- The Pattern Most Patients Notice After Surgery
- What “Failed Surgery” Actually Means (Persistent vs Recurrent)
- When Surgery Has Not Truly Failed, But Recovery Still Feels Wrong
- When the Original Diagnosis Was Wrong Before Surgery
- The Most Common True Reasons Parathyroid Surgery Fails
- Why Imaging and Surgical Planning Still Have Limits
- When Surgery Appears Successful but Disease Returns Silently
- Why Reoperative Parathyroid Surgery Is More Complex
- Reality Check: Not Every “Normal” Result Means Full Recovery
- The Functional Gap: What Surgery Does Not Address
- An Integrative Perspective on Restoring Calcium Balance
- When an Integrative Approach May Be Considered
- What Patients Often Realize Too Late
- Case Study
- What Should You Do Next
- When to Consider Further Evaluation
- FAQs
- Reference
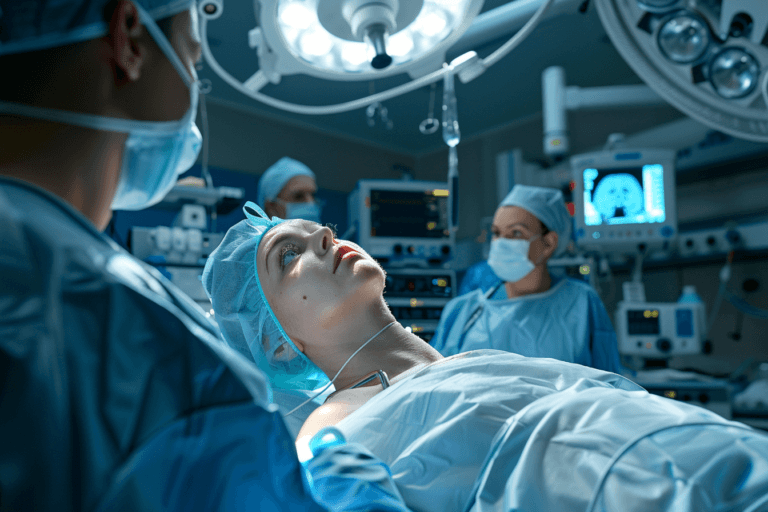
The Pattern Most Patients Notice After Surgery
Why parathyroid surgery fails is a concern many patients face when symptoms continue even after a technically successful procedure. While surgery removes the abnormal gland, recovery is not always complete, and persistent symptoms or abnormal calcium levels can still occur.
For many patients, the journey after parathyroid surgery does not follow the clear, linear recovery they were expecting. Initially, there may be a sense of relief when calcium levels begin to normalize or when the surgeon confirms that the abnormal gland has been removed. However, over the following weeks or months, a different pattern often starts to emerge. Symptoms that were expected to resolve completely may persist, fluctuate, or return subtly, creating confusion and concern.
Patients commonly report ongoing fatigue, low energy levels, difficulty concentrating, or a vague sense that their health has not fully returned to normal. Some continue to experience bone discomfort, muscle weakness, or intermittent digestive issues. Even more frustrating is the situation where follow-up lab reports fall within the “normal” range, yet the individual still feels unwell. This mismatch between laboratory results and lived experience is one of the most frequently overlooked aspects of postoperative recovery in parathyroid disorders. [5]
From a clinical perspective, this pattern is not entirely unexpected. Primary hyperparathyroidism is not limited to a single gland but affects multiple systems in the body, including bones, kidneys, and metabolic regulation. As a result, even after successful removal of the overactive gland, the body may take time to recalibrate, and in some cases, may not fully return to its previous balance. This explains why symptoms can linger despite technically successful surgery. [4]
In routine practice, healthcare systems often rely heavily on biochemical markers such as calcium and parathyroid hormone levels to assess outcomes. While these markers are important, they do not always capture the full clinical picture. Patients may be reassured that everything is “normal,” even when their symptoms suggest otherwise. This gap between clinical measurements and patient experience is increasingly recognized in real-world care settings. [16]
Understanding this pattern is the first step in recognizing that postoperative recovery is not always straightforward. It sets the foundation for exploring deeper reasons why symptoms may persist and why, in some cases, surgery alone may not fully resolve the condition.
Table: Parathyroid Surgery Outcomes: Quick Clinical Snapshot
| Outcome Type | What It Means | What Patients Experience |
|---|---|---|
| Successful Surgery | Calcium normalizes | Symptoms improve gradually |
| Persistent Disease | Calcium never normalizes | Symptoms continue immediately |
| Recurrent Disease | Calcium returns after months/years | Symptoms return slowly |
| Partial Recovery | Labs improve but symptoms remain | Confusion and incomplete recovery |
What “Failed Surgery” Actually Means (Persistent vs Recurrent)
When discussing why parathyroid surgery fails, it is important to clarify what “failure” means in clinical practice. Not all unsatisfactory outcomes are the same. Specialists clearly differentiate between persistent and recurrent hyperparathyroidism, as this distinction determines whether the issue remained after surgery or developed later. [8]
Table: Persistent vs Recurrent Hyperparathyroidism
| Feature | Persistent | Recurrent |
|---|---|---|
| Timing | Within 6 months | After 6 months |
| Cause | Missed gland or incomplete removal | Regrowth or new gland activity |
| Lab Pattern | Calcium never normal | Initially normal, then rises |
| Management | Re-evaluation required | Long-term monitoring needed |
Persistent Hyperparathyroidism
Persistent hyperparathyroidism refers to a situation where calcium levels do not return to normal after surgery or become elevated again within the first six months. This indicates that the underlying cause was not completely addressed during the initial procedure. Common reasons include a missed adenoma, unrecognized multigland disease, or ectopic parathyroid tissue that was not removed. [1]
From a clinical perspective, persistent disease suggests that the source of excess parathyroid hormone remained active at the time of surgery. This highlights the importance of accurate diagnosis and complete removal of all abnormal tissue.
