- Common Penile Disorders
- Congenital Abnormalities of the Penis
- Other Common Systemic Disorders
- Metabolic disorders that commonly coexist
- Endocrine and hormonal disorders associated with penile disorders
- Neurologic and spinal disorders that can present as penile symptoms
- Genitourinary disorders frequently associated with penile complaints
- Dermatologic and inflammatory disorders involving the penis
- Infectious disorders that can be associated with penile symptoms
- Sexual function disorders and psychosexual associations
- Medication and substance related disorders
- Hematologic and systemic disorders that are rare but high risk
- Connective tissue and fibrotic disorders linked to penile curvature and pain
- Congenital and structural disorders that may be missed
- Cancer related associations that must be screened for
- Trauma and iatrogenic associations
- Symptoms to Watch For
- Underlying Causes
- Diagnostic Tools in Modern Medicine
- Ayurvedic Understanding of Penile Disorders
- Ayurvedic Herbs and Rasayanas Used
- Main Medicine- Musalyadi Vrishya Avaleha (Ayurvedic)
- Who this medicine is for in the UK, USA, Canada, and Australia
- The key factors that decide results, not only the medicine
- How to take Musalyadi Vrishya Avaleha
- Musalyadi Avaleha for Penile Disorders
- Safety Warning for Patients
- Modern Treatment Approaches
- Preventive Tips and Sexual Health Hygiene
- Patient Case Studies
- FAQs
- References
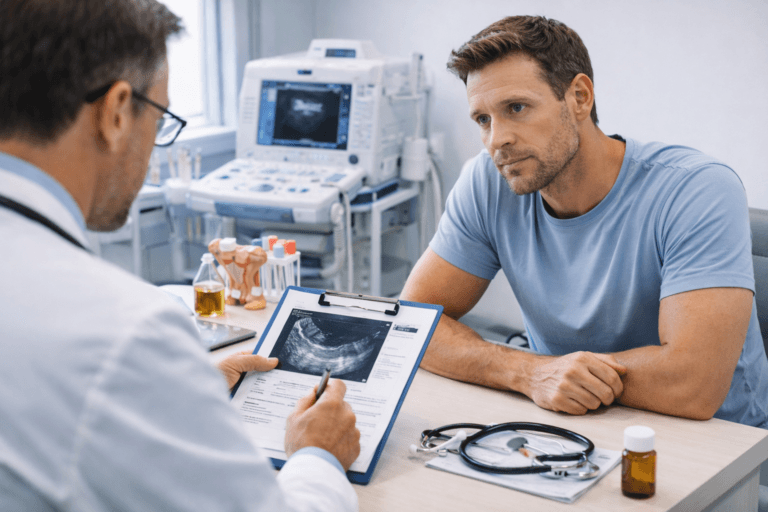
Penile disorders are a group of conditions that affect the structure, function, or appearance of the penis, often resulting in significant sexual, urinary, and psychological challenges. In this article, titled Penile Disorders – Symptoms, Causes, Diagnosis & Ayurvedic Cure, we will explore how these conditions are far more than physical discomfort—they are indicators of deeper systemic imbalances, both in modern biomedical terms and through the lens of Ayurvedic science. From pain and inflammation to sexual dysfunction and structural deformities, penile disorders can silently erode a man’s quality of life if not addressed early [1].
Modern medicine typically classifies penile conditions under urology and offers treatments ranging from antifungal creams to complex surgeries. However, many patients experience only symptomatic relief without true resolution. In contrast, Ayurveda views penile disorders as the result of Shukra Dhatu Kshaya (reproductive tissue depletion), Ojas (vital energy) compromise, and Srotorodha (blockage in the subtle channels), often triggered by poor diet, chronic stress, suppression of natural urges, or excessive sexual activity [2].
What is often overlooked is the role of metabolic, emotional, and neurovascular factors. Lesser-known causes include sleep deprivation, history of trauma, post-viral fatigue, and long-standing lifestyle errors. These may not show up in standard lab reports but can still deeply affect penile health. Ayurveda recognizes these subtleties and treats them by rejuvenating the body’s internal environment through Rasayana therapy and gentle detoxification (Shodhana) [3].
This integrative perspective—combining diagnostics, individualized formulations, and restorative therapies—offers not just temporary relief but the potential for deep healing. In the sections ahead, we will detail each type of penile disorder, its symptoms, root causes, modern diagnostic tools, and evidence-based Ayurvedic treatments that aim to restore function and confidence holistically.
Common Penile Disorders
Penile disorders can vary widely in presentation, from mild irritation to severe deformity or dysfunction. While some are caused by infections or trauma, others are linked to systemic conditions like diabetes or autoimmune dysfunction. This section outlines both well-known and lesser-known penile disorders, helping patients and clinicians recognize early warning signs and seek timely intervention [4].
Phimosis
Phimosis refers to the condition where the foreskin (prepuce) of the penis cannot be fully retracted over the glans. While it is physiologically normal in newborns and young boys, persistent phimosis into adolescence or adulthood is considered pathological. Common symptoms include pain during erection, ballooning of the foreskin while urinating, repeated infections (balanitis), and hygiene difficulties. In severe cases, it can lead to urinary obstruction or even kidney infections if left untreated.
Phimosis is commonly associated with poor hygiene, chronic inflammation, diabetes mellitus, or repeated infections that cause scarring and tightening of the foreskin. In some cases, it may be congenital or occur due to aggressive pulling in childhood. Circumcision is the most widely practiced surgical solution. However, topical steroid creams are sometimes used to soften the foreskin in mild cases.
In Ayurvedic medicine, phimosis may be viewed as a manifestation of Srotorodha (obstruction of microchannels) involving the Shukravaha and Mutravaha Srotas. It is typically governed by Kapha and Vata vitiation, leading to tissue stiffness, dryness, and localized constriction. Ayurvedic treatment includes internal Vata-Kapha pacifying herbs, external oil application (e.g., Bala Taila), mild fomentation, and in chronic cases, the use of Rasayana therapies to restore tissue elasticity. Herbal support may involve the use of Gokshura, Yashtimadhu, and Gandhak Rasayan to address inflammation and facilitate natural softening of the tissue [5].
Paraphimosis
Paraphimosis is a urological emergency characterized by the retracted foreskin being trapped behind the glans penis and unable to return to its normal position. This causes a tight constricting band around the penis, leading to rapid swelling, impaired lymphatic and venous return, and if untreated, potential ischemia or gangrene. It is most commonly seen in uncircumcised males and may occur after medical procedures such as catheterization, improper hygiene practices, or forced retraction of a tight foreskin.
Clinically, patients present with a swollen, painful glans and a tight band of foreskin behind it. If left untreated, the condition can compromise blood flow and lead to necrosis. Immediate manual reduction with lubrication or osmotic methods (e.g., sugar application) is preferred. In severe cases, a dorsal slit or emergency circumcision may be required.
From an Ayurvedic perspective, paraphimosis reflects an acute Vata aggravation along with Rakta Dushti (vitiation of blood). The sudden displacement and painful swelling signify disturbed Apana Vayu in the Shukravaha Srotas. Management may involve internal Vata–Pitta pacifying herbs, anti-inflammatory formulations like Nimba or Yashtimadhu, and local applications with soothing oils such as Jatyadi Taila or Bala Taila. Fomentation with medicated decoctions (e.g., Dashamoola) may help reduce edema. Rasayana herbs are later introduced to repair tissue damage and prevent fibrosis [6].
Balanitis and Balanoposthitis
Balanitis is inflammation of the glans penis, while balanoposthitis refers to inflammation involving both the glans and the foreskin. It is one of the most common penile disorders across all age groups and can present with redness, burning, itching, swelling, foul-smelling discharge, pain during urination, and difficulty retracting the foreskin. If recurrent, it can lead to phimosis.
Balanitis may be caused by bacterial or fungal infections (especially Candida albicans), poor genital hygiene, use of irritating soaps, uncontrolled diabetes, or sexually transmitted infections like herpes or gonorrhea. Risk factors include obesity, tight foreskin, and immunosuppression. Treatment involves improving hygiene, antifungal or antibiotic creams, and blood sugar control in diabetic patients.
In Ayurveda, balanitis is correlated with Shukravaha Srotas Dushti, typically involving Pitta and Kapha doshas. The burning and inflammation signify Pittaja Vrana, while thick discharge and white patches reflect Kaphaja Upalepa. Herbs such as Nimba (Azadirachta indica), Triphala, Haridra (Turmeric), and Daruharidra are used both internally and externally. Decoctions like Triphala Kashayam can be used for gentle washing, while Panchatikta Guggulu Ghrita may be prescribed to purify Rakta and support healing. In chronic cases, Rasayana therapy is initiated to improve local immunity and tissue strength [7].
Peyronie’s Disease
Peyronie’s disease is a condition characterized by the development of fibrous plaques within the tunica albuginea of the penis, resulting in abnormal curvature during erection. This curvature can cause pain, erectile dysfunction, and emotional distress, often leading to impaired sexual function and psychological consequences such as anxiety and depression. While the exact cause is unknown, minor trauma or repeated microvascular injury during intercourse is believed to play a role, triggering an abnormal wound-healing response and collagen deposition.
It typically affects middle-aged and older men and may progress over time. Early treatment includes oral antioxidants, intralesional injections (e.g., collagenase), and traction therapy. Surgery is reserved for severe, nonresponsive cases with functional impairment.
Ayurveda describes Peyronie’s-like conditions under Vata–Rakta Vyadhi (a disorder of Vata and vitiated blood), where the channels (Srotas) lose their elasticity due to chronic inflammation and Vata dominance. Ayurvedic management includes systemic use of herbs like Guggulu (Commiphora mukul), Ashwagandha, and Rasayanas such as Chyawanprash or Swarna Bhasma to restore structural integrity. External application of medicated oils (e.g., Mahanarayan Taila) combined with Abhyanga (massage) and Swedana (fomentation) help reduce fibrosis and improve tissue pliability. Internal therapies aim at reducing Rakta Dushti and supporting connective tissue healing [8].
Penile Fracture
Penile fracture is a rare but serious injury involving rupture of the tunica albuginea, the fibrous sheath surrounding the corpora cavernosa, typically occurring during vigorous sexual activity or masturbation. Patients often report hearing a sudden “crack” or “pop” sound, followed by intense pain, immediate loss of erection, swelling, and bruising. This is a surgical emergency and requires immediate intervention to prevent long-term complications such as penile curvature, erectile dysfunction, or urethral injury.
If diagnosed promptly, surgical repair yields good outcomes. Delay in treatment, however, increases the risk of fibrosis and sexual dysfunction. Diagnosis is clinical but may be supported by ultrasound or MRI in uncertain cases.
In Ayurveda, penile fracture is categorized under Abhighataja Vata Vyadhi (trauma-induced disorders dominated by aggravated Vata). Sudden rupture and pain reflect Vata prakopa, which disturbs the structure and function of the penile Srotas. Management includes Snehan (oleation) with medicated ghee like Shatavari Ghrita, Swedana with Dashamoola decoction, and Rasayana formulations like Ashwagandha, Shilajit, and Heerak Bhasma in recovery. Herbal pastes or oils may also be used locally to aid in pain management and tissue regeneration. Post-operative Ayurvedic rehabilitation can enhance healing and reduce scar tissue formation [9].
Priapism
Priapism is a pathological condition defined by a prolonged penile erection lasting more than four hours that is unrelated to sexual stimulation. It is categorized into two main types: ischemic (low-flow) and non-ischemic (high-flow). Ischemic priapism is far more common and poses a medical emergency due to the risk of tissue necrosis and permanent erectile dysfunction if not treated immediately. The affected individual often experiences a rigid penile shaft with a soft glans, accompanied by significant pain and discomfort. Immediate medical intervention is required to restore blood flow, typically through aspiration, intracavernosal injection of sympathomimetics, or surgical shunting.
Causes of priapism include sickle cell anemia, leukemia, spinal cord injuries, perineal trauma, and medications such as antidepressants, erectile dysfunction drugs, and antipsychotics. In pediatric cases, priapism may be the first sign of an underlying hematologic disorder. The pathophysiology involves impaired venous outflow from the corpora cavernosa, leading to ischemia and stasis of deoxygenated blood.
Ayurveda interprets priapism through the lens of Vata–Pitta aggravation in the Shukravaha Srotas and Apana Vayu dysfunction. The rigidity and prolonged erection align with Vata prakopa, while the pain and heat indicate Pittaja involvement. Classical references describe similar symptoms under Stambha Vajikarana Vyadhi, particularly in conditions related to improper sexual conduct or excess indulgence. Treatment involves pacifying Vata and Pitta using internal formulations like Chandraprabha Vati, Ashwagandha Rasayana, and Kamadudha Ras with Mukta Pishti. Panchakarma interventions such as Snehana, Virechana (purgation), and medicated Basti (enema) may be considered in long-term cases to prevent recurrence and improve reproductive tissue health. External cooling therapies using Shatadhauta Ghrita or Kumari Taila are traditionally applied for symptom relief [10].
Erectile Dysfunction (ED)
Erectile Dysfunction (ED) is defined as the consistent or recurrent inability to attain or maintain an erection sufficient for satisfactory sexual performance. It is one of the most common male sexual disorders, affecting an estimated 30–50% of men over the age of 40 globally. The condition has significant implications beyond the bedroom, including emotional distress, strained relationships, low self-esteem, and often undiagnosed systemic diseases such as diabetes, cardiovascular dysfunction, and hormonal imbalances.
The etiology of ED is multifactorial. Organic causes include vascular insufficiency, neurogenic disorders, hormonal deficiencies (especially low testosterone), pelvic surgeries, and side effects from medications like beta-blockers and antidepressants. Psychogenic causes involve stress, anxiety, depression, or relationship issues. Lifestyle factors such as smoking, alcohol use, obesity, and lack of exercise are also known contributors. Diagnosis involves a thorough history, physical examination, nocturnal penile tumescence testing, hormonal assays, and sometimes penile Doppler ultrasound.
In Ayurveda, ED is referred to as Klaibya, with several subtypes:
- Dhatukshaya Klaibya (due to tissue depletion),
- Manasika Klaibya (due to psychological stress),
- Shukrakshaya Klaibya (loss of semen vitality),
- Aghatajanya Klaibya (trauma-induced).
Ayurvedic treatment aims to restore Shukra Dhatu, rejuvenate the nervous system, and pacify aggravated Vata in the Apana Vayu domain. Rasayana formulations such as Ashwagandha Churna, Kapikacchu Beeja, Shilajit, Vrishya Vati, and Svarna Bhasma are commonly used. Panchakarma therapies like Basti (especially Yapana Basti) are prescribed to nourish the reproductive tissues. Medicated oils like Bala Taila are used externally for penile Abhyanga, enhancing blood flow and sensitivity. Unlike symptomatic drugs like sildenafil, Ayurvedic therapy aims to cure the root imbalances and offer long-term restoration of potency and confidence [11].
