- What’s Missing in Standard Care?
- When Standard Lung Cancer Treatment Stops Working
- How Integrative Oncology Supports Patients When Standard Treatment Reaches Its Limit
- Who Is the Ideal Candidate for an Integrative Approach in Lung Cancer
- What Makes This Integrative Approach Different From General Supportive Care
- A Personalised Integrative Evaluation for Lung Cancer Patients
- Common Disorders Associated With Lung Cancer
- Rare but Clinically Significant Disorders Associated With Lung Cancer
- Treatment-Related Associated Disorders
- Systemic Functional Disorders Seen in Long-Standing Disease
- Ayurvedic correlation of disorders associated with lung cancer
- Rare but clinically significant correlations
- Treatment related conditions
- Systemic functional disorders
- Clinical significance
- Holistic Approach to Cancer Care
- Herbal Therapies In Lung Cancer Care
- Ayurvedic View of Lung Cancer
- Ayurvedic Treatment for Lung Cancer
- Key Ayurvedic Formulations Lung Cancer
- Herbs & Minerals with Scientific Validation
- Post-Treatment Regeneration
- Strengthening the Immune Terrain
- Why Ayurveda Focuses on Terrain, Not Just Tumor Destruction
- Agastya Haritaki Avaleha Main Medicine For Recovery – Classical Respiratory Rasayana
- Classical Reference and Meaning for Patients
- Classical Ingredient Composition with Approximate Weight
- Highly Potent Mineral Rasayana (Added Only After Assessment)
- Dosage and Duration
- How It Works in the Body
- Why the Ingredients Change in Every Patient
- Important Warning – Do Not Buy Agastya Haritaki Avaleha From the Market for Therapeutic Use
- Absence of Yukti-Based Individualisation
- Disease Stage Mismatch
- Digestive Capacity Is Not Assessed
- No Stage-Specific Mineral Rasayana Integration
- Improper Classical Processing in Commercial Preparations
- Incompatibility With Ongoing Modern Treatment
- Patient Factors That Decide Whether the Avaleha Will Work
- Warning Against Self-Preparation
- Mandatory Medical Supervision
- Timing Matters in Personalized Oncology Support
- Why One Formula Doesn’t Fit All in Ayurvedic Oncology
- Common reasons lung cancer patients explore integrative treatment:
- FAQs (Frequently Asked Questions)
- References
Lung cancer alternative treatment is no longer a rare search. Across the world, patients with advanced or treatment-resistant disease are actively looking beyond chemotherapy and radiation when survival, strength, and quality of life begin to decline. This shift is not driven by misinformation. It is driven by real clinical challenges such as recurrence, drug resistance, severe side effects, and the need for a more personalised and human-centred approach to cancer care.
Lung cancer remains one of the most common and serious cancers worldwide. While conventional treatments such as surgery, chemotherapy, radiation therapy, targeted therapy, and immunotherapy have improved survival rates in many cases, they are often associated with significant challenges. These treatments can lead to serious side effects, including fatigue, nausea, weakened immunity, digestive problems, nerve damage, and other complications that reduce the patient’s quality of life. As a result, many individuals diagnosed with lung cancer begin to explore alternative or complementary therapies as part of their treatment journey.
The growing interest in alternative medicine is driven by several key factors. One of the most common reasons patients seek alternatives is to manage the side effects of conventional cancer treatments. Chemotherapy and radiation are powerful interventions aimed at killing cancer cells, but they can also harm healthy cells, leading to a wide range of unpleasant symptoms. Patients may experience extreme tiredness, difficulty eating, infections, and nerve pain, among other issues. Alternative therapies such as herbal medicine, acupuncture, and nutrition-based interventions are sometimes used alongside standard treatment to help reduce these side effects and improve comfort.
Another reason patients explore alternative medicine is the desire to strengthen their immune system during and after cancer treatment. Research has shown that a well-functioning immune system plays a critical role in detecting and controlling abnormal cells, including cancer. Unfortunately, many conventional treatments can weaken immune function, leaving the body more vulnerable. Patients are often interested in therapies that claim to support immune health, such as certain herbal remedies, dietary supplements, or stress-reducing practices. While not all alternative therapies have been proven effective in this regard, the appeal of boosting natural defenses is a significant motivator for many people.
In addition to managing side effects and supporting immunity, many patients are drawn to alternative medicine because it offers a more holistic approach to health. Conventional treatment tends to focus narrowly on eliminating the tumor, while alternative medicine emphasizes restoring balance throughout the entire body. This includes improving digestion, reducing inflammation, supporting detoxification, and promoting mental and emotional well-being. Some patients feel that their overall health and quality of life are better addressed through this whole-person approach, which may integrate physical, emotional, and lifestyle factors into the healing process.
For some individuals, the preference for alternative therapies is rooted in the perception that natural treatments are less toxic or gentler on the body. While it’s important to note that “natural” does not automatically mean safer or more effective, many patients are attracted to therapies derived from plants or traditional medical systems, believing they may cause fewer harmful effects than synthetic drugs. This belief leads some patients to prioritize herbal medicine, dietary changes, or non-invasive therapies as part of their care plan.
Another significant reason patients seek alternative therapies is the hope of preventing cancer recurrence after completing standard treatment. Even after a successful response to chemotherapy or surgery, the fear of cancer returning can be overwhelming. Some individuals turn to alternative medicine to help maintain their health, reduce inflammation, and support detoxification processes they believe may reduce the risk of recurrence. While research on the effectiveness of such strategies is still ongoing, the desire to actively participate in post-treatment health maintenance is a powerful motivator.
Cultural and personal beliefs also play a role in the decision to pursue alternative medicine. In many parts of the world, traditional medical systems like Ayurveda, Traditional Chinese Medicine, or naturopathy are well-established and trusted. Patients from these backgrounds may naturally turn to familiar therapies, either as a complement to Western medicine or as an independent approach. Even among patients without a cultural connection to alternative medicine, many individuals seek greater control over their treatment journey, feeling empowered by the ability to make choices that align with their values and preferences.
It is important to emphasize that alternative therapies should not replace standard cancer treatments without careful medical supervision. While some alternative approaches can be safely integrated with conventional care, others may interact negatively with chemotherapy, radiation, or targeted therapies. Patients are strongly encouraged to discuss any alternative treatments with their oncology team to avoid harmful interactions and ensure coordinated, safe care.
Increasingly, many patients find that the best path forward is integrative medicine—a medically supervised approach that combines conventional treatments with evidence-based complementary therapies. Integrative oncology aims to address the whole person while still using proven cancer-fighting interventions. By focusing on managing side effects, supporting immunity, improving nutrition, and enhancing quality of life, integrative care offers patients a broader framework for healing during and after cancer treatment.
In summary, patients explore alternative therapies for lung cancer for a variety of reasons, including managing side effects, boosting immunity, supporting whole-body healing, reducing recurrence risk, and aligning treatment with personal or cultural beliefs. While alternative medicine is not a substitute for evidence-based cancer treatment, it may play a supportive role for some individuals when integrated carefully and under professional guidance.
What’s Missing in Standard Care?
Lung cancer treatment has advanced significantly over the past few decades, with options such as surgery, chemotherapy, radiation therapy, targeted therapies, and immunotherapy offering new hope for patients. These treatments are designed to directly attack cancer cells or inhibit their growth. However, despite their powerful effects against tumors, conventional treatments may not address the broader biological, metabolic, and immune factors that influence cancer development and progression.
One of the main limitations of standard care is that it focuses narrowly on tumor eradication without always considering the health of the entire patient. For example, while chemotherapy and radiation are effective at destroying cancer cells, they can also harm healthy tissues, weaken the immune system, and cause long-term side effects. In many cases, these treatments do not work to rebuild or support the body’s natural defenses, leaving patients feeling depleted, vulnerable to infections, and struggling with chronic fatigue or digestive issues.
Research has shown that cancer arises not only from genetic mutations but also from interactions between cancer cells and their surrounding environment, including the immune system, inflammation, metabolism, and the health of connective tissues (Hanahan & Weinberg, 2011). However, conventional oncology often does not address these systemic factors directly. This can result in a situation where the tumor is treated, but the conditions that allowed cancer to develop—such as chronic inflammation, impaired detoxification, or immune dysfunction—remain unresolved.
Additionally, standard treatments may not fully support the patient’s nutritional needs, emotional well-being, or recovery of normal physiological function after therapy. Many patients report feeling that their care focuses heavily on tumor measurements and scans but offers little guidance on diet, stress management, sleep, or rebuilding strength. As a result, they may seek additional therapies to help fill these gaps.
An integrative or complementary approach aims to address these missing elements by focusing on whole-person care. This includes supporting digestion, improving nutrient absorption, enhancing immune resilience, reducing chronic inflammation, managing stress, and promoting tissue repair. By addressing these underlying factors, some believe the body may be better equipped to resist disease progression and recover from intensive treatments.
It’s important to note that alternative or complementary treatments are not a replacement for proven cancer therapies. However, they may play a valuable role in supporting the patient’s broader health needs, improving quality of life, and helping the body maintain a more balanced, resilient internal environment.
In summary, while conventional lung cancer treatment focuses on controlling the tumor, it may not always address the patient’s overall biological balance, immune strength, or recovery needs. Complementary approaches aim to fill these gaps by supporting the body as a whole, potentially improving well-being alongside standard medical care.
When Standard Lung Cancer Treatment Stops Working

For many patients, the search for broader and more personalised care does not begin at diagnosis. It begins at the point where standard treatment stops delivering meaningful improvement in survival, strength, or daily functioning. This moment is not always defined by tumour growth alone. It is often recognised through recurrence, drug resistance, and the clinical realities of advanced-stage disease.
Recurrence After Initial Response
A significant number of lung cancer patients experience an initial reduction in tumour size with chemotherapy, targeted therapy, radiation, or immunotherapy, followed by disease progression months or years later. This recurrence is one of the most emotionally and physically challenging phases of the cancer journey. Patients who once felt hopeful are suddenly faced with the return of symptoms, limited new treatment lines, and a progressive decline in performance status. It is at this stage that many begin to look for supportive strategies that can help maintain strength, appetite, breathing capacity, and treatment tolerance.
Drug Resistance and Diminishing Returns
Modern oncology has achieved remarkable advances, but tumour biology continues to evolve. Cancer cells adapt to targeted drugs and chemotherapy through genetic mutations and microenvironmental changes. Each subsequent line of treatment often produces a shorter and less durable response than the previous one. At the same time, toxicity accumulates. Fatigue becomes persistent, neuropathy may limit mobility, and nutritional status declines. Patients are not searching for an alternative because they reject science. They are searching because the benefit-to-burden ratio of treatment begins to change.
Stage IV Prognosis and the Shift in Treatment Goals
In advanced and metastatic lung cancer, the focus of care frequently shifts from cure to disease control, symptom relief, and preservation of quality of life. This transition is rarely discussed in emotional terms, yet it is deeply felt by patients and families. When survival statistics are presented alongside increasing physical weakness, many patients begin to ask a different question. Instead of asking how to destroy the tumour alone, they ask how to live better, breathe easier, eat normally, sleep well, and remain functional for as long as possible.
It is at this point that integrative and supportive approaches become clinically relevant. The goal is no longer defined only by tumour size on a scan, but by strength, resilience, immunity, and the ability to continue meaningful treatment with a better quality of life.
A change in treatment response is not the end of care.
For many patients, it is the beginning of a more personalised phase of medicine.
