- The Silent Nature of Herpes in Women
- How Common Is Asymptomatic Herpes in Women
- Why Women Often Do Not Notice Herpes Symptoms
- Estrogen and the Female Immune System
- Menstrual Cycle and Herpes Activity
- Internal Lesions That Women May Never See
- Why Herpes Testing Often Confuses Women
- Asymptomatic Viral Shedding
- Psychological Impact of Unexpected Diagnosis
- Why Many Women Discover Herpes During Fertility or Pregnancy Testing
- Ayurvedic Perspective on Silent Viral Infection
- When Women Should Seek Medical Evaluation
- Can Silent Herpes Infection Be Eliminated
- Key Facts Women Should Know About Silent Herpes Infection
- FAQ
- Reference
The Silent Nature of Herpes in Women
Many women are surprised to learn that they can carry herpes without symptoms for months or even years. The question of why women carry herpes without symptoms has become increasingly common among patients in the USA and UK, especially after routine blood tests reveal HSV antibodies despite the absence of visible sores. This silent pattern of infection is not unusual. In fact, modern epidemiological studies show that a large proportion of herpes infections in women remain unnoticed because the virus can stay dormant in nerve tissues while producing minimal or no outward signs of disease [2].
Many people are surprised to learn that herpes infection can remain silent for years. The virus often stays hidden in nerve cells and may not produce visible symptoms. A detailed explanation of diagnosis, transmission patterns, and treatment approaches is discussed in our comprehensive guide on Herpes Ayurvedic Treatment: Diagnosis, Symptoms, and Long-Term Viral Elimination
One of the reasons why women carry herpes without symptoms is that herpes viruses have a natural ability to establish latency in sensory nerve ganglia. After the initial exposure, the virus travels along peripheral nerves and hides in structures such as the sacral or trigeminal ganglia depending on the type of infection. During this phase, the virus may remain inactive for long periods while the immune system keeps viral replication under control. Because of this biological behavior, many infected individuals never develop the classic blister outbreaks that are typically associated with herpes infections [6].
Another factor explaining why women carry herpes without symptoms is the subtle nature of genital symptoms in female anatomy. Lesions can appear internally on the cervix, vaginal walls, or other mucosal surfaces that are not easily visible without clinical examination. These mild or hidden lesions may cause minimal discomfort and therefore go unnoticed. As a result, many women discover their infection only through blood testing during fertility evaluation, pregnancy screening, or routine sexual health assessments [5].
Understanding why women carry herpes without symptoms is important for both patients and clinicians. Silent infections contribute significantly to unintentional transmission because individuals who feel healthy may not realize they carry the virus. For this reason, public health authorities emphasize awareness, testing when risk factors exist, and open communication between partners. Recognizing the silent nature of herpes infection helps reduce stigma while encouraging informed health decisions and early evaluation when needed [2].
In clinical practice, this silent behavior explains why herpes is often described as a “hidden infection.” The virus may remain dormant for years before any noticeable outbreak occurs, and in some cases symptoms may never develop at all. This biological characteristic is the central reason why women carry herpes without symptoms, making education and awareness a critical component of responsible sexual health management [6].
How Common Is Asymptomatic Herpes in Women

Understanding why women carry herpes without symptoms requires first examining how common silent infections actually are. Epidemiological research consistently shows that most people infected with herpes simplex virus are unaware of their infection. In women, this phenomenon is even more frequent because genital symptoms may be mild, internal, or easily mistaken for other conditions. As a result, many women live with herpes for years without recognizing any visible signs of the virus [2].
Global public health data indicate that herpes infections are extremely widespread. The World Health Organization estimates that hundreds of millions of people worldwide carry herpes simplex virus type 2, the strain most commonly associated with genital herpes. However, only a minority of infected individuals report classic outbreaks. A large portion of women with HSV infection experience either very mild symptoms or no symptoms at all, which explains why routine screening sometimes reveals herpes antibodies in patients who have never noticed lesions [1].
Research studies examining sexual health clinics and population surveys have demonstrated that asymptomatic infection may account for the majority of herpes cases. In many cohorts, more than half of people who test positive for HSV-2 report no prior diagnosis or recognizable outbreaks. This pattern highlights an important aspect of why women carry herpes without symptoms, namely that the virus can remain biologically active in nerve tissues without producing noticeable lesions on the skin or mucosal surfaces [6].
Another reason silent infection is common in women relates to the anatomical structure of the female genital tract. Lesions may occur internally on the cervix or vaginal walls, areas that cannot be easily seen without a clinical examination. When symptoms do occur, they may present as mild irritation, itching, or small fissures that are mistaken for yeast infections or minor skin irritation. Because these symptoms are subtle, they often go unrecognized as herpes [2].
Public health experts therefore emphasize that herpes should not be viewed only as a disease characterized by visible blisters. In reality, asymptomatic infection represents a large portion of global HSV transmission. This is why awareness campaigns often highlight that a person can feel completely healthy while still carrying and potentially transmitting the virus. Understanding this silent epidemiology is a key step in explaining why women carry herpes without symptoms and why testing and education remain essential parts of sexual health care [1].
Why Women Often Do Not Notice Herpes Symptoms
One of the major reasons behind why women carry herpes without symptoms lies in the anatomical differences between male and female genital structures. Female reproductive anatomy includes internal mucosal surfaces such as the vaginal canal, cervix, and upper genital tract. When herpes lesions develop in these internal areas, they may not be easily visible or noticeable without a clinical examination. Because of this, many women experience infections that remain unnoticed or are mistaken for other minor gynecological conditions [1].
Herpes simplex virus infects epithelial tissues and mucous membranes. In women, these tissues extend deeper into the reproductive tract compared with men. Small lesions or fissures may appear inside the vagina or on the cervix where they produce minimal discomfort. Unlike external lesions that are easily seen on the skin, these internal lesions may heal quickly or cause only mild irritation. This biological characteristic contributes significantly to why women carry herpes without symptoms, as the infection can remain active without producing obvious visible signs [5].