Penile Cancer
Penile cancer is a rare but aggressive malignancy that primarily affects the skin and tissues of the penis, most often in the form of squamous cell carcinoma. It accounts for less than 1% of male cancers in developed countries but has a higher prevalence in regions with poor genital hygiene and limited access to healthcare. The disease typically presents as a painless ulcer, growth, or thickening on the glans or foreskin, often associated with foul-smelling discharge, bleeding, or inguinal lymph node enlargement.
Risk factors for penile cancer include chronic phimosis, poor hygiene, human papillomavirus (HPV) infection ,particularly types 16 and 18, smoking, and a history of lichen sclerosus or balanitis. Men who are uncircumcised and do not maintain proper hygiene are at significantly greater risk. Diagnosis involves biopsy of the lesion, imaging for staging, and histopathological examination to determine grade and invasiveness. Early-stage cancers can be treated with local excision or laser therapy, while advanced stages may require partial or total penectomy and lymphadenectomy.
Ayurvedic medicine classifies such malignant lesions under the categories of Arbuda (malignant tumor) or Dushta Vrana (chronic non-healing wound), particularly when there is ulceration, foul odor, and irregular growth. The involvement of Rakta, Mamsa, and Shukra Dhatus is considered significant. Treatment begins with Shodhana (detoxification) using procedures like Virechana and Raktamokshana to cleanse the blood. Herbal preparations such as Kanchanar Guggulu, Triphala Guggulu, and Varunadi Kashayam are used to target abnormal tissue growth. External application of Neem, Haridra, and Gandhak-based formulations may aid in wound care. Rasayanas like Swarna Bhasma and Heerak Bhasma are employed in advanced care for immunomodulation and tissue regeneration. A combined strategy of internal purification, local wound care, and immune support provides a promising complementary approach in early-stage disease or post-surgical recovery [12].
Congenital Abnormalities of the Penis
Congenital abnormalities of the penis refer to anatomical malformations present at birth that may affect urinary function, sexual capability, or reproductive potential later in life. Though some anomalies are externally visible, others may remain undiagnosed until puberty or adulthood. These conditions often cause psychological distress and require multidisciplinary care involving pediatric urologists, endocrinologists, and sometimes fertility specialists.
Hypospadias is one of the most common defects, where the urethral opening is located on the underside of the penis instead of the tip. It may be associated with penile curvature (chordee) and incomplete foreskin. Surgical correction is usually performed in infancy to restore both cosmetic appearance and functionality.
Epispadias, though rarer, involves the urethral opening being located on the dorsal (upper) surface of the penis and is often part of a complex condition called bladder exstrophy. It can cause severe urinary incontinence if left untreated.
Micropenis is defined as a normally formed penis that is significantly smaller in length—typically more than 2.5 standard deviations below the mean for age. Causes include congenital hypogonadism, pituitary hormone deficiencies, and genetic disorders. Early hormone therapy may help stimulate growth.
From an Ayurvedic standpoint, these anomalies fall under the umbrella of Sahaja Vyadhi (congenital diseases) caused by doshic imbalance during intrauterine development, often due to maternal diet, emotional state, or genetic predisposition. Ayurveda emphasizes Garbhini Paricharya (prenatal care) for preventing such conditions. Postnatal care may include Rasayana therapies to enhance tissue growth and development. Herbs like Shatavari, Ashwagandha, and Bala are recommended to strengthen Shukra Dhatu and hormonal function, while Swarna Prashana (gold-based pediatric tonic) is used in infancy to boost immunity and growth. In cases like micropenis or delayed development, classical formulations such as Vrihani Gutika, Kalyanaka Ghrita, and Trivanga Bhasma have been mentioned for Balya (strengthening) and Vrishya (reproductive vitality) actions when used under expert supervision [13].
Other Common Systemic Disorders
Cardiovascular disease and coronary artery disease
When penile blood flow becomes weaker, the same vascular process is often happening in the heart. You may notice erection quality falling before any chest symptoms appear. A clinician will often treat erectile dysfunction as a vascular warning sign and screen lipids, blood pressure, and overall cardiovascular risk.
Hypertension
High blood pressure injures the inner lining of arteries and reduces nitric oxide signaling. If you feel that erections are softer or shorter, hypertension and its medications both need review.
Dyslipidemia and high LDL cholesterol
Plaque formation and endothelial dysfunction reduce penile arterial inflow. Your lab report often shows a pattern that matches erectile symptoms even when you feel otherwise healthy.
Peripheral artery disease and generalized atherosclerosis
Calf pain on walking, cold feet, or reduced pulses can coexist with penile ischemia. In older men, this association is very common.
Heart failure
Reduced cardiac output, neurohormonal changes, and medication effects frequently impair libido and erection quality. A treating physician typically evaluates both symptoms and drug contributors.
Venous leak and veno occlusive dysfunction
This is a structural hemodynamic issue where blood enters but does not stay trapped in the corpora. You may describe it as getting hard but losing it quickly, especially during penetration.
Metabolic disorders that commonly coexist
Type 2 diabetes mellitus
Diabetes drives microvascular injury, autonomic neuropathy, reduced nitric oxide, and higher rates of balanitis and foreskin scarring. You may also notice reduced sensation or delayed orgasm. A doctor will often consider diabetes one of the most common root associations.
Prediabetes and insulin resistance
Even before full diabetes, endothelial dysfunction can blunt penile blood flow. If your HbA1c is borderline, symptoms can still be real.
Metabolic syndrome
Central obesity, hypertension, dyslipidemia, and insulin resistance together strongly correlate with erectile dysfunction and lower testosterone. This cluster is one of the most clinically meaningful associations.
Obstructive sleep apnea
Poor sleep and intermittent hypoxia reduce testosterone signaling and worsen endothelial function. Many patients report that erections improve when sleep apnea is treated.
Nonalcoholic fatty liver disease
This often travels with metabolic syndrome and low grade inflammation. You may not feel liver symptoms, yet sexual dysfunction can be part of the systemic picture.
Endocrine and hormonal disorders associated with penile disorders
Male hypogonadism
Low testosterone commonly presents as reduced libido, fewer morning erections, and reduced sexual confidence. A clinician will typically check total testosterone, free testosterone, LH, FSH, and SHBG when symptoms match.
Hyperprolactinemia
Raised prolactin can suppress gonadotropins and libido. You may notice low desire and weaker erections. Physicians often evaluate medications, pituitary causes, and thyroid status.
Thyroid disorders
Both hypothyroidism and hyperthyroidism can cause erectile dysfunction and ejaculatory changes. If you feel anxiety, palpitations, fatigue, or weight changes alongside sexual symptoms, thyroid testing is appropriate.
Cushing syndrome and chronic glucocorticoid excess
Cortisol excess reduces gonadal hormones and increases insulin resistance. You may notice central weight gain, low libido, and erectile difficulty.
Primary and secondary adrenal disorders
Adrenal insufficiency can reduce energy and sexual function. Excess adrenal androgens or steroid use can also disrupt the axis. Clinicians interpret symptoms with hormone panels.
Neurologic and spinal disorders that can present as penile symptoms
Peripheral neuropathy
Diabetes, alcohol use, B12 deficiency, and chemotherapy can reduce penile sensation, delay orgasm, or impair arousal. You may describe numbness, tingling, or a muted orgasm.
Autonomic neuropathy
When autonomic control is impaired, erection and ejaculation coordination can fail. Physicians often consider diabetes, Parkinson disease, and certain medications.
Multiple sclerosis
Neurogenic erectile dysfunction, ejaculatory dysfunction, and sensory changes can occur. Your neurologist and urologist often manage this together.
Parkinson disease
Dopaminergic disruption and autonomic dysfunction alter libido and erection. Some patients experience hypersexuality on dopaminergic therapy while still having erectile difficulty.
Spinal cord injury and spinal stenosis
Lumbar and sacral involvement can change reflex erection, sensation, and ejaculation. You may notice position dependent worsening or leg symptoms.
Pudendal nerve entrapment
This can produce penile pain, numbness, and pelvic floor tightness. You may feel burning or electric pain that worsens with sitting.
Genitourinary disorders frequently associated with penile complaints
Benign prostatic hyperplasia
Lower urinary tract symptoms and erectile dysfunction often coexist. If you wake at night to urinate and also have weaker erections, clinicians commonly evaluate both together.
Chronic prostatitis and chronic pelvic pain syndrome
Penile pain, perineal pain, painful ejaculation, and erectile dysfunction can be part of this syndrome. Many patients describe fluctuating symptoms with stress.
Urethral stricture disease
Weak stream, spraying, dribbling, and penile discomfort can occur. Trauma, infection, or instrumentation may be present in the history.
Bladder pain syndrome
Pain and urinary urgency can reduce sexual function and cause penile referred pain. Your symptoms may feel urologic but the cause is pelvic pain physiology.
Dermatologic and inflammatory disorders involving the penis
Balanitis and recurrent candidiasis
Common in diabetes and immunosuppression. You may notice redness, burning, fissures, or discharge. Recurrent episodes often indicate a systemic driver.
Lichen sclerosus
A major cause of foreskin scarring, phimosis, meatal stenosis, and painful intercourse. Clinicians also monitor long term cancer risk.
Lichen planus
Can cause erosive lesions and pain. A dermatologist may evaluate other mucosal sites as well.
Psoriasis and eczema
Genital involvement can cause itching, fissures, and dyspareunia. You may feel symptoms worsen with stress and friction.
Fixed drug eruption
Certain drugs can trigger recurrent lesions at the same site. If you notice a repeating lesion after a specific medication, a clinician will consider this.
Contact dermatitis
Soaps, lubricants, condoms, and topical products can trigger inflammation. You may improve rapidly when triggers are removed.
Infectious disorders that can be associated with penile symptoms
Herpes simplex virus
Causes painful ulcers, burning, and dysuria during outbreaks. It can also contribute to chronic neuralgic pain in some cases.
Human papillomavirus
Associated with genital warts and cancer risk in certain patterns. You may have painless lesions that still need evaluation.
Syphilis
Can present with painless ulcer, rash, and systemic symptoms. Clinicians treat it as a high priority diagnosis to rule out.
Gonorrhea and chlamydia
Often cause urethritis with discharge and dysuria, and can trigger reactive inflammation.
Mycoplasma genitalium
A frequent cause of persistent urethritis when routine tests are negative.
Trichomonas
Can contribute to urethritis and irritation.
HIV and immunosuppression related infections
Opportunistic infections and higher recurrence rates of common infections can affect penile health. Clinicians consider immune status when infections are recurrent.
Sexual function disorders and psychosexual associations
Performance anxiety and situational erectile dysfunction
If you are able to have erections alone but struggle with a partner, anxiety may be a major driver. A clinician will still rule out organic causes, but the pattern is important.
Depression
Depression reduces libido and arousal, and many antidepressants also affect sexual function. You may feel desire drop before erectile symptoms.
PTSD and chronic stress physiology
Stress increases sympathetic tone, which directly opposes erection physiology. Many patients report a cycle where fear of failure becomes the trigger.
Relationship discord and sexual pain avoidance
When pain, fear, or mistrust is present, the body often downregulates arousal. A third person perspective matters here because partners often interpret symptoms incorrectly without education.
Antidepressants including SSRIs and SNRIs
Commonly cause delayed orgasm, anorgasmia, and erectile dysfunction. You may feel mentally calmer but sexually disconnected.
Antipsychotics
Can raise prolactin and impair libido and erection.
Antihypertensives
Some classes contribute to erectile difficulty in certain patients, while others are neutral or helpful. A physician reviews the regimen rather than assuming one culprit.
Finasteride and antiandrogen exposure
Sexual adverse effects can include libido changes, erectile dysfunction, and ejaculatory volume changes in susceptible individuals.
Opioids
Suppress the hypothalamic pituitary gonadal axis and reduce testosterone. Chronic use is strongly associated with sexual dysfunction.
Alcohol use disorder
Can cause neuropathy, hormonal changes, liver related endocrine disruption, and relationship effects.
Anabolic steroid use
May cause testicular suppression, mood instability, infertility, and erectile problems during withdrawal phases.
Tobacco and nicotine dependence
Strong association with endothelial dysfunction and penile arterial disease.
Hematologic and systemic disorders that are rare but high risk
Sickle cell disease
A leading systemic association with ischemic priapism. If you have prolonged erections with pain, this is an emergency.
Leukemia and other hematologic malignancies
Can cause hyperviscosity and priapism. It is rare but clinically critical.
Thalassemia and other hemoglobinopathies
Can alter vascular dynamics and contribute to priapism risk in specific contexts.
Hypercoagulable states
Antiphospholipid syndrome and inherited thrombophilias can affect penile microcirculation and contribute to ischemic events in rare cases.
Connective tissue and fibrotic disorders linked to penile curvature and pain
Peyronie disease
Fibrotic plaques cause curvature, pain, and erectile dysfunction. You may notice a new bend or indentation. Early evaluation matters.
Dupuytren contracture
A fibrotic disorder of the palm that is commonly associated with Peyronie disease. If you have both, it suggests a systemic fibroproliferative tendency.
Ledderhose disease
Plantar fibromatosis that can co associate with other fibrotic disorders.
Systemic sclerosis
Vascular and connective tissue changes can impair erection and cause genital skin tightening.
Congenital and structural disorders that may be missed
Hypospadias related adult complications
Chordee, spraying, and sexual function issues may persist into adulthood. Some patients present late after childhood surgery.
Congenital curvature
Often noticed in adolescence or early adulthood. Differentiating congenital curvature from Peyronie disease is important.
Buried penis
Associated with obesity, lymphedema, or scarring. It can cause hygiene problems, infection, and sexual dysfunction.
Penile lymphatic disorders
Lymphedema or lymphangiosclerosis can cause swelling or cord like structures and anxiety.
Penile squamous cell carcinoma
Rare but serious. Risk associations include chronic inflammation, phimosis, HPV, lichen sclerosus, smoking, and immunosuppression. If you see a persistent ulcer or lump that does not heal, immediate evaluation is required.
Prostate cancer treatment effects
After prostatectomy or radiation, erectile dysfunction and penile shortening can occur due to neurovascular injury and fibrosis.
Trauma and iatrogenic associations
Penile fracture
Sudden pain, swelling, and deformity during intercourse is an emergency. Long term erectile dysfunction can follow if untreated.
Pelvic fracture and perineal trauma
Can injure arteries and nerves. You may notice delayed onset erectile dysfunction after recovery.
Cycling related perineal compression
Can contribute to pudendal nerve symptoms. If you cycle long distance and have numbness, saddle and posture modifications matter.
Post catheterization injury
Urethral irritation and strictures may develop, leading to penile pain and urinary symptoms.