How Integrative Oncology Supports Patients When Standard Treatment Reaches Its Limit
When the response to chemotherapy, targeted therapy, immunotherapy, or radiation begins to decline, the clinical need does not end. In many cases, this is the phase where patients require the most comprehensive and personalised support. Integrative oncology focuses on improving the body’s ability to tolerate treatment, maintain strength, and preserve quality of life while continuing evidence-based cancer care.
Restoring Strength and Functional Capacity
One of the most common challenges in advanced lung cancer is the progressive loss of energy, muscle mass, and appetite. This decline directly affects survival because patients who are physically weak are often unable to continue life-prolonging therapies. Integrative care places a strong emphasis on metabolic correction, nutritional restoration, and physiological resilience so that the patient remains fit for ongoing treatment. The clinical goal is simple but powerful: a stronger body responds better and tolerates therapy longer.
Improving Treatment Tolerance
Many patients discontinue effective modern treatments not because the drugs stop working, but because the side effects become unbearable. Persistent fatigue, severe mucosal dryness, neuropathy, breathlessness, and gastrointestinal disturbance reduce adherence and quality of life. A structured integrative approach aims to reduce this toxicity burden, allowing patients to continue their primary oncology protocol with better tolerance and fewer interruptions.
Supporting Immunological Stability
In advanced disease, immune function is often profoundly compromised, either by the cancer itself or by repeated lines of therapy. Integrative strategies are directed toward stabilising immune response, reducing chronic inflammation, and improving recovery between treatment cycles. This support becomes particularly important for patients receiving immunotherapy, where systemic balance plays a crucial role in response and tolerability.
Breath, Sleep, and Daily Life: The Outcomes That Matter to Patients
Clinical success is not measured by imaging alone. Patients consistently report that their most meaningful improvements are the ability to walk without severe breathlessness, sleep through the night, eat without discomfort, and remain mentally stable during treatment. Integrative oncology addresses these functional outcomes directly. When these improve, patients regain a sense of control, dignity, and emotional strength.
A Parallel, Not Opposing, Approach
Integrative oncology does not replace modern cancer treatment. It works alongside it. The purpose is not to delay evidence-based therapy, but to enhance the patient’s ability to benefit from it. This distinction is essential for medical safety, global credibility, and long-term outcomes.
In this phase of the cancer journey, the definition of progress changes. It is no longer only about shrinking a tumour. It is about extending meaningful survival with strength, stability, and the best possible quality of life.
Patients do not measure recovery in millimetres of tumour reduction.
They measure it in steps walked, hours slept, and meals completed without exhaustion.
Who Is the Ideal Candidate for an Integrative Approach in Lung Cancer
Integrative care is not required at the same stage for every patient. However, there are clearly defined clinical situations where a personalised, strength-focused approach becomes highly relevant. These are the phases in which the primary goal is not only disease control, but the preservation of physiological reserve, treatment tolerance, and day-to-day functional independence.
Patients With Advanced or Stage IV Disease
In metastatic lung cancer, treatment is often delivered in multiple lines over a prolonged period. With each successive line, the body’s tolerance becomes a critical factor in determining survival. Patients who experience progressive fatigue, weight loss, breathlessness, or declining appetite benefit from a structured approach aimed at restoring strength and improving their ability to continue essential oncology care.
Patients Experiencing Recurrence After Initial Treatment
Recurrence creates a second turning point in the cancer journey. The emotional and physical burden is significantly higher, and the available treatment options may be more limited than during first-line therapy. At this stage, improving treatment response is closely linked to improving the patient’s overall physiological condition. A personalised integrative plan helps rebuild this foundation.
Patients Unable to Tolerate Chemotherapy or Targeted Therapy
A large number of patients discontinue effective modern treatment because the side effects become unmanageable. Severe fatigue, persistent nausea, neuropathy, mucosal dryness, gastrointestinal disturbance, and loss of muscle mass reduce the ability to continue therapy. These patients are not out of options. They require supportive strategies that improve tolerance so that life-prolonging treatment can continue safely.
Patients With Rapid Physical Decline or Cancer-Related Weakness
Loss of strength, reduced mobility, and increasing dependence are among the most distressing aspects of lung cancer. This decline is often reversible to a meaningful extent when metabolic, nutritional, and inflammatory factors are addressed in a structured and personalised way. Early intervention in this phase produces the most visible improvement in daily life.
Patients Seeking Better Quality of Life During Ongoing Treatment
Many patients continue chemotherapy, immunotherapy, or targeted therapy but struggle with sleep disturbance, breathlessness on minimal exertion, poor appetite, anxiety, and an inability to perform normal daily activities. These patients are clinically stable but functionally compromised. Integrative care focuses directly on these measurable, patient-centred outcomes.
Patients Who Want a Personalised, Whole-Body Treatment Plan
Modern oncology protocols are necessarily standardised. Integrative care becomes relevant for patients who require an approach based on their strength, nutritional status, treatment history, metabolic condition, and recovery capacity. This level of individualisation is particularly important in long-term cancer management.
Integrative support is most effective when introduced at the right time. The goal is not to replace ongoing oncology treatment, but to help the patient remain strong enough to benefit from it for as long as possible.
The right time for supportive care is not the last stage.
It is the moment the body begins to lose strength.
What Makes This Integrative Approach Different From General Supportive Care

Supportive care is often misunderstood as the use of a standard diet plan, a few supplements, or general lifestyle advice. While these measures may provide temporary comfort, advanced lung cancer requires a far more structured and medically coordinated strategy. A true integrative oncology approach is not generic. It is stage-specific, treatment-linked, and continuously adapted to the patient’s changing clinical condition.
Personalisation Based on Clinical Stage and Treatment Line
No two patients with lung cancer have the same physiological reserve, treatment history, or recovery capacity. The needs of a patient receiving first-line therapy are completely different from those of a patient who has undergone multiple lines of chemotherapy or targeted treatment. A structured integrative protocol is designed only after analysing disease stage, current oncology treatment, weight trends, appetite, inflammatory status, sleep pattern, breathlessness, and functional mobility. This ensures that every intervention has a defined clinical purpose.
Designed to Work Alongside Ongoing Oncology Treatment
General wellness plans are usually created in isolation. In contrast, a medically supervised integrative approach is synchronised with chemotherapy cycles, immunotherapy schedules, radiation timing, and recovery phases. The objective is to improve treatment tolerance, reduce interruptions, and support faster physiological recovery between cycles. This coordination is what allows patients to continue essential cancer therapy for a longer duration.
Focus on Measurable Functional Outcomes
The success of supportive care is often described in vague terms. A structured integrative model measures real clinical outcomes such as improvement in appetite, stabilisation of body weight, increased walking capacity, better sleep duration, reduction in fatigue, and improved treatment tolerance. These changes directly influence survival because they determine whether a patient remains fit for ongoing therapy.
Metabolic and Inflammatory Correction
Advanced lung cancer is not only a local disease. It is associated with systemic inflammation, altered metabolism, progressive muscle loss, and immune dysregulation. Addressing these factors in a targeted and personalised manner is what differentiates a medical integrative program from general nutritional advice. When these internal parameters improve, patients often experience better energy, clearer breathing, and greater treatment resilience.
Continuous Monitoring and Adaptation
The clinical condition of a lung cancer patient can change within weeks. A fixed plan is therefore ineffective. A structured integrative program is dynamic, with regular assessment and modification based on response, laboratory parameters, treatment phase, and symptom profile. This ongoing adjustment is essential for long-term benefit.
A Medically Supervised and Safety-Oriented Model
The most important distinction is supervision. Every intervention is selected based on compatibility with the patient’s current oncology protocol, organ function, and overall strength. This ensures safety, global medical acceptability, and optimal outcomes.
Integrative oncology is not an alternative to treatment. It is a parallel, medically coordinated system designed to help the patient remain strong enough to continue fighting the disease.
Supportive care becomes powerful when it is personalised, monitored, and medically aligned with cancer treatment.
A Personalised Integrative Evaluation for Lung Cancer Patients
Every lung cancer journey is biologically and clinically unique. The stage of disease, the number of treatment lines received, current medications, nutritional status, weight changes, breathing capacity, sleep quality, and overall functional strength all influence what kind of support a patient actually needs. For this reason, a meaningful integrative plan cannot be generalised. It must begin with a detailed and structured medical evaluation.
This evaluation is designed to understand whether the patient’s current challenge is primarily treatment intolerance, progressive weakness, metabolic decline, uncontrolled inflammation, loss of appetite, or recovery delay between therapy cycles. Identifying these factors allows the creation of a stage-specific program that works alongside ongoing oncology care rather than in isolation.
For patients in advanced stages, the focus is often on restoring enough strength to continue essential treatment with better tolerance. For those experiencing recurrence, the priority may be to stabilise body weight, improve energy levels, and enhance physiological resilience. For patients who are clinically stable but functionally weak, the aim is to rebuild day-to-day independence and improve quality of life.
This process is not limited by geography. International patients can undergo the same structured assessment through a guided medical review of their reports, treatment history, and current symptoms. Based on this analysis, a personalised plan is developed that is aligned with the patient’s ongoing oncology protocol and current physical capacity.
What makes this step important is timing. Integrative support produces the greatest benefit when introduced at the point where the body begins to show signs of decline, not when the patient becomes completely exhausted by the disease or its treatment.
The objective is clear and clinically measurable: to help the patient remain strong enough to continue necessary cancer therapy, to improve daily functional ability, and to extend meaningful survival with a better quality of life.
Patients who wish to understand whether this approach is suitable for their stage and condition can undergo a detailed personalised evaluation based on their current medical reports and treatment status.
The goal is not only to add days to life, but to add strength to those days.
Common Disorders Associated With Lung Cancer

Lung cancer rarely exists as an isolated disease. Because of its effect on the respiratory system, metabolism, immunity, and distant organs, patients frequently experience a group of associated clinical conditions that influence strength, treatment tolerance, and prognosis.
Chronic Obstructive Pulmonary Disease (COPD)
COPD is one of the most common coexisting conditions because smoking and long-term airway inflammation are shared causative factors. It leads to reduced lung reserve, persistent breathlessness, chronic cough, and poor oxygenation, which directly affects the ability to tolerate surgery, chemotherapy, or radiation.
Recurrent Respiratory Infections
Obstruction of bronchi by tumour mass and reduced immunity predispose patients to repeated bacterial infections, post-obstructive pneumonia, and prolonged recovery after minor infections. These episodes further weaken Agni, reduce appetite, and accelerate weight loss.
Cancer Cachexia
Progressive weight loss, muscle wasting, fatigue, and anorexia occur due to systemic inflammation and altered metabolism. This is one of the most important factors reducing survival because it makes patients unfit for ongoing therapy.
Pleural Effusion
Fluid accumulation in the pleural cavity causes breathlessness, chest heaviness, dry cough, and inability to lie flat. Recurrent effusion significantly reduces daily functional capacity.
Anaemia
Chronic disease, nutritional deficiency, bone marrow suppression from treatment, and inflammatory cytokines lead to reduced haemoglobin, causing severe fatigue, dizziness, and poor tissue oxygenation.
Pulmonary Embolism
Malignancy increases hypercoagulability, leading to clot formation in pulmonary vessels. This presents with sudden breathlessness, chest pain, tachycardia, and requires urgent management.
Superior Vena Cava Syndrome
Compression of the superior vena cava causes facial swelling, neck vein distension, headache, and breathlessness. It is more common in centrally located tumours.
