- Why Diet Plays a Central Role in IBS Symptoms
- Common Foods That Trigger IBS Symptoms
- IBS-Friendly Foods That May Help Calm the Gut
- The Low-FODMAP Diet Explained
- Why IBS Diet Advice Often Conflicts
- Meal Timing and Eating Habits That Influence IBS
- Ayurvedic Perspective on Diet and IBS
- Why Diet Alone Often Fails to Resolve IBS
- Signs Your IBS May Require Deeper Treatment
- Reference
IBS Diet and the Role of Food in Digestive Symptoms
The IBS diet is one of the most important factors influencing symptoms of irritable bowel syndrome. Many individuals living with IBS notice that abdominal pain, bloating, diarrhea, or constipation often worsen after eating certain foods. Because of this strong connection between food and digestive symptoms, understanding how the IBS diet affects the gut has become essential for managing the condition.
Irritable bowel syndrome is a functional gastrointestinal disorder that affects the way the intestines move and respond to digestion. It is estimated that a significant portion of the global population experiences IBS symptoms, making it one of the most common digestive disorders worldwide [1]. While the exact cause of IBS is complex and multifactorial, diet remains one of the most immediate triggers for symptom flare-ups.
Food can influence IBS symptoms through several biological mechanisms. Certain carbohydrates may ferment in the colon, producing gas that leads to bloating and discomfort. Other foods may stimulate intestinal contractions or affect gut sensitivity, causing changes in bowel habits. Because the digestive system of IBS patients tends to be more sensitive than normal, even small dietary triggers can produce noticeable symptoms.
IBS Diet and the Gut Microbiome
Another important factor in the IBS diet is the interaction between food and the gut microbiome. The digestive tract contains trillions of microorganisms that help break down nutrients, regulate immune responses, and influence intestinal health. When certain foods are poorly absorbed, they can become substrates for bacterial fermentation in the colon.
This fermentation process produces gases and metabolites that may increase abdominal distension and intestinal discomfort in IBS patients [8]. As a result, foods that ferment easily in the gut are often associated with symptom worsening. Understanding which foods contribute to this fermentation is an important step in developing an effective IBS diet.
IBS Diet and the Gut–Brain Connection
The relationship between the IBS diet and digestive symptoms is also influenced by the gut–brain axis. The digestive tract contains an extensive network of nerves that communicate continuously with the central nervous system. In individuals with IBS, this communication pathway may become dysregulated, making the intestines more sensitive to normal digestive processes.
This heightened sensitivity means that even routine digestion after meals can produce discomfort or pain. Stress, emotional factors, and dietary triggers may all influence how the gut responds to food through this gut–brain signaling pathway [9]. Because of this complex interaction, the same meal may cause severe symptoms in one individual while remaining harmless for another.
IBS Diet and the Need for Personalized Nutrition
One of the most important realities of the IBS diet is that there is no single universal diet that works for every patient. Different individuals react differently to foods depending on their microbiome composition, digestive enzyme activity, gut motility patterns, and nervous system sensitivity.
For this reason, many patients experiment with dietary strategies such as eliminating trigger foods, following structured dietary plans, or adjusting meal timing. While some individuals experience significant improvement with dietary adjustments, others find that symptoms persist despite strict dietary control.
Why Diet Plays a Central Role in IBS Symptoms

Food Fermentation and Gas Production in the IBS Diet
The IBS diet strongly influences how food is processed in the digestive tract. One of the most common mechanisms through which food triggers IBS symptoms is fermentation inside the colon. When certain carbohydrates are not fully absorbed in the small intestine, they travel into the large intestine where gut bacteria begin to break them down. This fermentation process produces gases such as hydrogen, methane, and carbon dioxide, which can lead to bloating, abdominal pressure, and discomfort.
Many individuals with IBS are particularly sensitive to this gas production. Even normal amounts of intestinal gas may stretch the intestinal walls and produce pain due to increased visceral sensitivity. Research has shown that fermentable carbohydrates are among the most common dietary triggers reported by IBS patients, which explains why certain dietary approaches focus on reducing fermentable foods [4].
Understanding this fermentation process helps patients recognize why specific foods repeatedly cause symptoms. Foods that ferment quickly in the gut may trigger bloating or cramps within hours after eating, making dietary awareness an important part of symptom management.
Gut Microbiome Interaction and the IBS Diet
Another key reason diet plays such a major role in IBS symptoms is the interaction between food and the gut microbiome. The digestive system contains trillions of microorganisms that participate in digestion, nutrient absorption, and immune regulation. These microbes also influence how food components are metabolized within the intestines.
Different people have different microbial communities in their digestive tract. Because of this variation, the same food may be tolerated well by one person but trigger significant symptoms in another. When certain foods are consumed, gut bacteria may produce gases and metabolic byproducts that contribute to bloating, intestinal irritation, and changes in bowel habits [8].
This microbiome interaction explains why IBS diet recommendations often emphasize identifying personal food triggers rather than applying a universal dietary rule for all patients.