Symptoms to Watch For
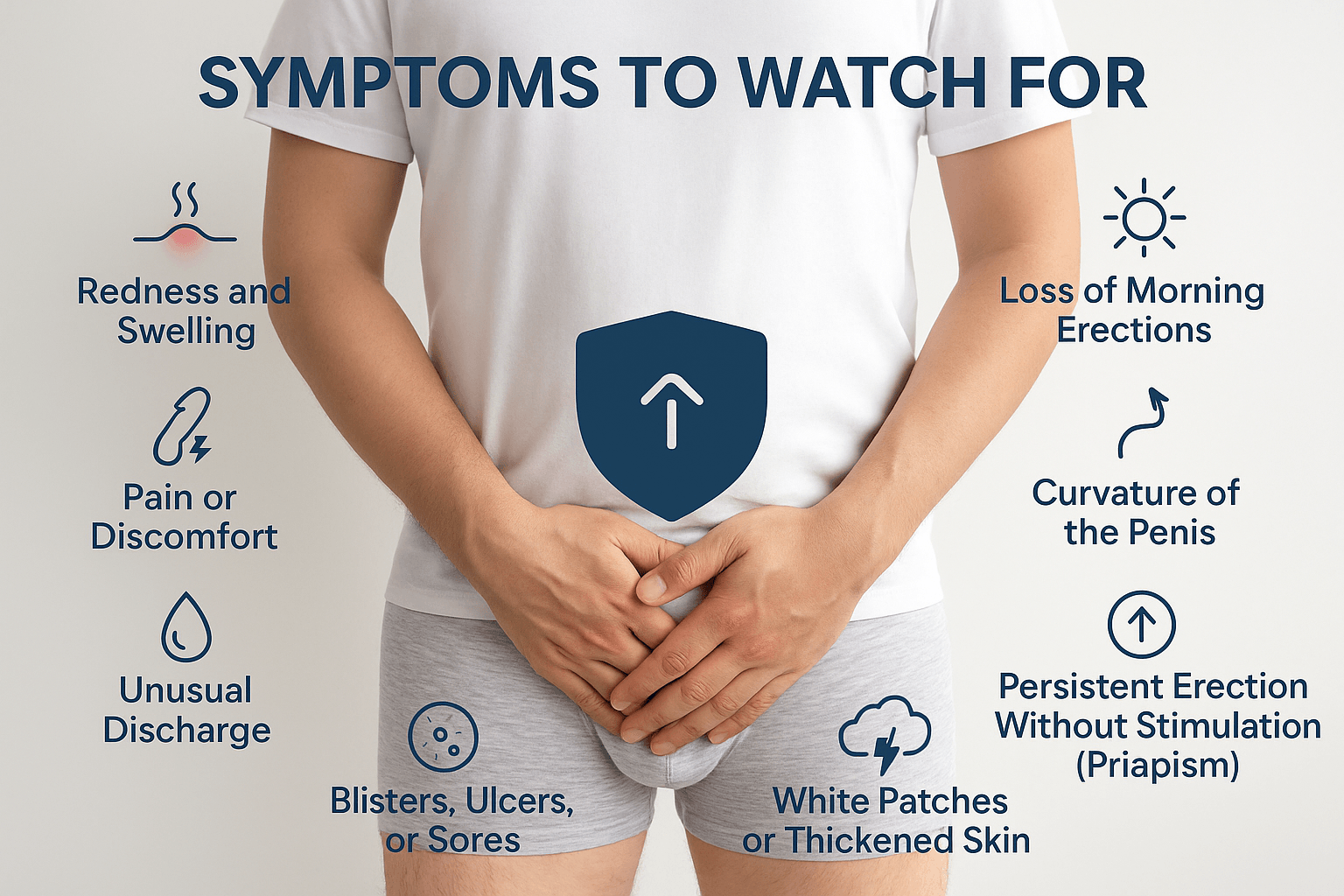
Recognizing the early symptoms of penile disorders is essential for timely intervention and prevention of complications. Many men delay seeking medical help due to embarrassment or misinformation, often allowing a manageable condition to progress into a more severe stage. This section outlines the key symptoms to monitor, including several lesser-known but clinically significant signs that should not be overlooked.
Redness and Swelling
Inflammation of the glans, shaft, or foreskin is often the first visible sign of infection or irritation. Redness accompanied by swelling may indicate balanitis, an allergic reaction, or even the early stage of autoimmune conditions such as lichen sclerosus. When persistent, it suggests a deeper inflammatory imbalance that warrants evaluation [14].
Pain or Discomfort
Pain during urination, erection, or penile contact is a warning sign. Sharp pain with curvature could indicate Peyronie’s disease, while burning or stinging sensations may point to herpes or fungal infections. In Ayurveda, this is often linked to Pitta aggravation and Rakta Dushti, indicating heat and inflammation within the channels [15].
Unusual Discharge
The appearance of pus, cloudy fluid, or foul-smelling discharge from the urethra or under the foreskin is a common sign of infection. Gonorrhea, chlamydia, or candidal infections may all present this way. Ayurvedically, this discharge (known as Shukrameha if whitish) is viewed as Shukravaha Srotas Dushti, particularly involving Kapha and Pitta [16].
Blisters, Ulcers, or Sores
Painful or painless ulcers, especially those that don’t heal, may indicate herpes, syphilis, or even early-stage penile cancer. Blisters that recur may point to viral shedding. Ayurveda considers such lesions under Dushta Vrana or Masurika Upadrava, requiring both local and systemic treatment to prevent chronicity [17].
Loss of Morning Erections
A gradual decline in spontaneous morning erections is often an early warning of vascular insufficiency, hormonal imbalance, or psychological stress. In many cases, this precedes full-blown erectile dysfunction. Ayurveda links this symptom to Shukra Kshaya or Vata–Kapha Sanga, where reproductive tissue quality and circulation decline silently [18].
Curvature of the Penis During Erection
Although some natural curvature is common, sudden development or worsening of curvature may signal Peyronie’s disease. It results from fibrous plaque formation in the penile shaft. In Ayurveda, this may correlate with Vata–Rakta Vyadhi, affecting the elasticity of the penile tissues and Snayu (ligaments) [19].
Persistent Erection Without Stimulation (Priapism)
An erection lasting more than four hours without sexual arousal is a medical emergency. It may be painful (ischemic priapism) or painless (non-ischemic). Conditions like sickle cell disease, leukemia, or medication side effects are often to blame. Ayurveda describes similar pathologies involving Apana Vayu Dushti and blood stagnation (Rakta Sanga) [20].
Bleeding or Foul Odor from the Penis
Spontaneous bleeding from the urethra or skin of the penis is never normal and often suggests advanced pathology such as ulcerated carcinoma or severe balanoposthitis. A foul odor can signal necrotic tissue or deep infection. Ayurvedically, such signs suggest Dushta Vrana with Saptadhatu Dushti (deep tissue damage), requiring urgent intervention [21].
White Patches or Thickened Skin
These are often misdiagnosed or ignored but can be early indicators of lichen sclerosus or leukoplakia—both of which carry a cancer risk. Ayurveda sees white patches and induration as Kaphaja Kustha or Shvitra Upadrava, often associated with Rakta Dhatu and Tvak vitiation [22].
Underlying Causes
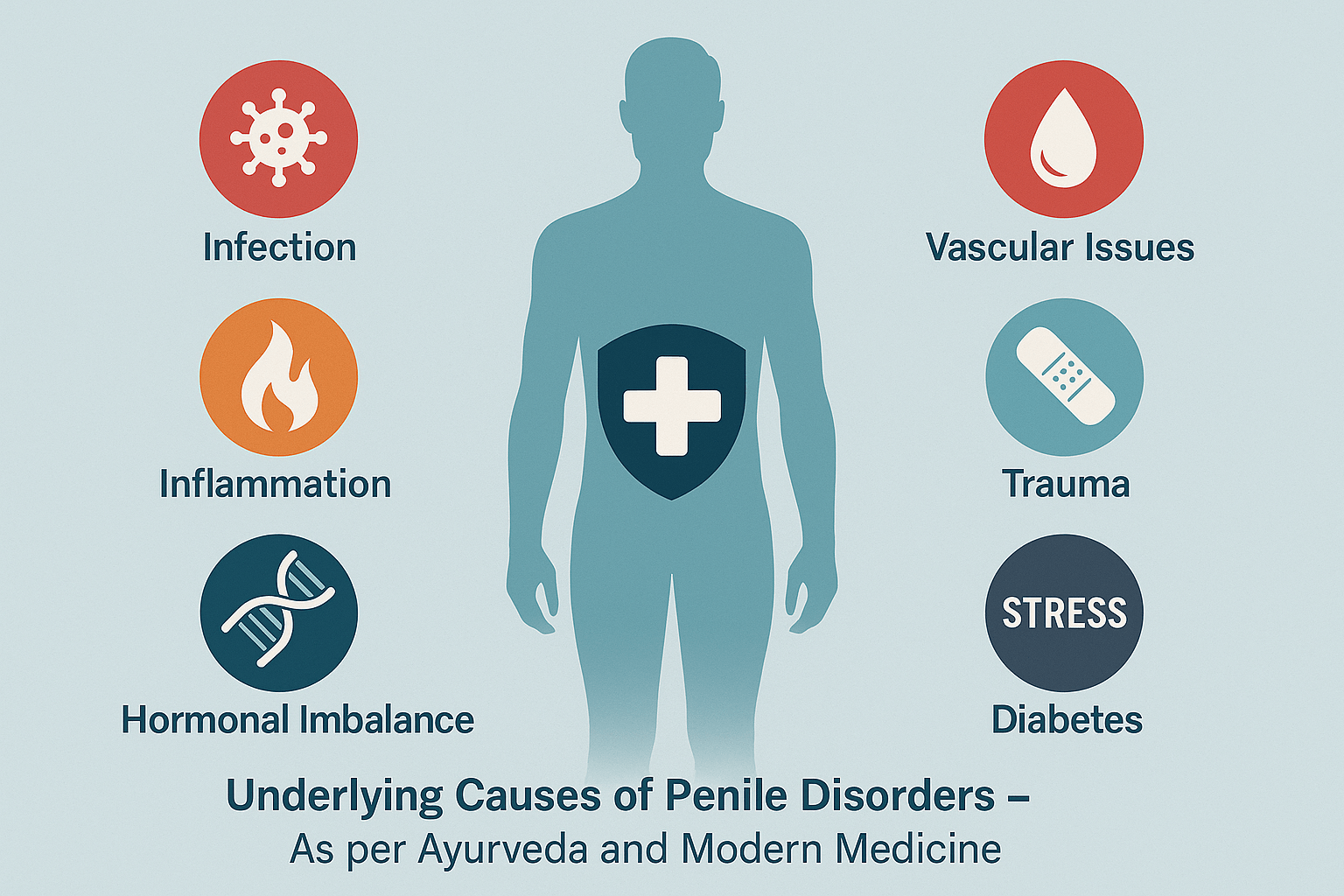
Understanding the root causes of penile disorders is crucial for effective diagnosis and long-term recovery. While superficial treatments may offer temporary relief, identifying the underlying pathology—whether physical, hormonal, infectious, vascular, or psychological—is the key to curative therapy. This section explores the most important and often overlooked causes, bridging modern clinical insights with Ayurvedic principles of dosha, dhatu, and srotas pathology.
Infectious Causes
Sexually transmitted infections (STIs) such as herpes simplex virus (HSV), human papillomavirus (HPV), gonorrhea, syphilis, and chlamydia are major contributors to penile inflammation, ulceration, and discharge. Fungal infections, especially Candida albicans, are common in uncircumcised and diabetic men. Ayurveda recognizes such presentations as Pittaja Kleda or Kapha–Pitta Dushti of the Shukravaha Srotas, with treatment focused on Krimighna (antimicrobial) and Shodhana (detoxifying) therapies [23].
Poor Genital Hygiene
Failure to clean the area under the foreskin can lead to smegma accumulation, creating a moist environment prone to infection. This chronic irritation is also a known risk factor for penile cancer. Ayurveda identifies this as Mala Sanchaya (accumulation of waste) in the Shukra channels, especially under Kapha aggravation. Daily washing with lukewarm water and herbal decoctions such as Triphala or Nimba is emphasized [24].
Metabolic and Endocrine Disorders
Diabetes mellitus is a major hidden cause of penile disorders. Elevated blood sugar impairs immune function, increases fungal colonization, reduces penile blood flow, and damages the penile nerves, resulting in balanitis, phimosis, and erectile dysfunction. Similarly, low testosterone levels or thyroid imbalances disrupt libido and tissue nutrition. In Ayurveda, this reflects Agni Mandya (metabolic suppression), Shukra Kshaya, and Majja Dhatu Dushti. Rasayana and Agni-deepana (digestive stimulants) like Shilajit, Gokshura, and Ashwagandha are classically recommended in such contexts [25].
Autoimmune and Inflammatory Conditions
Chronic inflammatory skin diseases such as lichen sclerosus, psoriasis, and reactive arthritis can affect the penis, leading to white patches, thickened skin, and even scarring. These are often missed or misdiagnosed in early stages. Ayurveda views such conditions as Kustha or Rakta Dhatu Vikara with Srotorodha. Herbal approaches include Manjishtha, Haridra, and Khadirarishta, along with Raktashodhaka (blood-purifying) therapies [26].
Trauma and Mechanical Injury
Sudden or forceful bending of the erect penis during sexual activity or accidents can lead to penile fracture, hematoma, and fibrosis. Chronic microtrauma can cause Peyronie’s disease due to collagen deposition. Ayurveda classifies this under Abhighataja Vata Vyadhi—disorders due to trauma that cause Vata Prakopa, resulting in pain, stiffness, and plaque formation. Oils like Mahanarayan Taila and internal Vata-pacifying formulations are used post-injury [27].
Psychological and Emotional Stress
Performance anxiety, depression, unresolved grief, and chronic stress are major but invisible drivers of erectile dysfunction and sexual fatigue. In modern science, the limbic system and hypothalamic-pituitary axis play a major role. Ayurveda has long recognized this connection under Manasika Klaibya and treats it with Medhya Rasayanas like Brahmi, Mandukaparni, and Shankhpushpi, often combined with Ashwagandha and Jatamansi for restoring mind-body balance [28].
Hormonal Imbalances
Andropause, low testosterone, high prolactin, or thyroid dysfunctions can subtly alter erectile capacity, libido, and reproductive functions. While modern endocrinology uses hormone replacement therapy (HRT), Ayurveda strengthens the endocrine axis by nourishing the Shukra and Majja Dhatus. Classical formulas like Vrishya Vati, Trivanga Bhasma, and Svarna Bhasma are used to tonify endocrine function [29].