Rare but Clinically Significant Disorders Associated With Lung Cancer
Paraneoplastic Syndromes
These occur due to hormone-like or immune-mediated effects of the tumour and may appear even before the lung lesion is diagnosed.
Syndrome of Inappropriate ADH Secretion (SIADH)
Leads to low sodium levels, confusion, weakness, nausea, and in severe cases altered consciousness. It is most commonly associated with small cell lung carcinoma.
Ectopic ACTH Production
Causes features of Cushing’s syndrome such as muscle weakness, weight changes, hyperglycaemia, and hypertension.
Hypercalcaemia
Often seen in squamous cell carcinoma and presents with constipation, confusion, excessive thirst, abdominal pain, and profound fatigue.
Lambert–Eaton Myasthenic Syndrome
An autoimmune neuromuscular disorder producing progressive muscle weakness that improves temporarily with activity. It is classically linked with small cell lung cancer.
Hypertrophic Pulmonary Osteoarthropathy
Characterised by clubbing of fingers, joint pain, periosteal inflammation of long bones, and reduced mobility.
Carcinomatous Meningitis
Metastatic spread to meninges causing headache, vomiting, cranial nerve palsy, altered sensorium, and neurological deficits.
Spinal Cord Compression
Vertebral metastasis may compress the spinal cord leading to back pain, limb weakness, sensory loss, and loss of bladder or bowel control. This is an oncological emergency.
Pericardial Effusion
Fluid accumulation around the heart produces breathlessness, tachycardia, chest discomfort, and reduced cardiac output.
These are not caused by the tumour itself but occur due to modern therapies and significantly influence patient strength.
Chemotherapy-Induced Neuropathy
Tingling, numbness, burning sensation in hands and feet, and reduced mobility.
Radiation-Induced Lung Fibrosis
Progressive breathlessness and reduced lung compliance months after therapy.
Immunotherapy-Related Pneumonitis
Inflammatory damage to lung tissue causing dry cough, fever, and oxygen desaturation.
Systemic Functional Disorders Seen in Long-Standing Disease
These conditions reflect Dhatu Kshaya and Oja depletion and determine recovery potential.
Severe Fatigue Syndrome
Persistent exhaustion not relieved by rest and associated with reduced mitochondrial function and chronic inflammation.
Sleep Disturbance and Anxiety
Due to breathlessness, metabolic imbalance, and psychological stress.
Loss of Appetite and Malabsorption
Leads to further weight loss and poor response to therapy.
Clinical Importance
Identification and management of these associated disorders is essential because they:
- decide treatment tolerance
- influence survival
- determine quality of life
- guide personalised Rasayana and Brimhana therapy
In advanced lung disease the major clinical goal is not only tumour control but stabilisation of these systemic and functional complications.
Ayurvedic correlation of disorders associated with lung cancer

Chronic obstructive pulmonary disease
COPD shows Vata Kapha predominance where Kapha creates obstruction in the respiratory channels and Vata loses its normal direction of movement. The main Dhatu involved are Rasa Dhatu and Mamsa Dhatu because long standing breathlessness reduces tissue nourishment and weakens the respiratory musculature. The primary Srotas affected are Pranavaha Srotas with Sanga and Margavarodha which explains air trapping, reduced expansion and chronic dyspnoea.
Recurrent respiratory infections
Repeated chest infections indicate Kapha with Pitta association in the later inflammatory phase. Rasa Dhatu becomes dushta and Oja reduces, leading to poor immunity and delayed recovery. The main Srotas involved are Pranavaha Srotas and Rasavaha Srotas, showing impaired circulation of primary nutrition and defence mechanism.
Cancer cachexia
Cachexia is a classical picture of Vata aggravation with severe Dhatu Kshaya. Rasa, Mamsa and Meda Dhatu progressively decline and finally Oja is affected. Rasavaha Srotas and Annavaha Srotas become weak due to Mandagni and poor absorption, resulting in weight loss, fatigue and muscle wasting.
Pleural effusion
Pleural fluid accumulation represents Kapha dominance with obstruction to the normal movement of Vata in the chest. Rasa Dhatu and Udaka metabolism are disturbed. Pranavaha Srotas and Udakavaha Srotas are involved, producing breathlessness, heaviness and reduced lung expansion.
Anaemia
Anaemia reflects Rakta Dhatu Kshaya with Pitta and Vata involvement. Raktavaha Srotas become weak leading to pallor, fatigue, dizziness and reduced oxygen carrying capacity.
Pulmonary embolism
This condition can be understood as Rakta Srotorodha where vitiated Vata disturbs normal circulation and Pitta affects the quality of Rakta. Raktavaha Srotas are the primary channels involved and the sudden obstruction produces acute breathlessness and chest pain.
Superior vena cava syndrome
This shows Kapha causing Margavarodha in the upper body with secondary Vata disturbance. Rasa and Rakta Dhatu circulation is impaired in the Urdhva Jatrugata region. Rasavaha and Raktavaha Srotas are affected leading to swelling and venous congestion.
Rare but clinically significant correlations
SIADH
This reflects disturbance of Jala Mahabhuta with Kapha Vata imbalance. Rasa Dhatu and Udakavaha Srotas are mainly involved causing fluid retention, weakness and confusion.
Ectopic ACTH production
This condition shows Pitta Vata vitiation with Meda and Mamsa Dhatu dushti. Medovaha Srotas are affected resulting in metabolic acceleration, muscle weakness and altered fat distribution.
Hypercalcaemia
Hypercalcaemia indicates Asthi Dhatu involvement with Pitta predominance and Rakta Dushti. Asthivaha Srotas and Raktavaha Srotas are affected producing constipation, burning sensation and neuromuscular weakness.
Lambert Eaton myasthenic syndrome
This is a Vata dominant disorder affecting Mamsa and Majja Dhatu. Majjavaha and Mamsavaha Srotas become weak leading to progressive muscle weakness and reduced neuromuscular transmission.
Hypertrophic pulmonary osteoarthropathy
This shows Vata Kapha involvement in Asthi and Mamsa Dhatu. Asthivaha and Mamsavaha Srotas are affected causing bone pain, joint swelling and clubbing of fingers.
Carcinomatous meningitis
This represents Vata Pitta vitiation in Majja Dhatu. Majjavaha Srotas are the main channels involved producing neurological symptoms and altered higher functions.
Spinal cord compression
A classical Vata aggravation in Asthi and Majja Dhatu where Majjavaha Srotas are compressed leading to pain, weakness and sensory loss.
Pericardial effusion
Kapha accumulation in the thoracic region obstructs normal Vata movement. Rasa Dhatu becomes dushta and Pranavaha Srotas around Hridaya are affected causing breathlessness and reduced cardiac efficiency.
Chemotherapy induced neuropathy
This is a pure Vata prakopa in Majja Dhatu and Majjavaha Srotas producing numbness, tingling and burning sensation.
Radiation induced lung fibrosis
This shows Vata Pitta involvement with Rasa and Mamsa Dhatu Kshaya and Srotosankocha of Pranavaha Srotas leading to dryness and reduced lung compliance.
Immunotherapy related pneumonitis
This represents Pitta Kapha dushti in Rakta and Rasa Dhatu affecting Pranavaha Srotas and producing inflammatory breathlessness and cough.
Systemic functional disorders
Severe fatigue syndrome
Fatigue indicates Rasa Dhatu Kshaya progressing towards Oja depletion with Vata predominance in Rasavaha Srotas.
Sleep disturbance and anxiety
These show Vata aggravation in Manovaha Srotas with Majja Dhatu Kshaya and reduced Oja leading to restlessness and insomnia.
Loss of appetite and malabsorption
Mandagni with Vata Kapha involvement affects Annavaha and Rasavaha Srotas and prevents proper formation of Rasa Dhatu, which becomes the root cause of further Dhatu depletion.
Clinical significance
This Dosha Dhatu Srotas mapping is essential because treatment in Ayurveda is not disease name based. The selection of Rasayana, Avaleha, Ghrita, Bhasma, Brimhana or Langhana depends on whether Vata depletion, Kapha obstruction, Pitta inflammation, Agnimandya or Oja Kshaya is dominant in that particular patient and at that particular stage.
Holistic Approach to Cancer Care
Lung cancer is not simply a disease of the lungs; it reflects a complex process involving the entire biological system. While modern oncology effectively targets cancer cells through chemotherapy, radiation, surgery, and immunotherapy, these approaches often focus narrowly on eradicating the tumor. However, cancer arises within an environment shaped by chronic inflammation, immune dysfunction, metabolic disturbances, and tissue-level imbalances. Therefore, healing the body from cancer requires more than tumor destruction , it involves restoring balance across multiple physiological systems.
The tumor microenvironment plays a pivotal role in cancer growth and progression. Scientific research has shown that cancer cells interact with surrounding immune cells, blood vessels, connective tissue, and signaling molecules to promote their survival. Chronic inflammation, suppressed immunity, disrupted nutrient pathways, and oxidative stress all contribute to this environment. While chemotherapy can shrink a tumor, it does not always correct the systemic imbalances that allowed the tumor to develop. This leaves a gap in care that patients feel physically and emotionally, especially during recovery.
A whole-body healing approach addresses these systemic factors by focusing on restoring digestion, reducing inflammation, rebuilding immunity, repairing tissues, and supporting emotional well-being. Digestive health is foundational because poor digestion impairs nutrient absorption and contributes to toxic metabolite buildup. In Ayurveda, impaired digestion leads to the accumulation of “Ama” (toxic residue), which obstructs the body’s internal channels and compromises tissue health. Chemotherapy and radiation often damage the gut lining, leading to nutrient malabsorption and microbiome imbalances. Whole-body healing seeks to restore gut integrity through nourishing foods, prebiotics, probiotics, and botanical therapies that repair mucosal tissues.
Supporting immune function is equally vital. Chemotherapy and radiation suppress immune cells such as lymphocytes and natural killer cells, weakening the body’s defense against cancer recurrence and infections. Scientific studies have explored immunomodulatory herbs like Tinospora cordifolia (Guduchi), Withania somnifera (Ashwagandha), and Curcuma longa (Turmeric), which may enhance immune surveillance and regulate inflammatory cytokines. In Ayurveda, immune vitality is reflected in the concept of “Ojas,” the essence that sustains strength and resilience. Rebuilding Ojas involves restoring energy reserves, reducing stress, and nourishing deep tissue layers.
Inflammation control is another central goal. Chronic inflammation fuels cancer cell proliferation, angiogenesis, and immune evasion. Elevated inflammatory markers like CRP and interleukins are linked to poor cancer outcomes. Whole-body healing uses anti-inflammatory nutrition, stress reduction, and herbal interventions such as Boswellia serrata and curcumin to lower pro-inflammatory signaling and promote tissue healing. Emotional health also plays a critical role in recovery. Psychological stress activates cortisol and catecholamine responses that suppress immunity and increase inflammatory mediators. Mind-body practices like yoga, meditation, and guided relaxation can reduce stress hormones, improve parasympathetic tone, and enhance emotional resilience, integral to healing.
Many patients experience long-term side effects after treatment, including fatigue, anemia, cognitive fog, and muscle wasting. Whole-body healing aims to rebuild tissues and restore metabolic balance through nutrient-dense diets, physical rehabilitation, Rasayana therapies, and gentle detoxification. The goal is not simply to return to baseline health but to create a stronger, more resilient internal environment that resists future disease.
