- Understanding What a Miscarriage Is
- Most Common Medical Causes of Miscarriage
- Rare Medical Causes of Miscarriage
- Chromosomal Abnormalities
- Hormonal Imbalance
- Uterine Abnormalities
- Immune and Clotting Disorders
- Hidden Causes Doctors Often Miss
- Viral or Infectious Triggers
- Poor Egg Quality and Maternal Age
- Poor Sperm DNA Integrity
- Lifestyle and Environmental Factors
- Ayurvedic Understanding of Recurrent Miscarriage
- How Miscarriage Risk Can Be Reduced
- When to Seek Medical Evaluation
- Can Recurrent Miscarriage Be Treated?
- Ayurvedic Fertility Restoration Approach
- Frequently Asked Questions
- Reference
Understanding What a Miscarriage Is
Understanding Reasons For Miscarriage is the first step toward recognizing why pregnancy loss occurs and how it can be prevented or managed. In medical terms, miscarriage refers to the spontaneous loss of a pregnancy before the fetus reaches viability, which is typically defined as before 20 weeks of gestation in most clinical guidelines. Early pregnancy loss is unfortunately common, and many cases occur before a woman even realizes she is pregnant [1].
Many couples experiencing pregnancy loss also struggle with underlying fertility issues. A deeper explanation of fertility causes and treatment approaches is explained in our detailed guide on infertility causes, diagnosis and treatment.
Medical Definition of Miscarriage
According to modern obstetric guidelines, miscarriage is defined as the loss of a clinically recognized pregnancy during the first half of gestation. Most miscarriages occur during the first trimester, particularly before 12 weeks of pregnancy. This period represents a critical phase in fetal development when genetic stability, hormonal balance, and uterine conditions must all work in harmony to sustain pregnancy [1].
Clinical studies indicate that approximately 10 to 20 percent of recognized pregnancies end in miscarriage. The actual number may be higher because very early pregnancy losses often occur before pregnancy testing or medical confirmation [2].
From a clinical perspective, miscarriage is categorized into several types, including threatened miscarriage, inevitable miscarriage, incomplete miscarriage, complete miscarriage, and missed miscarriage. Each category reflects different stages of pregnancy loss and requires different medical evaluation and care [1].
Table: Miscarriage Risk by Maternal Age
| Maternal Age | Estimated Miscarriage Risk |
|---|---|
| Under 30 | Lower risk |
| 30–34 | Moderate risk |
| 35–39 | Increased risk |
| 40+ | Significantly higher risk |
Why Miscarriages Occur
Pregnancy is a complex biological process that depends on precise coordination between genetic material from both parents, proper implantation of the embryo, adequate hormonal support, and a healthy uterine environment. When any of these factors becomes disrupted, pregnancy may not continue normally.
Medical research shows that chromosomal abnormalities in the developing embryo are the most common cause of early miscarriage. In many cases, the embryo contains missing or extra chromosomes that prevent normal development, leading the body to naturally terminate the pregnancy [3].
However, genetic factors are not the only cause. Structural problems in the uterus, hormonal disorders, autoimmune conditions, infections, and lifestyle factors may also contribute to pregnancy loss in some patients [2].
When Miscarriage Becomes a Medical Concern
A single miscarriage does not necessarily indicate a long-term fertility problem. Many women who experience pregnancy loss go on to have healthy pregnancies later.
However, when miscarriage occurs repeatedly, it may indicate an underlying medical condition. Recurrent pregnancy loss is generally defined as two or more consecutive miscarriages, and in such cases doctors typically recommend further medical evaluation to identify potential causes [2].
Specialized testing may include genetic screening, uterine imaging, hormone evaluation, and immune system assessments. Identifying the underlying cause is essential because some conditions contributing to recurrent miscarriage can be treated or managed with appropriate medical care [3].
The Emotional and Clinical Importance of Understanding Miscarriage
For many couples, miscarriage is not only a medical event but also an emotionally difficult experience. Understanding the biological reasons behind pregnancy loss can help reduce confusion, guilt, and fear that often accompany miscarriage.
Medical science now recognizes that miscarriage is usually not caused by anything the mother did wrong. Instead, it is often the result of biological factors that occur beyond human control. This understanding helps patients approach pregnancy planning and medical care with greater clarity and confidence [1].
For patients who experience repeated pregnancy loss, early medical evaluation and personalized treatment planning can significantly improve the chances of a successful pregnancy in the future [2].
Most Common Medical Causes of Miscarriage

Understanding the most common medical causes of miscarriage helps patients and clinicians identify why pregnancy loss occurs and what evaluations may be necessary. Pregnancy depends on a delicate biological balance involving genetic stability, uterine structure, hormonal regulation, immune tolerance, and maternal health. When one or more of these systems becomes disrupted, miscarriage may occur [1] [2] [3].
Many of these factors are closely connected with broader fertility disorders. A full explanation of these mechanisms is discussed in our guide on infertility causes and treatment.
Chromosomal Abnormalities in the Embryo
Chromosomal abnormalities are the leading cause of miscarriage, especially during the first trimester. When an embryo forms, it should receive 23 chromosomes from the mother and 23 from the father. If an error occurs during cell division, the embryo may have an abnormal number of chromosomes, known as aneuploidy.
Examples include trisomy, monosomy, and polyploidy. These genetic errors often prevent the embryo from developing normally, which leads to spontaneous pregnancy loss. Clinical research indicates that chromosomal abnormalities may account for more than half of early miscarriages [1] [3].
Most of these genetic abnormalities occur randomly and do not necessarily mean that the parents have a fertility disorder. However, in cases of recurrent miscarriage, genetic testing of the parents may sometimes reveal structural chromosomal rearrangements that increase the risk of abnormal embryos [2] [3].
Advanced Maternal Age
Maternal age is one of the strongest biological risk factors for miscarriage. As women age, the quality of the eggs gradually declines. During egg maturation, the mechanisms responsible for separating chromosomes become less reliable.
This increases the likelihood that the embryo will develop with chromosomal abnormalities. As a result, miscarriage rates rise progressively after the mid-thirties and increase significantly after age forty [1] [2].
Uterine Structural Abnormalities
The uterus must provide a supportive environment for implantation and fetal development. Structural abnormalities of the uterus may interfere with implantation, blood supply, or placental development.
Congenital uterine anomalies such as septate uterus, bicornuate uterus, or other Mullerian malformations are known to increase miscarriage risk. These abnormalities occur during fetal development and may remain undiagnosed until fertility investigations are performed [2] [4].
Acquired uterine conditions can also contribute to miscarriage. These include submucosal fibroids, intrauterine adhesions, or distortion of the uterine cavity. When the uterine environment becomes abnormal, the embryo may struggle to implant properly or may fail to receive adequate blood supply during early development [2] [3].
Hormonal and Endocrine Disorders
Hormonal stability is essential during early pregnancy because hormones regulate implantation, placental development, and fetal growth.
Thyroid disorders are one of the most well-recognized endocrine causes of miscarriage. Both hypothyroidism and hyperthyroidism can disrupt the hormonal environment required to sustain pregnancy. Thyroid autoimmunity has also been associated with recurrent pregnancy loss in some patients [2] [3] [5].
Poorly controlled diabetes is another endocrine disorder that may increase miscarriage risk. Elevated blood glucose levels can interfere with embryonic development and early placental function [2] [3].
Polycystic ovarian syndrome may also contribute to miscarriage in some patients due to hormonal imbalance, insulin resistance, and metabolic disturbances that affect reproductive physiology [2] [3].
Immune Disorders and Antiphospholipid Syndrome
Certain immune disorders can interfere with normal placental development. One of the most important and treatable causes of recurrent miscarriage is antiphospholipid syndrome.
This autoimmune condition leads to the production of antibodies that increase the tendency for abnormal blood clotting. In pregnancy, this can impair blood flow to the placenta and disrupt oxygen and nutrient delivery to the developing fetus [6].
Because antiphospholipid syndrome is treatable, it is an essential condition to identify in women with recurrent pregnancy loss.
Male Factors and Sperm DNA Integrity
Miscarriage is often viewed as a female reproductive issue, but male factors can also contribute. While routine semen analysis evaluates sperm count, movement, and morphology, it does not always assess the genetic integrity of sperm.
Some studies suggest that sperm DNA fragmentation or chromosomal abnormalities in sperm may increase the risk of miscarriage, particularly in cases of recurrent pregnancy loss [2] [3].
Table: Most Common Causes of Miscarriage
| Cause | How It Affects Pregnancy | Typical Stage of Loss |
|---|---|---|
| Chromosomal abnormalities | Embryo develops with missing or extra chromosomes | Early first trimester |
| Hormonal imbalance | Insufficient hormonal support for implantation | Early pregnancy |
| Uterine abnormalities | Abnormal uterine structure interferes with implantation | First or second trimester |
| Immune disorders | Autoimmune reactions affect placental blood flow | Early pregnancy |
| Infections | Inflammation damages placental or fetal tissues | Variable |
Rare Medical Causes of Miscarriage
Although less common, several rare medical conditions may contribute to miscarriage. These causes often become relevant when pregnancy loss occurs repeatedly or when standard evaluations fail to identify a clear explanation.
Parental Chromosomal Rearrangements
In a small percentage of couples with recurrent miscarriage, one partner may carry a balanced chromosomal translocation. In this condition, genetic material is rearranged but remains balanced in the parent.
While the carrier remains healthy, the rearranged chromosomes can lead to embryos with unbalanced genetic material, increasing the likelihood of miscarriage [2] [3].
Cervical Insufficiency
Cervical insufficiency occurs when the cervix weakens and opens prematurely during pregnancy. This condition typically causes pregnancy loss during the second trimester rather than the early weeks.
Although it is not a common cause of miscarriage, it is important to recognize because it can often be treated through medical interventions such as cervical cerclage [2].