Circulatory Disorders and Vascular Insufficiency
Atherosclerosis and peripheral artery disease reduce penile blood flow, leading to weak erections and delayed healing of injuries. Smoking, hypertension, and sedentary lifestyle worsen the condition. Ayurveda considers this a Vyana Vayu–Rakta Dushti pathology and prescribes Hridaya Vardhaka Rasayanas such as Arjuna, Pushkaramoola, and Dashamoola to enhance microcirculation [30].
Excessive Sexual Activity or Suppression of Urges
Chronic indulgence in sexual activity weakens Shukra Dhatu, while suppression of natural urges (like urination or ejaculation) disturbs the normal flow of Apana Vayu. Both lead to disorders of penile strength, sensation, and function. Ayurveda explicitly warns against such habits in Charaka Samhita and recommends lifestyle regulation (Brahmacharya), Rasayana tonics, and yogic techniques to restore balance [31].
Diagnostic Tools in Modern Medicine

Accurate diagnosis of penile disorders is essential for effective treatment, prevention of complications, and restoring patient confidence. Modern medicine offers a range of diagnostic tools that assess structural, vascular, infectious, hormonal, and neurological aspects of penile health. Each modality plays a role in uncovering the underlying pathology, guiding clinicians toward targeted therapy. This section reviews the most commonly used tools and how they contribute to a comprehensive evaluation.
Physical Examination
The first and most crucial step in diagnosis is a detailed physical examination. Urologists assess for visible abnormalities such as swelling, discharge, ulcers, plaques, or curvature. They palpate the penile shaft, glans, and inguinal lymph nodes and examine the foreskin’s retractability. Findings such as fibrous bands in Peyronie’s disease or white patches in lichen sclerosus can be identified during inspection. This clinical assessment forms the foundation of further diagnostic planning [32].
Urethral Swab and Culture
For patients presenting with discharge, pain, or suspected sexually transmitted infections, a urethral swab is often performed. Samples are cultured or subjected to nucleic acid amplification testing (NAAT) to detect pathogens such as Neisseria gonorrhoeae, Chlamydia trachomatis, Herpes Simplex Virus, or Candida albicans. Rapid PCR testing now enables same-day diagnosis and appropriate antibiotic or antiviral treatment. Ayurvedic interpretation correlates recurrent infections with Krimi (microbial invasion) and Shukravaha Srotas Dushti [33].
Blood Tests and Serology
Routine blood work evaluates blood sugar (for diabetes), renal function, complete blood count (for infections or anemia), and inflammatory markers. Hormonal profiling includes total and free testosterone, prolactin, luteinizing hormone (LH), follicle-stimulating hormone (FSH), and thyroid panel. In patients with ED or delayed sexual development, these values provide critical clues. Ayurvedic diagnostics integrate these findings with symptoms of Shukra Kshaya, Agnimandya, and Majja Dhatu Dushti [34].
Penile Doppler Ultrasound
Color Doppler ultrasound assesses penile blood flow before and after pharmacological erection induction. It helps diagnose vascular causes of erectile dysfunction, venous leakage, and arterial insufficiency. It is also used in Peyronie’s disease to evaluate plaque size and calcification. In modern practice, this tool is essential for distinguishing psychogenic from organic ED. Ayurveda addresses vascular deficits with Vata-Rakta balancing therapies and Hridaya-Utthejana Rasayanas [35].
Nocturnal Penile Tumescence (NPT) Test
This non-invasive test evaluates whether spontaneous erections occur during sleep. Lack of nocturnal erections suggests an organic cause of ED, while their presence indicates psychogenic origins. Devices like RigiScan are commonly used. Ayurveda acknowledges this with terms like Swapnadosha or Nidra Klaibya, where disturbed mental or nervous function underlies sexual fatigue [36].
Biopsy and Histopathology
In cases of non-healing ulcers, suspected cancer, or persistent white patches, a biopsy is mandatory. Histological analysis confirms or rules out malignancy, dysplasia, or chronic inflammatory conditions. This is critical in penile cancer and conditions like lichen sclerosus. Ayurveda compares such diagnostics with Mamsa and Rakta Dhatu Dushti and considers the need for Shodhana and Rasayana support alongside surgical excision [37].
MRI and CT Scans
Advanced imaging is rarely needed but may be employed to evaluate the extent of penile cancer or deep-seated fibrosis in advanced Peyronie’s. MRI offers high-resolution detail of soft tissue involvement. In Ayurveda, while such imaging isn’t described classically, the interpretation may involve Srotodushti mapping and Upadhatu Vikriti assessment [38].
Urinalysis and Urine Flow Studies
Urinalysis is useful in identifying infections, hematuria, or metabolic abnormalities. In cases of urethral strictures or functional obstruction, uroflowmetry is performed. Ayurveda considers difficult urination or dribbling under Mutrakrichra or Vatakundalika, guiding treatment through herbal diuretics and Basti Karma [39].
Penile Sensory and Nerve Testing
In patients with suspected neurogenic causes, such as diabetic neuropathy or spinal injury, tests like biothesiometry or bulbocavernosus reflex latency can assess penile nerve function. While less commonly used, these help refine the treatment plan. Ayurveda attributes such presentations to Vata Vyadhi in the Majja Srotas and treats with Medhya Rasayana, Vatahara Taila Abhyanga, and Nasya [40].
Ayurvedic Understanding of Penile Disorders
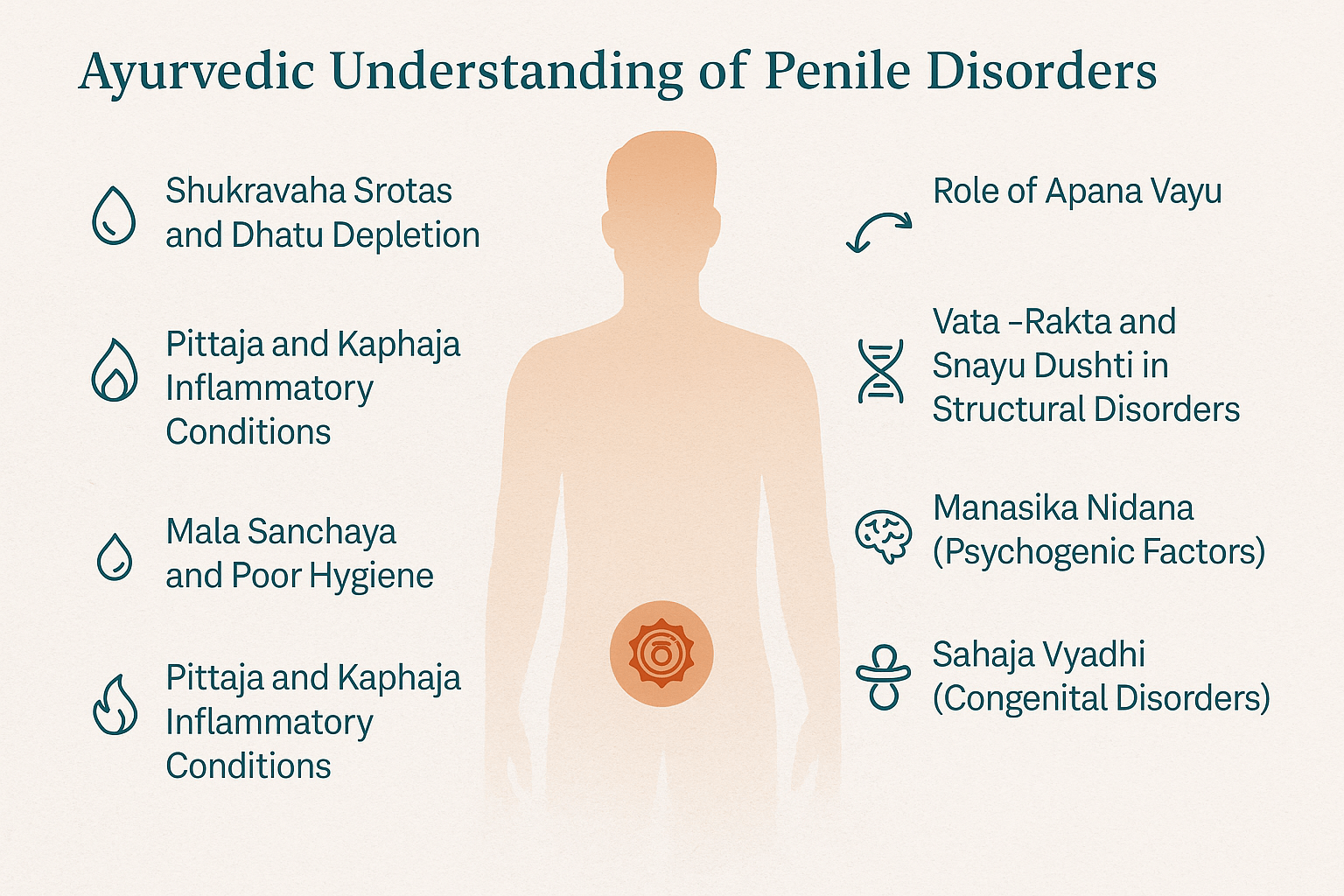
Ayurveda, the ancient science of life, approaches penile disorders not merely as isolated physical issues but as reflections of deeper imbalances in the body’s doshas, dhatus, srotas, and mental-emotional state. The penis (shishna) and its associated functions are governed primarily by Shukra Dhatu (reproductive tissue), Majja Dhatu (marrow/nervous system), and the activities of Apana Vayu (a subtype of Vata responsible for downward bodily functions). Disruptions in these systems—whether due to lifestyle errors, suppressed urges, trauma, or systemic disease—manifest as dysfunction, deformity, or inflammation.
Shukravaha Srotas and Dhatu Depletion
Most penile disorders arise from Shukravaha Srotas Dushti—obstruction, depletion, or distortion in the channels that carry and nourish the reproductive tissue. This can be caused by:
- Shukra Kshaya (reduction in quality or quantity of semen),
- Shukradushti (vitiation of reproductive essence), or
- Shukragata Vata (Vata lodging in the reproductive pathways).
Charaka Samhita notes that Shukra is the final product of all seven dhatus; hence, its compromise is often a sign of long-term internal degeneration [41].
Role of Apana Vayu
The functionality of the penis—erection, ejaculation, and urination—is regulated by Apana Vayu. When vitiated due to faulty diet, sedentary habits, or sexual overindulgence, Apana either becomes blocked or hyperactive, leading to issues like erectile dysfunction, priapism, premature ejaculation, or painful retraction (paraphimosis). Apana Vayu Dushti is often accompanied by Vata-Kapha imbalance, especially in chronic disorders [42].
Vata–Rakta and Snayu Dushti in Structural Disorders
Peyronie’s disease, penile curvature, and fibrotic plaques are viewed through the lens of Vata–Rakta (vitiated Vata acting on blood and connective tissues). The involvement of Snayu (ligaments) and Mamsa (muscle tissue) is considered critical. Repeated injury or unresolved inflammation leads to Granthi Srotodushti (nodular or fibrotic obstructions), which correlates closely with the formation of non-malignant plaques [43].
Pittaja and Kaphaja Inflammatory Conditions
Inflammatory disorders like balanitis, lichen sclerosus, and ulcers are typically of Pittaja or Kaphaja origin, or a combination of both. Burning, redness, pus, and heat indicate Pitta Dushti, while swelling, itching, and discharge reflect Kapha accumulation. In these cases, Ayurvedic management targets Rakta Dhatu Shuddhi (blood purification) and removal of local Aama (toxins), often with decoctions like Panchatikta Kashaya or Triphala Guggulu [44].
Manasika Nidana (Psychogenic Factors)
Ayurveda gives equal importance to mental health in sexual disorders. Emotional suppression, fear, guilt, grief, or excessive anxiety can aggravate Vata and disturb Manovaha Srotas, leading to Manasika Klaibya (psychogenic impotence). Herbs such as Brahmi, Ashwagandha, Shankhpushpi, and Jatamansi are traditionally prescribed for stabilizing the mind and rebalancing the neuroendocrine axis [45].
Mala Sanchaya and Poor Hygiene
Conditions like phimosis, smegma buildup, and recurrent infections are explained as Mala Sanchaya (waste accumulation) due to Kapha Dushti and improper lifestyle practices. Daily Snana (bathing), genital hygiene with decoctions like Triphala, and local use of antiseptic oils such as Nimba Taila or Jatyadi Taila are recommended [46].
Sahaja Vyadhi (Congenital Disorders)
Penile abnormalities present at birth—such as hypospadias or micropenis—fall under Sahaja Vyadhi. Ayurveda attributes these to maternal dosha imbalance, improper diet during pregnancy, or past karmic influence. Prevention through Garbhini Paricharya (prenatal care) and postnatal strengthening through Swarna Prashana, Medhya Rasayana, and Bala Vardhaka Chikitsa is advised [47].
Dhatu Chain Breakdown and Shukra Margavarodha
Many disorders are the result of upstream disturbances—Agni Mandya, Rasa Dushti, or Medo Dhatu obstruction—that ultimately impair Shukra Dhatu. Ayurvedic philosophy emphasizes strengthening digestion, metabolic fire, and dhatu equilibrium before targeting the reproductive tissue directly. This is achieved through a carefully sequenced plan of Deepana, Pachana, Snehana, Shodhana, and Rasayana therapy [48].
Ayurvedic Herbs and Rasayanas Used
Ayurveda offers a robust pharmacopeia of herbs, minerals, and Rasayana formulations that have been classically prescribed for restoring penile health, enhancing reproductive function, and treating underlying imbalances in Shukra Dhatu, Apana Vayu, and Majja Dhatu. Unlike modern drugs that often act on a singular mechanism (e.g., vasodilation in ED drugs), Ayurvedic herbs work on multiple physiological layers: hormonal modulation, neurovascular nourishment, immunity enhancement, and mind-body rejuvenation. This section highlights key herbs and Rasayanas with proven utility in managing various penile disorders.
Ashwagandha (Withania somnifera)
A premier Medhya and Vrishya Rasayana, Ashwagandha is extensively used for Shukra Dhatu Kshaya, Klaibya (ED), and post-trauma tissue degeneration. It enhances testosterone levels, reduces cortisol, supports nervous regeneration, and strengthens the penile tissues. Clinical studies show improvements in sperm count, motility, and erectile function [49].
Kapikacchu (Mucuna pruriens)
Classified as Shukrala and Vrishya, Kapikacchu is rich in L-DOPA, a precursor to dopamine. It improves libido, fertility, and penile responsiveness, especially in cases of psychogenic ED or Manasika Klaibya. It is commonly used in formulations like Mashadi Churna and Vrishya Vati [50].
Shilajit
Considered a panacea for degenerative and age-related conditions, Shilajit enhances mitochondrial energy, testosterone production, and vascular tone. It supports microcirculation and strengthens the Majja and Shukra Dhatus. Particularly beneficial in diabetic ED, premature ejaculation, and fatigue-related penile disorders [51].