Key principles of whole-body healing inlung cancer include:
- Supporting digestion and gut health to optimize nutrient absorption
- Rebuilding immune resilience after treatment-induced suppression
- Reducing chronic inflammation to create an anti-cancer environment
- Enhancing emotional well-being through stress reduction practices
- Promoting tissue repair and detoxification for recovery and strength
- Restoring metabolic balance and mitochondrial function for sustained energy
Whole-body healing does not aim to replace conventional treatment but to complement it by addressing the broader biological terrain in which cancer develops. By supporting digestion, immunity, inflammation resolution, emotional balance, and tissue repair, this approach empowers patients to participate actively in their recovery and strengthen their long-term health.
Herbal Therapies In Lung Cancer Care
In recent years, a growing number of lung cancer patients have turned to integrative and complementary therapies to support their recovery, manage side effects, and improve quality of life. These therapies are not intended to replace standard treatments such as chemotherapy, radiation, or surgery. Rather, they are used to support the patient’s overall well-being and address physiological imbalances that conventional care may not fully resolve. The integrative approach is rooted in combining evidence-based complementary therapies with mainstream oncology in a safe, coordinated, and patient-centered manner.
One of the most widely used branches of integrative care is herbal medicine. In systems like Ayurveda and Traditional Chinese Medicine (TCM), herbs are selected not only for their symptomatic relief but also for their systemic actions, such as modulating the immune system, reducing inflammation, improving respiratory function, or supporting detoxification. For instance, herbs like Withania somnifera (Ashwagandha), Tinospora cordifolia (Guduchi), Curcuma longa (Turmeric), and Ocimum sanctum (Tulsi) have been studied for their adaptogenic, antioxidant, and immunomodulatory effects. In modern research, curcumin has shown potential in reducing inflammation and influencing cell signaling pathways relevant to cancer progression.
Dietary therapy is another central pillar. Nutritional strategies often focus on anti-inflammatory diets rich in whole grains, seasonal vegetables, fruits, healthy fats, and plant-based proteins. These diets aim to reduce systemic inflammation, support digestive function, and improve metabolic health. Patients are encouraged to avoid processed foods, excessive sugar, and inflammatory oils. In some protocols, specific diets such as low-glycemic or intermittent fasting schedules may be considered, based on individual tolerance and oncological supervision.
Mind-body therapies such as meditation, yoga, breathwork (pranayama), and guided imagery are increasingly accepted within cancer care. These practices are not only helpful in reducing stress and anxiety but have also been shown to lower inflammatory markers and improve immune function in clinical studies. Stress and emotional trauma can influence disease outcomes, and mind-body therapies offer a structured way to calm the nervous system and restore emotional equilibrium.
Detoxification therapies, particularly in traditional systems like Ayurveda, focus on removing accumulated toxins (Ama) that are believed to block internal pathways and contribute to disease. Panchakarma, an Ayurvedic detoxification process, includes therapies like medicated oil massage (Abhyanga), herbal steam (Swedana), and controlled emesis or purgation (Vamana, Virechana) under expert guidance. These treatments are intended to improve metabolism, relieve toxin burden, and rejuvenate tissues. In modern contexts, detox strategies may also involve gentle liver support, increased hydration, and antioxidant supplementation, particularly post-chemotherapy.
Additionally, acupuncture, a core component of Traditional Chinese Medicine, has been studied for its role in reducing chemotherapy-induced nausea, improving appetite, regulating energy, and alleviating pain or neuropathy. Mistletoe therapy, used in integrative oncology clinics in Europe, is also being explored for its immunomodulatory properties and potential to enhance quality of life in cancer patients.
The use of these therapies should always be personalized, based on the patient’s medical history, cancer stage, current treatments, and underlying constitution. A qualified practitioner familiar with both conventional oncology and traditional systems can help guide patients safely through this process. Integrative therapies are most effective when they are coordinated, evidence-informed, and aligned with each patient’s treatment goals and biological needs.
Ayurvedic View of Lung Cancer
In Ayurvedic medicine, lung cancer does not correspond directly to a single term but is understood through several classical frameworks involving abnormal tissue growth, channel obstruction, and systemic imbalance. The disease may be interpreted using concepts such as Arbuda (malignant tumor), Granthi (benign growth), Kshata-Kshina (lung tissue injury), and Shvasa/Kasa Roga (chronic respiratory disorders), depending on the symptoms, tissue involvement, and disease stage.
According to Ayurveda, disease originates from the imbalance of the three Doshas—Vata, Pitta, and Kapha, which are the fundamental bioenergies governing physiological functions. Lung cancer, in most cases, involves a dominant Kapha-Vata dosha aggravation, particularly affecting the Pranavaha Srotas, the system responsible for respiration and life force circulation. Kapha dosha contributes to the formation of dense, mucous-like, and slow-growing tumors, while Vata dosha causes irregular cellular functions, rapid spread, and degeneration. If Pitta is involved, it can intensify inflammation and tissue destruction.
The pathogenesis (Samprapti) in Ayurvedic understanding begins with a disturbance in digestive fire (Agni) and accumulation of Ama, toxic metabolic waste that blocks cellular intelligence. This Ama travels through the microchannels (Srotas), especially the Pranavaha Srotas (respiratory channels), and settles in weak or pre-damaged tissues. Over time, it causes localized stagnation, depletion of Ojas (vital essence), and abnormal tissue formation in the lungs. These abnormal growths, when ignored, manifest as complex conditions such as Arbuda, described in the Sushruta Samhita as a deep-seated, non-suppurative, gradually enlarging mass, often painful and resistant to healing.
Furthermore, Ayurvedic texts emphasize the role of Dhatu Dushti—damage or vitiation of body tissues such as Rasa (plasma), Rakta (blood), and Mamsa (muscle). In lung cancer, one typically observes the involvement of Rasa-Rakta-Mamsa-Majja Dhatus, leading to progressive depletion of vitality, breathlessness, fatigue, and tissue distortion.
Ayurveda also recognizes the importance of Nidana (causative factors). These include improper diet (heavy, oily, kapha-increasing foods), chronic toxin exposure (inhaled or ingested), unresolved emotions (especially grief and fear affecting Vata), suppression of natural urges (Udavarta), and genetic tendencies (Beejadosha). In many ways, this overlaps with modern understandings of carcinogenesis—where inflammation, immune dysregulation, oxidative stress, and environmental triggers play key roles.
Treatment in Ayurveda focuses on breaking the pathogenesis at multiple levels. It involves removing Ama through purification (Shodhana), restoring Dosha balance with appropriate herbs and therapies, strengthening digestion and tissue metabolism, and rebuilding immunity through Rasayana (rejuvenation) therapy. Importantly, Ayurveda does not just target the tumor—it seeks to restore harmony in the internal environment, making the body less supportive of cancer development and recurrence.
In summary, Ayurveda views lung cancer as a multi-dimensional disorder rooted in Dosha imbalance, Srotas blockage, and Dhatu corruption—manifesting over time due to poor lifestyle, environmental exposures, and weakened immunity. Its approach aims to correct these imbalances systematically while supporting the body’s self-healing mechanisms.
Ayurvedic Treatment for Lung Cancer

Ayurveda approaches the treatment of lung cancer through a structured, multi-phase protocol aimed at detoxifying the body, correcting internal imbalances, strengthening weakened tissues, and restoring the body’s natural ability to heal. Unlike conventional medicine, which primarily targets the tumor itself, Ayurveda focuses on changing the biological terrain that allows cancer to arise and persist. This includes addressing digestive dysfunction, dosha imbalances, toxin accumulation, immune weakness, and depletion of vitality or Ojas.
The first phase of treatment typically involves Shodhana, or purification. This includes individualized detoxification therapies designed to eliminate accumulated Ama (toxins), which are believed to obstruct cellular communication and metabolism. Depending on the patient’s strength and disease stage, Panchakarma therapies such as Virechana (purgation), Basti (medicated enema), or Nasya (nasal cleansing) may be used to open blocked channels (Srotas) and remove pathogenic factors. These are always tailored to the patient’s current doshic imbalance, digestive capacity (Agni), and overall resilience.
Following detox, the focus shifts to Shamana, or palliative treatment, aimed at balancing aggravated doshas using herbal formulations, medicated oils, and lifestyle regulation. In cases of lung cancer, the treatment often targets aggravated Kapha and Vata. Herbs like Kanchanar Guggulu, Pippali, Vasa, Pushkarmool, and Haridra are chosen for their ability to break down growths, clear respiratory channels, modulate immune responses, and reduce inflammation. If Pitta involvement is dominant—manifesting as fever, bleeding, or inflammation—cooling and anti-inflammatory herbs like Guduchi, Amalaki, and Yashtimadhu may also be included.
The third phase of the Ayurvedic approach is Rasayana therapy, which focuses on rejuvenation and long-term tissue support. Cancer and its treatment deplete the body’s Dhatus (tissues), Ojas (vital essence), and mental resilience. Rasayana herbs such as Ashwagandha, Shatavari, Bala, Swarna Bhasma, Abhrak Bhasma, and Gandhak Rasayan are used to restore energy, enhance immune function, and protect against recurrence. These therapies not only help in physical recovery but also in stabilizing psychological strength, sleep patterns, and digestive integrity—areas often disrupted by the cancer journey.
Ayurveda also incorporates strict dietary guidance as part of the treatment plan. The diet is tailored to pacify the aggravated dosha, enhance Agni, and prevent toxin accumulation. Light, warm, easily digestible foods—such as vegetable soups, mung dal, cooked greens, and digestive spices—are commonly recommended. Heavy, cold, processed, and mucus-producing foods are typically avoided.
In addition to herbs and diet, lifestyle interventions play a vital role. This includes proper sleep, breathwork (Pranayama), gentle yoga, meditation, and daily routines (Dinacharya) that help maintain equilibrium and prevent further doshic disturbance. Emphasis is placed on reducing exposure to environmental toxins, smoke, psychological stress, and erratic routines—all of which are viewed as contributors to disease aggravation.
Overall, the Ayurvedic treatment approach does not promise a singular cure but aims to build an internal environment hostile to cancer cells and supportive of natural immunity and vitality. This process is gradual, personalized, and must be adapted to the patient’s Prakriti (constitution), Vikriti (disease state), and disease stage. When used alongside or after conventional therapies under expert supervision, it may help reduce recurrence risk, improve quality of life, and support long-term systemic balance.
Key Ayurvedic Formulations Lung Cancer
Ayurveda offers a range of classical and evidence-informed herbal and mineral formulations that may assist in managing lung cancer when used under expert supervision. These formulations are chosen not to directly “kill” cancer cells in the way modern chemotherapy does, but to modulate the internal environment, reduce tumor-promoting factors such as inflammation and immune dysfunction, and support systemic balance. The goal is to create a physiological state that is less favorable for tumor survival and more supportive of tissue regeneration, respiratory health, and immune integrity.
One of the most widely used classical formulations in respiratory and tumor-like conditions is Kanchanar Guggulu. This polyherbal preparation combines herbs such as Kanchanar, Triphala, Trikatu, Guggulu, and Varuna. It is traditionally used to address granthi (nodular growths), arbuda (tumors), and glandular swellings, especially in Kapha-dominant pathologies. Kanchanar helps to break down hardened tissue masses, improves lymphatic circulation, reduces Kapha accumulation, and supports metabolism at the cellular level. Its inclusion in cancer protocols is supported by its ability to regulate growths, clear channel obstructions, and stimulate sluggish tissue function.