Recurrent Hyperparathyroidism
Recurrent hyperparathyroidism occurs when calcium levels initially normalize after surgery but increase again after six months or more. This pattern reflects a return of the condition rather than incomplete treatment. [10]
Recurrence may result from regrowth of abnormal tissue, activation of previously inactive glands, or underlying multigland involvement that was not fully evident during the first surgery. In some cases, genetic factors may also contribute, making long-term follow-up essential.
Why This Distinction Matters
The difference between persistent and recurrent disease directly influences the next step in care. Persistent cases often point toward incomplete initial treatment, while recurrent cases suggest a more complex or evolving condition.
Recognizing this distinction early helps guide further evaluation and prevents unnecessary confusion, especially in patients who continue to experience symptoms after surgery.
When Surgery Has Not Truly Failed, But Recovery Still Feels Wrong
In some patients, recovery after parathyroid surgery does not feel complete, even though the procedure has achieved its intended biochemical outcome. Calcium levels may return to the normal range, and the surgery may be considered successful from a clinical standpoint. However, symptoms such as fatigue, weakness, or a general sense of imbalance can continue.
This situation often leads to confusion, especially when patients are reassured that their reports are normal while their physical experience suggests otherwise. It is important to recognize that not every postoperative concern reflects surgical failure. In many cases, the body is still adjusting after a prolonged period of hormonal imbalance, and this adjustment phase can produce symptoms that resemble ongoing disease.
Normocalcemic High PTH After Surgery
One commonly observed pattern after surgery is elevated parathyroid hormone levels despite normal calcium levels. This does not necessarily indicate that the surgery has failed. Clinical studies have shown that a subset of patients continues to have elevated PTH after successful removal of the abnormal gland without immediate recurrence of hypercalcemia. [12]
Several factors can contribute to this pattern, including vitamin D deficiency, increased calcium demand during bone recovery, altered kidney handling of calcium, or the severity of the disease before surgery. In many cases, these levels stabilize over time without requiring further surgical intervention. [13]
Because of this, interpreting PTH levels alone can be misleading. A broader clinical view that includes symptoms, trends over time, and overall metabolic status is more reliable.
Hungry Bone Syndrome and Postoperative Changes
Another important factor affecting recovery is hungry bone syndrome, which can occur after removal of an overactive parathyroid gland. Once excess hormone stimulation is removed, bones begin to absorb calcium rapidly in an effort to rebuild lost density.
This process can temporarily lower calcium levels, leading to symptoms such as tingling, muscle cramps, fatigue, or weakness. Although uncomfortable, this reflects a physiological correction rather than a failed surgical outcome. [11]
These early postoperative changes are often misunderstood, especially if patients are not informed in advance. Recognizing these patterns helps differentiate normal recovery processes from true surgical failure and prevents unnecessary concern or premature decisions regarding further treatment.
When the Original Diagnosis Was Wrong Before Surgery
In some cases, what appears to be failed parathyroid surgery is not due to the procedure itself but rather an issue with the initial diagnosis. Primary hyperparathyroidism shares overlapping features with other conditions that also cause elevated calcium or parathyroid hormone levels. If these conditions are not correctly identified before surgery, the outcome may seem ineffective, even though the surgery was technically performed as planned.
Accurate preoperative evaluation is therefore critical. Without proper differentiation between similar conditions, patients may undergo surgery that does not address the actual underlying cause of their abnormal laboratory findings.
Familial Hypocalciuric Hypercalcemia
Familial hypocalciuric hypercalcemia is a genetic condition that can closely resemble primary hyperparathyroidism. Patients typically present with mildly elevated calcium levels and normal or slightly increased parathyroid hormone levels, making it difficult to distinguish without specific testing. [5]
A key differentiating factor is low calcium excretion in urine, which can be identified through a 24-hour urine calcium test. In this condition, surgery is generally not indicated, as the underlying issue is not caused by an overactive parathyroid gland. Case reports and clinical observations show that when this condition is misdiagnosed as primary hyperparathyroidism, patients may undergo surgery without any meaningful improvement in their biochemical profile. [15]
Secondary Causes and Misclassification
Elevated parathyroid hormone levels can also occur as a secondary response to other physiological imbalances rather than a primary gland disorder. Conditions such as vitamin D deficiency or impaired kidney function can lead to compensatory increases in parathyroid hormone, which may be mistaken for primary hyperparathyroidism if not carefully evaluated. [5]
In such situations, the parathyroid glands are responding appropriately to a systemic issue rather than functioning abnormally. Treating the underlying cause, such as correcting vitamin D levels or addressing renal factors, often leads to normalization without the need for surgery. This highlights the importance of a comprehensive diagnostic approach before proceeding with surgical intervention. [4]
Recognizing these diagnostic pitfalls helps explain why some patients do not experience expected improvements after surgery. It reinforces the need for thorough evaluation and accurate classification before making treatment decisions
The Most Common True Reasons Parathyroid Surgery Fails
Even when the diagnosis is correct and the procedure is performed appropriately, there are well-recognized clinical reasons why parathyroid surgery may not achieve complete resolution. These causes are documented in surgical guidelines and clinical reviews and often relate to the complexity of gland identification and disease behavior rather than a simple technical error.