Chronic Maternal Medical Conditions
Certain chronic illnesses in the mother can increase miscarriage risk. Severe autoimmune disorders, inflammatory diseases, and metabolic disorders may disrupt the biological environment required to maintain pregnancy.
These systemic conditions are uncommon causes of miscarriage but should be considered in patients with complex medical histories [2] [3].
Inherited Clotting Disorders
Inherited thrombophilias have been investigated as potential contributors to miscarriage. Some clotting disorders may affect placental blood flow, although the evidence linking them directly to recurrent pregnancy loss is less consistent than for antiphospholipid syndrome [2] [3].
Because of this uncertainty, testing for inherited thrombophilia is usually recommended only in selected clinical situations.
Unexplained Recurrent Miscarriage
Despite advances in reproductive medicine, many miscarriages remain unexplained. Even after genetic testing, uterine imaging, hormonal evaluation, and immune screening, no specific cause may be identified.
This can be frustrating for patients, but it does not mean that future pregnancy is impossible. Many couples with unexplained recurrent miscarriage eventually achieve a successful pregnancy with appropriate medical care and monitoring [2] [3].
Understanding both the common and rare medical causes of miscarriage allows clinicians to design targeted evaluations and treatment strategies. Identifying the underlying factors affecting pregnancy can significantly improve the chances of maintaining a healthy pregnancy in the future [1] [2].
Chromosomal Abnormalities

Chromosomal abnormalities are widely recognized as the most common cause of miscarriage, particularly during the early stages of pregnancy. During fertilization, the embryo receives half of its genetic material from the mother and half from the father. When this genetic process occurs normally, the embryo develops with 46 chromosomes arranged in 23 pairs. However, errors can occur during the division of reproductive cells, resulting in an abnormal number or structure of chromosomes. These genetic abnormalities often prevent the embryo from developing normally and may lead to pregnancy loss [1] [3].
How Chromosomal Errors Occur
Chromosomal abnormalities usually arise during the formation of the egg or sperm through a process called meiosis. During this process, chromosomes must divide evenly so that each reproductive cell receives the correct genetic information. If this separation fails, the resulting embryo may have missing chromosomes, extra chromosomes, or structural rearrangements.
Common chromosomal abnormalities associated with miscarriage include trisomy, monosomy, and polyploidy. Trisomy occurs when an embryo has three copies of a chromosome instead of two, while monosomy occurs when one chromosome is missing. Polyploidy refers to the presence of extra sets of chromosomes. These abnormalities disrupt normal embryonic development and frequently result in early pregnancy loss [1].
Medical research indicates that chromosomal abnormalities account for a large proportion of miscarriages during the first trimester. Many of these abnormalities arise spontaneously and are not inherited from either parent. Because of this, a single miscarriage caused by chromosomal error does not necessarily indicate an underlying fertility problem [3].
The Role of Maternal Age
Maternal age plays a significant role in the risk of chromosomal abnormalities. As women age, the quality of the eggs gradually declines. The mechanisms responsible for accurately separating chromosomes during egg development become less efficient, increasing the likelihood of genetic errors.
For this reason, miscarriage risk increases with advancing maternal age. Women over the age of thirty five have a higher probability of conceiving embryos with chromosomal abnormalities compared with younger women. The risk continues to increase further after the age of forty [11].
Parental Chromosomal Rearrangements
In a small percentage of couples experiencing recurrent miscarriage, one partner may carry a structural chromosomal rearrangement known as a balanced translocation. In this condition, segments of chromosomes exchange positions without causing health problems in the parent. However, during fertilization these rearrangements may produce embryos with missing or extra genetic material.
Such embryos often fail to develop normally, leading to repeated pregnancy loss. For this reason, genetic testing of both partners may be recommended when miscarriage occurs repeatedly [3].
Why Chromosomal Abnormalities Lead to Miscarriage
The developing embryo depends on precise genetic instructions to guide cell division, organ formation, and placental development. When these instructions are disrupted by chromosomal imbalance, the embryo may be unable to develop normally.
In many cases the body naturally ends the pregnancy when severe chromosomal abnormalities are present. This biological process is often described as a protective mechanism that prevents the continuation of a nonviable pregnancy [1].
Hormonal Imbalance

Hormonal regulation plays a central role in sustaining pregnancy during its earliest stages. After fertilization occurs, a complex sequence of hormonal signals prepares the uterus for implantation, supports placental development, and maintains the physiological environment required for fetal growth. When these hormonal signals become disrupted, the pregnancy may not continue normally, and miscarriage can occur [2] [3].
The Role of Progesterone in Early Pregnancy
One of the most important hormones during early pregnancy is progesterone. This hormone is produced initially by the corpus luteum in the ovary and later by the developing placenta. Progesterone prepares the uterine lining, known as the endometrium, to allow implantation of the embryo and helps maintain the uterine environment throughout the first trimester.
If progesterone production is insufficient, the uterine lining may not provide adequate support for the developing embryo. Some clinicians refer to this condition as luteal phase insufficiency. Although the concept remains debated in reproductive medicine, inadequate progesterone support may contribute to pregnancy loss in certain patients with recurrent miscarriage [2] [3].
Thyroid Disorders and Pregnancy Loss
The thyroid gland regulates metabolism and influences many reproductive hormones. Thyroid dysfunction can disturb the hormonal environment necessary for pregnancy maintenance.
Both hypothyroidism and hyperthyroidism have been associated with an increased risk of miscarriage. In particular, autoimmune thyroid disease and elevated thyroid-stimulating hormone levels may interfere with implantation and early placental development. Because thyroid disorders are relatively common and treatable, screening for thyroid abnormalities is often recommended in women with recurrent pregnancy loss [2] [3] [5].
Diabetes and Metabolic Hormonal Disorders
Another endocrine condition associated with miscarriage is diabetes mellitus. When blood glucose levels are poorly controlled, the metabolic environment in early pregnancy may become unfavorable for embryonic development.
Elevated glucose levels can interfere with normal cellular growth and placental formation. For this reason, women with diabetes are often advised to achieve optimal glycemic control before conception to reduce the risk of pregnancy complications [2] [3].
Polycystic Ovarian Syndrome
Polycystic ovarian syndrome is one of the most common endocrine disorders affecting reproductive-age women. This condition involves hormonal imbalance, insulin resistance, and irregular ovulation.
Although not every woman with polycystic ovarian syndrome experiences miscarriage, the disorder may increase risk in some patients through metabolic disturbances, obesity, and altered hormonal signaling. These factors may affect implantation and early placental development [2] [3].
Hormonal Balance and Pregnancy Stability
Pregnancy requires precise coordination between ovarian hormones, thyroid hormones, metabolic regulation, and placental signaling. Even small disturbances in this hormonal network may influence the stability of early pregnancy.
For women who experience repeated pregnancy loss, evaluation of endocrine function may include thyroid testing, glucose assessment, and other hormonal investigations. Identifying and treating hormonal disorders can sometimes improve the chances of maintaining a healthy pregnancy [2] [3] [5].
Uterine Abnormalities
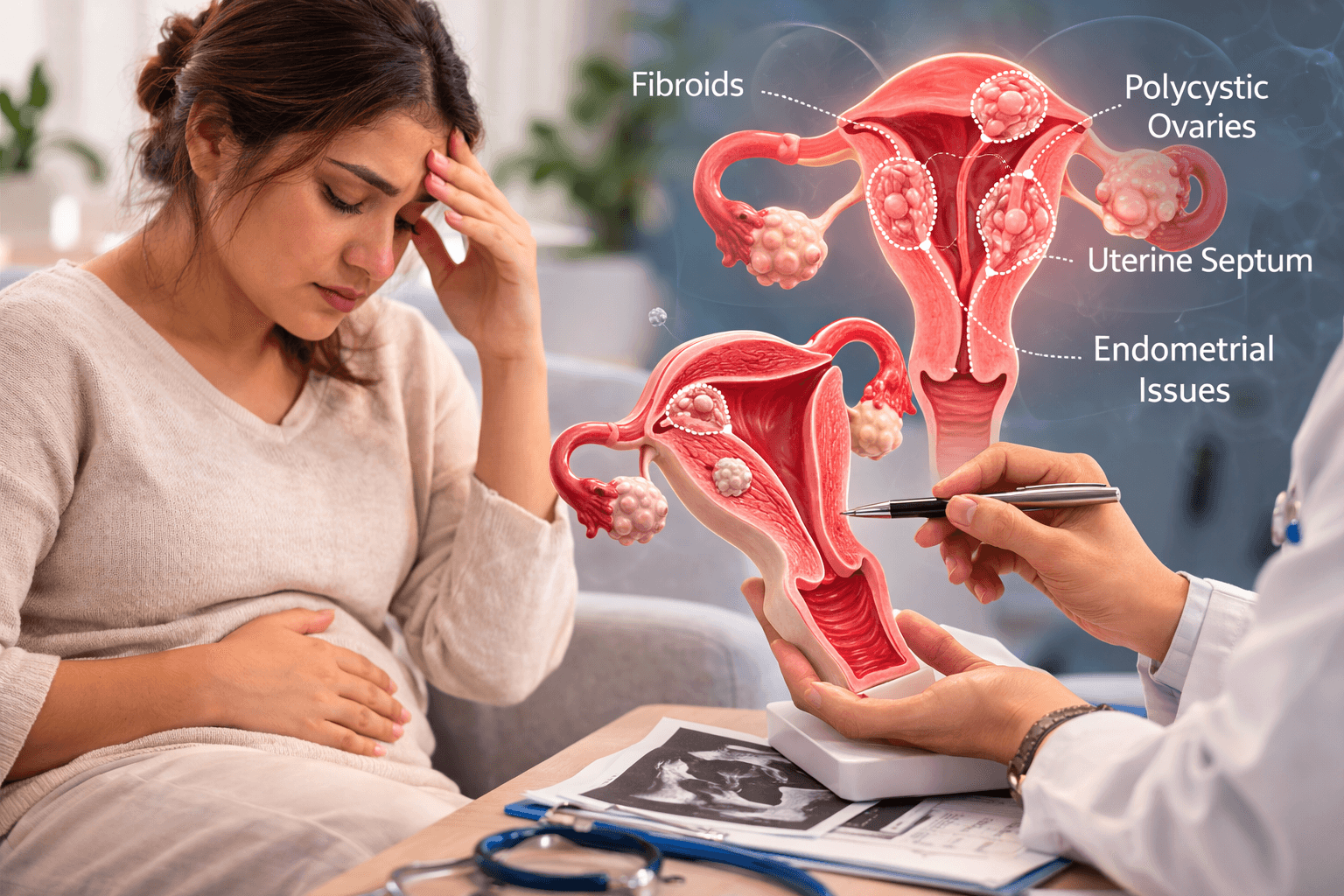
The uterus plays a critical role in supporting implantation, placental development, and the growth of the fetus throughout pregnancy. For a pregnancy to progress normally, the uterine cavity must provide adequate space, blood supply, and structural stability for the developing embryo. When abnormalities affect the structure or function of the uterus, implantation may become difficult or the pregnancy may fail to develop normally, increasing the risk of miscarriage [2] [4].