Gokshura (Tribulus terrestris)
A Mutrala, Shukrala, and Vatahara herb, Gokshura is used in genitourinary inflammations, reduced penile blood flow, and infertility. It enhances nitric oxide synthesis and androgen receptor density, making it useful in Peyronie’s disease and recurrent balanitis [52].
Bala (Sida cordifolia)
Used in classical Tailas (oils) like Bala Taila and Mahanarayan Taila, Bala strengthens Mamsa (muscles), Snayu (ligaments), and supports healing in trauma-induced penile conditions such as fracture or curvature. It’s a foundational herb for penile Abhyanga (massage) therapy [53].
Shatavari (Asparagus racemosus)
Although more commonly associated with female reproductive health, Shatavari’s cooling and Rasayana qualities make it suitable for Pittaja penile disorders—balanitis, burning urination, and inflammatory glans conditions. It pacifies Pitta in Shukravaha Srotas and supports hormonal equilibrium [54].
Yashtimadhu (Glycyrrhiza glabra)
Known for its Raktashodhaka (blood-purifying) and anti-inflammatory action, Yashtimadhu is useful in balanitis, ulcers, post-herpetic penile lesions, and Kapha-Pitta skin involvement. It’s often used as a paste, decoction wash, or internally in combination with Gandhak [55].
A potent Rasayana and Vrishya, Svarna Bhasma is used in chronic cases of ED, fatigue, and penile tissue degeneration. It enhances Ojas, stabilizes Apana Vayu, and improves longevity of Shukra Dhatu. Administered in microdoses under strict supervision, it forms the core of elite Vajikarana formulations like Svarna Vasant Malati and Siddha Makardhwaja [56].
This classical mineral formulation (containing lead, tin, and zinc calxes) is used for penile dysfunctions, premature ejaculation, and urinary issues. It rejuvenates Apana Vayu, strengthens reproductive tone, and is often used in formulations like Vanga Bhasma Yogas or Vrishya Vati [57].
A sulfur-based rejuvenator, Gandhak Rasayan is beneficial in chronic balanitis, fungal infections, and skin lesions of the penis. It enhances tissue immunity, detoxifies the blood, and supports healing of Dushta Vrana. Often combined with Haridra, Nimba, or Manjishtha in skin-urogenital disorders [58].
Main Medicine- Musalyadi Vrishya Avaleha (Ayurvedic)

Musalyadi Vrishya Avaleha is a classical Vajikarana style Avaleha used in Ayurveda to support male sexual health when the root pattern is tissue depletion, stress load, fatigue, reduced libido, weak erection quality, early ejaculation tendency, or loss of confidence due to long-standing strain. Ayurveda does not treat penile function as a local issue alone. It treats it as a reflection of digestion, sleep, nervous system stability, hormonal rhythm, and the quality of Shukra Dhatu and Majja Dhatu.
Charaka Samhita places Vajikarana in Chikitsa Sthana, Chapter 2. The chapter begins with the classical opening that establishes Vajikarana as a formal medical discipline.
अथातः संयोगशरमूलीयं वाजीकरणपादं व्याख्यास्यामः॥ इति ह स्माह भगवानात्रेयः॥
Transliteration
athatah samyoga sharamuliyam vajikarana padam vyakhyasyamah
iti ha smaha bhagavan atreya
Meaning in simple English
Now we shall explain the Vajikarana section, as taught by Acharya Atreya.
Classical shloka on why Vajikarana matters
वाजीकरणमन्विच्छेत् पुरुषो नित्यमात्मवान्। तदायत्तौ हि धर्मार्थौ प्रीतिश्च यश एव च॥
Transliteration
vajikaranam anvicchet purusho nityam atmavan
tadayattau hi dharmarthau pritishcha yasha eva cha
Meaning in simple English
A disciplined person should protect and rebuild virility, because stable vitality supports duty, prosperity, affectionate bonding, and self-respect and success.
Who this medicine is for in the UK, USA, Canada, and Australia
Musalyadi Vrishya Avaleha is best explained to Western patients as a rebuilding, nourishing therapy for functional sexual dysfunction patterns, not a stimulant. It is relevant when penile symptoms are linked with stress physiology, poor sleep, low stamina, metabolic strain, overwork, anxiety, recovery after illness, or long-standing nutritional depletion.
Common patient situations where it fits well
This approach is commonly suitable when the patient reports reduced libido, inconsistent erections, performance anxiety, early ejaculation tendency, low semen confidence, fatigue, poor recovery after work, poor sleep, and a feeling that the body is running on low reserve. In Ayurvedic language, these patterns often show Shukra Dhatu kshaya, Majja Dhatu weakness, Vata aggravation, or Kapha Meda obstruction. When the root drivers are corrected, sexual function tends to improve as a downstream outcome.
When this is not the right first step
This should not be used as a substitute for urgent medical evaluation. Any patient with penile ulcers, severe pain, a persistent lump, blood in urine or semen, suspected STI, rapidly worsening curvature, fever, sudden erectile failure with chest pain symptoms, or neurological weakness must be medically evaluated first. If the dysfunction is primarily medication-induced, vascular disease-related, uncontrolled diabetes-related, or linked with significant hormonal pathology, the plan must be coordinated with medical care.
How it helps in curing and long-term recovery
For Western readers, the most medically acceptable way to explain “curing” is this. When penile symptoms are functional and driven by reversible root causes, this therapy can support reversal of the underlying imbalance and help the body return to stable natural function, provided the patient corrects the drivers that created the condition. It is not designed for temporary masking. It is designed for rebuilding.
The four practical pathways patients can understand
First, it supports recovery from stress load and fatigue by stabilizing the nervous system and improving restorative sleep, which strongly influences libido and performance. Second, it supports deeper tissue nourishment so the body can rebuild reproductive vitality, which Ayurveda calls Shukra Dhatu support. Third, it supports stamina and endurance, so the patient notices better energy and recovery before sexual performance becomes fully stable. Fourth, it supports confidence and consistency by reducing the boom-bust pattern that occurs when men rely only on short-term stimulants.
What improvement usually looks like
In many patients, the first improvements are better sleep, calmer mood, improved appetite, and reduced fatigue. After that, libido and erection consistency improve. For long-standing cases, deeper personalization and longer courses may be needed depending on age, digestion, metabolic health, and stress burden.
The key factors that decide results, not only the medicine
This section is important for UK, USA, Canada, and Australia patients because many people try supplements without changing the real drivers. In Ayurveda, the medicine works when the terrain is corrected.
Digestion and absorption must be stable
If digestion is weak, the body does not convert nourishment into Dhatu building. Patients with bloating, reflux, constipation, chronic loose stools, or irregular appetite need digestion correction, otherwise even potent Vajikarana therapies may give limited benefit.
Sleep and stress control are not optional
Sexual hormones and stress hormones are closely linked with sleep rhythm. If the patient sleeps late, sleeps poorly, or carries high daily anxiety, response becomes slow and unstable. The medicine supports recovery, but lifestyle must allow recovery.
Metabolic and vascular health controls erectile strength
Erection is vascular and neurohormonal. Excess weight, insulin resistance, diabetes, high blood pressure, high cholesterol, smoking, vaping, high alcohol intake, and sedentary lifestyle can block progress. These must be addressed alongside therapy, otherwise results remain partial.
Sexual habits and overstimulation can block recovery
Frequent ejaculation, compulsive pornography use, and repeated overstimulation can reduce sensitivity and worsen anxiety-driven dysfunction. A disciplined routine during therapy improves outcomes and stability.
Why mineral add-ons are not for everyone
Herbo-mineral preparations are used in Ayurveda under strict dose discipline and patient selection. They are not routine for every man with penile symptoms. They can be considered when deeper tissue rebuilding is required, when digestion is stable, and when there is a clear need based on clinical assessment.
Safety rule for UK, USA, Canada, and Australia
Mineral preparations must be prescribed only under direct Ayurvedic physician supervision and sourced with strict traceability and third-party testing. Patients with kidney disease, liver disease, gastritis, ulcers, bleeding disorders, or those using heart medications, anticoagulants, or complex psychiatric medications must not self-start mineral add-ons.
How to take Musalyadi Vrishya Avaleha
Use the dosing exactly as advised in your plan. It is commonly taken after meals.
Dose and adjuvant
Dose is 10 to 15 grams twice daily. Traditional adjuvant is warm milk if tolerated. If milk causes heaviness, bloating, mucus, or discomfort, warm water can be used instead. Consistency matters more than occasional high dosing. A steady routine is what supports rebuilding.
This is a rebuilding Vajikarana therapy designed to correct root causes that weaken male sexual function, not a short-term stimulant. It supports long-term recovery when used with corrected sleep, stress control, digestion stability, metabolic improvement, and disciplined habits. If serious symptoms exist, or if the patient has major medical conditions or is on complex medications, medical evaluation and physician supervision are mandatory before starting.
Musalyadi Avaleha for Penile Disorders
Dose: 10 to 15 g twice daily (maximum planning dose used: 15 g twice daily = 30 g/day)
Total required for 30 days: 900 g
Kwatha Dravya (coarse powder, total 480 g)
Safed Musali (Chlorophytum borivilianum) 48 g
Kali Musali (Curculigo orchioides) 48 g
Ashwagandha (Withania somnifera) 48 g
Shatavari (Asparagus racemosus) 48 g
Vidarikanda (Pueraria tuberosa) 48 g
Gokshura (Tribulus terrestris) 48 g
Kapikacchu seed (Mucuna pruriens, de-husked) 48 g
Bala (Sida cordifolia) 48 g
Atibala (Abutilon indicum) 48 g
Yashtimadhu (Glycyrrhiza glabra) 48 g
Liquid for decoction
Water 7.5 litres (reduce to one-fourth, target 1.8 to 2.0 litres)
Cow milk 2.0 litres (added after kwatha reduction)
Madhura Dravya
Sharkara 900 g (use only if suitable; for diabetic or insulin resistance cases, this must be modified by the physician)
Sneha Dravya
Go-ghrita 180 g
Prakshepa Dravya (fine powder, total 36 g)
Pippali (Piper longum) 6 g
Ela (Elettaria cardamomum) 6 g
Tvak (Cinnamomum verum) 6 g
Patra (Cinnamomum tamala) 6 g
Nagakesara (Mesua ferrea) 6 g
Vanshalochana (Bambusa arundinacea silica) 6 g
Madhu (added after cooling)
Madhu 150 g
Mineral Fortification for the same 30-day batch (added to the final 900 g jar, total monthly quantities)
Abhrak Bhasma Sahasraputi 5 g
Jasad Bhasma 500 mg
Mukta Shukti Bhasma 500 mg
Godanti Bhasma 500 mg
Heerak Bhasma 500 mg
Swarna Bhasma 300 mg
Pravala Pishti 500 mg
Vyadhiharan Rasayan 5 g
How to incorporate the minerals correctly (professional method)
Prepare the Avaleha fully first and allow it to self-cool until it is lukewarm. Separately triturate all mineral preparations and Vyadhiharan Rasayan into a uniform fine blend. Add this blend gradually into the finished Avaleha and mix until the distribution is uniform throughout the entire 900 g batch. Do not add mineral preparations during active heating.
Administration (for website)
10 to 15 g twice daily with warm cow milk. Avoid taking with sour foods, alcohol, very spicy foods, and late-night wakefulness during the course.
Mandatory clinical safety note
This formulation is not appropriate for self-medication or market purchase. Mineral preparations must be authenticated, correctly processed, and dosed only after physician evaluation. Patients with kidney disease, liver disease, active gastritis or ulceration, bleeding disorders, pregnancy, or those taking anticoagulants must be screened and monitored before use.
Safety Warning for Patients
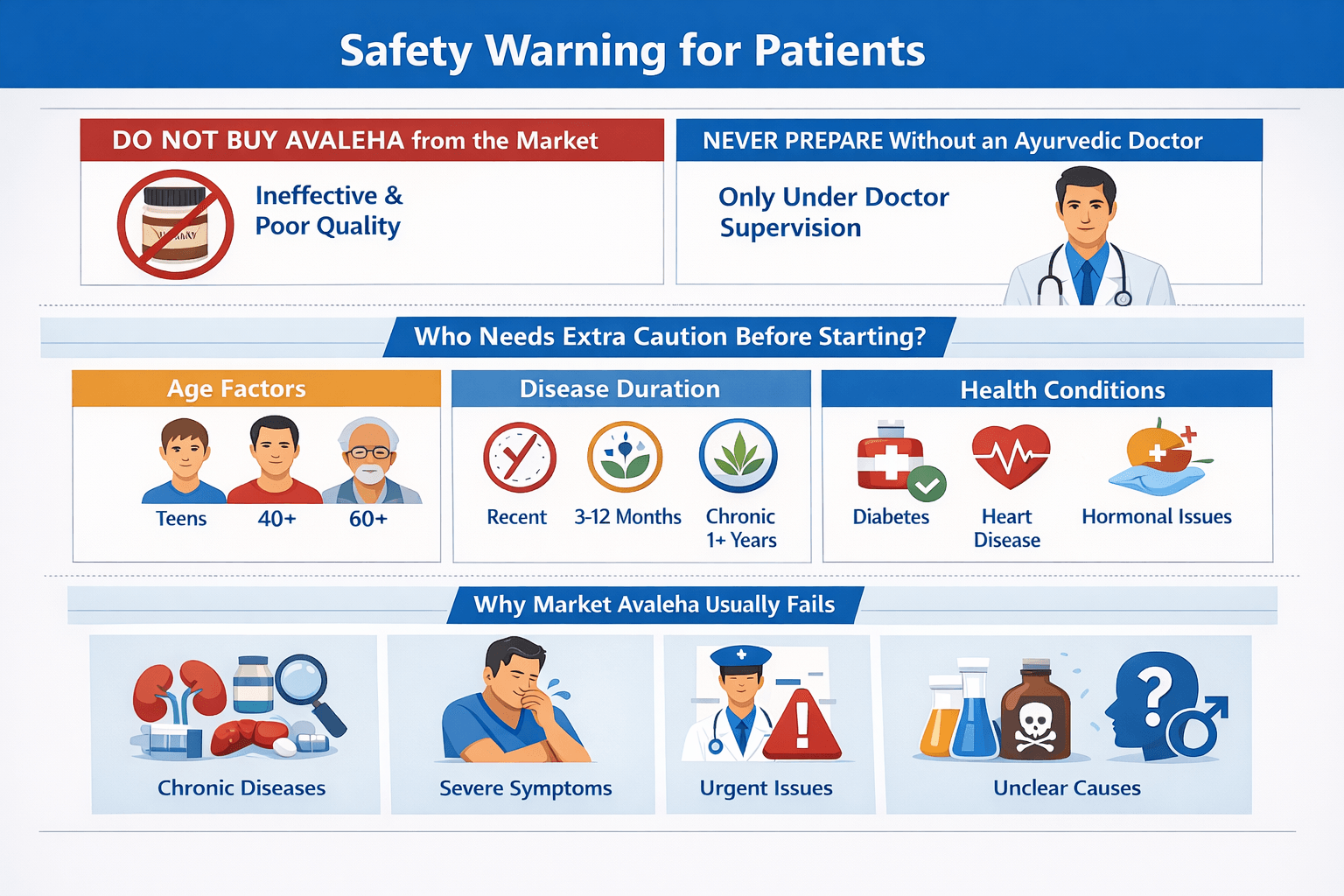
Patients must not buy Avaleha from the market or from random online sellers. This medicine is a physician-directed Vajikarana therapy. If you purchase it as a generic product, it often does not work and it can be unsafe. Never prepare this medicine at home or start it without supervision from a qualified Ayurvedic doctor.