Another factor explaining why women carry herpes without symptoms is that the early symptoms of genital herpes in women often resemble common gynecological conditions. Mild itching, slight vaginal discomfort, or a small amount of discharge may be attributed to yeast infections, bacterial imbalance, or minor irritation. Because these symptoms overlap with several routine reproductive health conditions, herpes infections may remain undiagnosed unless specific laboratory testing is performed [1].
Medical research has also shown that many first herpes infections in women are clinically subtle. The immune system may suppress viral replication quickly, resulting in very mild outbreaks that resolve before they are clearly recognized. In such cases, the virus still establishes latency in nearby nerve ganglia while the individual remains unaware of the infection. This pattern is a key biological explanation for why women carry herpes without symptoms, particularly during the early stages of infection [5].
These anatomical and physiological factors together make asymptomatic herpes more common in women than many people realize. Understanding these differences helps clinicians explain why many women only discover their infection through blood tests during routine health screening, pregnancy evaluation, or fertility investigations. Recognizing this silent presentation is essential for improving awareness and encouraging appropriate testing when risk factors are present [1].
Mild or Misidentified Symptoms
Another important reason why women carry herpes without symptoms is that the early signs of infection are often extremely mild or easily confused with other common gynecological conditions. Many women expect herpes to always cause painful blisters or obvious sores, but in reality the virus frequently produces subtle symptoms that may not immediately appear serious. Because these signs are mild, they may be ignored or attributed to routine irritation, hormonal changes, or minor infections [6].
In clinical practice, the initial symptoms of genital herpes in women can include slight itching, mild burning during urination, minor redness, or small fissures in the genital area. These symptoms may last only a short time and may resolve quickly without treatment. Since these sensations overlap with common conditions such as yeast infections, contact irritation, or bacterial imbalance, many women do not recognize them as herpes-related symptoms [5].
Another factor contributing to why women carry herpes without symptoms is that outbreaks may occur internally on mucosal surfaces where lesions are difficult to see. When lesions are located inside the vaginal canal or near the cervix, they may cause only mild discomfort or discharge rather than visible blisters. Because these internal symptoms are subtle, they may go unnoticed unless a medical examination is performed [6].
Misinterpretation of symptoms also plays a role. Many women treat mild irritation with over-the-counter antifungal medications or assume the discomfort is related to routine vaginal infections. When symptoms disappear quickly, the underlying viral infection remains undetected. This pattern of mild symptoms followed by rapid healing is another explanation for why women carry herpes without symptoms, particularly during early or infrequent outbreaks [5].
Medical research therefore shows that herpes infections often present in ways that differ from the dramatic descriptions commonly associated with the disease. Instead of severe lesions, many women experience small, short-lived symptoms that resemble other minor conditions. Because of this, herpes infections may remain unnoticed for long periods until laboratory testing reveals the presence of HSV antibodies [6].
Estrogen and the Female Immune System

Estrogen Immune Interaction
Hormonal physiology plays a major role in how the female body responds to viral infections in the reproductive tract. One of the most influential hormones is estrogen, particularly its biologically active form estradiol. This hormone regulates several immune mechanisms within the genital tract, including antiviral defense, mucosal barrier protection, and inflammatory signaling. Because estrogen directly affects how immune cells react to pathogens, it can influence the clinical expression of herpes simplex virus infections [8].
Scientific studies show that estradiol can modify susceptibility to viral infections in the genital tissues. When estrogen levels are higher, the epithelial lining of the vagina and cervix becomes thicker and produces protective secretions that strengthen the mucosal barrier. These physiological changes help protect the reproductive tract from pathogens and may reduce the severity of visible symptoms even when viral exposure occurs. In many cases, the immune system suppresses viral replication early, preventing the development of prominent lesions [3].
This hormonal influence also affects how herpes infections progress within the body. The immune system may control viral activity effectively, allowing the virus to remain in a low-level or latent state within sensory nerve ganglia. During this stage, individuals may experience minimal or no outward symptoms because the immune response prevents extensive inflammation in the infected tissues [8].
Hormonal Immune Modulation
Hormonal fluctuations throughout the menstrual cycle further influence immune responses within the female reproductive tract. Estrogen and progesterone levels change during different phases of the cycle, and these hormonal shifts affect immune cell activity, cytokine production, and antibody responses in the genital mucosa [9].
The female reproductive tract has a unique immune environment designed to balance protection against pathogens while preserving reproductive function. This immune balance sometimes leads to a moderated inflammatory response rather than an aggressive reaction. Because visible symptoms such as redness, swelling, and pain are typically caused by inflammation, a controlled immune response may result in mild or barely noticeable clinical signs despite the presence of viral infection [8].
Hormonal immune modulation therefore plays a critical role in shaping how viral infections manifest in women. At certain stages of the menstrual cycle, immune defenses within the genital mucosa may suppress viral activity effectively enough that outbreaks remain subtle or transient. The virus may still establish latency within nerve tissues, but outward symptoms may be minimal or easily overlooked [9].
Menstrual Cycle and Herpes Activity
Hormonal Fluctuations
The menstrual cycle creates continuous hormonal changes within the female body, particularly involving estrogen and progesterone. These fluctuations influence multiple biological systems, including immune function, mucosal protection, and inflammatory responses within the reproductive tract. Because viral infections are strongly influenced by immune activity, hormonal variation throughout the menstrual cycle can affect how viral infections behave within the body [8].
During different phases of the cycle, the immune environment of the genital tract changes. Estrogen levels rise during the follicular phase and decline before menstruation, while progesterone increases after ovulation. These hormonal shifts can alter the activity of immune cells and cytokines within the mucosal tissues of the reproductive tract. As a result, the body’s ability to suppress viral replication may vary at different points in the cycle [3].