Uterine abnormalities can be broadly divided into congenital conditions, which are present from birth, and acquired conditions, which develop later in life due to disease, injury, or surgical procedures.
Congenital Uterine Anomalies
Congenital uterine anomalies arise during fetal development when the Mullerian ducts, which form the female reproductive organs, do not fuse or develop normally. These structural variations may remain undetected for many years and may only be discovered during fertility evaluation or after recurrent pregnancy loss.
One of the most common congenital abnormalities associated with miscarriage is the septate uterus. In this condition, a fibrous or muscular partition divides the uterine cavity. Because the septum often has poor blood supply, embryos that implant on this tissue may fail to receive adequate nutrients and oxygen, leading to pregnancy loss [2] [4].
Other congenital anomalies include the bicornuate uterus, in which the uterus has a heart-shaped appearance due to incomplete fusion of the Mullerian ducts, and the uterus didelphys, where two separate uterine cavities develop. While some women with these conditions can carry pregnancies successfully, others may experience increased miscarriage risk depending on the severity of the anomaly [4].
Acquired Uterine Conditions
In addition to congenital anomalies, several conditions acquired later in life may affect the uterine cavity and contribute to miscarriage.
Uterine fibroids, particularly those located within the uterine cavity or directly beneath the endometrial lining, can interfere with implantation and disrupt the blood supply to the developing placenta. Submucosal fibroids are especially associated with reproductive complications [2].
Another condition is intrauterine adhesions, sometimes referred to as Asherman syndrome. These adhesions may form after uterine surgery, infections, or repeated uterine procedures. Scar tissue within the uterus can distort the uterine cavity and interfere with normal implantation and fetal development [2].
Large endometrial polyps may also contribute to implantation failure or early pregnancy loss in some patients.
How Uterine Abnormalities Affect Pregnancy
Successful pregnancy depends on proper implantation of the embryo into a healthy uterine lining with adequate blood supply. Structural abnormalities can disrupt this process in several ways. They may alter the shape of the uterine cavity, reduce the surface area available for implantation, or interfere with the development of the placenta.
When implantation occurs in an area with poor blood supply or structural support, the embryo may not receive sufficient oxygen and nutrients, leading to pregnancy loss [4].
Diagnosis of Uterine Abnormalities
Many uterine abnormalities can be diagnosed through imaging techniques such as pelvic ultrasound, hysterosalpingography, magnetic resonance imaging, or hysteroscopy. These diagnostic tools allow physicians to visualize the uterine cavity and identify structural changes that may contribute to miscarriage.
In women who experience recurrent pregnancy loss, evaluation of the uterine structure is an important part of fertility assessment because certain abnormalities can be corrected through surgical or medical treatment, improving the chances of a successful pregnancy [2].
Immune and Clotting Disorders

The immune system plays a crucial role during pregnancy. Under normal circumstances, the maternal immune system must recognize the developing embryo as compatible with the body while still maintaining its ability to protect against infections. Pregnancy therefore requires a delicate balance between immune tolerance and immune defense. When this balance becomes disturbed, certain immune or blood clotting disorders may interfere with placental development and increase the risk of miscarriage [2] [3].
Among the various immune-related conditions studied in reproductive medicine, the most clearly established cause of recurrent pregnancy loss is antiphospholipid syndrome, an autoimmune disorder that affects the body’s blood clotting mechanisms.
Antiphospholipid Syndrome
Antiphospholipid syndrome occurs when the immune system produces antibodies that mistakenly target proteins associated with cell membranes and blood vessels. These antibodies can increase the tendency for abnormal blood clot formation.
During pregnancy, normal placental development requires a stable blood supply between the mother and the developing fetus. In women with antiphospholipid syndrome, abnormal clotting may develop within the placental blood vessels. This process can impair oxygen and nutrient delivery to the embryo, which may lead to miscarriage or other serious pregnancy complications [6].
Clinical guidelines recognize antiphospholipid syndrome as one of the most important treatable causes of recurrent pregnancy loss. Diagnosis typically involves blood tests that detect antiphospholipid antibodies, combined with a history of pregnancy loss or thrombosis [2] [3].
When identified early, treatment strategies such as low-dose aspirin and anticoagulant therapy may significantly improve pregnancy outcomes in affected women.
Immune System Dysregulation
Beyond antiphospholipid syndrome, researchers have investigated several other immune-related mechanisms that may contribute to miscarriage. These include abnormalities in immune tolerance, inflammatory responses, and interactions between maternal immune cells and placental tissue.
During normal pregnancy, the maternal immune system adapts to allow the fetus, which contains genetic material from both parents, to develop without triggering immune rejection. Specialized immune cells within the uterus help regulate this process and support placental growth.
If immune tolerance mechanisms become disrupted, inflammatory reactions may interfere with implantation or early placental development. Although many aspects of immune-related miscarriage remain under investigation, immune system dysregulation is increasingly recognized as an important area of reproductive research [2] [3].
Inherited and Acquired Clotting Disorders
In addition to autoimmune conditions, certain clotting disorders have been studied as potential contributors to miscarriage. These conditions affect the body’s ability to regulate blood coagulation.
Inherited thrombophilias, which are genetic conditions that increase the risk of abnormal blood clotting, have been examined in relation to pregnancy loss. However, clinical guidelines emphasize that the evidence linking many inherited clotting disorders directly to recurrent miscarriage remains inconsistent.
Because of this uncertainty, testing for inherited thrombophilia is usually recommended only in selected cases where additional clinical risk factors are present [2] [3].
Importance of Diagnosis and Treatment
Identifying immune or clotting disorders is particularly important in patients with recurrent miscarriage because some of these conditions are treatable. With appropriate diagnosis and targeted medical management, the chances of maintaining a successful pregnancy may improve significantly.
In many cases, miscarriage is explained by well-recognized medical causes such as chromosomal abnormalities, uterine structural problems, or hormonal disorders. However, some pregnancy losses occur even when routine testing appears normal. In these situations, underlying factors may remain undetected unless more detailed evaluation is performed. Modern reproductive medicine recognizes that several hidden causes of miscarriage may contribute to pregnancy loss, particularly in couples experiencing recurrent miscarriage [2] [3].
These factors may involve subtle infections, sperm genetic damage, inflammatory conditions of the reproductive tract, or disturbances in the biological environment required for implantation and placental development. Although these causes are less obvious than major chromosomal or anatomical abnormalities, they may still influence pregnancy stability [7].
Chronic or Silent Reproductive Tract Infections
Certain infections within the reproductive tract may remain asymptomatic yet still interfere with implantation or early placental development. Inflammatory changes within the uterus or fallopian tubes can disrupt the delicate interaction between the embryo and the uterine lining.
Studies have examined the role of infections such as Chlamydia trachomatis in pregnancy loss. Chronic infection may produce inflammatory responses within the reproductive system that affect implantation and early embryonic development [10].
Public health guidelines also emphasize the importance of screening for sexually transmitted infections during pregnancy because untreated infections can affect maternal and fetal health. Early detection and treatment may reduce the risk of complications during pregnancy [8].
Subtle Inflammation of the Uterine Lining
Another hidden factor sometimes discussed in reproductive medicine is chronic endometrial inflammation. In this condition, low-grade inflammation within the uterine lining may affect the ability of the embryo to implant or develop normally.
Because symptoms may be mild or absent, this condition can remain undiagnosed during routine evaluation. Some fertility specialists investigate inflammatory markers or perform endometrial biopsy when repeated pregnancy loss occurs without a clear explanation [7].
Sperm DNA Damage
Male reproductive factors may also contribute to miscarriage risk. While standard semen analysis evaluates sperm count, motility, and morphology, it does not always assess the genetic integrity of sperm cells.
Research has shown that sperm DNA fragmentation may affect embryo development and increase the likelihood of early pregnancy loss in some couples. Damage to sperm DNA may occur due to oxidative stress, environmental exposures, or lifestyle factors. When sperm carrying damaged DNA fertilize an egg, embryonic development may be compromised [9].
For couples with recurrent miscarriage, some clinicians recommend additional tests that assess sperm DNA integrity in order to identify potential male-factor contributions.
Subclinical Immune and Inflammatory Conditions
In addition to infections, subtle immune or inflammatory disturbances within the uterus may influence implantation. Pregnancy requires complex communication between maternal immune cells and the developing placenta. When this communication becomes dysregulated, inflammatory responses may interfere with placental formation and embryo development.
Although many aspects of these immune mechanisms remain under investigation, reproductive specialists increasingly recognize that subtle inflammatory conditions may play a role in unexplained pregnancy loss [2] [3].