Intestinal Nerve Sensitivity and Food Triggers
In individuals with IBS, the nerves within the digestive tract often become hypersensitive. This condition, known as visceral hypersensitivity, means that the intestines respond more strongly to normal digestive processes such as stretching, gas formation, or bowel contractions.
When food enters the digestive tract, it naturally stimulates intestinal movement and secretion of digestive enzymes. For most people this process occurs without noticeable symptoms. However, in IBS patients these normal digestive events may produce pain, cramping, or discomfort because the intestinal nerves are more reactive [1].
As a result, certain foods may appear to cause symptoms even when they are not harmful themselves. The symptoms arise from the heightened sensitivity of the digestive nervous system rather than from structural damage to the intestines.
Changes in Intestinal Motility After Meals
The IBS diet also affects how quickly food moves through the digestive tract. After eating, the body activates a natural reflex known as the gastrocolic response, which increases intestinal contractions to help move digested material through the colon.
In individuals with IBS, this reflex may become exaggerated. Some patients experience rapid intestinal movement that leads to diarrhea shortly after meals, while others develop slowed motility that contributes to constipation. These motility changes can make symptoms closely linked to eating patterns [1].
Because of these physiological responses, diet often becomes the most noticeable trigger for IBS symptoms. Recognizing how food interacts with fermentation, microbiome activity, nerve sensitivity, and intestinal motility helps explain why dietary strategies play such an important role in managing irritable bowel syndrome.
Common Foods That Trigger IBS Symptoms

Many individuals living with irritable bowel syndrome notice that symptoms worsen after eating specific foods. Understanding these IBS food triggers is an important step in building an effective IBS diet. Certain foods can increase intestinal fermentation, stimulate gut motility, or irritate sensitive intestinal nerves, all of which may lead to abdominal pain, bloating, diarrhea, or constipation.
Research suggests that a large proportion of IBS patients report food-related symptom flare-ups, particularly after consuming fermentable carbohydrates or poorly digested nutrients [3]. Because digestion and gut microbiome composition vary between individuals, the exact foods that trigger symptoms may differ from one person to another. However, several categories of foods are consistently associated with worsening IBS symptoms and are often recommended to be limited in an IBS diet [4].
High-FODMAP Foods
High-FODMAP foods are among the most widely recognized dietary triggers for IBS symptoms. FODMAP is an acronym for fermentable oligosaccharides, disaccharides, monosaccharides, and polyols. These carbohydrates are poorly absorbed in the small intestine and can ferment in the colon, producing gas and drawing water into the bowel.
This fermentation process can lead to bloating, abdominal discomfort, and changes in bowel movements, particularly in individuals with sensitive intestines. Clinical studies have shown that reducing high-FODMAP foods in the IBS diet can significantly improve symptoms in many patients [3]. Common high-FODMAP foods include onions, garlic, apples, wheat-based products, beans, and certain sweeteners.
Dairy and Lactose Intolerance
Dairy products are another common dietary trigger for IBS symptoms, particularly in individuals who have lactose intolerance. Lactose is the natural sugar found in milk and dairy products. When lactose is not properly digested due to low levels of the enzyme lactase, it can reach the colon and undergo bacterial fermentation.
This fermentation can produce gas, bloating, and diarrhea, which closely resemble IBS symptoms. For this reason, many IBS patients experience symptom relief after reducing or eliminating lactose-containing foods from their IBS diet [6]. Dairy products such as milk, ice cream, and soft cheeses are the most common sources of lactose.
High-Fat Meals
High-fat foods may also worsen IBS symptoms, especially in individuals with diarrhea-predominant IBS. Fatty meals can stimulate strong contractions in the intestines and accelerate bowel movement, which may contribute to abdominal cramping and urgency.
In addition to affecting gut motility, high-fat meals may also slow gastric emptying and increase the sensation of fullness or bloating after eating. Fried foods, processed snacks, and heavy restaurant meals are frequently reported as triggers in the IBS diet and are often recommended to be limited for symptom control [4].
Artificial Sweeteners
Artificial sweeteners are commonly used in sugar-free foods, beverages, and chewing gums. Some sweeteners such as sorbitol, mannitol, and xylitol belong to the polyol group of FODMAP carbohydrates. Because these compounds are poorly absorbed in the intestine, they may ferment in the colon and produce gas and bloating.
In sensitive individuals, artificial sweeteners can also cause diarrhea due to their osmotic effect in the intestines. As a result, reducing sugar-free products and foods containing these sweeteners may help improve symptoms in some IBS patients [3].
Carbonated Beverages
Carbonated beverages can contribute to increased gas accumulation in the digestive tract. The dissolved carbon dioxide in these drinks is released as gas in the stomach and intestines, which can increase abdominal distension and bloating.
For individuals with IBS who already have heightened gut sensitivity, this additional gas may worsen discomfort or pressure in the abdomen. Limiting carbonated beverages such as sodas and sparkling drinks is often recommended as part of an IBS diet designed to reduce bloating and digestive irritation [6].
IBS-Friendly Foods That May Help Calm the Gut

For many individuals living with irritable bowel syndrome, adjusting the IBS diet to include foods that are easier to digest can significantly reduce symptoms such as bloating, abdominal discomfort, and irregular bowel movements. While some foods tend to trigger IBS symptoms, others are generally better tolerated and may help stabilize digestion.