Table: Most Common Reasons Why Parathyroid Surgery Fails
| Cause | What Happens | Impact on Patient |
|---|---|---|
| Missed Adenoma | Abnormal gland not removed | Persistent high calcium |
| Multigland Disease | Multiple glands overactive | Temporary improvement only |
| Ectopic Gland | Gland located outside neck | Difficult to detect |
| Incomplete Resection | Partial removal of tissue | Recurrence or persistence |
Missed Adenoma
One of the most common causes of persistent disease is a missed parathyroid adenoma. In some patients, more than one abnormal gland may be present, or the primary gland may not be clearly identified during imaging or surgery. Due to the small size and variable location of parathyroid glands, it is possible for an abnormal gland to remain undetected, especially if preoperative localization is inconclusive. [1]
Clinical literature highlights that even with modern imaging and surgical techniques, missed adenomas remain a recognized cause of persistent hyperparathyroidism. This is particularly relevant in patients who show little or no improvement in calcium levels after surgery. [8]
Multigland Disease
Multigland disease refers to a condition where more than one parathyroid gland is overactive. This is different from a single adenoma and requires a different surgical approach. If only one gland is removed while others remain hyperfunctioning, the patient may initially show partial improvement but later experience persistent or recurrent hyperparathyroidism. [8]
This condition is often underestimated before surgery because imaging studies are more effective at identifying a single dominant gland rather than multiple mildly enlarged glands. Clinical reviews and surgical guidelines emphasize that multigland involvement is a significant contributor to both persistent and recurrent disease. [10]
Accurate identification of multigland disease requires careful intraoperative assessment and, in some cases, advanced monitoring techniques. Without this, the likelihood of incomplete resolution increases. [1]
Ectopic Parathyroid Tissue
Parathyroid glands do not always reside in their typical anatomical position in the neck. During embryological development, these glands can migrate to unusual locations such as the mediastinum, within the thymus, or even inside the thyroid tissue. These are referred to as ectopic parathyroid glands.
Ectopic tissue is a well-documented cause of failed or persistent hyperparathyroidism, as it may not be detected during routine imaging or may be located outside the standard surgical field. Case-based evidence shows that such glands can remain active after surgery and continue to produce excess hormone. [14]
Clinical studies further confirm that ectopic localization significantly increases the complexity of both initial and repeat surgeries. [8]
Incomplete Resection
Incomplete removal of abnormal parathyroid tissue is another important cause of surgical failure. This may occur when a portion of the diseased gland is inadvertently left behind or when additional abnormal tissue is not recognized during the procedure.
In some cases, the gland may appear partially normal, leading to conservative removal, which later proves insufficient. Surgical guidelines emphasize the importance of complete excision of all hyperfunctioning tissue to achieve long-term resolution. [1]
Recurrent or persistent disease due to incomplete resection often requires re-evaluation and, in some cases, repeat surgery, which carries higher complexity and risk. [10]
These factors collectively explain why even technically well-performed surgeries may not always result in complete and lasting resolution of the condition.
Why Imaging and Surgical Planning Still Have Limits
Even with modern advances in diagnostic technology and surgical techniques, parathyroid surgery is not always straightforward. Outcomes depend heavily on accurate localization of abnormal glands and real-time decision-making during the procedure. Despite improvements in imaging and intraoperative tools, there are inherent limitations that can affect surgical success.
Table : Imaging vs Reality in Parathyroid Surgery
| Imaging Method | Strength | Limitation |
|---|---|---|
| Ultrasound | Easily available | Misses small or deep glands |
| Sestamibi Scan | Functional detection | Not reliable in multigland disease |
| 4D-CT | Better localization | Expensive and not always accurate |
| MRI | Useful in complex cases | Limited routine use |
Imaging Limitations
Preoperative imaging plays a central role in planning parathyroid surgery. Common modalities include ultrasound, sestamibi scans, and advanced techniques such as 4D-CT. While these tools are valuable, they are not completely reliable in all cases. False-negative results can occur when abnormal glands are too small, have atypical features, or are located in unusual anatomical positions. [7]
Additionally, imaging is generally more effective at identifying a single dominant adenoma rather than multiple mildly enlarged glands. This means that multigland disease may go undetected before surgery, increasing the risk of incomplete treatment. Clinical reviews highlight that reliance on imaging alone can lead to mislocalization or underestimation of disease extent. [8]
Because of these limitations, imaging should be viewed as a guide rather than a definitive diagnostic tool.
Intraoperative PTH Monitoring
To improve surgical accuracy, many surgeons use intraoperative parathyroid hormone monitoring. This technique measures PTH levels during surgery to assess whether the source of excess hormone has been successfully removed.
A significant drop in PTH levels during the procedure suggests that the abnormal gland has been excised. However, this method also has limitations. In cases of multigland disease or delayed hormonal response, PTH levels may not fall as expected, making interpretation more complex. [1]
Clinical evidence also indicates that while intraoperative monitoring improves success rates, it does not completely eliminate the possibility of persistent or recurrent disease, especially in complex cases. [10]
Surgeon Experience Variability
Parathyroid surgery is highly dependent on the surgeon’s experience and expertise. Unlike many other procedures, success relies not only on technical skill but also on the ability to identify subtle anatomical variations and make intraoperative judgments.