Gandhak Rasayan Avaleha, a refined sulfur-based formulation, is used to strengthen immunity, purify the blood, and improve tissue response. It is considered particularly beneficial when patients are undergoing detox or recovery phases. Sulfur (Gandhak), when properly purified and processed, is said to penetrate deep tissues, enhancing cellular function, removing metabolic waste, and boosting vitality (Ojas). In modern pharmacology, sulfur compounds are being investigated for their anti-inflammatory and antimicrobial potential, which supports its traditional uses.
Trikatu Churna, which contains equal parts of Pippali (long pepper), Shunthi (dry ginger), and Maricha (black pepper), is used to enhance Agni (digestive/metabolic fire) and bioavailability of other herbs. It is commonly included in cancer regimens to stimulate digestion, reduce Ama, and enhance the absorption of Rasayana herbs. Pippali also has demonstrated immune-modulating and bronchodilatory effects, making it highly relevant in pulmonary conditions.
Sitopaladi Churna is another well-known formulation that targets respiratory congestion, cough, and chronic lung irritation. It contains Vanshlochan (bamboo silica), Pippali, Ela, Twak (cinnamon), and Mishri. Though mild in action, it is often used in chronic conditions to soothe inflamed lung tissues and support expectoration, particularly when combined with stronger anti-cancer or Rasayana herbs.
Rasayana Bhasmas, such as Swarna Bhasma (gold ash), Heerak Bhasma (diamond ash), Abhrak Bhasma (mica ash), and Tamra Bhasma (copper ash), are incorporated in carefully designed protocols to rejuvenate tissues, improve immunity, and target deep-seated imbalances. These calcined minerals are used in microdoses following traditional guidelines, often in combination with Rasayana herbs, and should only be administered by skilled practitioners. Swarna Bhasma, in particular, has shown promise in laboratory studies for modulating immune activity and possibly exhibiting selective cytotoxicity against abnormal cells.
Vasa (Adhatoda vasica) and Pushkarmool (Inula racemosa) are also frequently used in lung conditions due to their mucolytic, anti-inflammatory, and expectorant properties. They help to clear respiratory blockages, soothe irritated bronchial tissues, and support the elimination of Kapha toxins from the lungs.
Each formulation is chosen based on the individual patient’s doshic profile, disease stage, tissue involvement, and strength (Bala). Ayurvedic cancer management is not a one-size-fits-all approach. The synergy between herbs, mineral compounds, dietary interventions, and lifestyle regulation defines the efficacy of the treatment protocol. When prescribed responsibly and integrated thoughtfully, these formulations may offer significant supportive care to patients undergoing or recovering from cancer therapies.
Herbs & Minerals with Scientific Validation
Ayurveda offers a robust therapeutic framework that combines the use of potent herbs and mineral compounds to address complex diseases like cancer. Unlike conventional treatments that focus solely on tumor eradication, Ayurveda works to correct the systemic terrain in which cancer arises—addressing immune dysfunction, metabolic imbalance, tissue degeneration, and toxin accumulation. This approach is grounded in Rasayana chikitsa (rejuvenation therapy), which emphasizes deep cellular nourishment, detoxification, and restoration of vitality. Modern pharmacological studies have increasingly validated these Ayurvedic interventions, identifying specific bioactive compounds and mineral elements responsible for their anticancer effects.
Among the most widely studied herbs is Curcuma longa (turmeric), whose active compound curcumin (C₂₁H₂₀O₆) exhibits powerful anti-inflammatory, antioxidant, and antiproliferative properties. It inhibits tumor pathways such as NF-κB, COX-2, STAT3, and IL-6 and induces apoptosis in cancer cells. However, curcumin’s low bioavailability is improved in Ayurvedic practice through the co-administration of Pippali (Piper longum), whose alkaloid piperine (C₁₇H₁₉NO₃) enhances absorption significantly. Withania somnifera (Ashwagandha) contains withaferin A (C₂₈H₃₈O₆), a steroidal lactone that selectively induces apoptosis in tumor cells while protecting healthy tissues. It downregulates Hsp90 and vimentin, both implicated in cancer progression, and enhances immune regulation via modulation of p53 expression.
Tinospora cordifolia (Guduchi) is another central Rasayana herb, known for its immunomodulatory and hepatoprotective functions. Its key constituents—tinosporaside and cordifolioside A (C₁₆H₂₆O₁₁) stimulate macrophage activity and enhance cytokine balance, especially IL-2 and IFN-γ, while supporting liver function during chemotherapy. Plumbago zeylanica (Chitrak) contains plumbagin (C₁₁H₈O₃), a potent naphthoquinone that generates reactive oxygen species in cancer cells, inhibits angiogenesis (via VEGF suppression), and blocks G2/M cell cycle progression.
Boswellia serrata (Shallaki) has emerged as an anti-inflammatory anticancer agent, primarily due to boswellic acids like AKBA (Acetyl-11-keto-β-boswellic acid, C₃₂H₄₈O₄), which inhibit 5-lipoxygenase pathways involved in leukotriene synthesis. It reduces peritumoral edema, enhances blood flow, and has shown potential in glioblastoma and colon cancer models. Similarly, Semecarpus anacardium (Bhallataka), when properly purified, demonstrates strong cytotoxicity against cancer cells through semecarpol and anacardic acids (C₁₅H₂₄O₂), which modulate immune activation and epigenetic expression via HAT inhibition.
In addition to herbs, Ayurveda employs a sophisticated category of mineral and metal-based formulations known as Bhasmas , calcined nano-sized ashes that are meticulously purified and processed to become biologically active. These include Swarna Bhasma (gold ash, elemental Au), Heerak Bhasma (diamond ash, C), Abhrak Bhasma (mica ash, KAl₂(AlSi₃O₁₀)(OH)₂·nH₂O), and Tamra Bhasma (copper ash, Cu). These are used in microgram to milligram doses, offering antioxidant, Rasayana, and immune-enhancing effects. Swarna Bhasma has shown selective uptake by macrophages and potential to stimulate T-cell mediated immunity. Heerak Bhasma is believed to penetrate deep tissues and correct DNA-level abnormalities, while Abhrak Bhasma strengthens respiratory tissues and supports mitochondrial energy production.
Other important mineral-based agents include Gandhak Rasayan, prepared from purified sulfur (S₈), which enhances immunity and detoxification when used as Avaleha (herbal jam), and Rasa Sindoor, a mercury-sulfur compound that is properly detoxified through classical samskara processes to become bioavailable and therapeutic. While controversial from a Western toxicological perspective, when prepared according to Ayurvedic pharmacopeia standards, these compounds are used to modulate metabolism, reduce tumor burden, and enhance vitality. Makshik Bhasma (CuFeS₂) and Trivanga Bhasma (a tri-metallic preparation of lead, tin, and zinc) are sometimes included in Kapha-Vata dominant presentations of arbuda (tumors), especially when digestion is weak and tissue infiltration is high.
Ayurveda also integrates protective botanicals like Azadirachta indica (Neem), Emblica officinalis (Amalaki), and Phyllanthus niruri (Bhumyamalaki), whose active constituents such as azadirachtin (C₃₅H₄₄O₁₆), gallic acid (C₇H₆O₅), and phyllanthin (C₂₄H₃₄O₆) respectively contribute to antimutagenic, hepatoprotective, and DNA repair functions.
Together, these herbs and minerals form synergistic protocols customized to the patient’s Prakriti (constitution), Vikriti (pathological state), and cancer stage. This layered, intelligent integration is what makes Ayurvedic oncology both systemic and adaptable—targeting the disease without compromising the terrain.
Post-Treatment Regeneration
Rasayana therapy is one of the most sophisticated branches of Ayurvedic medicine, designed not just for recovery but for deep rejuvenation of tissues, immunity, and cellular intelligence. In the context of lung cancer, Rasayana therapy becomes particularly important after the intensive catabolic phase of treatment—such as chemotherapy, radiation, and surgical intervention—when patients are often left with depleted energy reserves, weakened tissues, impaired digestion, emotional trauma, and compromised immunity. Modern medicine acknowledges this state as post-treatment fatigue, cachexia, or immunosuppression, while Ayurveda sees it as Dhatu Kshaya (tissue depletion) and Ojas Kshaya (loss of vitality).
The purpose of Rasayana therapy is to rebuild the Dhatus, restore Ojas, and reintegrate biological function through nutritive, adaptogenic, and restorative medicines. It is never a one-size-fits-all intervention but always tailored to the patient’s constitution (Prakriti), strength (Bala), digestion (Agni), and tissue state. Rasayana therapy is not limited to boosting immunity—it is a comprehensive reset of the internal ecosystem.
Key herbal Rasayanas used in lung cancer convalescence include Ashwagandha (Withania somnifera), Shatavari (Asparagus racemosus), Amalaki (Emblica officinalis), Bala (Sida cordifolia), Yashtimadhu (Glycyrrhiza glabra), and Guduchi (Tinospora cordifolia). Each of these has documented antioxidant, immunomodulatory, and adaptogenic effects. Ashwagandha and Bala help rebuild musculoskeletal strength and stamina. Shatavari and Amalaki nourish Shukra and Rasa Dhatus, promoting cellular regeneration. Guduchi modulates cytokine responses, supports leukocyte function, and guards against residual oxidative damage.
On the mineral side, Swarna Bhasma (gold ash), Abhrak Bhasma (mica ash), and Heerak Bhasma (diamond ash) are used in precise micro-doses to stimulate deep tissue repair, mitochondrial function, and immune response. These are often combined with herbal jam-like formulations called Avaleha, such as Chyawanprash, Swarna Prashan, or Gandhak Rasayan Avaleha, each chosen based on the patient’s stage of healing and doshic status.
Unlike synthetic vitamin or protein supplements, Rasayana formulations are prepared with Anupana (specific carriers) like ghee, honey, or warm milk, which act as bioavailability enhancers. These formulations not only rebuild tissues but restore the integrity of microchannels (Srotas), stabilize hormonal cycles, and re-establish physiological rhythm.
In modern biomedical terms, Rasayana therapy may be viewed as an integrative regenerative model that improves hematological parameters, strengthens the gut-immune axis, reduces treatment-related inflammation, and improves energy metabolism. Clinical studies have shown that Rasayana herbs improve antioxidant enzyme activity (like SOD, catalase), normalize cortisol levels, and enhance subjective markers of well-being, mood, and vitality.
Timing and sequence are critical. Rasayana is initiated only after the cleansing and detoxification (Shodhana) phase, when Agni is reestablished and tissues are ready to receive nourishment. It should not be rushed or layered over an inflamed or toxin-laden terrain, as it may overload already compromised systems. Therefore, Rasayana therapy in post-cancer care follows a phased model—light Rasayana like herbal teas or decoctions early on, followed by deeper formulations like Avaleha, and eventually mineral Rasayana if tolerated.
Ultimately, Rasayana therapy represents the essence of healing in Ayurveda. It is the return from survival to strength, from catabolism to regeneration, from fatigue to restored life force. In lung cancer recovery, it offers not only improved physical outcomes but a sense of renewal and restored dignity to patients who have endured intense medical trauma.
Strengthening the Immune Terrain
One of the most critical aspects of lung cancer recovery is ensuring that the internal terrain no longer favors cancer cell survival or recurrence. This requires more than immune “boosting.” It involves a systematic restructuring of the immune terrain—the complex ecosystem of cells, tissues, and signaling molecules that regulate surveillance, inflammation, repair, and tolerance. Ayurveda offers a multi-layered approach to immune restoration, grounded in its understanding of Ojas, Agni, and Srotas as the foundational pillars of health.