Dietary guidelines for IBS often emphasize choosing foods that produce less intestinal fermentation, support normal bowel function, and reduce irritation of the digestive tract [6]. Because IBS symptoms vary from person to person, identifying foods that calm the gut can help patients gain greater control over their digestive health and improve daily comfort.
Low-Fermentation Carbohydrates
Low-fermentation carbohydrates are often recommended as part of an IBS diet because they are less likely to produce gas during digestion. Unlike fermentable carbohydrates that rapidly break down in the colon, these foods are absorbed more efficiently in the small intestine and therefore produce fewer fermentation byproducts.
Examples of low-fermentation carbohydrates include rice, oats, quinoa, and potatoes. These foods provide energy while remaining relatively gentle on the digestive system. Many individuals with IBS find that replacing highly fermentable foods with these options helps reduce bloating and abdominal pressure.
Lean Proteins
Lean proteins are another important component of an IBS-friendly diet. Protein foods generally do not ferment in the intestine the same way certain carbohydrates do, which means they are less likely to produce gas or trigger bloating.
Common lean protein sources include fish, chicken, eggs, and tofu. These foods provide essential amino acids needed for tissue repair and metabolic function while remaining relatively easy to digest. Including balanced portions of lean protein in meals can also help maintain stable blood sugar levels and support overall digestive stability.
Gentle Fruits
Some fruits are better tolerated in IBS because they contain lower amounts of fermentable sugars. Gentle fruits such as bananas, blueberries, strawberries, and oranges are commonly included in IBS diet plans due to their relatively low fermentation potential.
These fruits provide vitamins, antioxidants, and dietary fiber while remaining less likely to trigger gas production. Choosing moderate portions of these fruits can allow individuals with IBS to obtain nutritional benefits without significantly increasing digestive discomfort.
Gut-Supportive Fermented Foods
Certain fermented foods may also support digestive balance by contributing beneficial microorganisms to the gut microbiome. Foods such as yogurt, kefir, and traditionally fermented vegetables contain probiotics that may influence microbial diversity in the digestive tract.
Clinical dietary guidelines for IBS note that probiotics and fermented foods may help improve some symptoms in certain individuals, although responses can vary depending on the individual’s microbiome composition [7]. For this reason, fermented foods are often introduced gradually as part of a carefully adjusted IBS diet.
Incorporating these IBS-friendly foods into daily meals can help many patients create a more stable digestive environment. As individuals begin identifying which foods calm their gut and which foods trigger symptoms, they often realize that dietary choices can play a powerful role in managing IBS symptoms and improving quality of life.
The Low-FODMAP Diet Explained

The low FODMAP diet IBS approach is one of the most widely researched dietary strategies for managing symptoms of irritable bowel syndrome. Many patients experience bloating, abdominal pain, and irregular bowel movements after eating certain fermentable carbohydrates. The low-FODMAP diet focuses on reducing these specific carbohydrates in order to minimize intestinal fermentation and improve digestive comfort.
Clinical research has shown that a carefully implemented low-FODMAP diet can significantly reduce IBS symptoms in many patients [3]. However, understanding how this diet works requires knowing what FODMAP carbohydrates are and how they interact with digestion and gut microbes.
What FODMAP Means
FODMAP is an acronym that stands for fermentable oligosaccharides, disaccharides, monosaccharides, and polyols. These are short-chain carbohydrates that are often poorly absorbed in the small intestine.
When these carbohydrates reach the colon without being fully digested, they become substrates for fermentation by intestinal bacteria. This fermentation produces gases such as hydrogen and methane, which can contribute to abdominal distension, bloating, and discomfort in individuals with sensitive digestive systems [4].
Common examples of high-FODMAP foods include onions, garlic, wheat-based products, beans, certain fruits like apples and pears, and sweeteners such as sorbitol or mannitol.
How FODMAP Foods Cause Gas and Bloating
The symptoms associated with high-FODMAP foods occur primarily because of two physiological mechanisms. First, these carbohydrates draw water into the intestine through an osmotic effect. Second, they are rapidly fermented by gut bacteria in the colon.
This fermentation process produces gas that expands the intestinal lumen, which can lead to bloating, abdominal pressure, and visible distension. For individuals with IBS, the digestive tract often exhibits heightened nerve sensitivity, meaning that even small increases in gas or intestinal stretching can trigger discomfort or pain [5].
Because of this combination of fermentation and gut sensitivity, high-FODMAP foods frequently act as dietary triggers in IBS.
The Three Phases of the Diet
The low-FODMAP diet is usually implemented in three structured phases to help identify individual food triggers.
The first phase is the elimination phase, during which high-FODMAP foods are temporarily restricted. This stage typically lasts several weeks and allows symptoms to stabilize.
The second phase is the reintroduction phase, where specific FODMAP groups are gradually reintroduced one at a time. This helps identify which carbohydrates are responsible for triggering symptoms.
The third phase is the personalization phase, where a long-term diet is developed based on individual tolerance. Instead of permanently avoiding all FODMAP foods, patients learn which foods they can safely include in their IBS diet without triggering symptoms.