Research has shown that certain hormonal phases may influence viral reactivation patterns. When hormone levels decline or immune activity becomes temporarily reduced, latent viruses within nerve ganglia may reactivate more easily. This phenomenon explains why some women notice periodic symptom flare-ups that appear to correspond with particular stages of the menstrual cycle [8].
Why Symptoms Sometimes Appear Around Menstruation
Many women report that symptoms become more noticeable shortly before or during menstruation. This observation is supported by research examining hormonal influence on genital tract immunity. The period leading up to menstruation involves a drop in estrogen and progesterone levels, which can temporarily reduce immune protection within the genital mucosa. When immune defenses decrease, viral activity may increase slightly, sometimes producing mild symptoms or localized irritation [5].
Another contributing factor involves changes in tissue sensitivity and inflammation during menstruation. Hormonal shifts can increase blood flow, alter the vaginal environment, and modify inflammatory responses within reproductive tissues. These physiological changes may make minor symptoms more noticeable even when viral activity remains relatively low [8].
It is also important to recognize that the relationship between the menstrual cycle and viral symptoms varies between individuals. Some women may experience periodic symptoms associated with hormonal fluctuations, while others may not notice any clear pattern. This variation reflects the complex interaction between hormones, immune responses, and viral latency within nerve tissues [5].
Internal Lesions That Women May Never See
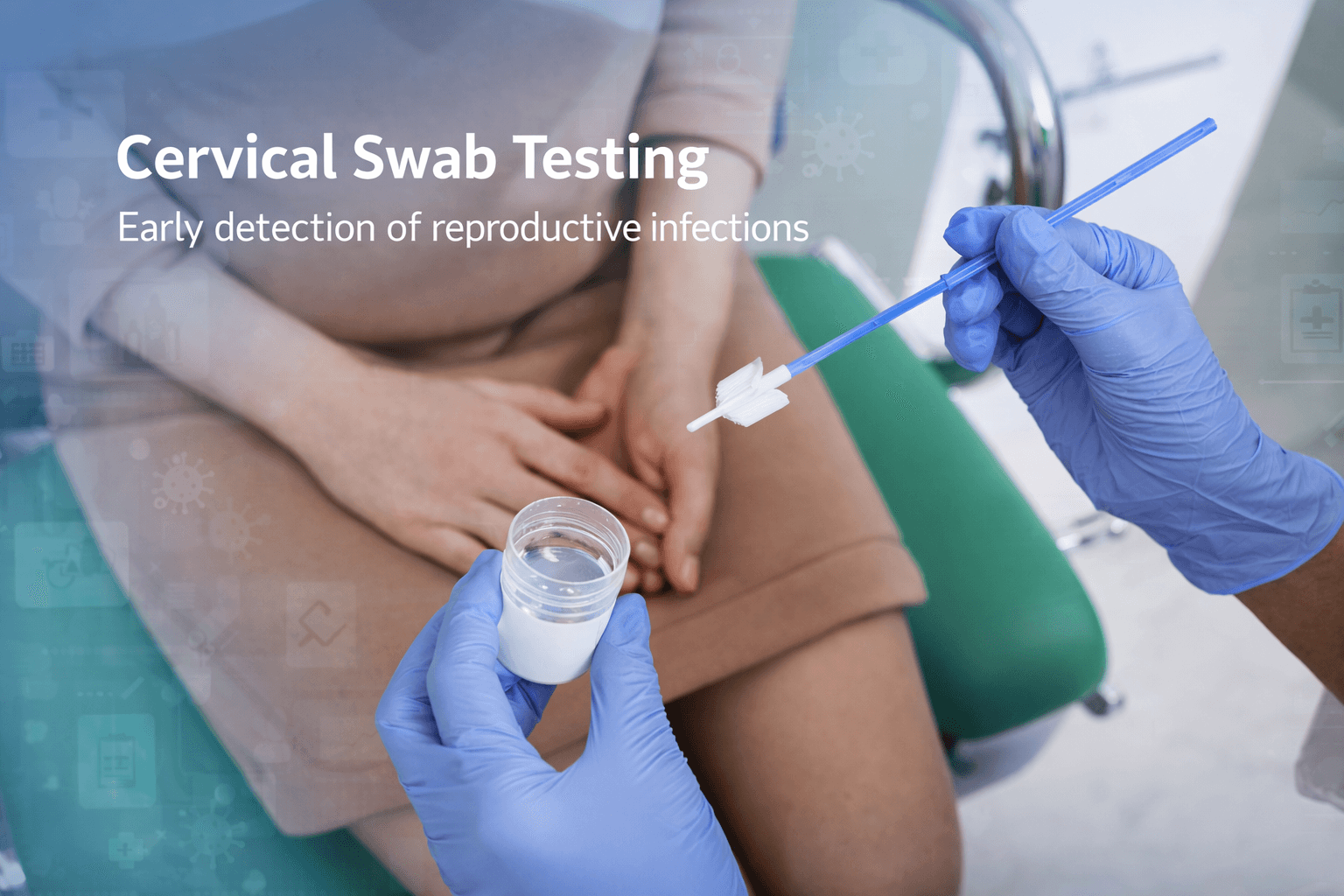
Hidden Location of Cervical and Vaginal Lesions
One of the most clinically important characteristics of genital herpes infection in women is that lesions may develop in anatomical areas that are not easily visible. The female reproductive tract includes internal mucosal structures such as the vaginal canal and cervix, where viral lesions can form without being immediately noticeable to the patient. Unlike external skin lesions that appear on visible areas of the body, internal genital lesions may remain hidden unless they are identified during a medical examination [1].