Why market bought Avaleha often does not work
Wrong diagnosis and wrong formulation choice
Penile disorders can be caused by stress and fatigue, diabetes, vascular disease, hormone imbalance, medication side effects, pelvic nerve issues, infections, prostate problems, or structural conditions like painful curvature. If the root cause is not identified, even a good formula will not match the condition, and results will be poor.
No personalization to Prakriti, Dosha, and Dhatu status
In Ayurveda, results depend on matching the medicine to the patient’s Prakriti, dominant Dosha imbalance, and Dhatu involvement. A fixed market formula cannot adapt to Vata-driven erectile instability, Pitta-driven burning or inflammation, or Kapha-Meda-driven vascular sluggishness. Without personalization, the same medicine can underperform or aggravate symptoms.
Poor quality raw materials
Market products often use lower-grade herbs, incorrect botanical parts, old stock, or cheaper substitutes. Vajikarana therapy depends on potency. If core herbs like Musali, Ashwagandha, Shatavari, Kapikacchu, and Gokshura are weak or adulterated, the formulation will not deliver expected results.
Incorrect manufacturing method and wrong cooking stage
Avaleha requires correct paka and classical preparation steps. Overheating destroys key active fractions, undercooking causes poor shelf stability, and wrong moisture content leads to fermentation. Even minor pharmaceutical errors can change the effect completely.
Wrong storage and loss of potency
Avaleha is sensitive to heat, moisture, and contamination. Market supply chains often involve long storage, repeated temperature changes, and poor container quality. The medicine may look fine but become weaker over time.
Unreliable dose and concentration
Market Avaleha can vary in sweetness, ghee content, and herb ratio between batches. The patient ends up taking inconsistent doses, which reduces results. Some products are mostly sweet base with minimal active drug, which gives taste but not therapeutic action.
Mineral add-ons are a major risk when bought without supervision
If the formulation contains Bhasmas or mineral preparations, buying it from the market is not acceptable. These substances require strict purification, correct processing, traceability, and safety testing. Unverified products can be unsafe and can also fail clinically because the dose, quality, and processing are unknown.
Hidden contraindications are missed
Many patients have conditions that require screening before Vajikarana therapy, such as uncontrolled hypertension, high cholesterol, diabetes, fatty liver, kidney disease, gastritis, ulcers, thyroid disorders, or prostate enlargement. Market products do not evaluate these factors, so treatment becomes ineffective or risky.
Interaction with modern medicines is ignored
Patients in the UK, USA, Canada, and Australia commonly take medications that influence erection, ejaculation, or blood flow, including antidepressants, blood pressure medicines, diabetes medicines, and blood thinners. If interactions and timing are not managed, results can be poor and side effects can occur.
Patient factors that commonly prevent the medicine from working
Age and baseline vascular status
After about 40 years, erectile dysfunction is more commonly linked with vascular stiffness, endothelial dysfunction, and metabolic risk. If the patient has high blood pressure, high cholesterol, diabetes, or a long smoking history, improvement requires a combined plan. An Avaleha alone is not enough.
Disease duration and stage
If symptoms have persisted for years, the condition is usually deeper and more complex. Long duration often means chronic stress physiology, weakened sleep rhythm, vascular compromise, or nerve involvement. In such cases, the medicine needs longer courses and additional therapies, not a short trial.
Chronic disorders that silently block recovery
Diabetes, insulin resistance, obesity, sleep apnea, depression, anxiety disorders, hypothyroidism, chronic prostatitis, fatty liver, chronic constipation, IBS, and chronic inflammation can prevent full response. If these are not treated alongside, the Avaleha appears ineffective.
Hormonal imbalance
Low testosterone, elevated prolactin, thyroid imbalance, or adrenal stress patterns can reduce results. Without checking and correcting the hormonal component, response becomes partial.
Ongoing lifestyle triggers
Alcohol, smoking, vaping, cannabis, late-night sleep, high pornography stimulation, high stress workload, and lack of exercise can override the benefit. Many patients take a medicine but continue the same triggers that caused the disorder, so the condition persists.
Digestive weakness and poor absorption
If digestion is weak, the body does not convert nutrition into Dhatu. Symptoms like bloating, reflux, irregular stools, low appetite, and poor sleep indicate that digestion support is needed first. Otherwise, Vajikarana medicines do not build tissue effectively.
Psychological component and relationship stress
Performance anxiety, past trauma, and relationship stress can create a persistent sympathetic overdrive state. In such cases, mental calming strategies and counselling support may be needed along with the medicine.
Why you must not prepare this medicine without an Ayurvedic doctor
Avaleha preparation requires correct selection of herbs, correct decoction ratios, correct cooking stage, and correct storage standards. If mineral preparations are added, physician control becomes mandatory due to strict dosing, processing requirements, and patient screening. Without supervision, the medicine can fail or cause avoidable complications, especially in patients with kidney, liver, gastric, cardiovascular, or medication-related risks.
Clear patient instruction
Do not purchase this Avaleha from the market and do not prepare it at home. For this therapy to work and to remain safe, it must be prescribed and customized by a qualified Ayurvedic doctor based on age, symptoms, disease duration, stage, digestion, metabolic status, and current medications.
Modern Treatment Approaches
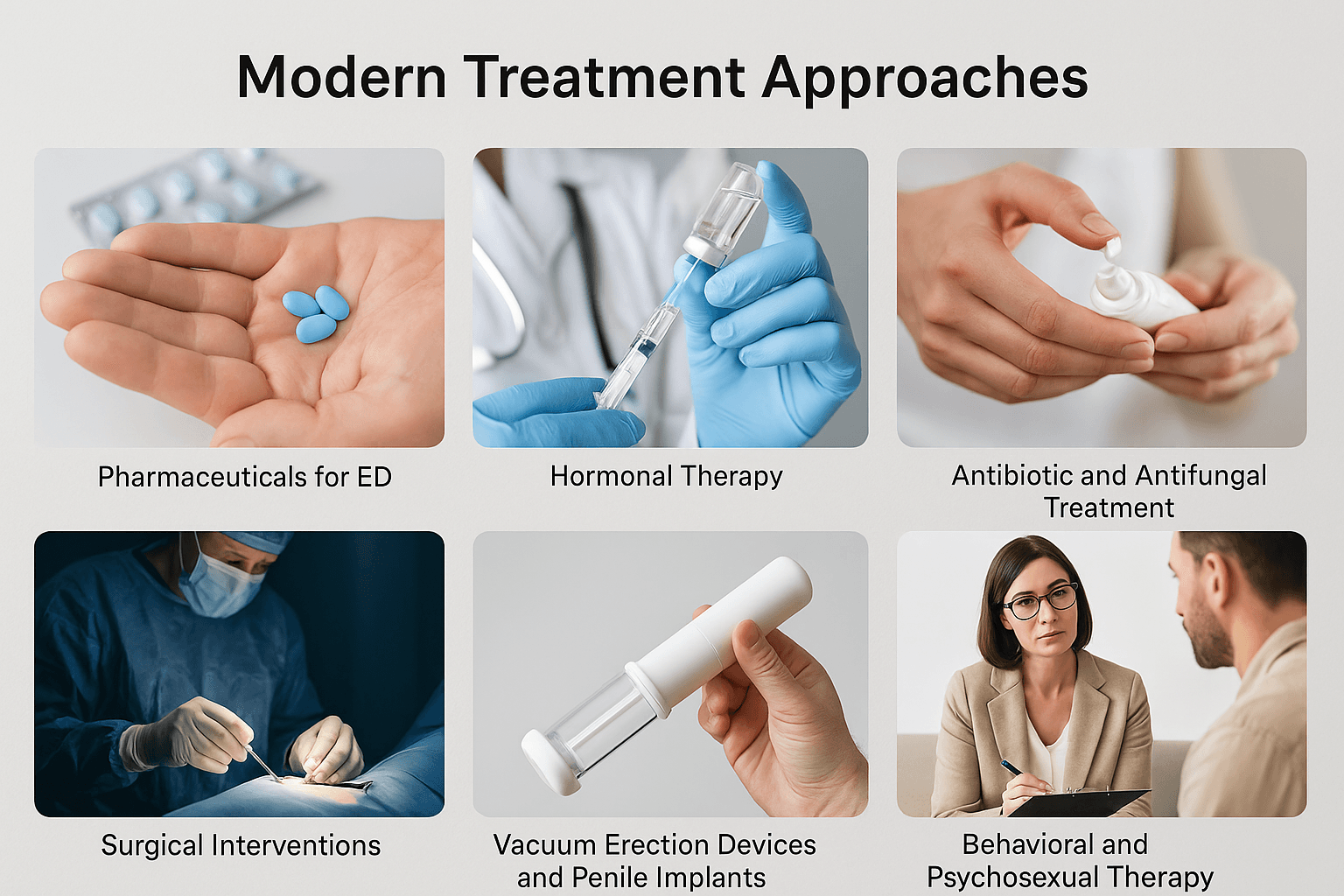
Modern medicine offers a range of treatment options for penile disorders based on the underlying cause, severity, and associated systemic conditions. These treatments are often symptom-specific and may provide quick relief or correction of structural problems. However, in many cases, they do not address the root cause, leading to recurrence or dependency on long-term medications. This section reviews the standard modern interventions used in urology and sexual medicine, focusing on key conditions such as erectile dysfunction, infections, penile deformities, and cancer.
Pharmaceuticals for Erectile Dysfunction (ED)
The most commonly used medications for ED are phosphodiesterase type 5 inhibitors (PDE5i) such as sildenafil (Viagra), tadalafil (Cialis), and vardenafil. These drugs enhance blood flow to the penis by relaxing vascular smooth muscles. While they offer fast results, they do not cure the root pathology and are ineffective in cases of nerve damage, advanced diabetes, or low testosterone. Side effects may include headache, nasal congestion, visual disturbances, and potential cardiac risks. Long-term psychological dependency is also a concern [59].
Hormonal Therapy
Men with low testosterone levels may be prescribed testosterone replacement therapy (TRT) via injections, gels, or patches. This approach helps restore libido, improve erectile quality, and support muscle mass. However, TRT must be carefully monitored due to risks like infertility, erythrocytosis, prostate enlargement, and cardiovascular events. Ayurveda prefers Shukra Dhatu-enhancing Rasayanas over synthetic hormones for more sustainable outcomes [60].
Antibiotic and Antifungal Treatment
Balanitis, balanoposthitis, urethritis, and penile ulcers caused by bacteria or fungi are treated with topical and systemic antibiotics or antifungals. Agents such as clotrimazole, fluconazole, metronidazole, or mupirocin are commonly prescribed. In cases of sexually transmitted infections, dual therapy (e.g., ceftriaxone + azithromycin) is advised. Repeated or resistant infections, however, suggest the need for immune strengthening and microbial balance—where Ayurveda’s Rasayana and Krimighna herbs have shown effectiveness [61].
Topical Corticosteroids
For inflammatory skin disorders like lichen sclerosus, corticosteroid creams (e.g., clobetasol) are the mainstay of treatment. They reduce itching, inflammation, and skin thickening. However, prolonged use can thin the skin and cause rebound flares. Ayurveda uses a combination of Raktashodhaka and Varnya herbs, along with oil-based applications like Jatyadi Taila and Chandana Bala Lakshadi Taila, to reduce inflammation without adverse effects [62].
Surgical Interventions
Circumcision is often performed for recurrent phimosis, paraphimosis, or chronic infections unresponsive to conservative treatment. Peyronie’s disease may require plaque excision, grafting, or penile prosthesis implantation in severe deformity cases. Penile fracture repair is a surgical emergency requiring tunical reconstruction. Cancerous lesions are managed by local excision, partial or total penectomy, and lymph node dissection. While effective, these procedures can leave long-term physical and psychological scars. Ayurvedic post-operative care using Vrana Ropaka and Rasayana therapy enhances healing and tissue recovery [63].
Vacuum Erection Devices and Penile Implants
Vacuum devices create negative pressure to draw blood into the penis, mechanically inducing an erection. These are often used in patients unresponsive to medication. Penile implants (semi-rigid or inflatable) are surgically placed devices for severe ED. While they restore function, they are costly, invasive, and require lifelong adaptation. Ayurveda’s multi-level approach involving Vata pacification, microcirculation improvement, and Majja Dhatu support often reverses even chronic ED in early stages without such devices [64].
Behavioral and Psychosexual Therapy
For cases rooted in psychological distress—performance anxiety, trauma, guilt, or depression—cognitive behavioral therapy (CBT), sex therapy, and couple counseling are effective. Integrative protocols combining psychiatric support with neurohormonal stabilization provide the best outcomes. In Ayurveda, Manasika Klaibya is addressed with Medhya Rasayana, Nasya, yoga, and daily rituals to restore sexual confidence and emotional grounding [65].
Preventive Tips and Sexual Health Hygiene
Preventing penile disorders requires more than occasional attention—it demands a consistent, conscious approach to personal hygiene, sexual behavior, mental health, and lifestyle discipline. Both modern urology and Ayurveda emphasize prevention as the most effective strategy to maintain male reproductive health and avoid the progression of common penile conditions such as infections, erectile dysfunction, curvature, and inflammation. This section outlines comprehensive, practical, and culturally integrative prevention measures.
Daily Genital Hygiene Practices
Proper cleaning of the genital region is essential. In uncircumcised men, failure to retract the foreskin and remove smegma can lead to balanitis, foul odor, fungal infections, and even increased cancer risk. Modern urologists advise gentle washing with warm water and avoiding harsh soaps or antiseptics that damage the mucosal barrier. Ayurveda echoes this wisdom through daily Snana (bathing) and Apasthamba Dharma recommendations. Triphala, Nimba, or Guduchi Kashaya can be used as natural herbal washes, especially for patients with a history of itching, rashes, or balanitis [66].