Limitations of Long-Term FODMAP Restriction
While the low-FODMAP diet can be highly effective for short-term symptom control, long-term restriction of fermentable carbohydrates may have certain limitations. Some FODMAP foods serve as prebiotics that support beneficial gut bacteria. Eliminating them for extended periods may reduce microbial diversity in the gut microbiome [5].
For this reason, most clinical guidelines recommend using the low-FODMAP diet as a temporary diagnostic and management tool rather than a permanent restrictive diet. A personalized IBS diet that balances symptom control with nutritional adequacy is generally considered the most sustainable long-term approach.
Why IBS Diet Advice Often Conflicts
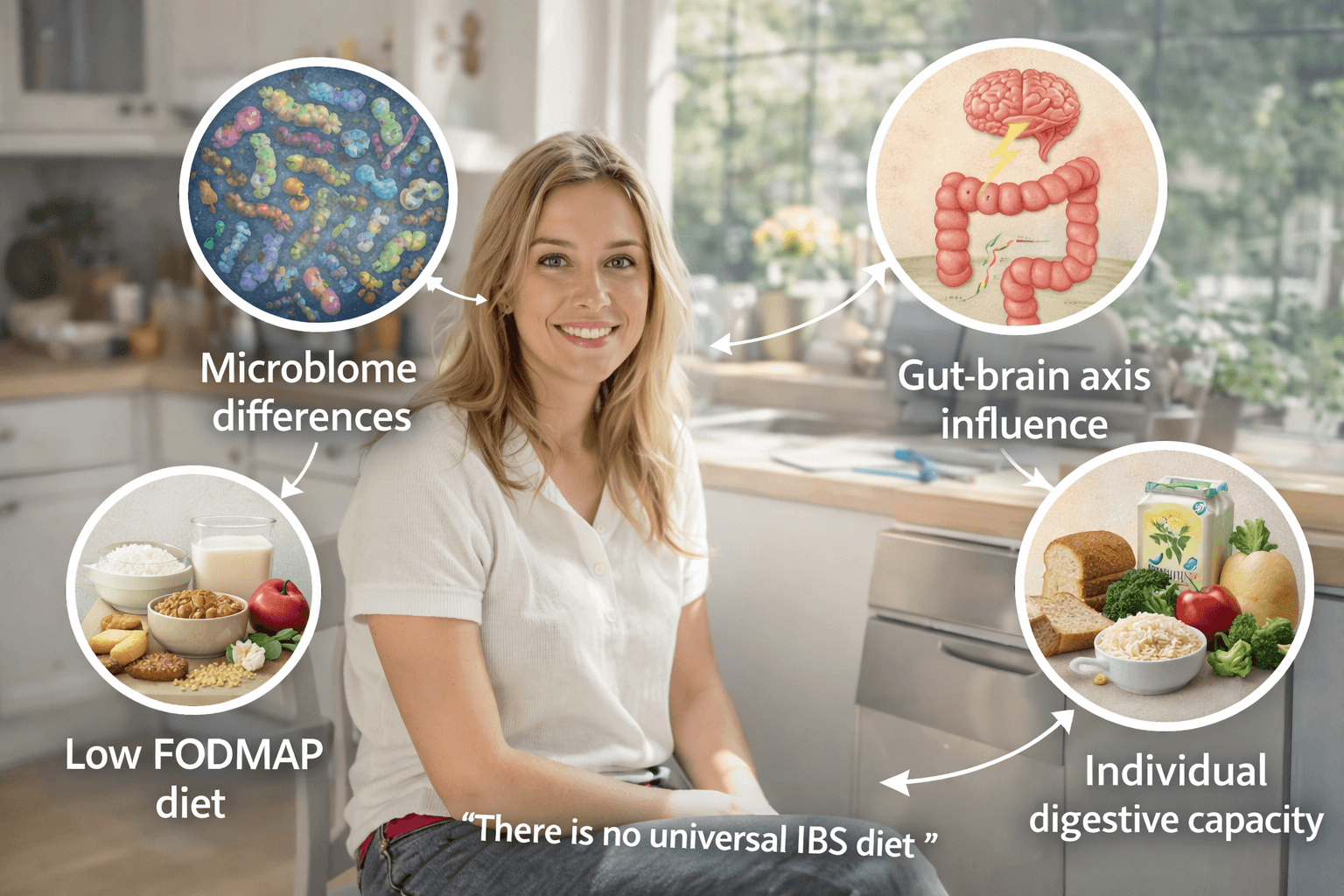
Many people searching for the best IBS diet quickly notice something confusing. Different sources often recommend completely different dietary strategies. Some doctors suggest a low-FODMAP diet, others recommend avoiding gluten or dairy, while certain nutritional programs emphasize increasing fiber or eating fermented foods. For many patients, these conflicting recommendations create frustration and uncertainty.
The reason IBS diet advice often conflicts is that irritable bowel syndrome is not a single uniform disease. Instead, it is a complex digestive disorder influenced by several biological factors, including gut microbiome composition, nervous system signaling, intestinal sensitivity, and individual digestive capacity. Because these factors vary significantly from one person to another, dietary triggers and responses can differ widely [5].