Herpes simplex virus primarily infects epithelial cells and mucosal tissues. In women, these tissues extend deeper into the reproductive tract compared with men. When the virus infects the cervix or upper vaginal walls, lesions may appear as small ulcers, fissures, or inflamed patches within the mucosal lining. Because these areas are not visible during routine self-observation, such lesions may go completely unnoticed [5].
Clinical gynecological examinations sometimes reveal cervical herpes lesions in patients who did not report typical symptoms. In these cases, the lesions may appear as small erythematous areas, shallow ulcerations, or localized mucosal inflammation. These findings demonstrate that viral activity can occur internally without producing the classic external blisters often associated with herpes infections [1].
Subtle Symptoms From Internal Lesions
When lesions occur inside the vagina or on the cervix, the symptoms they produce are often mild and nonspecific. Patients may experience slight vaginal discomfort, mild irritation, or an increase in vaginal discharge. These symptoms are common in many gynecological conditions, which makes it difficult to immediately recognize a viral cause [5].
In some cases, the only symptom may be minor pelvic discomfort or a transient burning sensation during urination. Because these symptoms overlap with urinary tract irritation or common vaginal infections, the underlying viral infection may not be suspected. As a result, internal herpes lesions may heal before the patient seeks medical evaluation [1].
The cervix in particular can host viral lesions that produce very subtle symptoms. Cervical mucosa contains fewer pain-sensitive nerve endings compared with external genital skin, which means inflammatory changes may produce minimal pain. This anatomical feature allows lesions to persist without causing the level of discomfort typically associated with visible genital sores [5].
Clinical Detection During Medical Examination
In many situations, internal herpes lesions are discovered only during a clinical gynecological examination. Physicians may identify suspicious lesions while performing pelvic examinations, Pap tests, or diagnostic procedures evaluating reproductive health. When visible abnormalities are detected, laboratory testing such as viral PCR or culture can confirm the presence of herpes simplex virus [1].
Modern diagnostic techniques have shown that internal genital herpes lesions may be more common than previously recognized. Advances in molecular testing allow clinicians to detect viral DNA even when visible lesions are minimal or absent. These diagnostic methods help explain why some individuals receive positive herpes test results despite never having observed classic outbreaks [5].
Clinical Significance of Internal HSV Lesions
The presence of internal lesions has important implications for clinical diagnosis and patient awareness. Because these lesions may not produce obvious symptoms, infections can remain undetected for extended periods. Individuals may only learn about the infection during routine screening, pregnancy testing, or fertility evaluations [1].
Understanding the possibility of hidden lesions also helps clinicians interpret unusual symptom patterns. When patients report mild irritation or unexplained genital discomfort, healthcare providers may consider viral infections as part of the differential diagnosis. Awareness of internal lesion patterns improves the likelihood of early identification and appropriate diagnostic testing [5].
The ability of herpes simplex virus to infect both external skin and internal mucosal tissues highlights the complexity of genital infections. Internal lesions represent an important clinical feature of the disease and demonstrate why visible symptoms alone cannot always determine whether infection is present. Careful medical evaluation and appropriate laboratory testing remain essential for accurate diagnosis and patient counseling [1].
Why Herpes Testing Often Confuses Women

Herpes diagnosis is often far more complicated than many women expect. In clinical practice, it is common for patients to receive test results that appear contradictory or difficult to interpret. Some women test positive despite never experiencing visible symptoms, while others have recurring genital discomfort but receive negative laboratory reports. These situations frequently lead to confusion, anxiety, and unnecessary fear about long-term health or fertility. The complexity arises primarily because herpes testing methods detect different biological markers of infection, and each test has specific limitations. Understanding how these tests work helps explain why many women struggle to interpret their results correctly.
Many patients discover herpes during routine blood tests even when they never experienced symptoms. If you want to understand how testing works and what different results mean, you can read our detailed guide on Herpes Ayurvedic Treatment: Diagnosis, Symptoms, and Long-Term Viral Elimination.
Blood Tests Detect Antibodies, Not the Virus
One of the most widely used diagnostic methods for herpes is the HSV IgG blood test. This test does not detect the herpes virus itself. Instead, it measures antibodies produced by the immune system after exposure to the virus. When a person becomes infected with herpes simplex virus, the immune system gradually produces IgG antibodies that remain in the body for life. These antibodies act as immunological memory, allowing the immune system to recognize the virus if it reactivates.
Because the test measures antibodies rather than the virus, the result only indicates that the immune system has encountered herpes at some point in the past. It cannot determine when the infection occurred, whether the virus is currently active, or where in the body the virus resides. For example, a person who had oral herpes in childhood may test positive decades later even if they never develop genital symptoms. This characteristic of antibody testing often leads to misunderstanding, as many patients interpret a positive result as evidence of a recent or severe infection.
Another limitation is the time required for antibodies to develop. After initial exposure to HSV, the immune system may take several weeks to months before producing detectable IgG antibodies. If testing occurs too early after infection, the result may appear negative even though the virus is already present in the body. For this reason, many diagnostic guidelines recommend repeat testing after an appropriate window period when clinical suspicion remains high.
Positive Test but No Symptoms
A particularly confusing situation occurs when women receive a positive herpes blood test but have never experienced visible lesions, blisters, or discomfort. This scenario is extremely common because herpes infections frequently remain asymptomatic or produce symptoms so mild that they go unnoticed. Many individuals carry the virus for years without recognizing any clear signs of infection.
Research shows that a large proportion of herpes infections are discovered incidentally through routine screening or unrelated medical testing. In such cases, the positive antibody result reflects prior exposure rather than active disease. The virus may remain dormant in nerve cells without causing outbreaks for long periods. Some individuals may never develop noticeable symptoms at all.