Experienced endocrine surgeons are more likely to recognize multigland disease, identify ectopic tissue, and adjust their approach during surgery. In contrast, less experienced operators may rely more heavily on preoperative imaging, which can increase the risk of missed pathology. [1]
Guidelines and clinical reviews consistently emphasize that outcomes are significantly better when surgery is performed by specialists with focused experience in parathyroid procedures. [10]
These factors explain why, despite modern tools, surgical planning and execution still have limitations that can influence outcomes.
When Surgery Appears Successful but Disease Returns Silently
In some patients, parathyroid surgery initially appears successful. Calcium levels return to the normal range, symptoms improve, and early follow-up suggests that the condition has been resolved. However, over time, a different pattern can emerge where the disease gradually returns without clear early warning signs.
This silent return is characteristic of recurrent hyperparathyroidism. Clinical data suggest that persistent disease occurs in approximately 2–5% of patients, while recurrent hyperparathyroidism develops in about 5–10% of cases over long-term follow-up, depending on underlying factors such as multigland disease and surgical expertise. [10] These numbers are small but clinically significant, especially considering the expectation of a definitive cure after surgery.
From a physiological perspective, primary hyperparathyroidism affects multiple systems, including bone metabolism, kidney function, and calcium regulation. Even after removal of the primary abnormal gland, these systems may not immediately return to equilibrium, particularly in patients with long-standing disease. This creates a setting where biochemical changes can occur gradually before symptoms become noticeable. [4]
In many cases, recurrence develops slowly. Patients may initially feel better, but subtle symptoms such as fatigue, reduced stamina, mild bone discomfort, or cognitive changes begin to reappear over time. These symptoms are often nonspecific and may be attributed to aging or lifestyle factors rather than recurrence. [8]
Another important clinical observation is that recurrence does not always present with immediate elevation of both calcium and parathyroid hormone levels. In some patients, one parameter may rise before the other, making early detection more challenging. This reinforces the importance of periodic monitoring rather than relying on a single follow-up test.
Because this progression is gradual and often silent in its early phase, recurrence can go unnoticed for months or even years. This is why endocrine guidelines emphasize the need for long-term biochemical monitoring even after apparently successful surgery, especially in patients with risk factors such as multigland disease or borderline preoperative findings. [10]
Recognizing that parathyroid disease can return silently helps set realistic expectations. It also highlights the importance of continued evaluation and awareness, rather than assuming permanent resolution after a single intervention.
Why Reoperative Parathyroid Surgery Is More Complex
Reoperative parathyroid surgery is fundamentally different from the first procedure. Unlike initial surgery, which is performed in a relatively undisturbed anatomical field, repeat surgery takes place in an area that has already been altered by previous intervention. This creates both technical and clinical challenges that require a higher level of precision and experience.
Altered Anatomy and Scar Tissue
After the first surgery, normal tissue planes are disrupted and replaced by fibrosis and scar formation. Structures that were once clearly visible may become difficult to distinguish, and anatomical landmarks can be distorted. This makes surgical dissection more demanding and increases the risk of unintended injury. [1]
Increased Risk to Critical Structures
One of the most important concerns in reoperative surgery is the recurrent laryngeal nerve, which controls vocal cord movement. In a previously operated field, this nerve may be displaced or embedded within scar tissue. As a result, identifying and preserving it becomes more complex, and the risk of nerve injury is higher compared to primary surgery. [1]
Difficulty in Localizing Residual Disease
In patients requiring reoperation, the source of persistent or recurrent disease is often not immediately obvious. The remaining abnormal tissue may be a missed adenoma, a second hyperfunctioning gland, or ectopic tissue located outside the usual surgical field. These situations require more advanced imaging and a careful review of previous surgical findings. [10]
Even with improved imaging techniques, localization in reoperative cases remains less reliable. Changes from the previous surgery can affect imaging clarity, and small or atypically located glands may still be difficult to detect.
Lower Success Rates and Higher Complication Risk
Clinical experience shows that reoperative parathyroid surgery generally has lower success rates compared to first-time procedures. At the same time, the risk of complications is higher due to the altered surgical field and complexity of disease. This does not reflect poor surgical practice, but rather the inherent difficulty of these cases. [1]
More Complex Decision-Making
Not all patients with persistent or recurrent hyperparathyroidism require immediate repeat surgery. The decision depends on multiple factors, including symptom severity, calcium levels, overall health, and risk of complications. In some cases, careful monitoring or alternative approaches may be more appropriate than immediate reintervention. [10]
Need for Specialized Expertise
Because of these complexities, reoperative parathyroid surgery is best managed by surgeons with focused experience in endocrine and parathyroid procedures. A multidisciplinary approach involving endocrinologists, radiologists, and surgeons is often required to reassess the condition and plan the safest and most effective strategy.
Reoperative surgery is therefore not simply a repeat procedure. It is a more advanced and higher-risk intervention that requires careful planning, precise execution, and individualized patient evaluation.
Reality Check: Not Every “Normal” Result Means Full Recovery
After parathyroid surgery, many patients are reassured when laboratory values such as calcium fall within the normal range. While this is an important indicator of surgical success, it does not always reflect complete physiological recovery. A normal lab report does not necessarily mean that the body has fully returned to balance or that all symptoms will resolve.