Microbiome Differences
One of the most important reasons IBS diet advice varies is the unique composition of the gut microbiome in each individual. The human digestive tract contains trillions of microorganisms that help break down food, regulate immune responses, and produce metabolites that influence intestinal function.
However, the balance of these microorganisms differs from person to person. When fermentable foods reach the colon, gut bacteria break them down and produce gases and other byproducts. In some individuals, this fermentation may cause minimal symptoms, while in others it may produce significant bloating, abdominal discomfort, and bowel changes [8].
Because microbiome composition differs among individuals, a food that triggers symptoms in one patient may be well tolerated by another. This explains why IBS diet recommendations often appear inconsistent across different sources.
Gut–Brain Axis Influence
Another factor that contributes to conflicting IBS diet advice is the interaction between the digestive system and the nervous system. The gut contains an extensive network of nerves that communicate continuously with the brain through what is known as the gut–brain axis.
In individuals with IBS, this communication pathway may become dysregulated, causing heightened sensitivity in the intestinal nerves. As a result, normal digestive processes such as gas production or intestinal stretching may trigger pain or discomfort [9].
Because stress levels, emotional state, and nervous system signaling differ between individuals, dietary triggers may also vary depending on how the gut–brain axis responds to food.
Individual Digestive Capacity
Digestive enzyme activity and intestinal motility also differ among individuals. Some people efficiently digest carbohydrates, fats, and proteins, while others may have reduced enzyme activity or altered intestinal movement patterns.
These variations influence how food is processed within the digestive tract. For example, some individuals may tolerate dairy products well, while others develop symptoms due to lactose malabsorption. Similarly, certain fibers may improve bowel function in some patients while worsening bloating in others.
Because digestive capacity is highly individualized, dietary strategies that improve symptoms for one IBS patient may not produce the same results for another.
Meal Timing and Eating Habits That Influence IBS

The IBS diet is not only about the types of foods consumed but also about when and how those foods are eaten. Meal timing and eating habits can strongly influence digestive function, intestinal motility, and symptom severity in individuals with irritable bowel syndrome. Many patients notice that symptoms such as bloating, abdominal pain, and changes in bowel movements are closely related to their eating patterns.
Digestive physiology follows a coordinated rhythm involving stomach emptying, intestinal contractions, and hormonal signaling. Disruptions in these rhythms, such as irregular meals or large food portions, can trigger abnormal gut responses in IBS patients [7]. Because the digestive tract in IBS is often more sensitive to stimulation, even small changes in meal timing or eating behavior can affect symptom intensity.
Large Meals and Gut Motility
Consuming very large meals can place significant stress on the digestive system. When a large amount of food enters the stomach, it stimulates strong digestive reflexes that increase intestinal motility. In individuals with IBS, these exaggerated contractions can trigger abdominal cramping, urgency, or diarrhea.
Large meals may also increase the production of digestive hormones that stimulate bowel movement, particularly in patients with diarrhea-predominant IBS. For this reason, many dietary guidelines recommend dividing daily food intake into smaller, more frequent meals rather than consuming two or three large meals per day.
Smaller meal portions reduce the burden on the digestive system and may help stabilize intestinal motility. This strategy can be an important component of an effective IBS diet, particularly for patients who experience symptoms shortly after eating.
Irregular Meal Timing
Irregular eating schedules can also influence digestive stability. The gastrointestinal tract follows a circadian rhythm that regulates gastric emptying, intestinal contractions, and hormone secretion. When meals occur at unpredictable times, this rhythm can become disrupted, leading to irregular bowel function.
Patients who skip meals, eat very late at night, or frequently change their eating schedule may experience worsening IBS symptoms. Maintaining a consistent daily meal pattern helps the digestive system anticipate food intake and regulate digestive processes more efficiently [9].
Establishing regular meal timing can therefore support digestive rhythm and reduce sudden changes in intestinal motility.
Stress and Eating Speed
Another important factor in IBS eating habits is the speed at which meals are consumed. Eating too quickly can increase the amount of air swallowed during meals, which may contribute to bloating and abdominal distension. Rapid eating can also reduce proper chewing of food, making digestion more difficult.
Stress during meals can further influence digestive function through the gut–brain axis. Emotional stress activates the autonomic nervous system, which may alter intestinal motility and increase gut sensitivity. In IBS patients, this stress response may amplify digestive symptoms after meals [9].
Adopting slower, more mindful eating habits may therefore help improve digestion and reduce symptom triggers. Taking time to chew food thoroughly, eating in a relaxed environment, and maintaining consistent meal schedules are simple behavioral strategies that can support a balanced IBS diet.
Ayurvedic Perspective on Diet and IBS

Understanding the IBS diet from an Ayurvedic perspective requires examining the classical concept of Grahani, the digestive organ governed by the strength of Agni (digestive fire). In Ayurveda, disorders resembling modern irritable bowel syndrome are commonly explained through disturbances of Grahani and impaired digestive metabolism. Classical Ayurvedic texts repeatedly emphasize that when digestive fire becomes weak or unstable, the digestive system cannot properly process food, resulting in irregular bowel movements, bloating, abdominal discomfort, and alternating diarrhea and constipation.