Another factor contributing to confusion is the difference between HSV-1 and HSV-2 antibodies. HSV-1 is extremely widespread globally and is often acquired during childhood through non-sexual contact such as kissing or sharing utensils. A positive HSV-1 antibody test therefore does not necessarily indicate genital herpes. However, many laboratory reports do not clearly explain this distinction, leading patients to assume the infection is sexually transmitted when it may simply reflect a common childhood exposure.
Diagnostic guidelines emphasize that laboratory results should always be interpreted in the context of clinical symptoms and patient history. A positive antibody test alone cannot determine the site of infection or whether the virus is currently causing disease. Physicians typically rely on direct viral testing of lesions, such as PCR swabs, when symptoms are present because these tests detect the actual viral genetic material rather than immune response markers.
For many women, the confusion surrounding herpes testing stems from the gap between laboratory science and everyday understanding. Blood tests provide valuable information about prior exposure, but they do not offer a complete picture of viral activity. Proper interpretation requires combining laboratory data with clinical examination and patient history to arrive at an accurate diagnosis.
Table: Why Herpes Infection Often Remains Unnoticed in Women
| Factor | Explanation | Why It Causes Diagnostic Confusion |
|---|---|---|
| Internal lesions | Herpes sores may develop inside the cervix or vaginal canal where they are not visible | Women may not notice symptoms because lesions are internal |
| Mild symptoms | Early outbreaks can resemble yeast infection, irritation, or ingrown hair | Symptoms may be ignored or treated as another condition |
| Asymptomatic viral shedding | The virus can reactivate without visible sores | Infection can spread even when no symptoms are present |
| Antibody blood testing | HSV blood tests detect past exposure rather than active infection | Positive results may appear even when no symptoms occurred |
| Hormonal influence | Hormonal changes affect immune responses in the genital tract | Symptoms may appear only occasionally or around menstrual cycles |
| Latent infection | HSV remains dormant inside nerve ganglia for long periods | Infection may remain undetected for years |

Herpes simplex virus has a unique biological behavior that makes it difficult to detect and control. One of the most important characteristics of the virus is asymptomatic viral shedding, a process in which the virus is released from the skin or mucous membranes without producing any visible symptoms. In other words, a person can carry and transmit the virus even when no blisters, ulcers, or irritation are present. This phenomenon explains why herpes often spreads unknowingly between partners and why many individuals become infected without recalling any obvious exposure event [4].
How Viral Shedding Occurs
After the initial infection, herpes simplex virus travels through sensory nerve endings and establishes lifelong latency inside nerve ganglia. During this dormant stage, the virus remains inactive within nerve cells. However, certain triggers can cause the virus to reactivate. When reactivation occurs, the virus travels along nerve pathways back to the skin or mucosal surface where it begins replicating again.
In some cases this reactivation leads to visible symptoms such as cold sores or genital blisters. In many other cases, however, the virus reaches the surface tissues and begins replicating without producing any noticeable lesions. During this silent replication phase, viral particles can still be released onto the skin surface. This is what clinicians describe as asymptomatic shedding, meaning the virus is actively present and capable of transmission even though the infected person feels completely normal [5].
Why Asymptomatic Shedding Is Common in Women
Clinical studies show that asymptomatic shedding occurs frequently in individuals with both HSV-1 and HSV-2 infections. Women may experience silent viral shedding from the cervix, vulva, or vaginal tissues without visible signs of irritation. Because the mucosal lining of the female reproductive tract provides an environment where the virus can replicate quietly, shedding episodes may occur without pain or discomfort.
This biological behavior is one of the main reasons many women test positive for herpes antibodies despite never noticing a typical outbreak. The virus may have been present for years while producing only microscopic viral release that goes completely unnoticed [3].
Why Routine Testing Often Misses It
Another factor contributing to confusion is that asymptomatic shedding is difficult to detect using routine medical testing. Blood tests measure antibodies rather than viral activity, and standard screening is usually performed only when symptoms are present. Because silent shedding episodes are temporary and unpredictable, they may occur between clinic visits or outside the time window of laboratory testing.
For this reason, even individuals who have never experienced visible herpes lesions can still carry the virus and occasionally shed it. Modern molecular diagnostic tools such as PCR testing can detect viral genetic material during active shedding, but these tests are typically used only when clinicians suspect active infection.
Why This Matters for Transmission
The concept of asymptomatic viral shedding has important implications for public health and patient education. Many people assume that herpes is contagious only when blisters are present. However, research shows that a significant proportion of transmission occurs during periods when infected individuals have no symptoms at all. This silent spread explains why herpes remains one of the most common viral infections worldwide.
Psychological Impact of Unexpected Diagnosis
Receiving a herpes diagnosis can have a profound emotional and psychological impact, especially when the diagnosis comes unexpectedly. Many women discover they are infected through routine blood tests, fertility evaluations, or screening performed for unrelated health concerns. Because herpes infections are often asymptomatic or produce only mild symptoms, a positive test result may feel shocking and difficult to understand. Patients frequently report feelings of confusion, anxiety, and distress immediately after learning about the diagnosis [6].
Emotional Reactions After Diagnosis
One of the most common reactions to an unexpected herpes diagnosis is emotional shock. Many women initially believe the result must be incorrect because they have never experienced visible sores or typical symptoms associated with the infection. This discrepancy between laboratory results and personal experience can create significant emotional turmoil. Individuals may question their past relationships, worry about future partnerships, and fear social stigma associated with sexually transmitted infections.
Psychological research shows that the emotional burden of herpes often arises not only from the infection itself but from the cultural stigma surrounding it. The virus is widely misunderstood, and many people incorrectly associate it with promiscuity or poor health habits. These misconceptions can lead patients to feel shame or embarrassment even though herpes is extremely common worldwide. As a result, some individuals delay discussing the condition with partners or healthcare providers, which can increase emotional stress [2].