Why These Causes Are Often Missed
Hidden causes of miscarriage are often overlooked because they may not appear during standard fertility testing. Many routine evaluations focus primarily on hormonal levels, uterine structure, and chromosomal factors.
However, infections, inflammatory processes, and sperm DNA abnormalities may require specialized testing that is not always included in the initial diagnostic workup. As reproductive medicine continues to evolve, physicians are becoming more aware of these subtle contributors to pregnancy loss [7].
Importance of Comprehensive Evaluation
For couples who experience recurrent miscarriage or unexplained pregnancy loss, a comprehensive evaluation may help identify hidden factors affecting reproductive health. This evaluation may include screening for infections, advanced sperm analysis, immune assessments, and detailed reproductive tract evaluation.
Identifying these hidden causes can sometimes provide valuable insight into why miscarriage occurred and may guide more targeted treatment strategies aimed at improving the chances of a successful pregnancy in the future [2] [3].

Infections represent an important but often overlooked factor in miscarriage. While chromosomal abnormalities remain the leading cause of pregnancy loss, several viral or infectious triggers of miscarriage can disrupt implantation, placental development, or fetal growth. These infections may affect pregnancy by causing inflammation of reproductive tissues, damaging placental cells, or disturbing the immune tolerance required for maintaining pregnancy [7].
Some infections produce clear symptoms such as fever, rash, or genital lesions. However, many infections remain silent, meaning a woman may not realize she has been exposed. Because of this, infectious causes of miscarriage may sometimes be missed unless physicians perform targeted testing [8].
Herpes Family Viruses and Pregnancy
Several viruses belonging to the herpes virus family have been studied in relation to pregnancy complications. These viruses are extremely common worldwide and remain in the body in a latent state after initial infection.
One example is cytomegalovirus (CMV), which is part of the herpesvirus family. CMV infection during pregnancy can affect the placenta and developing fetus. When a primary infection occurs during early pregnancy, it may lead to miscarriage, fetal growth problems, or congenital infection in the newborn [7].
Another virus in the herpes family is Epstein–Barr virus (EBV). Although EBV is best known for causing infectious mononucleosis, research has explored whether immune responses triggered by EBV may influence pregnancy outcomes in certain situations. However, the relationship between EBV and miscarriage remains complex and continues to be studied.
Herpes simplex virus (HSV), which causes oral or genital herpes, has also been investigated in pregnancy research. Most women with HSV infections have normal pregnancies, but active infection or systemic viral activity during early pregnancy may contribute to inflammation and immune responses that affect pregnancy stability in rare cases.
Because herpes family viruses remain dormant in the body and can reactivate during times of immune stress, they have attracted increasing attention in reproductive medicine as potential contributors to unexplained pregnancy complications [7].
Rubella Virus and Pregnancy Loss
Rubella, also known as German measles, is one of the most well-established viral causes of pregnancy complications. Infection with the rubella virus during early pregnancy can interfere with fetal development and may lead to miscarriage, stillbirth, or severe congenital abnormalities.
The virus can cross the placenta and infect the developing fetus. Because the fetus has an immature immune system, viral infection may disrupt organ formation and normal development. For this reason, vaccination against rubella before pregnancy is considered an essential preventive measure in reproductive health [8].
Other Viral Infections Affecting Pregnancy
Several other viral infections have also been investigated for their potential role in miscarriage or pregnancy complications. These include viruses that cause systemic illness or significant immune activation in the mother.
Examples include:
- Parvovirus B19, which can infect fetal red blood cells and cause fetal anemia.
- Varicella-zoster virus, the virus responsible for chickenpox.
- Influenza and other systemic viral infections, which may produce high fever and systemic inflammation.
These infections do not always lead to miscarriage, but when they occur during critical stages of pregnancy, they may increase the risk of pregnancy complications.
Bacterial Infections and Reproductive Tract Inflammation
In addition to viral infections, certain bacterial infections may contribute to pregnancy loss. Chronic infections of the reproductive tract can produce inflammation that interferes with implantation or placental development.
One example studied in medical research is Chlamydia trachomatis, a common sexually transmitted bacterium. Chronic infection may damage reproductive tissues and has been associated with miscarriage and infertility in some cases [10].
Because many sexually transmitted infections produce mild or no symptoms, screening is recommended for women planning pregnancy or experiencing pregnancy complications [8].
Why Infection-Related Miscarriages Are Often Missed
Infectious causes of miscarriage are frequently overlooked because many infections remain silent or produce nonspecific symptoms. Routine fertility evaluations may focus on hormones, genetics, and uterine structure, while subtle infections may not be investigated unless there is clinical suspicion.
Modern reproductive medicine increasingly recognizes that infections can influence the uterine environment, immune responses, and placental development. For this reason, targeted screening may be considered when recurrent miscarriage occurs without an obvious cause [7].
Table: Viral and Infectious Causes of Miscarriage
| Infection | Type | How It May Affect Pregnancy |
|---|---|---|
| Rubella virus | Viral | Can cross placenta and disrupt fetal development |
| Cytomegalovirus (CMV) | Herpes virus family | May cause congenital infection and pregnancy complications |
| Herpes simplex virus (HSV) | Herpes virus family | Rarely linked to early pregnancy complications |
| Epstein–Barr virus (EBV) | Herpes virus family | May trigger immune responses affecting pregnancy |
| Chlamydia trachomatis | Bacterial | Chronic reproductive tract inflammation affecting implantation |
Poor Egg Quality and Maternal Age

Among the biological factors influencing pregnancy success, poor egg quality and maternal age play a significant role in miscarriage risk. The quality of the oocyte determines whether the embryo will receive stable genetic material and develop normally during early pregnancy. When egg quality declines, the likelihood of chromosomal abnormalities increases, which can result in pregnancy loss [1] [3].
How Egg Quality Influences Pregnancy
Every woman is born with a finite number of eggs stored in the ovaries. Over time, both the number and the biological quality of these eggs gradually decline. Egg quality refers to the ability of the oocyte to undergo normal fertilization, proper chromosomal division, and healthy embryo development.
When eggs age, the cellular mechanisms responsible for separating chromosomes during cell division may function less accurately. This increases the chance that an embryo will form with missing or extra chromosomes. Embryos with significant chromosomal abnormalities often fail to develop normally and may lead to early miscarriage [1].
Egg quality therefore directly affects embryo viability, implantation success, and pregnancy stability.
Maternal Age and Miscarriage Risk
Maternal age is one of the strongest predictors of miscarriage risk. As women age, particularly after their mid-thirties, the probability of chromosomal abnormalities in eggs increases. This is primarily due to age-related changes in the ovarian environment and the cellular machinery responsible for chromosome segregation.
Clinical observations show that miscarriage risk increases gradually with age. Younger women generally have lower miscarriage rates, while the risk rises significantly after the age of thirty five and continues to increase after forty. This age-related risk is largely driven by declining egg quality and increased chromosomal errors during fertilization [1] [11].
Diminished Ovarian Reserve
In addition to chronological age, some women may experience diminished ovarian reserve, meaning the number and functional quality of eggs in the ovaries decline earlier than expected. This condition may occur due to genetic factors, autoimmune conditions, ovarian surgery, chemotherapy exposure, or other medical influences.
Diminished ovarian reserve does not always prevent pregnancy, but it may increase the likelihood of chromosomal abnormalities and miscarriage because fewer healthy eggs remain available for fertilization [3].
Impact on Embryo Development
Healthy embryo development requires precise coordination of genetic signals that guide cell division and organ formation. When an embryo originates from an egg with compromised genetic integrity, the resulting developmental errors may prevent proper implantation or early fetal growth.
In many cases the body naturally ends the pregnancy when severe chromosomal abnormalities are present. Although emotionally difficult, this process represents a biological mechanism intended to prevent the continuation of a nonviable pregnancy [1].
Importance of Early Evaluation
Because maternal age and egg quality significantly influence pregnancy outcomes, clinicians often consider these factors when evaluating recurrent miscarriage. Fertility specialists may assess ovarian reserve using hormone testing and ultrasound evaluation to estimate the reproductive potential of the ovaries.