In modern immunology, cancer is recognized not just as a problem of cell mutation but as a failure of immune detection and response. Tumors often evade immune attacks by creating immunosuppressive microenvironments, manipulating cytokines, and exhausting T cells. In post-treatment patients, the immune system is often further weakened by chemotherapy-induced lymphopenia, gut microbiome disruption, and chronic inflammation. Ayurveda describes this as a state of Ojakshaya (loss of immune essence), where even a minor insult can reignite systemic dysfunction.
The Ayurvedic immune system is not a single organ or cell type. It is an integrated intelligence that depends on strong Agni (digestive-metabolic fire), unobstructed Srotas (channels), balanced Tridoshas, and vital tissue essence (Ojas). Therefore, the strategy for long-term protection focuses not only on killing residual tumor cells but also on restoring these core regulatory systems.
At the center of this terrain reconstruction is Rasayana therapy, a specialized branch of Ayurveda targeting cellular nutrition, DNA repair, hormonal balance, and immunomodulation. Herbs like Guduchi (Tinospora cordifolia), Amalaki (Emblica officinalis), Shatavari (Asparagus racemosus), and Ashwagandha (Withania somnifera) play documented roles in restoring immune homeostasis. These herbs regulate pro-inflammatory cytokines such as IL-1β, TNF-α, and IL-6 while enhancing phagocytic activity, T-cell responsiveness, and antibody production.
Mineral Rasayanas such as Swarna Bhasma and Abhrak Bhasma act on a deeper level—rebuilding depleted tissues, activating macrophage signaling, and supporting stem-cell-like regeneration. Swarna Bhasma, when properly administered, has shown upregulation of CD4+ T cells and increased IgG levels in animal models, indicating its role in adaptive immunity.
Beyond pharmacological intervention, the gut-immune axis plays a key role in terrain healing. Chemotherapy and radiation disrupt microbiota diversity, leading to increased intestinal permeability (leaky gut), chronic inflammation, and altered antigen recognition. Ayurvedic texts acknowledge this through the connection between Agni and Ojas, poor digestion leads to undigested food (Ama), which then becomes a source of systemic toxicity and immune confusion. Therapies like Ama Pachana (Ama-reducing decoctions), Virechana (controlled purgation), and buttermilk enemas (Takra Basti) are used to cleanse the gut terrain, restore microbial harmony, and rebuild mucosal immunity.
Lifestyle also plays a powerful role in immune architecture. Proper sleep (Nidra), controlled exposure to natural sunlight, daily Abhyanga (oil massage), Pranayama, and Nasya are all used to maintain circadian regulation, stimulate lymphatic movement, and optimize neuroendocrine-immune feedback loops. These practices regulate melatonin, cortisol, and vagal tone—all of which profoundly affect immunity.
Strengthening the immune terrain is not about overstimulation. Ayurveda warns against prematurely pushing immunity in a weak or inflamed body. Instead, it advocates sequential rebuilding—first clearing residual toxins, then calming inflammation, and only then gradually introducing Rasayana formulations to rebuild Ojas and re-pattern immunity.
In conclusion, Ayurveda offers a precise roadmap for terrain healing in cancer survivors. It treats the immune system not as a mechanical defense but as a sensitive ecological matrix—a system that must be nourished, aligned, and intelligently activated. Through personalized interventions targeting digestion, detox, rejuvenation, and lifestyle, it seeks to establish long-term immune stability and make recurrence biologically unlikely.
Why Ayurveda Focuses on Terrain, Not Just Tumor Destruction

In modern oncology, the dominant approach to cancer revolves around tumor eradication—cut, poison, or burn the tumor through surgery, chemotherapy, and radiation. While these methods have proven life-saving for many, they often ignore the biological terrain in which the tumor developed. This terrain includes everything from immune balance, metabolic function, inflammation levels, microbiome health, hormonal integrity, and emotional state—all of which influence whether cancer cells are destroyed, tolerated, or allowed to regrow.
Ayurveda, by contrast, does not view the tumor as the primary problem—it sees it as the manifestation of deeper systemic disharmony. This approach is not passive; it is deeply proactive. Instead of targeting the “enemy” (the tumor), Ayurveda focuses on transforming the battlefield—the internal environment that allowed the enemy to thrive. This is known as Rogi Bala Chikitsa, or treating the host’s strength and resilience.
The Ayurvedic model understands cancer (often categorized under Arbuda, Granthi, or Dushta Vrana) as an outcome of Srotorodha (channel obstruction), Dosha aggravation, Dhatu corruption, and Ojas depletion. This means that unless the terrain—the body’s soil—is restored, removing the tumor is like cutting weeds without changing the soil. Cancer may disappear temporarily, but its root conditions remain untouched.
Modern systems biology increasingly aligns with this terrain-focused view. Cancer is now recognized as a systems disease, involving disruptions in energy metabolism (Warburg effect), immune evasion, chronic inflammation, mitochondrial dysfunction, and circadian rhythm disorders. These systemic disturbances are exactly what Ayurveda addresses through its individualized, layered protocols involving Agni (digestion), Ama (toxicity), Ojas (vitality), Prana (life force), and Dhatu Shuddhi (tissue purification).
By treating the terrain, Ayurveda doesn’t merely suppress symptoms—it re-patterns the internal ecosystem to make cancer recurrence biologically unlikely. It does this through:
- Cleansing (Shodhana): To eliminate deep-seated metabolic waste and pharmaceutical residues
- Balancing Doshas (Shamana): To calm systemic disturbances in Kapha, Pitta, and Vata
- Rebuilding Dhatus (Tissue Regeneration): Through Rasayana and tailored nutrition
- Restoring Agni and Ojas: So that metabolism and immunity become self-regulating
- Aligning with Rhythms (Dinacharya, Ritucharya): To prevent future imbalances before they form
This terrain-based strategy is not anti-modern medicine—it is complementary. Ayurveda can work alongside surgery or chemotherapy by reducing side effects, improving tissue recovery, and restoring balance after the toxic burden. However, its long-term focus remains different: it doesn’t just aim for tumor reduction; it seeks systemic correction, immune re-education, and physiological re-alignment.
In conclusion, the Ayurvedic focus on terrain reflects its philosophy of sustainability, not just survival. By correcting what allowed cancer to grow—rather than only removing what was visible—Ayurveda aims to make healing deeper, more enduring, and aligned with the body’s natural intelligence.
Agastya Haritaki Avaleha Main Medicine For Recovery – Classical Respiratory Rasayana
Agastya Haritaki Avaleha is a time-honoured Ayurvedic formulation described for chronic respiratory disorders, long-standing cough, breathlessness, tissue depletion, and loss of strength. In classical practice it is used to nourish the lungs, improve digestion, rebuild body weight, and enhance overall vitality during prolonged illness.
Classical Reference and Meaning for Patients
Shloka – Kasa and Shwasa Chikitsa
अगस्त्यहरीतकी नाम रसायनमनुत्तमम् ।
कासश्वासक्षयहरं बलवर्णाग्निवर्धनम् ॥
Ashtanga Hridaya, Chikitsa Sthana – Kasa Chikitsa
This Rasayana is described as one of the best rejuvenative formulations for chronic cough, breathlessness, tissue depletion, and loss of strength. It improves digestive power, complexion, and overall energy.
Shloka – Action on Respiratory Channels
हरीतकी प्रधानत्वात् कफवातहरं परम् ।
दीपनं पाचनं चैव प्राणवहस्रोतसां हितम् ॥
Bhaishajya Ratnavali – Kasa Roga Adhikara
Because Haritaki is the dominant ingredient, it clears mucus obstruction, regulates Vata in the chest, kindles digestion, and supports the respiratory system.
Classical Ingredient Composition with Approximate Weight
Main Herbal Base
Haritaki (Terminalia chebula) coarse powder – 1 kg
Dashamoola decoction preparation (from 10 roots) – 4 to 5 litres (reduced for Avaleha paka)
Pranavaha Srotas–Supporting Herbs
Pippali – 100 g
Pippalimoola – 100 g
Shunthi – 100 g
Maricha – 100 g
Chitraka – 100 g
Bharangi – 100 g
Kantakari – 100 g
Brihati – 100 g
Shati – 100 g
Guduchi – 200 g
Brimhana and Rasayana Support
Ghee – 500 g
Tila taila – 500 ml
Guda (jaggery) – 1.5 to 2 kg (as per classical Avaleha paka)
Madhu (honey) – added after cooling – 500 g
These quantities represent the classical bulk preparation. In clinical dispensing, the final Avaleha is standardised into patient-specific doses.
Highly Potent Mineral Rasayana (Added Only After Assessment)
In advanced tissue depletion and severe weakness, the formulation may be fortified with selected mineral Rasayana in micro-doses:
Swarna Bhasma
For Ojas support, immunity, and deep tissue rejuvenation
Heerak Bhasma
For cellular strength, metabolic activation, and advanced Rasayana effect
Abhraka Bhasma (Sahasraputi)
For lung capacity, tissue regeneration, and long-term debility
Swarna Makshika Bhasma
For energy metabolism and fatigue
Pravala Pishti
For inflammatory balance and respiratory heat
Mukta Pishti
For debility, burning sensation, and Pitta stabilisation
Lauha Bhasma
For anaemia and severe exhaustion
These are never added as a fixed formula. Their inclusion depends on:
- strength of the patient
- digestion
- stage of disease
- ongoing treatment
- inflammatory status
Dosage and Duration
Standard Dose
15 grams twice daily
Morning – empty stomach or before food with warm water or milk as advised
Evening – before dinner or as per digestive capacity
Duration
30 days in one treatment cycle, followed by reassessment.
Dose may be adjusted in:
- low digestion
- severe weakness
- high Pitta symptoms
- during chemotherapy cycles
How It Works in the Body
On the Lungs
- Reduces chronic cough and breathlessness
- Clears mucus obstruction
- Improves oxygen utilisation through better tissue nourishment
On Digestion and Weight
- Kindles Agni
- Improves appetite
- Enhances nutrient absorption
- Helps stabilise body weight
On Strength and Energy
- Rebuilds depleted Dhatu
- Improves walking capacity and daily activity tolerance
- Supports better recovery between treatments
On Immunological Resilience
- Acts as Rasayana
- Supports Vyadhikshamatva
- Helps in long-term recovery phase
Why the Ingredients Change in Every Patient
This formulation is always personalised based on:
Prakriti
- Vata dominant patients require more unctuous and Brimhana support
- Pitta dominant patients require cooling mineral balance
- Kapha dominant patients require stronger Deepana and Lekhana
Stage of Disease
- Inflammatory phase
- Severe weight loss phase
- Low digestion phase
- Recovery phase
Bala and Agni
- In very low digestion, mineral Rasayana are introduced later
- In strong patients, full Rasayana protocol can be given earlier
- This classical individualisation is called Yukti-vyapashraya Chikitsa.
Expected Patient-Level Improvements When Properly Selected
- Improved appetite
- Better bowel regularity
- Gradual increase in energy
- Reduced cough frequency
- More comfortable breathing
- Improved sleep
- Stabilisation of body weight
- These changes indicate improved internal strength and better treatment tolerance.
Essential Patient Guidance
This Avaleha should always be:
- prepared and prescribed under Ayurvedic medical supervision
- matched to digestion and strength
- modified during treatment phases
It is not a general over-the-counter preparation because the stage of illness and metabolic capacity determine the correct formulation.
