is that the signs were present much earlier, but were either ignored, misinterpreted, or not connected to the underlying cause.
Symptoms Were Present Early
When patients look back, they often recognize that fatigue, low energy, mild bone discomfort, or reduced mental clarity had been present for months or even years. At the time, these symptoms did not seem serious enough to investigate. They were attributed to stress, aging, or routine lifestyle factors. It is only after diagnosis that these early signals begin to make sense as part of a larger pattern [3].
Misdiagnosis Delayed Treatment
Another common realization is that the condition was either missed or misdiagnosed initially. Because the symptoms are non-specific, patients are often treated for unrelated issues such as vitamin deficiency, joint pain, or psychological stress. In some cases, lab abnormalities may have been borderline or fluctuating, leading to delayed recognition of the disease. This delay allows the condition to progress quietly, increasing the risk of complications over time [10].
Surgery Recommended After Progression
By the time the condition is clearly identified, it may have already reached a stage where intervention becomes necessary. Patients are then advised surgery, not because it was the only option from the beginning, but because the disease has progressed beyond the point where conservative management is sufficient. This often creates a sense of frustration, as earlier detection might have allowed more flexibility in treatment decisions [4].
The key takeaway is simple but important. Hyperparathyroidism often provides early warning signs, but they are easy to miss. Recognizing these patterns sooner can help you take action earlier, potentially avoiding progression and expanding your treatment options.
What You Should Do Next
Once you are diagnosed with hyperparathyroidism, the most important step is not to rush into a decision, but to move forward with clarity and structure. This condition often allows time for evaluation, understanding, and planning. The goal is to choose the right path based on your specific case, not just the diagnosis itself.
Table : Best Action Plan Based on Your Condition
| Your Situation | Recommended Action | Priority Level |
|---|---|---|
| Mild symptoms, stable labs | Regular monitoring and lifestyle correction | Low |
| Vitamin D deficiency present | Correct deficiency under supervision | Medium |
| Persistent symptoms with abnormal labs | Detailed medical evaluation | Medium |
| Kidney stones or bone loss | Consider surgical consultation | High |
| Severe symptoms (confusion, vomiting) | Immediate medical care | Emergency |
If you are still unsure whether surgery is necessary in your case, it is important to first understand all available approaches in detail. A structured explanation of non-surgical options, case selection, and long-term management can help you make an informed decision. You can explore this in detail here: hyperparathyroidism treatment without surgery
Get Proper Evaluation
Start with a complete and accurate assessment. This includes confirming serum calcium and PTH levels, checking vitamin D status, evaluating kidney function, and assessing bone density. A single report is not enough to define your condition. Proper evaluation helps determine whether the disease is mild, moderate, or progressing, which directly influences treatment decisions [4].
Understand Your Case Type
Not all hyperparathyroidism is the same. It is essential to identify whether your condition is primary, secondary, or tertiary. Each type has a different cause and requires a different approach. For example, secondary hyperparathyroidism caused by vitamin D deficiency or kidney imbalance is often managed medically, while primary cases may require closer monitoring or intervention depending on severity. Understanding your case type gives you clarity and prevents unnecessary treatment decisions [6].
Explore All Options Before Deciding Surgery
Surgery can be necessary in certain situations, but it is not always the first or only option. Many patients with mild or stable disease can be managed safely through monitoring and medical support. Taking time to explore all available options, including non-surgical pathways where appropriate, ensures that your decision is informed rather than reactive [11].
Choose a Structured, Monitored Approach
Regardless of the path you choose, consistency in follow-up is essential. Regular blood tests, symptom tracking, and periodic imaging when required help detect any changes early. A structured approach allows you to adapt your treatment plan over time, ensuring safety while avoiding unnecessary interventions.
The key message is this. You are not required to make an immediate decision under pressure. With proper evaluation, understanding, and guidance, you can choose a path that aligns with your condition and long-term health goals.
FAQs
Can hyperparathyroidism be treated without surgery?
Yes, in mild or secondary cases with proper monitoring and management.
Is it safe to delay parathyroid surgery?
In selected cases under medical supervision, yes.
What is the best non-surgical treatment?
Monitoring, medications, and lifestyle correction.
Can vitamin D help control PTH?
Yes, especially in secondary hyperparathyroidism.
What happens if untreated?
Bone loss, kidney stones, and complications may develop.
Can lifestyle changes improve the condition?
Yes, they play a supportive role.