Anxiety and Fear of Transmission
Another major psychological concern following diagnosis is the fear of transmitting the virus to a partner. Women who receive a positive test result often worry about unknowingly infecting someone they care about. Because herpes can spread during asymptomatic viral shedding, patients may feel uncertain about when transmission could occur. This uncertainty can lead to heightened anxiety during intimate relationships and may cause individuals to avoid sexual activity altogether.
In addition, women who are planning pregnancy may worry about potential risks to future children. Although neonatal herpes is rare and preventable with appropriate medical care, many patients are unaware of this information when they first receive their diagnosis. Without proper counseling, these fears can become overwhelming and may contribute to long-term psychological distress.
Importance of Education and Support
Accurate medical education plays a crucial role in reducing the psychological burden associated with herpes. When patients understand that the infection is common, manageable, and often asymptomatic, many of their initial fears begin to decrease. Healthcare professionals emphasize that millions of people worldwide live normal lives with herpes and maintain healthy relationships without major complications.
Supportive counseling can also help patients cope with the emotional impact of diagnosis. Open discussions with healthcare providers allow individuals to ask questions about transmission risk, treatment options, and long-term outlook. This information helps replace fear and uncertainty with knowledge and confidence.
For many women, the psychological distress associated with herpes gradually improves once they receive reliable information and emotional support. Understanding the biology of the virus, the nature of asymptomatic infections, and the effectiveness of preventive strategies can help patients regain a sense of control over their health and well-being.
Why Many Women Discover Herpes During Fertility or Pregnancy Testing
Many women first learn about a herpes infection during fertility evaluations or routine pregnancy screening. This discovery often occurs unexpectedly because the majority of herpes infections remain silent for long periods. Unlike many other viral illnesses that cause obvious symptoms soon after infection, herpes simplex virus can remain dormant in the body while producing minimal or no visible signs. As a result, women may carry the virus for years without realizing they are infected. When laboratory tests are performed during reproductive health assessments, previously unrecognized infections may suddenly appear in the test results [1].
Routine Screening During Fertility Evaluations
Fertility investigations frequently include comprehensive infectious disease screening to ensure the safety of both the patient and a future pregnancy. During these evaluations, physicians may request blood tests that detect antibodies against several viruses, including herpes simplex virus. The purpose of this screening is to identify infections that could influence reproductive health, pregnancy outcomes, or neonatal safety.
The most commonly used test is the HSV IgG antibody test, which measures whether the immune system has previously encountered the virus. Because antibodies remain in the body for life, this test can detect past exposure even if the infection occurred many years earlier. For women who have never experienced visible sores or genital symptoms, the discovery of positive antibodies can be surprising. Many patients assume that a viral infection must produce noticeable illness, but herpes often behaves differently by remaining clinically silent.
This situation is particularly common among women undergoing assisted reproductive procedures such as in vitro fertilization or other fertility treatments. These programs often require detailed infectious disease screening before treatment begins, which increases the likelihood that previously unnoticed viral infections will be detected.
Testing During Prenatal Care
Pregnancy care also includes a variety of laboratory tests designed to protect maternal and fetal health. Although routine prenatal screening may not always include herpes testing in every healthcare system, many physicians order herpes antibody tests when there is a history of genital symptoms, unexplained lesions, or concerns about possible exposure.
When herpes antibodies are detected during pregnancy testing, women may feel worried about potential risks to the baby. In reality, most women who already carry herpes before pregnancy deliver healthy infants without complications. The greatest risk of neonatal infection occurs when a woman acquires herpes for the first time late in pregnancy, not when the infection has been present for many years. Therefore, discovering a preexisting infection during prenatal testing often helps doctors plan appropriate monitoring and preventive strategies [6].
Silent Infections Are Common
The reason herpes frequently appears during fertility or pregnancy testing is that the infection often remains unnoticed for long periods. Many individuals experience mild symptoms that resemble minor skin irritation, ingrown hairs, or fungal infections rather than classic herpes lesions. These mild symptoms may resolve quickly and never receive medical evaluation. In other cases, the virus remains entirely asymptomatic while persisting quietly within nerve cells.
Because herpes simplex virus establishes lifelong latency in nerve ganglia, antibody tests can reveal exposure long after the initial infection occurred. The virus may have been acquired years earlier through oral contact, intimate relationships, or other forms of close skin contact. By the time fertility or pregnancy screening occurs, the infection may already be well established without ever producing obvious warning signs.
Importance of Clear Medical Counseling
Discovering herpes during fertility or prenatal testing can be emotionally challenging, particularly when patients did not expect the diagnosis. Clear medical counseling is therefore essential. Healthcare providers usually explain that antibody testing indicates previous exposure rather than active disease, and that many people carry the virus without symptoms. They also discuss preventive strategies that reduce transmission risk and ensure safe pregnancy outcomes.
Understanding the biology of herpes infection helps reduce unnecessary anxiety. For most women, the presence of herpes antibodies does not prevent successful fertility treatment or healthy pregnancy. Instead, early awareness allows doctors to monitor symptoms carefully and implement appropriate precautions when needed.
Ayurveda has long described disease processes that remain hidden within the body before producing visible symptoms. Classical Ayurvedic physicians understood that certain pathogens or disease-causing factors may stay dormant in tissues, gradually disturbing internal balance without immediately producing external signs. This concept closely parallels what modern medicine describes as latent or asymptomatic viral infections, where pathogens remain inactive for long periods and reactivate under specific conditions.
In the Ayurvedic framework, silent infections are primarily understood through the concepts of Krimi (microbial organisms), Dosha imbalance, Dhatu Dushti (tissue disturbance), and Srotas obstruction. When pathogenic factors enter the body but are not strong enough to produce immediate disease, they may remain in a dormant state within tissues. Over time, if the body’s defensive mechanisms weaken, these hidden factors can reactivate and manifest as visible illness.