Important Warning – Do Not Buy Agastya Haritaki Avaleha From the Market for Therapeutic Use
Agastya Haritaki Avaleha used in serious and chronic respiratory illness is a personalised classical medicine and not a general health product. A ready-made market preparation is manufactured in a fixed composition and fixed dose for mass use, whereas in clinical Ayurveda the formulation is always selected after examining Prakriti, Bala, Agni, stage of disease, tissue depletion, and ongoing treatments. When these factors are ignored the Avaleha becomes either too heavy to digest, poorly absorbed, incompatible with the patient’s condition, or therapeutically ineffective. Therefore a patient should never expect disease-level benefit from an over-the-counter product.
Absence of Yukti-Based Individualisation
In classical Chikitsa the medicine is designed according to the individual and not according to the disease name alone. Two patients with the same diagnosis may receive different doses, different adjuvants, different Sneha proportion, or different Rasayana combinations. Market products cannot adjust for Vata-dominant tissue depletion, Pitta-dominant inflammatory state, Kapha-dominant mucus obstruction, low Agni, or severe cachexia. Because this individualisation is missing, the Avaleha fails to act at the Dhatu level.
Disease Stage Mismatch
The requirement of a patient in early functional decline is completely different from that of a patient with long-standing weight loss, severe breathlessness, active inflammation, or recovery phase after intensive therapy. In many advanced cases Deepana and Pachana must be done first, Rasayana must be introduced gradually, mineral support may be delayed, and dose must be titrated. A fixed commercial product cannot adapt to these stages and therefore does not produce the expected effect.
Digestive Capacity Is Not Assessed
Avaleha is Guru and Brimhana in nature and requires adequate Agni for proper digestion and absorption. In Mandagni it produces Ama, bloating, anorexia, heaviness, and coating of channels instead of nourishing tissues. Classical physicians first assess Jatharagni and Dhatvagni and only then introduce Rasayana in a suitable dose. Without this step even the best formulation becomes ineffective.
No Stage-Specific Mineral Rasayana Integration
In advanced depletion carefully selected micro-doses of Swarna Bhasma, Heerak Bhasma, Abhraka Bhasma, Swarna Makshika, Pravala, Mukta, or Lauha may be required for Ojas, metabolic activation, haematinic support, and tissue regeneration. These are never added in a routine manner and their dose depends on strength, digestion, inflammatory status, and current therapy. Market products either do not contain them, contain them in non-indicated combinations, or contain them in forms that are not clinically processed for absorption.
Improper Classical Processing in Commercial Preparations
The therapeutic potency of Avaleha depends on correct Kashaya preparation, proper reduction, precise Avaleha paka stage, correct Sneha integration, and addition of Madhu only after cooling. In mass production these steps are often altered for shelf stability and speed, which reduces bioavailability, increases heaviness, and diminishes Rasayana effect at the tissue level.
Incompatibility With Ongoing Modern Treatment
Patients undergoing chemotherapy, immunotherapy, targeted therapy, or radiation require specific timing, dose adjustment, liver function monitoring, and digestion assessment. Self-use of a market product without medical coordination may reduce tolerance instead of improving it because the formulation is not synchronised with treatment cycles and recovery phases.
Patient Factors That Decide Whether the Avaleha Will Work
Age
Elderly patients have lower Agni and reduced metabolic reserve and therefore require smaller doses, different Sneha proportion, and gradual Rasayana introduction, whereas younger patients with stronger digestion can tolerate classical dosing.
Associated Chronic Diseases
Conditions such as diabetes, severe anaemia, liver dysfunction, renal impairment, autoimmune disorders, and metabolic syndrome alter digestion, tissue nutrition, and drug metabolism and therefore require modification of the Avaleha composition and dose.
Duration of Illness
Early-stage tissue depletion responds faster whereas long-standing disease requires preparatory Deepana-Pachana, gradual Brimhana, phased Rasayana, and longer duration of therapy.
Strength and Body Weight
In severe cachexia full-dose Avaleha cannot be digested initially and must be introduced in a graded manner after metabolic correction.
Agni Status
Agni is the most decisive factor. Without correcting Agni first Rasayana cannot reach the Dhatu and will not produce strength, weight gain, or respiratory improvement.
Dominant Symptom Pattern
Breathlessness-dominant presentation, inflammatory phase with heat and irritation, Kapha-dominant mucus obstruction, and Vata-dominant dryness and wasting all require different modifications in the formulation and adjuvant.
Warning Against Self-Preparation
Preparing this Avaleha without classical training leads to incorrect Kashaya concentration, wrong Avaleha paka, improper Sneha integration, incorrect temperature during Madhu addition, and inaccurate herb proportion. These errors destroy the Rasayana property and may make the formulation difficult to digest.
Mandatory Medical Supervision
Agastya Haritaki Avaleha for therapeutic use must always be prescribed after clinical examination, matched to digestion and strength, modified according to stage, and regularly monitored. This personalised approach is the essence of Yukti-Vyapashraya Chikitsa and is the reason why the same formulation produces profound benefit in one patient and no effect in another when used without supervision.
Timing Matters in Personalized Oncology Support
In the journey of cancer treatment, the question is no longer if integrative care should be used—but when and how. Ayurveda, as a holistic medical science, offers profound therapeutic value when aligned with the body’s healing rhythms. However, timing is critical. The effectiveness and safety of Ayurvedic intervention depend not only on the patient’s constitution and stage of cancer but also on the phase of conventional treatment they’re undergoing—whether it’s surgery, chemotherapy, radiation, or remission.
During active chemotherapy or radiation, the body is in a state of high oxidative stress, inflammation, and immune suppression. At this stage, Ayurveda focuses primarily on supportive care—preserving digestive strength (Agni), protecting Ojas (vital energy), and reducing side effects like nausea, mucositis, fatigue, and anxiety. Gentle herbs such as Yashtimadhu (licorice), Guduchi (Tinospora), Triphala, Shatavari, and Brahmi are introduced in carefully monitored doses. These do not interfere with cytotoxic treatments but work to buffer their impact on the gut, liver, nerves, and mood.
What is strictly avoided during active treatment are strong Rasayana or metal-based Bhasmas, unless used under extremely precise conditions and supervision. The body’s detox and excretion systems are already overwhelmed; adding potent formulations too early may lead to unintended interactions or burden.
Post-treatment, when conventional therapies have ended, the body often enters a phase of exhaustion, poor digestion, cognitive fog, and emotional depletion—what many call the “rebuilding window.” This is the ideal time for deeper Ayurvedic integration. Here, the goals shift toward detoxification (Shodhana), tissue repair (Dhatu Pushti), and immune terrain restoration (Ojas building). Depending on the strength (Bala) and digestion (Agni), personalized Panchakarma therapies may be introduced: Virechana (purgation), Nasya (nasal clearing), mild Basti (enemas) or Ama Pachana protocols like light fasting, digestive teas, and detox diets.
Once cleansing is complete and stability is restored, the patient can begin Rasayana phase—long-term rejuvenation using formulations such as Chyawanprash, Ashwagandha Avaleha, Swarna Bhasma in microdose, or Abhrak-based preparations designed to nourish mitochondria, rebuild tissue, and enhance adaptive immunity. This phase may last several months to a year, depending on the cancer type, treatment impact, and recurrence risk.
Importantly, integration must be personalized. Some patients benefit from Ayurveda during treatment, others post-treatment, and some only during the recovery phase. This decision is based on their Prakriti, cancer staging, emotional state, digestive strength, comorbidities, and willingness to commit to a comprehensive healing protocol.
Coordination with the oncology team is also essential. The goal is not to replace, but to complement, avoiding herb-drug interactions and maintaining a transparent, collaborative approach. Patients who use Ayurveda without guidance during active treatment may unknowingly create contradictions—while those who wait too long may miss the window where terrain correction is most effective.
In conclusion, Ayurveda is not a static alternative—it is a dynamic, timing-sensitive support system. When properly phased into a patient’s journey, it offers protection during treatment, nourishment after treatment, and regeneration for the long term. Its strength lies not just in what it offers, but in when and how it is offered.
Why One Formula Doesn’t Fit All in Ayurvedic Oncology
One of the most profound strengths of Ayurveda lies in its refusal to generalize. While modern medicine often applies standardized protocols across all patients with the same cancer type, Ayurveda insists that no two individuals with the same diagnosis have the same disease process. The treatment must therefore be designed around the individual—not just the tumor. This is where the concept of Prakriti (constitutional type) and Vikriti (disease deviation) becomes central.
Prakriti reflects the unique balance of Vata, Pitta, and Kapha that governs a person’s physiology, psychology, metabolism, and immune profile from birth. Lung cancer in a Vata-dominant individual may manifest as dryness in the chest, weakness, anxiety, weight loss, and sleep disruption. In contrast, the same condition in a Kapha-dominant person may present as mucus congestion, fluid retention, sluggish digestion, and slow metabolic response. In Pitta types, the cancer may grow aggressively, accompanied by inflammation, bleeding, irritability, and burning sensations.
Each of these profiles requires a different therapeutic strategy. A Vata-predominant patient may benefit from nourishing Rasayanas, medicated ghee, nervine herbs like Ashwagandha and Bala, and warm, grounding dietary interventions. A Kapha profile calls for deeper detoxification (Shodhana), Kapha-reducing herbs like Trikatu, Guggulu, Pushkarmool, and Vasa, and lighter, mucolytic nutrition. Pitta types may require cooling anti-inflammatory agents like Amalaki, Guduchi, Yashtimadhu, and a pitta-pacifying diet.
Additionally, Ayurveda doesn’t just personalize by constitution—it customizes by stage of cancer and strength of the patient (Bala). A Stage I or II patient with strong digestion and mental clarity may tolerate stronger detox regimens and early Rasayana. A Stage III or IV patient, or one undergoing chemotherapy, may need gentler interventions focused on preserving Agni and stabilizing Ojas before deeper therapies are attempted. Patients in remission may benefit from seasonal Rasayana, cyclical fasting, or low-dose Swarna Prashan to maintain immune terrain.
This adaptive model of care also integrates comorbidities. For example, if the patient has diabetes, Kapha-reducing Rasayanas and non-sugar-based Avalehas are preferred. If liver function is compromised, hepatoprotective agents like Bhumi Amalaki and Kalmegh are introduced. If anxiety dominates the clinical picture, Vata-calming rituals and medhya herbs like Brahmi and Shankhpushpi are emphasized.
This precision extends to dosage, timing, anupana (carrier substances), and even herb combinations, which are all adjusted based on digestive strength, season, daily routine, sleep pattern, and psychological profile.
In conclusion, Ayurvedic oncology does not offer a one-size-fits-all formula—it offers a living protocol that changes with the person’s condition, strength, constitution, and response. It is this level of personalization, rooted in centuries of clinical observation and refined through modern integration, that positions Ayurveda as not just an alternative but a strategic, adaptable partner in the long-term healing of cancer.
Common reasons lung cancer patients explore integrative treatment:
• Recurrence after initial therapy
• Drug resistance
• Severe treatment side effects
• Progressive weakness and weight loss
• Desire for better quality of life
• Need for a personalised treatment plan
FAQs (Frequently Asked Questions)
When do lung cancer patients usually start looking for alternative or integrative treatment?
Most patients begin exploring broader supportive approaches when standard therapies start causing severe fatigue, loss of appetite, breathlessness, or when scan results show recurrence or limited response. At this stage, the priority often shifts from tumour reduction alone to maintaining strength, treatment tolerance, and quality of life.
Is integrative oncology used instead of chemotherapy or together with it?