Poor Sperm DNA Integrity
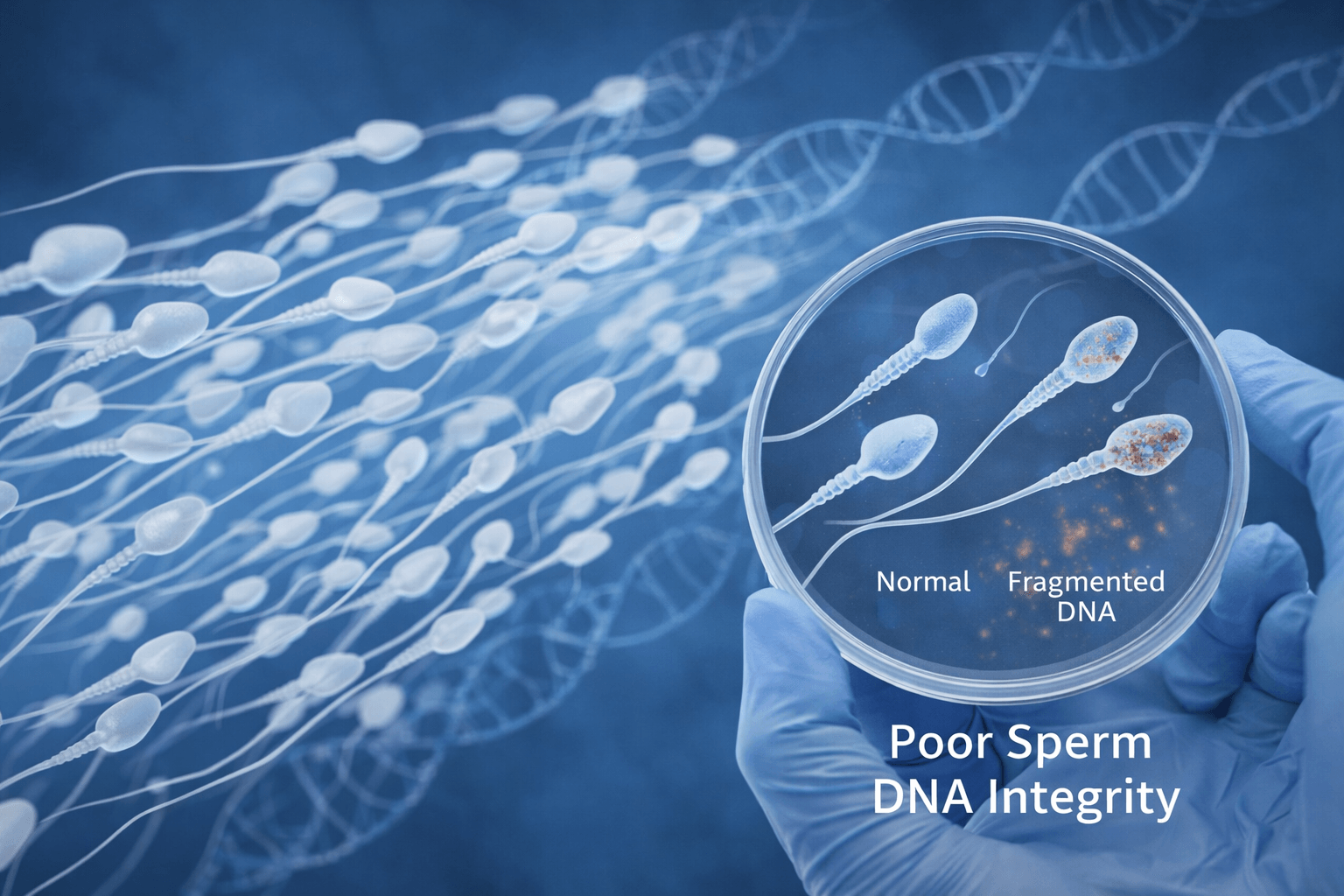
While miscarriage is often discussed in relation to female reproductive factors, research increasingly shows that male reproductive health can also influence pregnancy outcomes. One of the most important male factors associated with pregnancy loss is poor sperm DNA integrity. Damage to sperm DNA may interfere with embryo development after fertilization and increase the likelihood of miscarriage, particularly in cases of recurrent pregnancy loss [3] [9].
Understanding Sperm DNA Integrity
Sperm DNA carries the paternal genetic information that combines with the maternal genetic material to form the embryo. For normal embryo development to occur, this DNA must remain intact and stable.
Traditional semen analysis evaluates sperm count, motility, and morphology. However, these parameters do not always reflect the genetic quality of sperm. A man may have a normal semen report while still having significant DNA fragmentation within sperm cells.
Sperm DNA fragmentation refers to breaks or damage within the genetic material of sperm. When sperm with fragmented DNA fertilizes an egg, the resulting embryo may struggle to develop normally. In some cases, the embryo may fail to implant or may stop developing shortly after implantation, leading to miscarriage [9].
Causes of Sperm DNA Damage
Several biological and environmental factors can contribute to sperm DNA damage. One of the most common causes is oxidative stress, which occurs when harmful reactive oxygen species accumulate within reproductive tissues.
Oxidative stress may damage sperm DNA during sperm production in the testes or during sperm maturation within the epididymis. Factors known to increase oxidative stress include smoking, environmental toxins, excessive heat exposure, infections, and certain metabolic conditions.
Age may also influence sperm DNA quality. Although male fertility does not decline as sharply as female fertility, advancing paternal age has been associated with increased DNA fragmentation and genetic mutations in sperm [9].
Impact on Embryo Development
After fertilization, the embryo must undergo rapid cell division to develop properly. When sperm DNA damage is present, the embryo may inherit unstable genetic material that disrupts this process.
Some embryos with mild DNA damage may still develop normally because the egg has mechanisms that can repair limited genetic defects. However, when the degree of sperm DNA damage is severe, these repair mechanisms may not be sufficient.
In such cases the embryo may fail to implant, stop developing shortly after implantation, or result in early miscarriage [9].
Male Factors in Recurrent Miscarriage
In couples experiencing recurrent pregnancy loss, physicians sometimes evaluate male reproductive health more closely. Although sperm DNA testing is not routinely performed for every patient, it may be considered when miscarriage occurs repeatedly without an obvious cause.
Studies suggest that elevated sperm DNA fragmentation may be associated with reduced fertility and increased miscarriage risk in some couples [3] [9].
Importance of Male Reproductive Health
The role of male reproductive factors in miscarriage has gained increasing attention in recent years. While female reproductive health remains central to pregnancy success, recognizing the contribution of sperm DNA integrity helps provide a more complete understanding of reproductive biology.
Lifestyle and Environmental Factors
In addition to genetic, hormonal, and structural medical conditions, several lifestyle and environmental factors can influence the risk of miscarriage. These factors may affect reproductive hormones, egg and sperm quality, placental development, or the biological environment required to sustain pregnancy. While not all miscarriages are preventable, addressing modifiable lifestyle risks may help reduce pregnancy complications and support healthier reproductive outcomes [11] [12].
Smoking and Tobacco Exposure
Smoking is one of the most consistently identified lifestyle factors associated with miscarriage. Cigarette smoke contains numerous toxic chemicals, including nicotine, carbon monoxide, and heavy metals, which can interfere with normal reproductive physiology.
These substances may reduce blood flow to the placenta, impair oxygen delivery to the developing embryo, and increase oxidative stress within reproductive tissues. Studies have shown that women who smoke during pregnancy have a higher risk of miscarriage compared with non-smokers [12].
Exposure to secondhand smoke may also contribute to reproductive complications because inhaled toxins can affect both maternal circulation and fetal development.
Alcohol Consumption
Alcohol consumption during pregnancy has been associated with an increased risk of miscarriage and fetal developmental problems. Alcohol can cross the placenta and reach the developing embryo, where it may disrupt cellular growth and organ formation.
Because early pregnancy is a critical period for embryonic development, medical guidelines generally recommend avoiding alcohol when planning pregnancy or during pregnancy. Even moderate alcohol intake during early pregnancy may increase miscarriage risk in some studies [11].
Obesity and Metabolic Health
Body weight and metabolic health also influence reproductive outcomes. Obesity is associated with hormonal disturbances, insulin resistance, and chronic inflammation, all of which may affect fertility and pregnancy stability.
Women with obesity may experience higher rates of miscarriage compared with women with a healthy body weight. Excess adipose tissue can alter hormonal balance and influence the uterine environment, potentially affecting implantation and placental development [12].
Improving metabolic health through balanced nutrition, physical activity, and medical management of metabolic conditions may support healthier pregnancy outcomes.
Caffeine Intake
Caffeine is a stimulant commonly consumed in coffee, tea, energy drinks, and certain medications. While moderate caffeine intake is generally considered safe, very high levels of caffeine consumption during pregnancy have been associated with an increased risk of miscarriage in some observational studies.
Because caffeine can cross the placenta and affect fetal metabolism, many health authorities recommend limiting caffeine intake during pregnancy to moderate levels [11].
Environmental Toxins and Chemical Exposure
Environmental exposures may also affect reproductive health. Contact with industrial chemicals, pesticides, heavy metals, or environmental pollutants has been investigated for possible links to miscarriage.
These substances may influence hormonal signaling, increase oxidative stress, or interfere with fetal development. Occupational exposure to toxic chemicals in certain industries may therefore pose reproductive health risks if adequate protective measures are not taken [12].
Importance of Preventive Lifestyle Measures
While lifestyle factors are not responsible for most miscarriages, they represent modifiable influences that can support healthier pregnancy outcomes. Maintaining a balanced diet, avoiding tobacco and alcohol, limiting caffeine intake, and reducing exposure to environmental toxins may help improve reproductive health.
Healthcare providers often emphasize preventive care and healthy lifestyle choices as part of preconception counseling because improving overall health can contribute to better fertility and pregnancy outcomes [11] [13].
Ayurvedic Understanding of Recurrent Miscarriage

In Ayurveda, miscarriage is not viewed as an isolated reproductive event but as a disturbance in the delicate biological harmony required to sustain pregnancy. Classical Ayurvedic texts describe pregnancy as a coordinated interaction between the reproductive tissues of both parents, the uterine environment, maternal nutrition, and the balance of doshas. When these elements lose balance, pregnancy may not continue normally.
Recurrent miscarriage is discussed in Ayurvedic literature under the concepts of Garbha Srava and Garbha Pata, which refer to early and later pregnancy loss respectively. These conditions arise when the physiological support necessary for fetal development becomes weakened due to disturbances in doshas, reproductive tissues, or maternal health.
Garbha Formation and Stability in Ayurveda
Ayurvedic scholars emphasized that successful pregnancy depends on four essential factors: healthy reproductive elements from both parents, proper timing, a receptive uterine environment, and adequate maternal nutrition.
Charaka Samhita explains the formation of the embryo through the interaction of maternal and paternal reproductive tissues within the uterus.
Sanskrit Verse
“शुक्रशोणितसंयोगे जीवः गर्भाशयं गतः।
काले गर्भत्वमाप्नोति बीजभूमिसमाश्रयः॥”
Reference
Charaka Samhita, Sharira Sthana, Chapter 4, Verse 6.
Translation
When the reproductive elements of the father (Shukra) and mother (Shonita) unite in the uterus at the proper time, the living embryo becomes established within a suitable uterine environment.
This verse highlights a foundational Ayurvedic principle: pregnancy requires not only fertilization but also a healthy uterine environment and proper biological timing. When these conditions become disturbed, the embryo may fail to implant or may not continue developing.