Krimi Theory and Hidden Pathogens
Ancient Ayurvedic texts recognize microscopic organisms that may reside in the body and contribute to disease development. The term Krimi refers broadly to microorganisms, parasites, and subtle disease-causing entities that may inhabit different tissues.
Sanskrit Shloka
कृमयो बहवो देहे दृश्यादृश्याः प्रकीर्तिताः।
तेषां केचित् बहिर्भागे केचिदन्तः शरीरिणाम्॥
Transliteration
Krimayo bahavo dehe drishyadrishyah prakirtitah
Tesham kechit bahirbhage kechid antah sharirinam
Translation
Many types of organisms exist within the body, some visible and some invisible.
Some reside externally, while others live inside the human body.
Source
Charaka Samhita, Vimana Sthana, Chapter 7
This classical description acknowledges that certain disease-causing organisms may exist internally without producing obvious symptoms. The concept resembles modern understanding of viral latency, where pathogens remain hidden within tissues until conditions favor their reactivation.
Dormant Disease and Dosha Imbalance
Ayurveda explains that disease does not always appear immediately after exposure to pathogenic factors. Instead, the body may temporarily maintain balance despite the presence of harmful influences. When Doshas such as Vata, Pitta, and Kapha remain stable, disease manifestations may remain silent. However, when these regulatory forces become disturbed, dormant disease processes can become active.
Sanskrit Shloka
दोषा धातु मलमूलं हि शरीरम्।
Transliteration
Dosha dhatu mala mulam hi shariram
Translation
The body is sustained by the balanced interaction of Doshas, Dhatus, and Malas.
Source
Charaka Samhita, Sutra Sthana, Chapter 15
When these regulatory systems lose balance, pathogens that were previously dormant may begin to cause disease. In the context of viral infections, triggers such as stress, fatigue, hormonal changes, or immune suppression can disturb internal equilibrium and allow latent viruses to reactivate.
Dhatu Involvement in Latent Infections
Ayurveda also describes how pathogens can reside within deeper tissues of the body. The concept of Dhatu Dushti explains how disease processes may gradually affect specific tissues before producing visible symptoms.
Sanskrit Shloka
रसादीनां धातूनां क्रमशो विकृतिः भवति।
Transliteration
Rasadinaam dhatunam kramasho vikritih bhavati
Translation
The disturbance of tissues occurs progressively from one Dhatu to the next.
Source
Sushruta Samhita, Sutra Sthana, Chapter 15
This gradual tissue involvement explains how infections may remain hidden during early stages while affecting deeper biological systems. In viral diseases such as herpes, the virus may persist within nerve tissues for long periods before producing visible symptoms. From an Ayurvedic viewpoint, this can be interpreted as a subtle disturbance affecting deeper Dhatus and Srotas.
Role of Ojas and Immune Strength
Ayurveda places great importance on Ojas, the vital essence responsible for immunity, resilience, and overall vitality. When Ojas is strong, the body can suppress or control many disease processes even if pathogens are present.
Sanskrit Shloka
ओजः सर्वधातूनां सारम्।
Transliteration
Ojah sarva dhatunam saram
Translation
Ojas is the vital essence of all bodily tissues.
Source
Ashtanga Hridaya, Sutra Sthana, Chapter 11
Strong Ojas helps maintain equilibrium and prevents dormant infections from becoming active. Conversely, when Ojas becomes depleted due to stress, illness, poor nutrition, or lifestyle factors, latent pathogens may become active and produce clinical disease.
Integrating Classical Wisdom With Modern Virology
The Ayurvedic understanding of hidden disease processes aligns remarkably with modern scientific insights about viral latency and asymptomatic infections. While classical texts did not describe viruses in modern molecular terms, they recognized the existence of invisible disease-causing entities that could remain dormant within the body.
Modern virology explains that herpes simplex virus establishes lifelong latency within sensory nerve ganglia, reactivating periodically under favorable conditions. Ayurveda describes a similar concept through Krimi persistence, Dhatu involvement, and Dosha imbalance, emphasizing that disease may remain silent until internal balance is disturbed.
This integrative perspective highlights the depth of Ayurvedic medical observation and its relevance to contemporary infectious disease understanding. Silent infections, whether described through ancient terminology or modern virology, reflect a common biological principle: pathogens can remain hidden within the body until physiological conditions permit their activation.
When Women Should Seek Medical Evaluation
Table: Symptoms That Should Prompt Medical Evaluation
| Symptom | Possible Explanation | When to Seek Medical Advice |
|---|---|---|
| Persistent genital itching | Viral irritation or early infection | If symptoms last more than a few days |
| Burning during urination | Lesions near urethra | If pain occurs repeatedly |
| Recurrent vaginal discomfort | Possible internal lesions | When symptoms do not respond to routine treatments |
| Unexplained genital sores | Possible herpes infection | Immediate clinical examination recommended |
| Pain during intercourse | Inflammation of genital tissues | Medical evaluation if persistent |
| Positive HSV blood test without symptoms | Silent infection | Consultation to understand test results |
Herpes infection in women can sometimes present with subtle or easily misinterpreted symptoms. Because the virus can affect internal genital tissues such as the cervix and vaginal canal, early signs may not always be visible externally. Medical evaluation becomes essential when symptoms persist, worsen, or create uncertainty about the underlying cause. Clinical guidelines for sexually transmitted infections emphasize the importance of early consultation when symptoms suggest possible viral or genital infection [6].
Timely medical evaluation allows physicians to perform appropriate diagnostic tests, rule out other conditions, and provide accurate counseling regarding transmission, management, and prevention. Many women initially attribute symptoms to common gynecological conditions such as yeast infections, urinary tract infections, or hormonal irritation, which can delay correct diagnosis. Recognizing when professional medical assessment is necessary can therefore prevent prolonged discomfort and reduce the risk of complications.