Clinical studies show that a subset of patients continues to have elevated parathyroid hormone levels even after calcium normalizes. This pattern can persist without immediate recurrence of hypercalcemia, making interpretation more complex. [13] In such cases, relying solely on laboratory values can lead to an incomplete assessment of recovery.
Primary hyperparathyroidism is not limited to a single gland but affects multiple systems in the body, including bone metabolism, kidney function, and overall calcium regulation. Even after removal of the abnormal gland, these systems may take time to stabilize, especially if the condition was present for a long period before surgery. Residual effects on bone density, renal handling of calcium, and metabolic function can continue to influence how a patient feels. [4]
From a clinical care perspective, it is also recognized that symptom resolution does not always occur immediately. Patients may continue to experience fatigue, weakness, or cognitive changes despite normal laboratory findings. This highlights a gap between biochemical success and functional recovery, which is increasingly acknowledged in patient-centered care models. [5]
For this reason, postoperative evaluation should not rely solely on a single set of lab results. A broader assessment that includes symptom progression, long-term trends in calcium and parathyroid hormone levels, and overall metabolic recovery provides a more accurate picture of outcome.
Recognizing this distinction helps prevent false reassurance and encourages a more complete evaluation when recovery does not align with expectations.
The Functional Gap: What Surgery Does Not Address
Parathyroid surgery focuses on removing the overactive gland, and in many cases, it successfully lowers calcium levels. However, the condition itself involves a broader disturbance across multiple systems in the body. This creates a gap between correcting the structural issue and restoring full physiological balance.
System-Wide Effects of Long-Standing Disease
Primary hyperparathyroidism affects more than a single gland. Over time, elevated parathyroid hormone influences bone turnover, kidney function, and intestinal calcium absorption. Bones may lose density due to prolonged calcium release, while the kidneys adapt to handling increased calcium levels. These changes develop gradually and do not reverse immediately after surgery. [4]
As a result, even when the abnormal gland is removed, the body may continue to function in a previously altered state. Recovery of these systems often requires time and may not always be complete, particularly in patients with long-standing disease.
Persistent Metabolic Imbalance After Surgery
The relationship between calcium, parathyroid hormone, vitamin D, and renal function is complex and interdependent. After surgery, these regulatory pathways may continue to behave differently due to prior adaptation. Hormonal feedback mechanisms may take time to stabilize, and in some cases, may remain partially altered. [3]
This explains why patients can experience ongoing symptoms despite normalization of calcium levels. Fatigue, weakness, or subtle cognitive changes may persist because the underlying metabolic systems are still adjusting rather than fully restored.
Gap Between Biochemical Correction and Clinical Recovery
A key limitation of surgery is that it primarily addresses the source of hormone excess, not the downstream effects that have developed over time. Laboratory values may improve, but functional recovery at the level of tissues and organ systems may lag behind.
This gap between biochemical correction and clinical improvement is often overlooked. Patients may be reassured based on normal lab results, while their symptoms suggest incomplete recovery. Recognizing this difference is essential for a more accurate evaluation of outcomes.
Why This Gap Matters in Long-Term Recovery
Acknowledging this functional gap shifts the perspective from viewing the condition as a localized problem to recognizing it as a broader metabolic disturbance. It highlights the need for continued monitoring and a more comprehensive approach to recovery, especially in patients whose symptoms persist after surgery.
This section serves as a transition point, where it becomes clear that removing the gland does not always equate to full restoration of balance, setting the stage for exploring broader approaches to long-term recovery.
If you want a complete understanding of parathyroid disorders, symptoms, diagnosis, and long-term management, it is important to look beyond just surgical outcomes and evaluate the condition as a whole.
Explore here:
https://panaceayur.com/parathyroid-disorders-symptoms-diagnosis-ayurvedic-cure/
An Integrative Perspective on Restoring Calcium Balance
After recognizing that surgical correction does not always restore complete physiological balance, it becomes necessary to consider a broader perspective on recovery. In patients with persistent symptoms, fluctuating laboratory values, or incomplete functional improvement, focusing only on gland removal may not fully address the complexity of the condition.
Table : Surgery vs Functional Recovery
| Aspect | Surgery Focus | Full Recovery Reality |
|---|---|---|
| Target | Remove abnormal gland | Restore systemic balance |
| Outcome | Calcium correction | Whole-body regulation |
| Timeline | Immediate biochemical change | Gradual recovery |
| Symptoms | May persist | Require deeper evaluation |
Why a Broader Approach Becomes Relevant
Primary hyperparathyroidism influences multiple systems, including bone metabolism, kidney function, and calcium regulation pathways. These systems often adapt over time in response to prolonged hormonal imbalance. Even after surgery corrects the primary source of excess hormone, these adaptations may persist and continue to affect how the body regulates calcium. [4]
In such cases, recovery is not limited to normalizing laboratory values but involves gradual restoration of systemic balance. Clinical observations and reviews emphasize that long-term outcomes depend on how effectively the body recalibrates these interconnected systems after surgical intervention. [3]
This is why a broader approach becomes relevant, particularly in patients who do not experience complete recovery despite technically successful surgery.
Looking Beyond the Gland
Focusing only on the parathyroid gland can overlook the wider physiological context in which the disorder develops. Calcium balance is maintained through a coordinated interaction between the skeleton, kidneys, gastrointestinal system, and hormonal feedback mechanisms.