Garbha Srava and Garbha Pata
Ayurveda classifies pregnancy loss based on the stage of gestation. Early pregnancy loss is known as Garbha Srava, while later pregnancy loss is referred to as Garbha Pata.
Sushruta Samhita describes these conditions in relation to disturbances of the doshas and weakness of the reproductive tissues.
Sanskrit Verse
“दोषैर्विकृतगर्भाशये गर्भः स्रवति निश्चयम्।
दुर्बलत्वाद्धि गर्भस्य पातो वा भवति ध्रुवम्॥”
Reference
Sushruta Samhita, Sharira Sthana, Chapter 2, Verse 33.
Translation
When the uterus becomes disturbed by aggravated doshas, the fetus may be expelled. If the fetus becomes weakened within such an environment, pregnancy loss inevitably occurs.
This classical explanation parallels modern understanding that the uterine environment must remain stable for pregnancy to continue. Disturbances in the internal biological environment can compromise fetal stability.
Beeja Dushti and Reproductive Tissue Health
Ayurvedic texts also emphasize the importance of the reproductive seed, known as Beeja. Beeja represents the genetic and biological integrity of reproductive cells from both parents.
If the reproductive seed becomes impaired, the embryo may not develop properly.
Bhavaprakasha explains this concept clearly.
Sanskrit Verse
“दुष्टे बीजे नरो नारी गर्भं न स्थापयेत् ध्रुवम्।
स्थापितोऽपि न तिष्ठेत् दोषदूषितजीवितः॥”
Reference
Bhavaprakasha, Purva Khanda, Chapter 3, Verse 21.
Translation
When the reproductive seed becomes defective in either the man or the woman, pregnancy may fail to establish, or if established it may not continue.
This concept of Beeja Dushti closely resembles the modern understanding of chromosomal abnormalities or genetic disturbances affecting embryo viability.
Dosha Imbalance and Pregnancy Loss
Ayurveda also explains miscarriage through disturbances in the three doshas: Vata, Pitta, and Kapha.
Among these, Vata dosha plays a particularly important role in pregnancy stability because it governs movement and physiological regulation within the body. When Vata becomes aggravated, it may disturb the stability of the fetus within the uterus.
Ashtanga Hridaya describes how aggravated doshas affect pregnancy.
Sanskrit Verse
“दोषैर्विकृतशरीरायां स्त्रियाम् गर्भो न तिष्ठति।
विशेषतः प्रकोपेण वातस्य पतनं ध्रुवम्॥”
Reference
Ashtanga Hridaya, Sharira Sthana, Chapter 1, Verse 44.
Translation
When the body of the pregnant woman becomes disturbed by aggravated doshas, the fetus may fail to remain in the uterus. In particular, aggravation of Vata can lead to pregnancy loss.
This principle explains why Ayurvedic pregnancy care focuses on stabilizing Vata, nourishing reproductive tissues, and maintaining systemic balance.
Importance of Maternal Health and Nutrition
Ayurveda places strong emphasis on maternal nutrition and lifestyle during pregnancy. The mother’s diet, emotional state, and daily habits directly influence fetal development.
Classical texts describe pregnancy as a condition in which the developing fetus draws nourishment from the mother’s tissues.
Charaka Samhita explains this relationship clearly.
Sanskrit Verse
“यथा वृक्षस्य मूलं सिंचेत् तदा शाखा प्रसर्पति।
तथा मातृपोषणेन गर्भः पुष्यति नित्यशः॥”
Reference
Charaka Samhita, Sharira Sthana, Chapter 8, Verse 32.
Translation
Just as watering the root of a tree nourishes its branches, proper nourishment of the mother sustains the growth of the fetus.
When maternal nutrition becomes insufficient or metabolic balance is disturbed, fetal growth may be compromised, increasing the risk of pregnancy loss.
Integrative Perspective
The Ayurvedic understanding of recurrent miscarriage emphasizes that pregnancy is sustained through harmony between reproductive tissues, uterine health, maternal nourishment, and doshic balance.
When these elements become disturbed through genetic defects, uterine disorders, hormonal disturbances, or systemic imbalance, pregnancy stability may be affected. By focusing on restoring reproductive tissue health, strengthening maternal vitality, and stabilizing doshic balance, Ayurvedic medicine seeks to create conditions that support successful pregnancy.
This classical perspective highlights that miscarriage is not merely a reproductive event but reflects deeper disturbances within the body’s systemic balance. Understanding these principles provides a broader framework for addressing recurrent pregnancy loss from a holistic perspective rooted in traditional Ayurvedic knowledge [14] [15] [16] [17].
How Miscarriage Risk Can Be Reduced
Reducing the risk of miscarriage requires a comprehensive approach that focuses on improving maternal health, identifying underlying medical conditions, and minimizing preventable risk factors. While not all miscarriages can be prevented, modern reproductive medicine recognizes that certain medical treatments and lifestyle measures can improve pregnancy outcomes in many patients. Addressing known risk factors before and during pregnancy can significantly increase the likelihood of a healthy pregnancy [2] [12].
Early Identification of Underlying Medical Conditions
One of the most effective ways to reduce miscarriage risk is to identify and manage underlying medical conditions that may interfere with pregnancy. Women who experience recurrent miscarriage or pregnancy complications may benefit from a detailed clinical evaluation.
Medical assessment may include evaluation of uterine structure, hormonal function, immune conditions, and genetic factors. Identifying the underlying cause allows physicians to recommend targeted treatment strategies. For example, structural abnormalities of the uterus may sometimes be corrected surgically, while endocrine disorders such as thyroid disease or diabetes can often be controlled with appropriate medical management [2].
Early medical evaluation is particularly important for women who have experienced repeated pregnancy loss because some causes of miscarriage are treatable once diagnosed.
Management of Immune and Clotting Disorders
Certain immune conditions can increase the risk of miscarriage by affecting placental blood flow. One of the most recognized conditions is antiphospholipid syndrome, an autoimmune disorder that increases the likelihood of abnormal blood clot formation.
When antiphospholipid syndrome is diagnosed, treatment with medications such as low-dose aspirin and anticoagulant therapy may help improve blood circulation to the placenta and support pregnancy continuation. Clinical studies have shown that appropriate treatment significantly improves pregnancy outcomes in affected women [6].
Because this condition is both diagnosable and treatable, screening for antiphospholipid antibodies is often recommended in patients with recurrent pregnancy loss.
Optimizing Preconception Health
Improving overall health before pregnancy can play an important role in reducing miscarriage risk. Preconception care focuses on optimizing maternal health and addressing modifiable risk factors that may affect reproductive outcomes.
Maintaining a healthy body weight, managing chronic medical conditions, and ensuring balanced nutrition can improve reproductive health. Obesity, metabolic disorders, and chronic inflammation have all been associated with adverse pregnancy outcomes in some clinical studies [12].
Regular medical checkups and early prenatal care allow healthcare providers to monitor pregnancy progress and identify potential complications early.
Avoiding Harmful Lifestyle Exposures
Lifestyle factors can influence pregnancy outcomes, and avoiding harmful exposures is an important preventive measure.
Smoking and tobacco exposure have been associated with increased miscarriage risk because toxic substances in cigarette smoke can reduce oxygen delivery to the developing embryo. Alcohol consumption during pregnancy may also disrupt fetal development and increase the likelihood of pregnancy complications.
Healthcare guidelines therefore recommend avoiding tobacco and alcohol when planning pregnancy or during pregnancy. Limiting caffeine intake and maintaining a balanced lifestyle may also support healthier pregnancy outcomes [13].
Preventive Screening and Vaccination
Preventive health care can also reduce certain pregnancy risks. Screening for infections, managing chronic diseases, and ensuring appropriate vaccination status are important components of preconception and prenatal care.
For example, vaccination against infections such as rubella before pregnancy can prevent serious complications that may affect fetal development. Early detection and treatment of infections may also reduce reproductive health risks.
Importance of Comprehensive Care
Reducing miscarriage risk often requires a coordinated approach involving obstetricians, fertility specialists, and other healthcare professionals. Because pregnancy involves multiple physiological systems, comprehensive care helps ensure that potential risk factors are identified and addressed early.
Although some miscarriages cannot be prevented, proactive medical evaluation, healthy lifestyle choices, and early prenatal care can significantly improve the chances of maintaining a successful pregnancy [2] [6] [12] [13].
When to Seek Medical Evaluation
Although miscarriage is relatively common and many pregnancies end spontaneously during the early weeks, certain situations require medical evaluation to ensure maternal safety and to identify possible underlying causes. Recognizing when to seek medical evaluation after miscarriage is important because early assessment may help detect complications, guide treatment, and improve future pregnancy outcomes [1] [2].
Medical guidelines emphasize that while a single miscarriage often occurs due to spontaneous genetic abnormalities, repeated pregnancy loss or unusual symptoms may indicate an underlying medical condition that requires investigation [3].
Persistent or Severe Symptoms During Pregnancy
Women should seek immediate medical care if they experience symptoms that may indicate complications during pregnancy or miscarriage. Heavy vaginal bleeding, severe abdominal pain, dizziness, or fainting may signal conditions such as incomplete miscarriage, infection, or ectopic pregnancy.
Medical evaluation helps ensure that the uterus has cleared properly and that no complications such as infection or retained pregnancy tissue remain. In some cases imaging tests such as ultrasound may be used to evaluate the uterus and confirm whether the pregnancy has been completely expelled [1].
After Recurrent Pregnancy Loss
Medical evaluation becomes especially important when miscarriage occurs repeatedly. Recurrent pregnancy loss is generally defined as two or more consecutive miscarriages.
In such cases physicians may recommend a comprehensive evaluation to identify possible contributing factors. Diagnostic assessment may include genetic testing, hormonal evaluation, uterine imaging, and immune system screening.