A medically supervised integrative approach is designed to work alongside chemotherapy, immunotherapy, targeted therapy, or radiation. Its purpose is to improve the body’s ability to tolerate treatment, recover faster between cycles, and remain fit enough to continue essential oncology care.
Can integrative care help in stage IV lung cancer?
In advanced stages, the main clinical goals are disease control, symptom relief, preservation of strength, and better day-to-day functioning. Integrative support focuses on improving appetite, stabilising weight, reducing fatigue, supporting breathing capacity, and enhancing overall resilience so that meaningful survival is improved.
Why do some patients stop responding to chemotherapy or targeted therapy?
Cancer cells can adapt over time through genetic and metabolic changes, leading to drug resistance. With each subsequent line of treatment, the duration of response may become shorter and side effects may increase. This is one of the most common reasons patients begin looking for additional supportive strategies.
Does exploring an integrative approach mean a patient is giving up modern treatment?
No. In most cases, patients seek integrative care because they want to continue their oncology treatment for as long as possible but are physically unable to tolerate it. The aim is to strengthen the body so that ongoing medical therapy can be continued more effectively.
Which lung cancer patients benefit the most from integrative support?
Patients with advanced disease, recurrence after initial treatment, severe treatment-related weakness, progressive weight loss, poor appetite, persistent fatigue, or reduced functional capacity often experience the most visible improvement when supportive care is introduced at the right time.
Can integrative care improve quality of life during lung cancer treatment?
Yes. Patients commonly report better sleep, improved appetite, increased walking capacity, reduced exhaustion, and improved emotional stability. These functional outcomes are clinically important because they directly influence treatment continuity and overall survival.
Is this approach suitable for international patients?
A structured integrative plan can be developed through a detailed review of medical reports, treatment history, and current symptoms. This allows stage-specific recommendations that remain aligned with the patient’s ongoing oncology care in their home country.
When is the best time to start integrative support in lung cancer?
The greatest benefit is seen when supportive care is introduced at the first signs of physical decline, treatment intolerance, or progressive weakness. Starting early helps patients remain eligible for life-prolonging therapies for a longer period.
What is the main goal of an integrative approach in lung cancer?
The primary objective is to help patients remain strong enough to continue necessary treatment, maintain independence in daily activities, improve symptom control, and extend meaningful survival with better quality of life.
References
- Aggarwal, B. B., Sundaram, C., Malani, N., & Ichikawa, H. (2007). Curcumin: The Indian solid gold. Advances in Experimental Medicine and Biology, 595, 1–75. https://doi.org/10.1007/978-0-387-46401-5_1
- Balachandran, P., & Govindarajan, R. (2005). Cancer—An ayurvedic perspective. Pharmacological Research, 51(1), 19–30. https://doi.org/10.1016/j.phrs.2004.04.005
- Gupta, S. C., Patchva, S., & Aggarwal, B. B. (2013). Therapeutic roles of curcumin: Lessons learned from clinical trials. The AAPS Journal, 15(1), 195–218. https://doi.org/10.1208/s12248-012-9432-8
- Kaushik, D., Kumar, A., Kaushik, P., & Rana, A. C. (2018). Immunomodulatory potential of Tinospora cordifolia: A review. Journal of Immunology Research, 2018, 1622607. https://doi.org/10.1155/2018/1622607
- Reiche, E. M. V., Nunes, S. O. V., & Morimoto, H. K. (2004). Stress, depression, the immune system, and cancer. The Lancet Oncology, 5(10), 617–625. https://doi.org/10.1016/S1470-2045(04)01597-9
- Sengar, M., Juneja, S., & Noronha, V. (2020). Integrative oncology: Need of the hour. South Asian Journal of Cancer, 9(2), 85–87. https://doi.org/10.1055/s-0040-1711494
- Singh, N., Bhalla, M., de Jager, P., & Gilca, M. (2011). Withania somnifera (Ashwagandha): A rejuvenating herbal medicine. Pharmacognosy Reviews, 5(9), 82–86. https://doi.org/10.4103/0973-7847.79101
- Touchefeu, Y., Montassier, E., Nieman, K., Gastinne, T., Potel, G., Bruley des Varannes, S., … & Le Vacon, F. (2014). Systematic review: The role of the gut microbiota in chemotherapy- or radiation-induced gastrointestinal mucositis. Alimentary Pharmacology & Therapeutics, 40(5), 409–421. https://doi.org/10.1111/apt.12881
- Tripathi, Y. B., & Sharma, M. (2010). The interaction between Rasayana drugs and mitochondria: A role in cancer therapy. AYU, 31(4), 515–520. https://doi.org/10.4103/0974-8520.82038
- Goel, A., Kunnumakkara, A. B., & Aggarwal, B. B. (2008). Curcumin as “Curecumin”: From kitchen to clinic. Biochemical Pharmacology, 75(4), 787–809. https://doi.org/10.1016/j.bcp.2007.08.016
- Jagetia, G. C., & Aggarwal, B. B. (2007). “Spicing up” of the immune system by curcumin. Journal of Clinical Immunology, 27(1), 19–35. https://doi.org/10.1007/s10875-006-9066-7
- Borchers, A. T., Hackman, R. M., Keen, C. L., Stern, J. S., & Gershwin, M. E. (1997). Complementary medicine: A review of immunomodulatory effects of botanicals. American Journal of Clinical Nutrition, 66(6), 1402S–1406S. https://doi.org/10.1093/ajcn/66.6.1402S
- Chatterjee, A., & Pakrashi, S. C. (1997). The Treatise on Indian Medicinal Plants (Vol. 1–6). Publications and Information Directorate, CSIR.
- Kumar, D., Arya, V., Kaur, R., Bhat, Z. A., Gupta, V. K., & Kumar, V. (2012). A review of immunomodulators in the Indian traditional health care system. Journal of Microbiology, Immunology and Infection, 45(3), 165–181. https://doi.org/10.1016/j.jmii.2011.09.030
- Pandey, M. M., Rastogi, S., & Rawat, A. K. S. (2013). Indian traditional Ayurvedic system of medicine and nutritional supplementation. Evidence-Based Complementary and Alternative Medicine, 2013, 1–12. https://doi.org/10.1155/2013/376327
- Sundaram, C., & Aggarwal, B. B. (2011). Anticancer properties of curcumin: Evidence from laboratory to clinical studies. Anticancer Research, 31(10), 3633–3655. https://pubmed.ncbi.nlm.nih.gov/21965684/
- Kuttan, R., Sudheeran, P. C., & Josph, C. D. (1990). Turmeric and curcumin as topical agents in cancer therapy. Tumori Journal, 76(5), 431–432. https://doi.org/10.1177/030089169007600511
- Kumar, A., & Kaushik, V. (2022). Ayurvedic management of stage IV lung cancer with classical and Rasayana therapy: A case study. Journal of Ayurveda and Integrative Medicine. https://doi.org/10.1016/j.jaim.2021.10.010
- Kumar, N., Singh, B., Singh, D., & Singh, H. (2020). Herbal medicines for cancer therapy in Ayurveda: A review. Journal of Herbal Medicine, 21, 100324. https://doi.org/10.1016/j.hermed.2020.100324
- Sarma, S. P., & Sengupta, A. (2013). Abhrak Bhasma: A herbo-metallic preparation of Ayurveda. Indian Journal of Traditional Knowledge, 12(3), 398–403. http://nopr.niscpr.res.in/handle/123456789/22238
- Mishra, L. C., Singh, B. B., & Dagenais, S. (2001). Scientific basis for the therapeutic use of Withania somnifera (Ashwagandha): A review. Alternative Medicine Review, 6(3), 334–346. https://www.altmedrev.com/archive/publications/6/3/334.pdf
- Bani, S., Gautam, M., Sheikh, F. A., et al. (2002). Selective Th1 up-regulating activity of Withania somnifera aqueous extract in an experimental system using flow cytometry. Journal of Ethnopharmacology, 75(2–3), 231–239. https://doi.org/10.1016/S0378-8741(01)00497-0
- Gautam, M., Diwanay, S., Gairola, S., & Patwardhan, B. (2004). Immune response modulation to DPT vaccine by aqueous extract of Withania somnifera in experimental system. International Immunopharmacology, 4(6), 841–849. https://doi.org/10.1016/j.intimp.2004.02.005
- Baliga, M. S., & Dsouza, J. J. (2011). Amla (Emblica officinalis Gaertn), a wonder berry in the treatment and prevention of cancer. European Journal of Cancer Prevention, 20(3), 225–239. https://doi.org/10.1097/CEJ.0b013e32834473f4






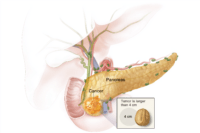




5 Responses
Thanks.
Cet article m’a vraiment permis de mieux comprendre pourquoi de nombreux patients atteints de cancer du poumon se tournent vers les thérapies alternatives. Il met en lumière le rôle essentiel de ces approches pour améliorer la qualité de vie, en complément des traitements conventionnels.
J’ai particulièrement apprécié la mise en garde sur les dangers d’abandonner la médecine traditionnelle, ainsi que les conseils pour intégrer des pratiques comme le yoga, l’acupuncture ou encore la phytothérapie de manière encadrée.
Merci pour votre commentaire réfléchi. Il est encourageant de savoir que cet article vous a aidé à mieux comprendre pourquoi de nombreux patients atteints de cancer du poumon choisissent les thérapies alternatives dans leur parcours de soins. Comme vous l’avez souligné, des approches comme le yoga, l’acupuncture et la phytothérapie peuvent jouer un rôle essentiel dans l’amélioration du bien-être global, en complément des traitements médicaux classiques.
Nous apprécions également votre reconnaissance de l’importance de ne pas abandonner la médecine conventionnelle. Intégrer les thérapies complémentaires de manière encadrée permet d’en maximiser les bienfaits en toute sécurité. C’est cette approche équilibrée et fondée sur les preuves qui guide notre travail autour des soins intégratifs contre le cancer.
Thank you for your insightful comment. It’s encouraging to hear that the article helped clarify why many lung cancer patients choose alternative therapies as part of their healing process. As you noted, approaches like yoga, acupuncture, and phytotherapy can play a powerful role in improving overall well-being when used alongside conventional treatments.
We also appreciate your recognition of the important reminder not to abandon standard medical care. Integrating complementary therapies with guidance ensures safety and maximizes benefits. This balanced, evidence-informed approach is at the heart of what we aim to share through our work on integrative cancer care.
Achei interessante esse artigo,ensina muito sobre terapia alternativa para cura do câncer de pulmão,e como pode ajudar bastante as pessoas
Agradecemos sinceramente pelo seu comentário. Este artigo mostra como a cura do câncer de pulmão pode ser abordada de forma científica e personalizada através da Ayurveda. Não se trata de oferecer esperança vaga, mas de aplicar protocolos ayurvédicos com base em evidências clínicas, adaptados ao estado de saúde de cada paciente. Utilizamos plantas medicinais, minerais purificados e Rasayana terapias para promover a cura real e sustentável. Continue acompanhando nosso blog para mais conteúdos sobre cura natural, imunidade e ciência ayurvédica.
Thank you sincerely for your comment. This article highlights how lung cancer can be cured using scientific and personalized Ayurvedic methods. We are not offering vague hope — our protocols are clinically validated and tailored to each patient’s health condition. By using medicinal herbs, purified minerals, and Rasayana therapies, we aim for real, sustainable cures through Ayurveda. Stay connected with our blog for more content on natural cures, immunity, and the science of Ayurveda.