Even after removal of the abnormal gland, these systems may continue to function in an altered state. Bone density recovery, renal calcium handling, and metabolic regulation may take time to stabilize. In some cases, these processes remain partially dysregulated, contributing to ongoing symptoms or delayed recovery. [4]
Looking beyond the gland allows for a more comprehensive view of the condition, where recovery is seen as a systemic process rather than a single corrective event.
Ayurveda Interpretation
From a broader medical perspective, some systems of healthcare interpret such conditions not as isolated organ disorders but as disturbances affecting the body at multiple levels. In this view, long-standing imbalance is considered to influence tissues, metabolic processes, and regulatory mechanisms across the system.
This approach places emphasis on restoring overall balance rather than focusing solely on structural correction. It aligns with the observation that patients may continue to experience symptoms even after successful surgical intervention, highlighting the need to consider recovery beyond a single anatomical focus.
When an Integrative Approach May Be Considered
In clinical practice, not every patient with hyperparathyroidism requires a broader or alternative strategy. However, there are specific situations where a more comprehensive approach becomes relevant, particularly when the expected outcomes of surgery are not fully achieved or when the clinical picture remains unclear.
Persistent or Recurrent Disease After Surgery
An integrative approach may be considered in patients who continue to have elevated calcium levels after surgery or experience recurrence after an initial period of normalization. These scenarios often reflect more complex disease patterns such as multigland involvement, missed adenoma, or underlying factors that were not fully addressed during the initial procedure. Clinical guidelines emphasize the importance of careful reassessment in such cases before proceeding with repeat intervention. [1]
Recent clinical reviews also highlight that persistent and recurrent hyperparathyroidism require a more detailed evaluation, including review of previous findings and consideration of additional contributing factors, rather than immediate repetition of the same treatment strategy. [10]
A deeper evaluation of the condition, including long-term regulation and recovery pathways, can provide more clarity before making further decisions.
Learn more:
https://panaceayur.com/parathyroid-disorders-symptoms-diagnosis-ayurvedic-cure/
Persistent Symptoms Despite Normal Laboratory Results
Some patients continue to experience fatigue, musculoskeletal discomfort, or reduced quality of life even when calcium levels are within the normal range. In these cases, biochemical correction does not fully align with clinical recovery.
This situation reflects the broader systemic impact of the condition, where recovery of bone, kidney, and metabolic function may lag behind laboratory normalization. Recognizing this mismatch can support the need for a more comprehensive approach to recovery rather than focusing solely on numerical values. [5]
Uncertainty in Diagnosis or Disease Pattern
An integrative approach may also be relevant when there is uncertainty in the initial diagnosis or when the clinical presentation does not clearly fit a single pattern. Conditions that mimic primary hyperparathyroidism or variations in disease expression can complicate decision-making.
In such cases, reassessment that includes both biochemical and systemic evaluation can provide a clearer direction for management, especially before considering repeat surgical intervention. [5]
Consideration Before Repeat Surgery
Repeat parathyroid surgery carries increased complexity and risk compared to the initial procedure. For this reason, guidelines recommend careful patient selection and thorough evaluation before proceeding with reoperation. [1]
In patients with mild biochemical abnormalities, stable symptoms, or uncertain localization, a broader approach may be considered as part of a stepwise strategy rather than immediate reintervention. [10]
A Shift Toward Comprehensive Evaluation
These scenarios highlight a shift from a purely procedural approach to a more comprehensive evaluation of the condition. Instead of focusing only on structural correction, attention is given to long-term regulation, symptom patterns, and overall physiological balance.
This approach does not replace surgical management when clearly indicated, but it provides an additional layer of consideration in patients where outcomes are not straightforward or where conventional pathways do not fully explain the clinical picture.
What Patients Often Realize Too Late
In many cases, the full picture of recovery becomes clear only after some time has passed following surgery. Initially, patients are reassured by improvement in laboratory values or by confirmation that the abnormal gland has been removed. However, as weeks or months go by, a different realization often begins to take shape.
Symptoms Do Not Always Disappear Completely
One of the most common realizations is that symptoms do not always resolve as expected. Patients may continue to experience fatigue, reduced energy, or subtle physical discomfort despite normal calcium levels. This can be confusing, especially when follow-up reports suggest that the condition has been successfully treated. [5]
This disconnect between laboratory results and real-world experience highlights that recovery is not always immediate or complete at the functional level.
The Condition Was Not Limited to a Single Gland
Another important realization is that the condition extends beyond the parathyroid gland itself. Primary hyperparathyroidism affects multiple systems, including bones, kidneys, and metabolic regulation. Over time, these systems adapt to prolonged hormonal imbalance, and those changes do not reverse instantly after surgery. [4]
As a result, removing the gland addresses the source of excess hormone production but does not immediately restore the body to its previous equilibrium.
Recovery Is a Process, Not a Single Event
Many patients initially expect surgery to provide a complete and immediate resolution. However, recovery often follows a gradual course. Bone density may take time to improve, metabolic balance may need to stabilize, and symptoms may resolve slowly rather than all at once.
Recognizing this helps shift expectations from a one-time correction to an ongoing recovery process.
Delayed Recognition Can Affect Decision-Making
When these patterns are not recognized early, patients may either ignore persistent symptoms or assume that nothing further can be done. In some cases, this leads to delayed follow-up or incomplete evaluation of ongoing issues.
Acknowledging these realities earlier allows for more informed decisions and encourages a more comprehensive approach to long-term health rather than relying solely on initial surgical outcomes.