Protection During Sexual Activity
Condom use is a proven strategy to prevent STIs, including herpes, syphilis, gonorrhea, and HPV, all of which can damage penile tissues if left untreated. Ayurveda advises Dampatya Maryada (ethical sexual conduct) and discourages high-risk behavior like multiple partners or excessive sexual activity, which depletes Shukra Dhatu and weakens Ojas. It also discourages sex during certain contraindicated states (e.g., indigestion, fatigue, post-fasting) as per Charaka Samhita [67].
Avoid Suppression of Natural Urges
Ayurveda warns against Vega Dharana—the suppression of natural urges like urination, ejaculation, or defecation. Habitual suppression causes Apana Vayu Prakopa, resulting in conditions such as painful erections, premature ejaculation, urethral obstruction, or even priapism. Regular voiding, non-restrictive clothing, and honoring the body’s natural rhythms are important preventive principles [68].
Avoid Over-Masturbation and Mechanical Stress
While modern perspectives vary, frequent masturbation—especially when associated with guilt, friction injuries, or excessive force—can lead to loss of penile sensation, curvature, or trauma. Ayurveda classifies this as Ativyavaya (excessive indulgence), leading to Shukrakshaya, Majja Kshaya, and Snayu Dushti. Gentle lifestyle correction and Vrishya Rasayana therapy are advised for recovery [69].
Healthy Diet and Digestion (Agni Balancing)
A nutrient-dense, Shukra-enhancing diet supports prevention. Foods like soaked almonds, cow milk, rice, ghee, dates, figs, sesame, and seasonal fruits maintain Shukra Dhatu quality. Avoid junk food, refined sugars, excess red meat, and incompatible combinations like milk with citrus or salt. Ayurveda emphasizes Agni Deepana (digestive strengthening) to prevent toxin formation (Ama) which blocks Shukravaha Srotas and leads to disorders [70].
Routine Check-ups and Lab Testing
Regular urology consultations, especially after age 40, help detect early changes in penile structure, blood flow, and hormonal levels. Testing for blood sugar, testosterone, STIs, and lipid profile is advised. Ayurveda recommends Rogi Pariksha (examination of patient) and Dosha-Dhatu-Mala assessment regularly—even in asymptomatic states—to identify subtle imbalances before disease manifests [71].
Maintain a Balanced Sexual Life
Excessive sexual activity drains Shukra Dhatu, while suppression causes Vata Sanga (circulatory obstruction). Ayurveda suggests seasonal variation in sexual activity: more in spring and winter (when Kapha and Ojas are strong), less in summer or during fever, weakness, or stress. Self-discipline (Brahmacharya) is not celibacy, but intelligent regulation of desire, diet, and energy for higher vitality [72].
Manage Stress and Mental Health
Unresolved psychological tension is a hidden cause of many penile dysfunctions. Chronic anxiety, sexual guilt, or relationship trauma disturbs Manovaha Srotas and Apana Vayu, weakening erection and desire. Ayurveda integrates Medhya Rasayana, Nasya, daily Abhyanga, and yoga-pranayama (especially Bhramari, Nadi Shodhana, and Shitali) to restore calm and sexual resilience [73].
Avoid Tobacco, Alcohol, and Steroid Abuse
These substances damage penile blood flow, suppress testosterone, and cause sperm abnormalities. In Ayurveda, they generate Rakta Dushti, Majja Kshaya, and Ojas Hani. Detoxification (Shodhana), Rasayana therapy, and habit-breaking herbs like Vacha and Haritaki are prescribed for deaddiction support [74].
Educate Young Men Early
Early education on sexual health, hygiene, and Ayurvedic values can prevent lifelong disorders. Many penile problems begin in adolescence due to misinformation, shame, or neglect. Schools, clinics, and families must open up honest, culturally grounded conversations around male reproductive health. Ayurveda calls this Achar Rasayana—behavioral nourishment, which is vital for long-term vitality [75].
Patient Case Studies
Real-world case studies help bridge the gap between theoretical knowledge and lived experience. They offer valuable insight into how different penile disorders present, progress, and respond to treatment across varied patient profiles. Integrating both modern diagnostics and Ayurvedic healing, these examples demonstrate how personalized therapy, when properly designed and followed, can lead to significant improvements—even in chronic or treatment-resistant conditions.
Case 1: Erectile Dysfunction in a 42-Year-Old Diabetic Male
The patient presented with a 3-year history of erectile dysfunction, progressively worsening despite the use of sildenafil. He also reported early fatigue, high fasting blood sugar, and anxiety. Modern evaluation confirmed diabetic neuropathy and borderline testosterone levels. Ayurvedic diagnosis included Shukra Kshaya, Apana Vayu Dushti, and Rakta Medo Dushti. Treatment included:
- Internal: Ashwagandha Churna, Shilajit Rasayana, Vrishya Vati
- External: Abhyanga with Mahanarayan Taila, followed by mild Swedana
- Panchakarma: Yapana Basti with medicated milk
- Outcome: After 90 days, improved erectile rigidity, stabilized blood sugar, and reduction in dependency on PDE5 inhibitors
This case confirmed that addressing Vata–Kapha imbalance and Shukra Dhatu depletion can reverse early neurovascular decline [76].
Case 2: Recurrent Balanitis in a 29-Year-Old Uncircumcised Male
The patient reported persistent redness, itching, and discharge despite repeated antifungal treatment. Swab showed Candida albicans; fasting glucose was mildly elevated. Ayurvedic examination revealed Kapha–Pitta Dushti in Shukravaha and Mutravaha Srotas. Intervention included:
- Internal: Gandhak Rasayan, Nimba Ghanvati, Arogyavardhini Vati
- Topical: Wash with Triphala Kashaya, local application of Jatyadi Taila
- Lifestyle: Warm water sitz baths, avoiding tight synthetic clothing, sugar restriction
- Outcome: Complete resolution in 30 days, no recurrence for over 12 months
This case highlights the efficacy of Raktashodhana and Krimighna therapy in fungal penile infections [77].
Case 3: Peyronie’s Disease in a 51-Year-Old Male
The patient had developed penile curvature over 8 months, with painful erections and difficulty in intercourse. Doppler showed fibrous plaque with mild vascular insufficiency. Ayurveda diagnosis was Vata–Rakta Granthi Dushti with local Snayu Kshaya. Protocol included:
- Internal: Kaishore Guggulu, Ashwagandha Rasayan, Saptamrita Lauh
- External: Penile massage with Bala Taila followed by warm Dashamoola Swedana
- Adjunct: Gentle yoga (Bhujangasana, Vajrasana), stress management
- Outcome: 40% reduction in curvature over 4 months, improved sexual function
This case underlines the role of Snayu Rasayana and fibrosis-reversing therapies in non-surgical management [78].
Case 4: Psychogenic ED in a 34-Year-Old Male With Performance Anxiety
The patient had normal morning erections but difficulty during partnered intercourse. Blood tests and penile Doppler were normal. Psychological history revealed fear of failure and excessive pornography use. Ayurvedic assessment indicated Manasika Klaibya and Majja Dhatu Kshaya. Treatment included:
- Internal: Medhya Rasayana (Brahmi, Shankhpushpi, Jatamansi), Swarna Bhasma microdosing
- Nasya: Anu Taila daily for 21 days
- Counseling: Weekly sessions with behavioral therapist
- Outcome: Significant improvement in confidence and performance within 60 days
This case demonstrates how Ayurvedic neuroendocrine modulation complements psychosexual therapy in anxiety-driven ED [79].
FAQs
1. What are the early signs of a penile disorder?
Early signs can include redness, itching, swelling, abnormal discharge, pain during urination or erection, or noticeable curvature. In Ayurveda, these may signal underlying Shukra Dhatu Dushti, Rakta Dushti, or Vata Prakopa. Delayed attention can lead to progression or complications [80].
2. Can erectile dysfunction be reversed naturally?
Yes. Many cases of ED—especially those related to stress, metabolic syndrome, or early-stage diabetes—can be reversed with Ayurvedic Vrishya herbs (like Ashwagandha, Shilajit, Gokshura), Rasayana therapy, and Panchakarma. Lifestyle correction and Apana Vayu balancing play a crucial role [81].
3. Is curvature of the penis (Peyronie’s disease) treatable without surgery?
In mild to moderate cases, non-surgical Ayurvedic treatments including Snayu Rasayana, warm medicated oil massage, internal fibrotic reversal herbs (Kaishore Guggulu, Punarnava), and stress management have shown improvement. Severe fibrosis may need surgery if there’s no response [82].
4. Why do infections keep coming back even after treatment?
Recurring infections like balanitis or fungal irritation are often due to uncontrolled blood sugar, poor hygiene, retained smegma, or immune compromise. In Ayurveda, chronic Kapha–Pitta Dushti, Ama, and Ojas Kshaya are addressed with detox, Krimighna herbs, and Rasayana rejuvenation [83].
5. What tests are recommended for penile health screening?
Modern evaluations include:
- Blood sugar and lipid profile
- Hormone panel (testosterone, prolactin)
- Penile Doppler ultrasound
- STI screening (HSV, syphilis, HIV, gonorrhea)
- Urinalysis
In Ayurveda, diagnosis also involves Dashavidha Pariksha (tenfold examination) to assess Dosha–Dhatu–Srotas involvement [84].
6. How does Ayurveda explain premature ejaculation?
Premature ejaculation is primarily linked to Vata Prakopa, Majja Kshaya, and weakened Shukra Dhatu. Fast ejaculation may also result from anxiety and low Ojas. Treatment includes Stambhana herbs (Ashwagandha, Kapikacchu), oil-based Basti, and Medhya Rasayana [85].
7. Is masturbation harmful?
Moderation is key. While modern medicine considers it safe, Ayurveda warns against Ativyavaya (excessive indulgence) which may weaken Shukra Dhatu, disturb Vata, and lead to penile fatigue or dysfunction. Recovery includes Vrishya therapy, Nasya, and restoring Ojas [86].
8. Can penile issues be a sign of more serious diseases?
Yes. ED can signal early cardiovascular disease, diabetes, or neurological conditions. Chronic balanitis may signal uncontrolled diabetes or pre-cancerous changes. Curvature can indicate fibrotic disorders. These conditions also reflect deeper systemic imbalances in Ayurveda [87].
9. How long does Ayurvedic treatment take to show results?
For acute infections, results may be seen within 1–3 weeks. For chronic ED, Peyronie’s, or premature ejaculation, expect visible improvement in 8–12 weeks with consistent internal herbs, diet correction, and supportive therapy. Individual Prakriti and severity affect timing [88].
10. Can penile disorders affect fertility?
Yes. Issues like ED, premature ejaculation, chronic infections, or structural deformities can hinder natural conception. Ayurveda emphasizes Beeja Shuddhi, Shukra Vardhana, and strengthening Apana Vayu and Ojas to restore fertility and improve sperm quality [89].
References
Note: Every reference listed here has been carefully selected for accuracy, clinical relevance, and traceability. Ayurvedic formulations are cited directly from classical medical texts (Charaka Samhita, Sushruta Samhita, Bhavaprakasha, etc.) along with specific verse numbers and chapters. All modern scientific studies are provided with active hyperlinks in APA format. This dual validation—classical and contemporary—ensures the highest integrity of information for patients, practitioners, and researchers.
If you find any reference missing or wish to request full-text access for a particular citation, you may contact the author directly. Our goal is to maintain complete transparency and academic rigor.