The purpose of this evaluation is to identify treatable causes of miscarriage so that appropriate management strategies can be implemented before future pregnancies [2] [3].
When There Is a History of Medical Conditions
Women with certain preexisting medical conditions should consult healthcare providers early during pregnancy or when planning pregnancy. Conditions such as thyroid disorders, diabetes, autoimmune disease, and clotting disorders may influence pregnancy outcomes and require careful medical management.
Early medical supervision allows physicians to adjust medications, monitor hormonal balance, and reduce potential pregnancy complications [2].
Suspected Infection During Pregnancy
Infections during pregnancy may increase the risk of complications if not properly managed. Symptoms such as fever, unusual vaginal discharge, pelvic pain, or signs of sexually transmitted infection should prompt medical evaluation.
Healthcare providers may perform laboratory testing to detect infections and recommend appropriate treatment. Screening for certain infections is also recommended as part of routine prenatal care to protect maternal and fetal health [8].
Difficulty Conceiving After Miscarriage
If pregnancy does not occur after a prolonged period following miscarriage, fertility evaluation may also be appropriate. Physicians may assess reproductive health through hormone testing, ovarian reserve evaluation, semen analysis, and imaging studies of the reproductive organs.
These evaluations help identify factors that may affect fertility and guide treatment planning for future pregnancies [3].
Importance of Early Medical Guidance
Seeking medical evaluation at the appropriate time helps ensure that complications are identified early and that patients receive proper guidance for future pregnancies. While miscarriage can be emotionally difficult, timely medical care allows physicians to determine whether the pregnancy loss was likely a random event or whether further evaluation is needed.
Table: When to Seek Medical Evaluation After Miscarriage
| Situation | Why Medical Evaluation Is Important |
|---|---|
| Two or more consecutive miscarriages | May indicate underlying fertility disorder |
| Heavy bleeding or severe pain | Could indicate incomplete miscarriage or ectopic pregnancy |
| Fever or infection symptoms | Possible infection affecting reproductive health |
| Difficulty conceiving after miscarriage | May require fertility evaluation |
| Known hormonal or immune disorders | Requires monitoring during pregnancy |
Can Recurrent Miscarriage Be Treated?
Recurrent miscarriage is one of the most emotionally difficult experiences for couples attempting to conceive. However, modern reproductive medicine recognizes that in many cases recurrent miscarriage can be treated or managed once the underlying cause is identified. Clinical guidelines emphasize that recurrent pregnancy loss is not a single disease but rather a condition with multiple possible causes, including genetic abnormalities, uterine structural problems, hormonal disorders, immune conditions, and lifestyle influences [2] [3].
Because these causes vary widely between patients, treatment strategies must be individualized based on the specific medical factors affecting pregnancy.
Treatment After Identifying the Underlying Cause
The first step in treating recurrent miscarriage is identifying the underlying cause through detailed evaluation. Physicians may investigate genetic factors, uterine structure, endocrine health, immune conditions, and reproductive infections.
Once the cause is identified, targeted treatment may be recommended. For example, structural abnormalities of the uterus such as a uterine septum may be corrected surgically, improving the chances of successful pregnancy. Similarly, endocrine disorders such as thyroid dysfunction or diabetes can often be managed with appropriate medical therapy to restore hormonal balance during pregnancy [2] [3].
Management of Antiphospholipid Syndrome
One of the most important treatable causes of recurrent miscarriage is antiphospholipid syndrome, an autoimmune disorder that affects blood clotting.
This condition causes the body to produce antibodies that increase the tendency for blood clots to form within blood vessels. During pregnancy, abnormal clotting can interfere with blood flow to the placenta, preventing the fetus from receiving adequate oxygen and nutrients.
When antiphospholipid syndrome is diagnosed, treatment with medications such as low-dose aspirin and anticoagulants can significantly improve pregnancy outcomes. Studies show that many women with this condition are able to carry pregnancies successfully when appropriate therapy is provided [6].
Genetic Counseling and Assisted Reproductive Options
In cases where parental chromosomal abnormalities are identified, genetic counseling may help couples understand their reproductive risks and possible treatment options.
Some couples may benefit from assisted reproductive technologies such as in vitro fertilization combined with preimplantation genetic testing. This approach allows embryos to be screened for chromosomal abnormalities before implantation, potentially reducing the risk of miscarriage [3].
Monitoring and Support During Pregnancy
Even when no specific cause is identified, many women with recurrent miscarriage can still achieve successful pregnancies with careful medical monitoring.
Early ultrasound examinations, hormonal monitoring, and supportive medical care can help physicians identify potential complications at an early stage. Regular follow-up also provides reassurance and emotional support during the early weeks of pregnancy, which are often the most stressful for couples with a history of miscarriage [2].
When the Cause Remains Unexplained
Despite extensive testing, a substantial proportion of recurrent miscarriage cases remain unexplained. In these situations, it may not be possible to identify a specific medical cause.
However, clinical studies indicate that many couples with unexplained recurrent pregnancy loss eventually achieve successful pregnancies without specialized interventions. This suggests that some miscarriages may result from temporary biological disturbances that resolve naturally over time [2] [3].
Importance of Individualized Care
Because recurrent miscarriage has many possible causes, effective treatment requires a personalized approach. Careful evaluation, evidence-based medical treatment, and ongoing pregnancy monitoring can significantly improve reproductive outcomes for many patients.
Ayurvedic Fertility Restoration Approach
In Ayurveda, the restoration of fertility and the prevention of recurrent miscarriage are approached through the broader framework of reproductive tissue health, dosha balance, and systemic vitality. Classical Ayurvedic texts explain that pregnancy stability depends on the integrity of the reproductive elements of both parents, the health of the uterus, proper nourishment of the maternal body, and balanced physiological regulation. When these elements become disturbed, pregnancy may fail to establish or may not continue normally.
Ayurvedic scholars describe this reproductive foundation through the concept of Beeja (reproductive seed), Kshetra (uterine environment), Ambu (nutritive support), and Kala (proper timing). When these four factors remain balanced, conception and fetal development can proceed normally.
Beeja Shuddhi: Purification of the Reproductive Seed
Ayurvedic literature emphasizes that the reproductive elements of both partners must be healthy for successful conception. The reproductive seed represents the biological integrity of the sperm and ovum that form the embryo.
Charaka Samhita describes the importance of healthy reproductive elements in the formation of a stable pregnancy.
Sanskrit Verse
“शुक्रशोणितसंयोगे जीवः गर्भाशयं गतः।
काले गर्भत्वमाप्नोति बीजभूमिसमाश्रयः॥”
Reference
Charaka Samhita, Sharira Sthana, Chapter 4, Verse 6.
Translation
When the reproductive elements of the father and mother unite within a suitable uterine environment at the proper time, the embryo becomes established and pregnancy begins.
This concept parallels modern reproductive medicine, which recognizes that genetic integrity of sperm and egg is essential for embryo viability and pregnancy continuation [2] [3].
Ayurvedic therapy therefore focuses on strengthening reproductive tissues and improving the biological quality of sperm and ovum before conception.
Kshetra Shuddhi: Restoring Uterine Health
The uterus is described in Ayurveda as the Kshetra, or field, in which the embryo grows. For pregnancy to continue normally, this field must be healthy, nourished, and free from disturbances.
Sushruta Samhita explains how disturbances in the uterine environment can lead to pregnancy loss.
Sanskrit Verse
“दोषैर्विकृतगर्भाशये गर्भः स्रवति निश्चयम्।
दुर्बलत्वाद्धि गर्भस्य पातो वा भवति ध्रुवम्॥”
Reference
Sushruta Samhita, Sharira Sthana, Chapter 2, Verse 33.
Translation
When the uterus becomes disturbed by aggravated doshas, the fetus may be expelled or fail to remain established.
This classical description reflects the importance of maintaining a stable uterine environment, similar to the modern understanding that uterine abnormalities, inflammation, or hormonal disturbances can interfere with pregnancy stability [2] [3].
Ayurvedic therapies for reproductive health therefore focus on restoring uterine balance, improving circulation, and strengthening the reproductive system.
Role of Dosha Balance in Pregnancy Stability
Ayurveda explains pregnancy stability through the balanced function of the three doshas: Vata, Pitta, and Kapha. Among these, Vata dosha plays a particularly important role because it governs movement and physiological regulation within the body.
Ashtanga Hridaya explains that aggravation of Vata can disturb the stability of the fetus within the uterus.
Sanskrit Verse
“दोषैर्विकृतशरीरायां स्त्रियाम् गर्भो न तिष्ठति।
विशेषतः प्रकोपेण वातस्य पतनं ध्रुवम्॥”
Reference
Ashtanga Hridaya, Sharira Sthana, Chapter 1, Verse 44.
Translation
When the body becomes disturbed by aggravated doshas, the fetus may fail to remain in the uterus. Aggravation of Vata especially leads to pregnancy loss.
Because of this principle, Ayurvedic reproductive care often emphasizes stabilizing Vata and nourishing the reproductive tissues during pregnancy.
Importance of Maternal Nourishment
Ayurvedic texts also emphasize that the mother’s health and nutrition directly influence fetal development. The developing fetus draws nourishment from the mother’s tissues, and inadequate maternal nutrition may weaken pregnancy stability.
Bhavaprakasha highlights the importance of maternal nourishment for fetal growth.
Sanskrit Verse
“यथा मूलं सिच्यते वृक्षस्य तदा शाखा प्रसर्पति।
तथा मातृपोषणेन गर्भः पुष्यति नित्यशः॥”
Reference
Bhavaprakasha, Purva Khanda, Chapter 3, Verse 21.
Translation
Just as watering the root nourishes the branches of a tree, proper nourishment of the mother supports the growth of the fetus.
This concept corresponds to modern medical understanding that maternal health, nutrition, and metabolic balance are essential for maintaining pregnancy [2] [3].