Case Study
Clinical patterns become clearer when viewed through real-world scenarios. The following case snapshots reflect commonly reported situations in medical literature and help illustrate why outcomes after parathyroid surgery may not always be straightforward.
Case 1: Ectopic Mediastinal Adenoma
A young adult patient presented with persistent hypercalcemia despite undergoing parathyroid surgery based on neck imaging. Initial evaluation had focused on the typical cervical region, and no additional abnormal glands were identified during surgery. However, symptoms and elevated calcium levels continued after the procedure.
Further investigation using advanced imaging revealed an ectopic parathyroid adenoma located in the mediastinum, outside the usual surgical field. This gland had remained undetected during the initial operation. Once identified, a targeted surgical approach was performed, leading to normalization of calcium levels and improvement in symptoms. [14]
This case highlights how atypical gland locations can contribute to persistent disease and why comprehensive localization is essential before and after surgery.
Case 2: Familial Hypocalciuric Hypercalcemia Misdiagnosed
A middle-aged patient was diagnosed with primary hyperparathyroidism based on elevated calcium and parathyroid hormone levels. Surgery was performed with the expectation of resolving the condition. However, postoperative laboratory values remained largely unchanged, and symptoms persisted.
Subsequent evaluation revealed that the patient had familial hypocalciuric hypercalcemia, a genetic condition that mimics primary hyperparathyroidism but does not benefit from surgical intervention. The key diagnostic clue, low urinary calcium excretion, had not been fully considered before surgery.
This case demonstrates how misclassification of the condition can lead to unnecessary procedures and apparent surgical failure when the underlying issue is different. [15]
Case 3: Persistent High PTH After Surgery
In another scenario, a patient underwent successful removal of a parathyroid adenoma, and calcium levels normalized after surgery. Despite this, follow-up tests showed persistently elevated parathyroid hormone levels.
The patient experienced mild fatigue but no clear signs of recurrent hypercalcemia. Further evaluation suggested that the elevated PTH was related to postoperative metabolic adjustment, possibly influenced by factors such as bone remineralization or vitamin D status, rather than persistent disease.
Clinical studies have shown that this pattern is not uncommon and does not always indicate surgical failure. In many cases, hormone levels stabilize over time without the need for additional intervention. [13] [12]
This case emphasizes the importance of interpreting postoperative results within a broader clinical context rather than relying on a single laboratory parameter.
What Should You Do Next
If recovery after parathyroid surgery does not match expectations, the next step is not immediate reintervention but careful reassessment. A structured approach helps clarify whether the issue is persistent disease, recurrence, postoperative adaptation, or an alternative diagnosis.
Confirm the Current Clinical Status
Start by reviewing recent laboratory results, including calcium and parathyroid hormone levels, along with symptom patterns. Trends over time are more informative than a single test. This helps distinguish between persistent disease, recurrence, and normal postoperative variation. [5]
Re-evaluate the Diagnosis
If findings are inconsistent or unclear, reassessing the original diagnosis is essential. Conditions that can mimic primary hyperparathyroidism should be reconsidered, and appropriate tests such as urine calcium evaluation may be needed. Accurate classification guides the next steps and avoids unnecessary interventions. [5]
Review Previous Surgical and Imaging Details
A detailed review of prior operative notes and imaging studies can identify what was removed and what may have been missed. This is particularly important in cases of persistent or recurrent disease, where missed adenomas, multigland involvement, or ectopic tissue are possible explanations. [10]
Consider Specialist Evaluation Before Repeat Surgery
Repeat surgery carries higher complexity and risk. Clinical guidelines recommend that patients with persistent or recurrent hyperparathyroidism be evaluated by experienced endocrine surgeons before considering reoperation. A specialist assessment helps determine whether surgery is necessary and, if so, how it should be approached. [1]
Take a Broader View of Recovery
In situations where symptoms persist despite normal laboratory values, a broader evaluation of systemic recovery may be appropriate. This includes assessing bone health, kidney function, and overall metabolic balance rather than focusing only on calcium levels. [10]
Avoid Immediate Decisions Without Complete Assessment
It is important not to rush into repeat procedures without a clear understanding of the underlying cause. A stepwise evaluation ensures that decisions are based on a complete clinical picture rather than isolated findings. [1]
Taking these steps provides a more informed and balanced pathway forward, helping ensure that further management is appropriate, safe, and aligned with the patient’s overall condition.
Table : When to Consider Further Evaluation
When to Consider Further Evaluation
| Situation | What It Suggests |
|---|---|
| High calcium after surgery | Persistent disease |
| Symptoms with normal labs | Functional imbalance |
| Rising calcium after months | Recurrence |
| Confusing diagnosis | Misclassification |
FAQs
Can parathyroid surgery fail?
Yes, parathyroid surgery can fail if abnormal glands are missed, multiple glands are involved, or the condition recurs over time.
What is persistent vs recurrent hyperparathyroidism?
Persistent means calcium stays high after surgery. Recurrent means calcium becomes normal but rises again later.
Why is PTH still high after parathyroid surgery?
PTH may remain high due to vitamin D deficiency, bone recovery, or underlying metabolic imbalance.
What are signs that parathyroid surgery did not work?
Signs include persistent fatigue, high calcium levels, kidney stones, bone pain, or continued symptoms despite “normal” reports.
Can hyperparathyroidism come back after surgery?
Yes, recurrence can occur months or years later, especially in multigland disease or incomplete removal cases.