These classical explanations closely resemble the symptom pattern described in modern gastroenterology for IBS, where altered intestinal motility, microbial fermentation, and digestive sensitivity contribute to chronic digestive symptoms.
Grahani and Digestive Fire
Ayurveda describes Grahani as the organ responsible for retaining food until it is properly digested and releasing it once digestion is complete. When Agni is strong, digestion occurs normally and nutrients are absorbed efficiently. When Agni becomes weakened, Grahani loses its ability to regulate digestion properly.
This concept is described in Charaka Samhita, Chikitsa Sthana, Chapter 15 (Grahani Chikitsa):
“अग्निमन्द्याद् भवेद् रोगो ग्रहन्याख्यो विशेषतः।
अजीर्णं दीर्घकालं च दोषानां च प्रवृद्धता॥”
Transliteration
Agnimandyad bhaved rogo grahanyakhyo visheshatah
Ajirnam dirghakalam cha doshanam cha pravriddhata
English Translation
“When digestive fire becomes weakened, a disorder known as Grahani develops. This leads to chronic indigestion and aggravation of the doshas.”
Reference
Charaka Samhita, Chikitsa Sthana, Chapter 15, Verse 44–45.
This verse explains that digestive weakness is the fundamental cause of Grahani disorders. In modern clinical terms, this parallels impaired digestion, altered gut motility, and microbial fermentation that contribute to IBS symptoms.
Agni and Food Digestion
The role of Agni in digestion is a central principle in Ayurvedic physiology. Agni represents the metabolic force responsible for transforming food into absorbable nutrients and energy. When Agni functions normally, digestion remains stable and the gastrointestinal system maintains proper rhythm.
This principle is described in Charaka Samhita, Sutra Sthana, Chapter 27:
“रोगाः सर्वेऽपि मन्देऽग्नौ।”
Transliteration
Rogah sarve api mande agnau
English Translation
“All diseases arise when digestive fire becomes weakened.”
Reference
Charaka Samhita, Sutra Sthana, Chapter 27, Verse 341.
This classical statement highlights the importance of digestive strength in maintaining overall health. From an IBS diet perspective, this concept implies that digestive capacity determines how well the body can process different foods. When Agni is weak, even normally healthy foods may produce gas, bloating, or irregular bowel movements.
Why Digestive Strength Matters More Than Food Elimination
Ayurveda emphasizes that the goal of dietary management is not only to remove triggering foods but also to restore digestive strength. Restricting multiple foods without correcting the underlying digestive imbalance may provide temporary symptom relief but does not restore long-term digestive stability.
This principle is explained in Ashtanga Hridaya, Nidana Sthana, Chapter 8:
“दोषैः प्रदूषिता ग्रहनिः भोजनं न पचत्यलम्।”
Transliteration
Doshaih pradushita grahanih bhojanam na pachatyalam
English Translation
“When Grahani becomes disturbed by aggravated doshas, it loses the ability to properly digest food.”
Reference
Ashtanga Hridaya, Nidana Sthana, Chapter 8, Verse 1.
This verse highlights that digestive disorders occur when Grahani loses its functional capacity due to imbalance in digestive fire and doshas. In modern understanding, this resembles impaired digestion, abnormal gut motility, and intestinal hypersensitivity.
For this reason, Ayurvedic dietary guidance focuses on strengthening digestive fire through appropriate diet, balanced meal timing, and digestive-supporting foods rather than relying solely on restrictive elimination diets. When digestive capacity improves, the body becomes better able to tolerate a wider range of foods without triggering symptoms.
Why Diet Alone Often Fails to Resolve IBS
Many people initially focus on improving the IBS diet when trying to control symptoms such as bloating, abdominal pain, diarrhea, or constipation. While dietary adjustments can reduce symptom triggers for many patients, diet alone often does not completely resolve irritable bowel syndrome. This is because IBS is a complex condition influenced by multiple physiological systems within the body.
Research increasingly shows that IBS involves interactions between gut microbes, intestinal nerves, immune responses, and hormonal signaling pathways [1]. Because of this multifactorial nature, simply eliminating certain foods may reduce symptoms temporarily but may not address the deeper mechanisms contributing to the disorder.
Gut Microbiome Imbalance
One major factor involved in IBS is disruption of the gut microbiome. The digestive tract contains a large ecosystem of microorganisms that help regulate digestion, immune function, and intestinal barrier integrity. In many individuals with IBS, this microbial balance becomes altered.
Changes in microbial composition may lead to increased gas production, abnormal fermentation of carbohydrates, and greater sensitivity of the intestinal lining. These microbial changes can persist even when dietary triggers are removed, which explains why some patients continue to experience symptoms despite strict dietary control [8].
When the microbiome remains imbalanced, digestive discomfort may continue even with a carefully managed IBS diet.
Nervous System Dysregulation
Another important contributor to IBS is dysfunction of the gut–brain axis. The digestive tract contains an extensive network of nerves known as the enteric nervous system, which communicates continuously with the central nervous system.