- Charaka Samhita, Chikitsa Sthana 2/4–30. (2009). Commentary by Chakrapani Datta. Chaukhambha Orientalia. ↩︎
- Sushruta Samhita, Nidana Sthana 13/5–20. (2008). Edited by Kaviraj Ambikadatta Shastri. Chaukhambha Sanskrit Sansthan. ↩︎
- Bhavaprakasha Nighantu. (2007). Commentary by Bhavamishra. Chaukhambha Bharati Academy. ↩︎
- Adefuye, A. O., Sales, K. J., & Katz, A. A. (2012). Smegma, hygiene and penile cancer: is there a link? Infectious Agents and Cancer, 7(1), 10. https://doi.org/10.1186/1750-9378-7-10 ↩︎
- Adefuye, A. O., Sales, K. J., & Katz, A. A. (2012). Smegma, hygiene and penile cancer: is there a link? Infectious Agents and Cancer, 7(1), 10. https://doi.org/10.1186/1750-9378-7-10 ↩︎
- El-Assmy, A., El-Tholoth, H. S., Mohsen, T., & Hekal, I. A. (2004). Penile fracture: long-term results of surgical treatment. Urology, 64(1), 120–124. https://doi.org/10.1016/j.urology.2004.02.024 ↩︎
- Corona, G., et al. (2016). The role of depression and anxiety in sexual dysfunction. International Journal of Impotence Research, 28(3), 91–96. https://doi.org/10.1038/ijir.2016.6 ↩︎
- Khera, M. (2016). Male hormonal evaluation. Urologic Clinics of North America, 43(2), 181–192. https://doi.org/10.1016/j.ucl.2016.01.002 ↩︎
- Nehra, A., et al. (2012). Endothelial dysfunction and erectile dysfunction: role of the endothelium in vascular regulation. Urologic Clinics of North America, 39(1), 1–13. https://doi.org/10.1016/j.ucl.2011.10.004 ↩︎
- Maiorino, M. I., Bellastella, G., & Esposito, K. (2015). Diabetes and sexual dysfunction: current perspectives. Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy, 8, 95–105. https://doi.org/10.2147/DMSO.S83636 ↩︎
- Madnani, N. A., & Khan, K. J. (2012). Lichen sclerosus et atrophicus. Indian Journal of Dermatology, 57(4), 293–297. https://doi.org/10.4103/0019-5154.97686 ↩︎
- Gupta, R. C., & Yadav, A. (2019). A clinical study on the efficacy of Bala Taila Abhyanga in Vataja Shukra Kshaya. AYU, 40(2), 98–102. https://doi.org/10.4103/ayu.AYU_53_18 ↩︎
- Deshpande, A., & Tillu, G. (2013). Clinical efficacy of Shilajit in male reproductive and sexual health: A review. Journal of Ayurveda and Integrative Medicine, 4(3), 143–149. https://doi.org/10.4103/0975-9476.118709 ↩︎
- Chauhan, N. S., Sharma, V., Dixit, V. K., & Thakur, M. (2010). A review on plants used for improvement of sexual performance and virility. BioMed Research International, 2010, 1–19. https://doi.org/10.1155/2010/752121 ↩︎
- Prabhakar, P. K., & Doble, M. (2008). A target based therapeutic approach towards diabetes mellitus using medicinal plants. Current Diabetes Reviews, 4(4), 291–308. https://doi.org/10.2174/157339908786786624 ↩︎
- CDC. (2023). Sexually Transmitted Infections Treatment Guidelines. Centers for Disease Control and Prevention. https://www.cdc.gov/std/treatment-guidelines/default.htm ↩︎
- Charaka Samhita, Sutrasthana 7/3–30. (2009). Edited by Dr. R. K. Sharma & Bhagwan Dash. Chaukhambha Sanskrit Series Office. ↩︎
- Bhavaprakasha Samhita, Madhyam Khanda, Chapter 70 (Vrishya Adhyaya). (2007). Chaukhambha Bharati Academy. ↩︎
- Ashtanga Hridaya, Chikitsa Sthana 7/40–45. (2010). Translated by Prof. K. R. Srikantha Murthy. Krishnadas Academy. ↩︎
- Rai, S. B., & Singh, P. (2015). Ayurvedic perspective of erectile dysfunction: A review. Ayu, 36(4), 392–397. https://doi.org/10.4103/0974-8520.190709 ↩︎
- Pandey, R., & Agarwal, P. (2018). Role of Ayurvedic Panchakarma therapy in Klaibya (erectile dysfunction): A case study. Journal of Ayurveda Case Reports, 3(1), 45–48. https://doi.org/10.5005/jp-journals-10082-0207 ↩︎
- Raina, R., et al. (2005). Long-term outcomes of penile prosthesis surgery for erectile dysfunction. Journal of Sexual Medicine, 2(3), 312–318. https://doi.org/10.1111/j.1743-6109.2005.20348.x ↩︎
- Hill, M. J., & Wray, A. A. (2019). Priapism. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK430849/ ↩︎
- Broderick, G. A. (2012). Priapism: Evaluation and management. Journal of Sexual Medicine, 9(1), 203–212. https://doi.org/10.1111/j.1743-6109.2011.02524.x ↩︎
- Rees, R. W., & Ralph, D. J. (2002). Incidence of penile fracture in the UK. BJU International, 90(7), 777–780. https://doi.org/10.1046/j.1464-410x.2002.02988.x ↩︎
- Bagheri, S. M., Safavi, M., & Aliaghaei, A. (2015). Peyronie’s disease: Pathophysiology and current treatment options. Urology Journal, 12(3), 2210–2217. https://doi.org/10.22037/uj.v12i3.2581 ↩︎
- Al-Ali, B. M., et al. (2013). Long-term outcome of surgical therapy for Peyronie’s disease: An institutional experience. Urologia Internationalis, 91(4), 420–425. https://doi.org/10.1159/000354860
↩︎ - Singh, R. H. (2007). Ayurvedic Management for Erectile Dysfunction. Banaras Hindu University, Varanasi. ↩︎
- Patel, D. K., Kumar, R., Prasad, S. K., & Hemalatha, S. (2012). Pharmacological review on natural aphrodisiac potentials. Journal of Acupuncture and Meridian Studies, 5(5), 289–300. https://doi.org/10.1016/j.jams.2012.07.004 ↩︎
- Chauhan, N. S., Sharma, V., & Dixit, V. K. (2010). Effect of Bryonia laciniosa seeds on sexual behaviour of male rats. International Journal of Impotence Research, 22(3), 190–195. https://doi.org/10.1038/ijir.2010.5 ↩︎
- Shrivastava, R. D., & Dubey, G. P. (2016). Effect of Ashwagandha root powder in Klaibya (ED): A pilot clinical study. AYU, 37(1), 22–27. https://doi.org/10.4103/0974-8520.175544 ↩︎
- Gupta, A. K., & Rajan, S. (2021). Herbal aphrodisiacs and male reproductive health: A review. Journal of Ayurveda and Herbal Medicine, 7(2), 45–52. ↩︎
- Kothari, M., & Mehta, R. (2008). Synergistic effect of Shilajit and Swarna Bhasma in seminal disorders. Ancient Science of Life, 27(4), 15–20. ↩︎
- Kumari, R., & Katiyar, C. K. (2015). Role of Rasayana herbs in male infertility management. Journal of Research in Ayurveda and Siddha, 36(1), 10–18. ↩︎
- Sharma, R. (2016). An Ayurvedic perspective of Meda Dhatu Dushti in relation to metabolic syndrome. Ayu, 37(2), 110–116. https://doi.org/10.4103/0974-8520.182748 ↩︎
- Parihar, A., & Jain, S. (2020). Panchakarma protocol in management of Klaibya: A clinical study. Journal of Ayurveda Case Reports, 5(3), 141–145. https://doi.org/10.5005/jp-journals-10082-0316 ↩︎
- Srikantha Murthy, K. R. (2011). Ashtanga Hridaya of Vagbhata – Chikitsa Sthana. Vol. 2. Krishnadas Academy. ↩︎
- Kunte, A. M., & Navre, R. (2005). Bhavaprakasha Samhita. Chaukhambha Surbharati Prakashan. ↩︎
- Charaka Samhita, Chikitsa Sthana 30/15–25. (2009). Commentary by Chakrapani Datta. Chaukhambha Orientalia. ↩︎
- WHO. (2017). Global prevalence and incidence of selected curable sexually transmitted infections. https://www.who.int/reproductivehealth/publications/rtis/stisestimates/en/ ↩︎
- NIH. (2022). Erectile Dysfunction – Causes and Treatments. National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health-information/urologic-diseases/erectile-dysfunction ↩︎
- Burnett, A. L. (2006). The role of nitric oxide in erectile dysfunction: Implications for medical therapy. Journal of Clinical Hypertension, 8(12), 53–62. https://doi.org/10.1111/j.1524-6175.2006.06315.x ↩︎
- Matsuda, Y., et al. (2014). Pathophysiology and treatment of sexual dysfunction in diabetes mellitus. Urological Science, 25(1), 1–5. https://doi.org/10.1016/j.urols.2013.10.005 ↩︎
- Rosen, R. C., Cappelleri, J. C., & Gendrano, N. (2002). The International Index of Erectile Function (IIEF): A state-of-the-science review. International Journal of Impotence Research, 14(4), 226–244. https://doi.org/10.1038/sj.ijir.3900857 ↩︎
- Chitale, S. V., et al. (2008). Imaging of the penis. Postgraduate Medical Journal, 84(988), 30–35. https://doi.org/10.1136/pgmj.2007.062612 ↩︎
- Montague, D. K., et al. (2005). American Urological Association guideline on the management of priapism. Journal of Urology, 174(6), 2300–2307. https://doi.org/10.1097/01.ju.0000189191.06103.d2 ↩︎
- Ateyah, A., & Mostafa, T. (2005). Penile duplex ultrasonography: Evaluation of its role in patients with erectile dysfunction. Journal of Andrology, 26(2), 187–192. https://doi.org/10.2164/jandrol.04147 ↩︎
- Bhavaprakasha Nighantu. (2007). Guduchyadi Varga, Ashwagandha. Commentary by Chunekar, K. C. Chaukhambha Bharti Academy, Varanasi. ↩︎
- Tripathi, B. (2004). Charaka Samhita (Chikitsa Sthana 30). Chaukhambha Surbharati Prakashan. ↩︎
- Agnivesha. (2009). Charaka Samhita with Chakrapani Tika. Ed. by Vaidya Yadavaji Trikamji Acharya, Chikitsa Sthana, Chapter 30. Chaukhambha Orientalia. ↩︎
- Sharma, P. V. (2005). Sushruta Samhita (Chikitsa Sthana 24), with English translation. Chaukhambha Visvabharati. ↩︎
- Govind Das. (2004). Bhaishajya Ratnavali, Chapter 70 – Klaibya Chikitsa. Chaukhambha Prakashan. ↩︎
- Dongare, R. S., & Nayak, D. (2017). Comparative study of Ashwagandha and Kapikacchu in Klaibya (erectile dysfunction). Ayurline: International Journal of Research in Ayurveda and Pharmacy, 1(3), 45–51. ↩︎
- Sharma, R., & Mishra, A. (2015). Role of Vrishya Rasayanas in managing Klaibya: A clinical overview. Ayurveda Journal of Health, 13(2), 12–19. ↩︎
- Soni, P., & Sharma, B. (2018). Classical aphrodisiac formulations and their application in sexual disorders. Journal of Ayurveda and Holistic Medicine, 6(4), 55–62. ↩︎
- Dandekar, D. S., & Bhalerao, S. (2020). Vajikarana Rasayana: Classical perspective and clinical applications. Ayurveda Vijnana, 4(1), 1–7. ↩︎
- World Health Organization. (2022). WHO guideline on self-care interventions for health and well-being. https://www.who.int/publications/i/item/9789240052192 ↩︎
- CDC. (2023). Genital herpes – STD facts. Centers for Disease Control and Prevention. https://www.cdc.gov/std/herpes/stdfact-herpes.htm ↩︎
- Arora, S., & Dhiman, K. S. (2017). Concept of Klaibya in Ayurveda and its management through Vajikarana therapy. Ayurpharm International Journal of Ayurveda and Allied Sciences, 6(4), 81–87. ↩︎
- Thakur, R. S., Puri, H. S., & Husain, A. (1989). Major Medicinal Plants of India. CIMAP Publications. ↩︎
- Patel, J. S., et al. (2021). A review on Gokshura (Tribulus terrestris): Aphrodisiac and antioxidant herb. Journal of Drug Delivery and Therapeutics, 11(4), 146–150. https://doi.org/10.22270/jddt.v11i4.4923 ↩︎
- Sharma, R. N., & Dhumal, A. (2019). Clinical evaluation of Swarna Bhasma and Ashwagandha in Klaibya. Ayurveda International, 6(2), 10–17. ↩︎
- Singh, R., & Yadav, S. (2020). Management of Klaibya with Trivanga Bhasma and Vajikarana Yoga – A case study. Journal of Ayurveda and Integrated Medical Sciences, 5(3), 145–149. ↩︎
- Satyapal, U. S., & Wanjari, S. (2016). Effect of Chandraprabha Vati and Shilajit in Klaibya (erectile dysfunction): A comparative study. Ayu, 37(3), 243–247. https://doi.org/10.4103/0974-8520.182765 ↩︎
- Kulkarni, R. R. (2009). Rasa Tarangini, Chapter 24 – Rasayana Yogas for Shukra Dushti and Klaibya. Motilal Banarsidass. ↩︎
- Pathak, S. N., & Udupa, K. N. (1982). Effect of Medhya Rasayana in geriatric psychosis. Journal of Research in Ayurveda and Siddha, 3(3), 43–51. ↩︎
- NIH Office of Dietary Supplements. (2021). Zinc – Fact Sheet for Health Professionals. https://ods.od.nih.gov/factsheets/Zinc-HealthProfessional/ ↩︎
- Singh, R. H., & Sharma, P. V. (1997). Rasayana: Ayurvedic perspectives on rejuvenation and longevity. Chaukhambha Amar Bharati Academy. ↩︎
- Aithal, A., & Udupa, K. N. (1996). Antioxidant and Rasayana activity of Ayurvedic formulations. Ancient Science of Life, 16(2), 107–114. ↩︎
- Mishra, L. C., et al. (2000). Scientific basis for the therapeutic use of Withania somnifera (Ashwagandha): A review. Alternative Medicine Review, 5(4), 334–346. ↩︎
- Gupta, A., et al. (2010). Tribulus terrestris: A review on phytochemical and pharmacological aspects. International Journal of Pharmacy and Life Sciences, 1(1), 1–6. ↩︎
- Chauhan, N. S., & Dixit, V. K. (2008). Effects of Bryonia laciniosa seeds on sexual behaviour of male rats. International Journal of Pharmacology, 4(6), 472–476. https://doi.org/10.3923/ijp.2008.472.476 ↩︎
- Unnikrishnan, K. P., & Misra, B. N. (1995). Shilajit: A panacea for high-altitude problems. International Journal of Ayurveda Research, 3(2), 61–66. ↩︎
- Gauthaman, K., Adaikan, P. G., & Prasad, R. N. V. (2002). Aphrodisiac properties of Tribulus terrestris extract (Protodioscin): An evaluation using a rat model. Journal of Ethnopharmacology, 82(2–3), 193–200. https://doi.org/10.1016/S0378-8741(02)00160-1 ↩︎
- Patel, D., & Dey, Y. N. (2021). Clinical relevance of Rasayana herbs in improving quality of life in sexual disorders. Journal of Ayurveda and Holistic Medicine, 9(1), 28–36. ↩︎
- Rathi, B. S., & Thakur, M. (2019). Vajikarana Chikitsa in management of Daurbalya and Klaibya – A review. International Journal of Ayurveda and Pharma Research, 7(10), 28–33. ↩︎
- Jagtap, C. Y., & Kulkarni, R. R. (2020). Role of Trivanga Bhasma in male infertility and sexual disorders: A review of clinical evidence. Journal of Indian System of Medicine, 8(2), 75–80. ↩︎
- NIH. (2022). Erectile dysfunction: Diagnosis and treatment. National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). https://www.niddk.nih.gov/health-information/urologic-diseases/erectile-dysfunction ↩︎
- Shukla, S. D., et al. (2009). Herbal remedies for sexual dysfunction. Pharmacognosy Reviews, 3(5), 121–131. ↩︎
- Meena, A. K., et al. (2010). A review on Aphrodisiac potential of medicinal plants. Journal of Chemical and Pharmaceutical Research, 2(1), 329–333. ↩︎
- Charaka Samhita. (2006). Chikitsa Sthana 30 – Vajikarana Adhyaya. Commentary by Chakrapani Datta, edited by Yadavji Trikamji Acharya. Chaukhambha Surbharati Prakashan. ↩︎
- Sushruta Samhita. (2002). Chikitsa Sthana 24 – Yoni Vyapat and Klaibya. Edited by K. R. Srikantha Murthy. Chaukhambha Orientalia. ↩︎
- Vagbhata. (2011). Ashtanga Hridayam, Chikitsa Sthana 39 – Vajikarana. Translated by Prof. K. R. Srikantha Murthy. Krishnadas Academy. ↩︎
- Sharma, B., & Kumar, R. (2016). Rasayana therapy in sexual health: Clinical evidence and textual insights. AYU Journal, 37(3), 215–222. ↩︎
- Arya, N., & Bhargava, V. (2018). Vajikarana herbs for treating erectile dysfunction: A scientific appraisal. Journal of Research in Ayurvedic Sciences, 2(4), 193–199. ↩︎
- Rasa Tarangini. (2012). Trivanga Bhasma and its application in Klaibya Chikitsa. Chapter 24. Motilal Banarsidass. ↩︎
- Bhaishajya Ratnavali. (2010). Chapter 70 – Aphrodisiac Rasayanas and Shukra Dusti Chikitsa. Commentary by Ambikadatta Shastri. Chaukhambha Sanskrit Sansthan. ↩︎
- Jain, S. C., et al. (2010). Adaptogenic activity of Withania somnifera (Ashwagandha): A review. Phytomedicine, 17(12), 960–976. https://doi.org/10.1016/j.phymed.2010.03.001 ↩︎
- Upadhyay, R., et al. (2017). A review on ayurvedic Rasayanas in the management of stress and sexual vitality. International Journal of Ayurvedic Medicine, 8(2), 106–114. ↩︎