Ayurvedic Perspective on Fertility Restoration
The Ayurvedic approach to fertility restoration therefore focuses on strengthening reproductive tissues, improving uterine health, balancing doshas, and nourishing the maternal body. By restoring systemic balance and enhancing reproductive vitality, Ayurvedic medicine aims to create a physiological environment that supports stable pregnancy.
This classical perspective emphasizes that recurrent miscarriage may reflect deeper disturbances in reproductive health rather than a single isolated cause. Through comprehensive care aimed at restoring biological balance, Ayurveda seeks to support successful conception and healthy pregnancy outcomes [14] [15] [16] [17] while aligning with modern reproductive understanding of pregnancy health [2] [3].
Recurrent miscarriage is often a symptom of deeper fertility problems. Understanding these underlying issues is essential for restoring reproductive health. Our detailed guide explains this in depth in Infertility Causes, Diagnosis and Treatment.
Frequently Asked Questions
What is the most common cause of miscarriage?
The most common cause of miscarriage is chromosomal abnormality in the embryo. These genetic errors occur when the embryo receives an abnormal number of chromosomes during fertilization, preventing normal development. Most early miscarriages happen for this reason and are usually random events that cannot be prevented.
Can stress cause miscarriage?
Normal levels of emotional stress are not considered a direct cause of miscarriage. However, extreme physical stress, severe illness, or significant physiological strain on the body may contribute to pregnancy complications. Maintaining good physical and emotional health during pregnancy is still important for overall well-being.
Does age increase the risk of miscarriage?
Yes. Maternal age is one of the strongest risk factors for miscarriage. As women age, egg quality gradually declines, increasing the likelihood of chromosomal abnormalities in the embryo. This is why miscarriage rates tend to increase after the mid-thirties.
Can infections lead to miscarriage?
Certain infections can increase the risk of pregnancy complications. Viral infections such as rubella, cytomegalovirus, and some bacterial infections affecting the reproductive tract may interfere with placental development or fetal growth. Screening and preventive care help reduce these risks.
Is recurrent miscarriage treatable?
In many cases recurrent miscarriage can be treated once the underlying cause is identified. Medical evaluation may detect hormonal disorders, uterine abnormalities, immune conditions, or genetic factors that can be managed through appropriate medical treatment.
How many miscarriages are considered recurrent miscarriage?
Recurrent miscarriage is usually defined as two or more consecutive pregnancy losses. When this occurs, physicians often recommend further medical evaluation to identify possible underlying causes and guide treatment strategies.
Can lifestyle factors affect miscarriage risk?
Yes. Smoking, alcohol consumption, obesity, and exposure to environmental toxins may increase miscarriage risk. Maintaining a healthy lifestyle, balanced nutrition, and proper medical care before and during pregnancy can support better reproductive outcomes.
Can men contribute to miscarriage risk?
Yes. Male reproductive health can influence pregnancy outcomes. Damage to sperm DNA or genetic abnormalities in sperm may affect embryo development and may contribute to miscarriage in some couples.
Can miscarriage be prevented?
Not all miscarriages can be prevented because many occur due to genetic abnormalities beyond human control. However, managing medical conditions, maintaining good health, and receiving appropriate prenatal care can help reduce the risk in some cases.
When should someone see a doctor after a miscarriage?
Medical evaluation is recommended if miscarriage occurs repeatedly, if there are severe symptoms such as heavy bleeding or infection, or if pregnancy does not occur again after a prolonged period. A physician can help determine whether further testing or treatment is needed
Reference
[1] American College of Obstetricians and Gynecologists. (2018). Early pregnancy loss: Practice Bulletin No. 200. Obstetrics & Gynecology, 132(5), e197-e207. ACOG clinical guidance page: https://www.acog.org/clinical/clinical-guidance/practice-bulletin/articles/2018/11/early-pregnancy-loss
Brief: This is a core clinical source for defining miscarriage, explaining diagnosis, and outlining standard medical management of early pregnancy loss.
[2] ESHRE Guideline Group on Recurrent Pregnancy Loss. (2023). ESHRE guideline: Recurrent pregnancy loss, update in 2022. Human Reproduction Open, 2023(1), hoad002. https://academic.oup.com/hropen/article/2023/1/hoad002/7068067
Brief: This is one of the most important evidence-based guidelines for recurrent miscarriage. It covers definition, investigations, uterine causes, endocrine causes, thrombophilia-related issues, and treatment pathways.
[3] Practice Committee of the American Society for Reproductive Medicine. (2012). Evaluation and treatment of recurrent pregnancy loss: A committee opinion. Fertility and Sterility, 98(5), 1103-1111. https://www.asrm.org/practice-guidance/practice-committee-documents/evaluation-and-treatment-of-recurrent-pregnancy-loss-a-committee-opinion-2012/
Brief: This committee opinion is a foundational reproductive medicine reference on recurrent miscarriage workup, including parental genetics, uterine abnormalities, endocrine disorders, antiphospholipid syndrome, and selected male factors.
[4] Chan, Y. Y., Jayaprakasan, K., Zamora, J., Thornton, J. G., Raine-Fenning, N., & Coomarasamy, A. (2011). The prevalence of congenital uterine anomalies in unselected and high-risk populations: A systematic review. Human Reproduction Update, 17(6), 761-771. https://pubmed.ncbi.nlm.nih.gov/21705770/
Brief: This systematic review helps explain how congenital uterine abnormalities are more common in women with infertility and pregnancy loss histories. It is useful for the uterine-abnormality subsection.
[5] Sarkar, D. (2013). Recurrent pregnancy loss in patients with thyroid dysfunction. Indian Journal of Endocrinology and Metabolism, 17(Suppl 1), S111-S114. https://pmc.ncbi.nlm.nih.gov/articles/PMC3603072/
Brief: This paper explains how thyroid dysfunction and thyroid autoimmunity may contribute to recurrent miscarriage risk. It is useful for the hormonal-imbalance section.
[6] Murvai, V. R., et al. (2025). Antiphospholipid syndrome in pregnancy: A comprehensive literature review. Biomedicines, 13(3), 563. https://pmc.ncbi.nlm.nih.gov/articles/PMC11934569/
Brief: This review explains how antiphospholipid syndrome can affect pregnancy, including recurrent miscarriage, placental complications, and management principles.
[7] Giakoumelou, S., Wheelhouse, N., Cuschieri, K., Entrican, G., Howie, S. E. M., & Horne, A. W. (2016). The role of infection in miscarriage. Human Reproduction Update, 22(1), 116-133. https://pubmed.ncbi.nlm.nih.gov/26386469/
Brief: This is a major review on infection-related miscarriage risk. It is useful when discussing hidden infectious contributors, while still keeping the wording balanced and evidence-based.
[8] Centers for Disease Control and Prevention. (2025). About STIs and pregnancy. https://www.cdc.gov/sti/about/about-stis-and-pregnancy.html
Brief: This CDC page explains why sexually transmitted infections matter during pregnancy and why appropriate screening and treatment are important for maternal and fetal health.
[9] Agarwal, A., Majzoub, A., Baskaran, S., Panner Selvam, M. K., Cho, C. L., Henkel, R., & Parekh, N. (2024). Sperm DNA fragmentation and infertility: A narrative review. Translational Andrology and Urology, 13(7), 1211-1228. https://pubmed.ncbi.nlm.nih.gov/38990348/
Brief: This review is useful for explaining why normal semen parameters do not always rule out male-factor contribution to recurrent miscarriage, especially when sperm DNA fragmentation is involved.
[10] Baud, D., Goy, G., Jaton, K., Osterheld, M. C., Blumer, S., Borel, N., & Greub, G. (2011). Role of Chlamydia trachomatis in miscarriage. Emerging Infectious Diseases, 17(9), 1630-1635. https://wwwnc.cdc.gov/eid/article/17/9/10-0865_article
Brief: This original study is highly relevant for hidden infectious causes, especially silent genital infection and its association with miscarriage.
[11] National Health Service. (2023). Miscarriage: Causes. https://www.nhs.uk/conditions/miscarriage/causes/
Brief: This patient-friendly NHS source is useful for explaining age-related miscarriage risk and recognized lifestyle-associated factors such as smoking, alcohol, obesity, and excessive caffeine.
[12] Wesselink, A. K., et al. (2022). Pre-pregnancy lifestyle characteristics and risk of miscarriage: The Australian Longitudinal Study on Women’s Health. Human Reproduction, 37(6), 1276-1286. https://pmc.ncbi.nlm.nih.gov/articles/PMC8887017/
Brief: This cohort study supports the role of pre-pregnancy lifestyle factors such as smoking, weight status, and alcohol in miscarriage risk.
[13] National Health Service. (2023). Miscarriage: Prevention. https://www.nhs.uk/conditions/miscarriage/prevention/
Brief: This source helps with the prevention section by supporting practical advice on smoking cessation, alcohol avoidance, healthy weight, and general pregnancy-health measures.
[14] Agnivesha. Charaka Samhita, Sharira Sthana, standard edition used in your manuscript.
Brief: This classical text is useful for Garbha formation, Beeja, maternal contribution, and the Ayurvedic basis of fetal stability and reproductive health.
[15] Sushruta. Sushruta Samhita, Sharira Sthana, standard edition used in your manuscript.
Brief: This text supports Ayurvedic interpretation of fetal development, pregnancy maintenance, and pathological states related to pregnancy loss.
[16] Vagbhata. Ashtanga Hridaya, Sharira Sthana / Uttara Sthana, standard edition used in your manuscript.
Brief: This source is useful for maternal regimen, preservation of pregnancy, and doshic factors that may affect Garbha stability.
[17] Bhavamishra. Bhavaprakasha, Purva Khanda, standard edition used in your manuscript.
Brief: This text is useful for Artava, Beeja Dushti, and reproductive tissue understanding in the Ayurvedic section.