In IBS patients, this communication network may become dysregulated, leading to heightened sensitivity of intestinal nerves. As a result, normal digestive processes such as intestinal contractions or gas movement can produce pain or discomfort [9].
Because this nerve sensitivity originates from the interaction between the brain and the digestive system, dietary changes alone may not fully normalize this neural response.
Hormonal Influence
Hormonal signaling also plays an important role in digestive function. Hormones regulate gastric emptying, intestinal motility, and fluid secretion within the digestive tract. Fluctuations in these signals can influence IBS symptoms.
For example, many patients notice changes in digestive symptoms during periods of stress or hormonal shifts. In women, IBS symptoms may fluctuate during the menstrual cycle due to hormonal changes that influence intestinal motility and sensitivity [7].
These hormonal influences demonstrate that IBS symptoms are not determined solely by dietary triggers.
Chronic Low-Grade Inflammation
Some studies suggest that a subset of IBS patients may experience low-grade inflammation within the intestinal lining. This mild inflammatory response can alter gut permeability, immune signaling, and nerve sensitivity.
Even when food triggers are removed from the IBS diet, this inflammatory environment may continue to stimulate intestinal discomfort and irregular bowel function [1].
Because inflammation may persist independently of dietary intake, symptom relief may require broader strategies beyond simple dietary elimination.
Understanding the Limits of Diet in IBS
Dietary management remains an important tool for reducing symptom triggers and improving digestive comfort. However, the presence of microbiome imbalance, nervous system dysregulation, hormonal influences, and low-grade inflammation means that IBS often requires a more comprehensive approach.
Recognizing that diet alone may not fully resolve IBS symptoms helps patients move beyond endless food restriction and toward strategies that address the deeper physiological mechanisms involved in digestive health. This understanding often marks an important turning point in the management of irritable bowel syndrome.
Signs Your IBS May Require Deeper Treatment
For many individuals, adjusting the IBS diet can reduce symptoms such as bloating, abdominal discomfort, and irregular bowel movements. However, some patients continue to experience persistent digestive problems despite carefully following dietary recommendations. In these situations, the ongoing symptoms may indicate that deeper digestive imbalances are present and that dietary changes alone may not fully resolve the condition.
Research suggests that irritable bowel syndrome often involves multiple physiological mechanisms, including altered gut motility, microbiome imbalance, intestinal hypersensitivity, and dysregulation of the gut–brain axis [1]. When these underlying factors remain unaddressed, symptoms may continue even when patients avoid known dietary triggers.
Symptoms Lasting for Many Years
One of the most common indicators that IBS may require a broader treatment approach is the persistence of symptoms over long periods of time. Many patients report experiencing digestive discomfort, bloating, constipation, or diarrhea for several years despite trying multiple dietary strategies.
When symptoms persist for such extended durations, it often suggests that the digestive system has developed chronic functional changes that cannot be corrected through diet alone. Long-standing IBS symptoms may involve deeper disturbances in intestinal motility, nerve signaling, and microbial balance.
Normal Medical Tests but Persistent Symptoms
Another frustrating situation for many IBS patients occurs when medical tests repeatedly return normal results, yet symptoms continue. Blood tests, colonoscopy, and imaging studies are frequently performed to rule out inflammatory bowel disease, infections, or structural abnormalities.
In IBS, these tests often appear normal because the disorder primarily affects the functional behavior of the digestive tract rather than producing visible structural damage. As a result, patients may continue experiencing symptoms even though standard diagnostic evaluations show no obvious abnormalities [7].
Repeated Diet Failures
Many individuals with IBS try several dietary strategies in an attempt to control their symptoms. These may include eliminating dairy products, following a low-FODMAP diet, avoiding gluten-containing foods, or increasing fiber intake.
While these approaches may provide temporary improvement, some patients find that symptoms eventually return despite strict dietary adherence. Repeated failure of dietary strategies can indicate that deeper factors such as microbial imbalance, nervous system dysregulation, or chronic digestive dysfunction may be contributing to ongoing symptoms.
Frequent Symptom Relapse
Another sign that IBS may require broader management is the pattern of recurring symptom flare-ups. Patients often describe periods where symptoms improve for a short time, followed by sudden relapse after stress, dietary changes, illness, or travel.
This cycle of improvement and relapse suggests that the digestive system may still be unstable. Even when trigger foods are avoided, underlying digestive sensitivity may remain, allowing symptoms to return repeatedly.
Recognizing these patterns can help patients understand when it may be appropriate to explore more comprehensive treatment strategies. When symptoms persist despite careful dietary management, broader approaches that address digestive function, microbiome balance, and nervous system regulation may become necessary.
This is where broader digestive treatment approaches become important. These are explained in detail in our article on IBS Ayurvedic Treatment: Diagnosis, Symptoms, and Cure which explores integrative strategies designed to support long-term digestive stability.