Do all patients need repeat parathyroid surgery?
No, repeat surgery is not always required. Further evaluation is needed to confirm the cause before considering another procedure.
How common is failed parathyroid surgery?
Persistent disease occurs in about 2 to 5 percent of cases, while recurrence may occur in around 5 to 10 percent over time.
Why do symptoms continue even after normal calcium levels?
Symptoms may persist because the condition affects bones, kidneys, and metabolism, which take time to recover.
Is imaging always accurate before parathyroid surgery?
No, imaging can miss small, multiple, or ectopic glands, which may lead to incomplete treatment.
When should I seek further evaluation after surgery?
If symptoms persist, calcium rises again, or recovery feels incomplete, further evaluation is recommended.
Reference
[1] Wilhelm, S. M., Wang, T. S., Ruan, D. T., et al. (2016).
The American Association of Endocrine Surgeons guidelines for definitive management of primary hyperparathyroidism. JAMA Surgery, 151(10), 959–968.
Link: https://pubmed.ncbi.nlm.nih.gov/27532368/
Brief: Core surgical guideline explaining diagnosis, operative strategy, persistent disease, recurrence, and the need for expert evaluation in complex cases.
[3] Bilezikian, J. P., Bandeira, L., Khan, A., & Cusano, N. E. (2022).
Evaluation and management of primary hyperparathyroidism: Summary statement and guidelines from the Fifth International Workshop.
Link: https://www.endocrinology.org/media/boodt50x/bilezikian-et-al-guidelines.pdf
Brief: Comprehensive guideline covering diagnosis, systemic effects, calcium metabolism, and long-term management strategies.
[4] Walker, M. D., & Silverberg, S. J. (2018).
Primary hyperparathyroidism. Nature Reviews Endocrinology, 14(2), 115–125.
Link: https://pubmed.ncbi.nlm.nih.gov/28885621/
Brief: High-quality review explaining how the disease affects bone, kidney, and overall physiology, not just a single gland.
[5] National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). (2026).
Primary hyperparathyroidism.
Link: https://www.niddk.nih.gov/health-information/endocrine-diseases/primary-hyperparathyroidism
Brief: Authoritative patient-friendly source explaining causes, diagnosis, urine calcium testing, and conditions like familial hypocalciuric hypercalcemia.
[7] Johnson, N. A., Tublin, M. E., & Ogilvie, J. B. (2007).
Parathyroid imaging: Technique and role in preoperative evaluation. American Journal of Roentgenology, 188(6), 1706–1715.
Link: https://pubmed.ncbi.nlm.nih.gov/17515397/
Brief: Explains imaging techniques and why scans like ultrasound and sestamibi are helpful but not always accurate.
[8] Uludag, M., Unlu, M. T., Kostek, M., et al. (2023).
Persistent and recurrent primary hyperparathyroidism: Etiological factors and preoperative evaluation.
Link: https://www.researchgate.net/publication/389681370_Persistence_and_recurrence_of_primary_hyperparathyroidism
Brief: Defines persistent vs recurrent disease and explains major causes like missed glands, multigland disease, and ectopic tissue.
[10] Alnajmi, R. A. Y., Ali, D. S., & Khan, A. A. (2025).
Persistence and recurrence of primary hyperparathyroidism. Best Practice & Research Clinical Endocrinology & Metabolism, 39, 101986.
Link: https://www.sciencedirect.com/science/article/pii/S1521690X25000193
Brief: Recent review covering recurrence mechanisms, surgical limitations, and challenges in reoperative cases.
[11] Cartwright, C., & Anastasopoulou, C. (2025).
Hungry bone syndrome. In StatPearls.
Link: https://www.ncbi.nlm.nih.gov/books/NBK549880/
Brief: Explains postoperative calcium shifts where patients may feel worse temporarily due to bone remineralization, not surgical failure.
[12] Denizot, A., Pucini, M., Chagnaud, C., et al. (2001).
Normocalcemia with elevated parathyroid hormone after surgery. The American Journal of Surgery, 182(1), 15–19.
Link: https://pubmed.ncbi.nlm.nih.gov/11532408/
Brief: Shows that elevated PTH after surgery with normal calcium is relatively common and does not always mean failure.
[13] Solorzano, C. C., Mendez, W., Lew, J. I., et al. (2008).
Long-term outcomes in patients with elevated PTH after parathyroidectomy. Archives of Surgery, 143(7), 659–663.
Link: https://pubmed.ncbi.nlm.nih.gov/18645108/
Brief: Demonstrates that some patients maintain high PTH levels post-surgery without immediate recurrence of hypercalcemia.
[14] Hemead, H. M., et al. (2021).
Ectopic mediastinal parathyroid adenoma: Case report.
Link: https://pmc.ncbi.nlm.nih.gov/articles/PMC8666502/
Brief: Real clinical case showing how ectopic glands outside the neck can be missed and cause persistent disease.
[15] Abdullah, A. L. R., et al. (2024).
Familial hypocalciuric hypercalcemia case report.
Link: https://pmc.ncbi.nlm.nih.gov/articles/PMC11070985/
Brief: Demonstrates how misdiagnosis can lead to unnecessary surgery and apparent “failure” when the underlying condition is different.
[16] NHS. (2025).
Hyperparathyroidism.
Link: https://www.nhs.uk/conditions/hyperparathyroidism/
Brief: Trusted UK clinical resource explaining symptoms, treatment pathways, and need for follow-up after treatment.