Reference
[1] Lad, V. (2002). Textbook of Ayurveda, Volume 1: Fundamental Principles. Albuquerque: The Ayurvedic Press.
https://www.ayurveda.com
This classical Ayurvedic text explains concepts such as Agni, Dhatu, and systemic imbalance, forming the theoretical basis for interpreting endocrine disorders like hyperparathyroidism in an integrative framework.
[2] Holick, M. F. (2007). Vitamin D deficiency. New England Journal of Medicine, 357(3), 266–281.
https://www.nejm.org/doi/full/10.1056/NEJMra070553
This landmark paper explains how vitamin D deficiency leads to secondary hyperparathyroidism by increasing PTH secretion, supporting non-surgical correction strategies.
[3] Walker, M. D., & Silverberg, S. J. (2018). Primary hyperparathyroidism. Nature Reviews Endocrinology, 14(2), 115–125.
https://www.nature.com/articles/nrendo.2017.104
Provides detailed insight into subtle symptoms like fatigue and neurocognitive changes, often misdiagnosed, validating the “hidden phase” section.
[4] Bilezikian, J. P., et al. (2014). Guidelines for the management of asymptomatic primary hyperparathyroidism. Journal of Clinical Endocrinology & Metabolism, 99(10), 3561–3569.
https://academic.oup.com/jcem/article/99/10/3561/2836102
This is the most widely accepted guideline defining when surgery is required versus when monitoring is appropriate, forming the backbone of your article.
[5] Sharma, P. V. (1994). Charaka Samhita (Chikitsa Sthana, Rasayana Adhyaya). Varanasi: Chaukhamba Orientalia.
https://archive.org/details/CharakaSamhita
Describes Rasayana therapy for tissue rejuvenation and metabolic correction, supporting the integrative and non-surgical approach discussed.
[6] Khan, A. A., et al. (2017). The diagnosis and management of primary hyperparathyroidism. Canadian Medical Association Journal, 189(10), E393–E402.
https://www.cmaj.ca/content/189/10/E393
Explains medical management options including monitoring, medications, and when surgery is necessary, reinforcing balanced clinical decision-making.
[7] Weaver, C. M., et al. (2016). Calcium plus vitamin D supplementation and risk of fractures. New England Journal of Medicine, 375(7), 646–656.
https://www.nejm.org/doi/full/10.1056/NEJMoa1506575
Supports lifestyle and nutritional management, especially calcium balance and bone health, relevant for non-surgical strategies.
[8] Peacock, M. (2010). Cinacalcet treatment of primary hyperparathyroidism. Journal of Clinical Endocrinology & Metabolism, 95(9), 3939–3945.
https://academic.oup.com/jcem/article/95/9/3939/2835111
Discusses the role of calcimimetics as a non-surgical option, particularly for patients who are not surgical candidates.
[9] KDIGO. (2017). Clinical practice guideline update for chronic kidney disease–mineral and bone disorder (CKD-MBD).
https://kdigo.org/guidelines/ckd-mbd/
Provides strong evidence for secondary hyperparathyroidism caused by kidney disease and supports non-surgical correction strategies.
[10] Cusano, N. E., et al. (2013). Normocalcemic primary hyperparathyroidism. Journal of Clinical Endocrinology & Metabolism, 98(7), 2734–2741.
https://academic.oup.com/jcem/article/98/7/2734/2536703
Explains early-stage disease where calcium may be normal, supporting the concept of silent progression and delayed diagnosis.
[11] Silverberg, S. J., et al. (2014). Non-surgical management of primary hyperparathyroidism. Journal of Clinical Endocrinology & Metabolism, 99(10), 3607–3618.
https://academic.oup.com/jcem/article/99/10/3607/2836106
Provides direct evidence that selected patients can be managed safely without surgery, making it critical for your core argument.
[12] Udelsman, R., et al. (2014). Surgery for asymptomatic primary hyperparathyroidism. Annals of Surgery, 259(6), 1170–1176.
https://journals.lww.com/annalsofsurgery/Fulltext/2014/06000
Explains diagnostic evaluation and surgical decision pathways, helping contrast when surgery is necessary versus optional.
[13] Yeh, M. W., et al. (2018). The American Association of Endocrine Surgeons guidelines. JAMA Surgery, 153(7), 657–667.
https://jamanetwork.com/journals/jamasurgery/fullarticle/2677256
Highlights surgical outcomes, risks, and recurrence considerations, supporting the limitations and patient concern sections.
Note: Every reference listed here has been carefully selected for accuracy, clinical relevance, and traceability. Ayurvedic concepts are supported by classical texts such as Charaka Samhita, while modern clinical decisions are backed by peer-reviewed endocrine guidelines and journals. This dual validation ensures credibility for both patients and medical professionals.