Reference
[1] Ford, A. C., Lacy, B. E., Talley, N. J. (2017). Irritable bowel syndrome. New England Journal of Medicine, 376(26), 2566–2578.
https://doi.org/10.1056/NEJMra1607547
This comprehensive review from the New England Journal of Medicine explains the pathophysiology, diagnosis, and treatment of IBS. It confirms that IBS affects roughly 10–15% of the global population and highlights how dietary triggers, gut-brain signaling, and microbiome changes influence symptoms. It supports the article sections on IBS overview and why diet influences IBS.
[2] Lacy, B. E., Mearin, F., Chang, L., et al. (2016). Bowel disorders. Gastroenterology, 150(6), 1393–1407.
https://doi.org/10.1053/j.gastro.2016.02.031
This publication outlines the Rome IV diagnostic criteria for IBS, which are the global standard for diagnosing functional bowel disorders. It explains symptom patterns such as abdominal pain associated with bowel movements and supports sections describing IBS classification and clinical presentation.
[3] Halmos, E. P., Power, V. A., Shepherd, S. J., Gibson, P. R., Muir, J. G. (2014). A diet low in FODMAPs reduces symptoms of irritable bowel syndrome. Gastroenterology, 146(1), 67–75.
https://doi.org/10.1053/j.gastro.2013.09.046
This landmark randomized controlled trial demonstrated that a low-FODMAP diet significantly reduces IBS symptoms compared with a typical Western diet. It provides scientific evidence for dietary fermentation as a trigger for IBS symptoms and supports the sections discussing FODMAP foods and IBS diet strategies.
[4] Gibson, P. R., Shepherd, S. J. (2010). Evidence-based dietary management of functional gastrointestinal symptoms: The FODMAP approach. Journal of Gastroenterology and Hepatology, 25(2), 252–258.
https://doi.org/10.1111/j.1440-1746.2009.06149.x
This influential paper introduced the concept of FODMAP carbohydrates as triggers of IBS symptoms. It explains how poorly absorbed carbohydrates ferment in the colon, producing gas and bloating. It supports the sections explaining how diet affects IBS physiology.
[5] Staudacher, H. M., Whelan, K. (2017). The low FODMAP diet: Recent advances in understanding its mechanisms and efficacy in IBS. Gut, 66(8), 1517–1527.
https://doi.org/10.1136/gutjnl-2017-313750
This review examines how the low-FODMAP diet improves IBS symptoms and how dietary restriction affects gut microbiota composition. It provides evidence for the benefits and limitations of long-term FODMAP restriction and supports sections discussing diet personalization.
[6] McKenzie, Y. A., Bowyer, R. K., Leach, H., et al. (2016). British Dietetic Association systematic review and evidence-based practice guidelines for the dietary management of IBS in adults. Journal of Human Nutrition and Dietetics, 29(5), 549–575.
https://doi.org/10.1111/jhn.12385
This guideline summarizes dietary interventions used for IBS management and recommends structured dietary strategies such as the low-FODMAP diet. It supports sections describing foods to eat, foods to avoid, and diet planning.
[7] Moayyedi, P., Andrews, C. N., MacQueen, G., et al. (2019). Canadian Association of Gastroenterology clinical practice guideline for the management of IBS. Journal of the Canadian Association of Gastroenterology, 2(1), 6–29.
https://doi.org/10.1093/jcag/gwy071
This clinical guideline evaluates treatment strategies for IBS, including dietary management, probiotics, and pharmacological therapies. It supports sections discussing when diet alone may not be sufficient for IBS treatment.
[8] Simrén, M., Barbara, G., Flint, H. J., et al. (2013). Intestinal microbiota in functional bowel disorders. Gut, 62(1), 159–176.
https://doi.org/10.1136/gutjnl-2012-302167
This study explains the role of gut microbiota in IBS and how fermentation of certain carbohydrates can influence symptom severity. It supports sections describing fermentation, gas production, and microbiome influences on IBS symptoms.
[9] Mayer, E. A., Savidge, T., Shulman, R. J. (2014). Brain–gut microbiome interactions and functional bowel disorders. Gastroenterology, 146(6), 1500–1512.
https://doi.org/10.1053/j.gastro.2014.02.037
This paper explains the gut-brain axis and how stress, nervous system signaling, and microbiome interactions affect IBS symptoms. It supports sections discussing stress, nervous system regulation, and why IBS symptoms vary between individuals.
[10] Charaka Samhita. Chikitsa Sthana, Chapter 15 (Grahani Chikitsa), verses 44–60. Classical Ayurvedic text on digestive disorders.
https://archive.org/details/CharakaSamhitaEnglishTranslation
This classical Ayurvedic medical text describes Grahani, a condition involving impaired digestion and intestinal dysfunction. The text explains the importance of digestive fire (Agni) and diet regulation in managing chronic digestive disorders. It supports the Ayurvedic perspective section of the article.
Note: Every reference listed here has been carefully selected for accuracy, clinical relevance, and traceability. Ayurvedic formulations are cited directly from classical medical texts such as Charaka Samhita along with specific chapter references. All modern scientific studies are provided with active hyperlinks in APA format. This dual validation ensures the highest integrity of information for patients, practitioners, and researchers. If you find any reference missing or wish to request full-text access for a particular citation, you may contact the author directly. Our goal is to maintain complete transparency and academic rigor.