Persistent Genital Discomfort or Unusual Sensations
Medical consultation is recommended when genital discomfort lasts for several days without improvement. Symptoms may include burning, tingling, itching, or mild irritation in the genital region. These sensations sometimes occur before visible lesions develop and may represent the early stages of viral activity. Clinical descriptions of herpes infections note that prodromal symptoms can appear before visible lesions emerge, making professional evaluation important when unexplained genital sensations occur [1].
Some women also experience mild swelling, localized tenderness, or a feeling of pressure in the genital area. These signs are often overlooked because they resemble common inflammatory or hormonal conditions. However, persistent or recurrent episodes warrant proper clinical examination to determine the underlying cause.
Recurrent Vaginal or Cervical Irritation
Another reason to seek medical evaluation is repeated episodes of genital irritation that do not respond to routine treatments. When antifungal medications or standard therapies for bacterial infections fail to resolve symptoms, clinicians may consider viral causes such as herpes simplex infection. Gynecological examinations may reveal subtle lesions inside the vaginal canal or on the cervix that are not visible without medical instruments [1].
Such internal lesions may produce symptoms such as vaginal discomfort, unusual discharge, or mild pelvic pain. Because these signs overlap with several gynecological disorders, laboratory confirmation through swab testing or serological testing may be required to clarify the diagnosis.
Pain During Urination or Intercourse
Pain or burning during urination can sometimes occur when lesions are present near the urethral opening. Similarly, discomfort during sexual intercourse may result from inflammation or microscopic lesions within the genital tissues. These symptoms can be mistaken for urinary infections or vaginal dryness, particularly when external sores are absent.
Clinical guidelines recommend medical assessment when genital pain interferes with daily activities, sexual health, or urinary comfort. Accurate diagnosis allows healthcare professionals to provide appropriate counseling and treatment strategies [6].
Unexplained Flu Like Symptoms with Genital Discomfort
During initial viral exposure, some individuals may experience systemic symptoms such as mild fever, fatigue, or body aches alongside genital irritation. These symptoms resemble common viral illnesses and may not immediately suggest a genital infection.
If systemic symptoms occur together with genital discomfort or lesions, medical evaluation becomes particularly important. Early testing during this stage can help confirm viral infection and guide management strategies [6].
Uncertainty After Sexual Exposure
Women who have had recent sexual contact with a partner diagnosed with herpes or another sexually transmitted infection should consider medical evaluation even if symptoms are mild or absent. Many herpes infections are transmitted during periods when the infected partner has no visible lesions. Because asymptomatic viral shedding can occur, testing and counseling may be recommended after potential exposure [1].
Consultation with a healthcare professional provides an opportunity to discuss risk factors, prevention strategies, and appropriate testing options. Education about transmission patterns can also help reduce anxiety and confusion surrounding the infection.
Symptoms That Continue Without Clear Diagnosis
In some situations, women may experience recurring genital symptoms despite multiple consultations or normal laboratory results. Persistent symptoms without a clear explanation should prompt further evaluation by clinicians familiar with sexually transmitted infections and gynecological disorders.
Specialized testing methods, including polymerase chain reaction (PCR) analysis, may detect viral DNA even when lesions are minimal or healing. These advanced diagnostic tools help clarify cases where traditional testing methods provide inconclusive results [6].
Importance of Early Clinical Assessment
Early medical evaluation plays a crucial role in managing genital infections effectively. Accurate diagnosis helps distinguish herpes infection from other conditions such as bacterial vaginosis, yeast infections, contact dermatitis, or autoimmune disorders affecting the genital skin.
Clinical assessment also allows healthcare providers to discuss long term management, preventive strategies, and lifestyle considerations that may influence recurrence patterns. Understanding the nature of the infection empowers patients to make informed decisions about their health and relationships.
Recognizing when professional evaluation is necessary ensures that symptoms are addressed promptly and appropriately. For many women, early consultation provides clarity, reassurance, and access to effective care options that support both physical and emotional well being.
Can Silent Herpes Infection Be Eliminated

Silent herpes infection refers to the presence of the herpes simplex virus (HSV) in the body without visible symptoms. Many individuals carry the virus for years without recognizing it because the virus remains dormant inside nerve cells. Modern virology describes this stage as viral latency, where the virus hides inside sensory nerve ganglia after the initial infection [3].
During this latent phase the virus does not actively replicate, which is why a person may have no visible sores or discomfort. The virus remains stored primarily in the trigeminal ganglia in oral infections and in the sacral nerve ganglia in genital infections. Because the immune system cannot easily eliminate viral DNA inside neurons, conventional medical treatment focuses mainly on suppressing viral activity rather than eliminating the infection completely [4].
Viral Latency and Hidden Infection
After entering the body through skin or mucosal tissue, herpes virus travels along peripheral nerves toward clusters of nerve cells called ganglia. Inside these neurons the viral genome remains present as episomal DNA and becomes inactive.
During latency the virus does not produce new viral particles, and therefore visible symptoms may not appear. This biological strategy allows HSV to persist silently inside the nervous system for long periods [5].
Because the virus is hidden inside nerve cells, many individuals may test positive for HSV antibodies while having no visible outbreaks. This is why herpes infection is often discovered incidentally during routine blood tests, fertility screening, or pregnancy examinations.
Reactivation Cycles and Silent Viral Shedding
Although the virus may remain dormant, it can reactivate periodically. Reactivation occurs when the virus begins replicating again within nerve cells and travels back along nerve pathways toward the skin or mucosal surfaces.
Triggers such as stress, immune suppression, hormonal fluctuations, fever, illness, or tissue irritation can stimulate viral reactivation. However, reactivation does not always produce visible lesions. In many cases viral shedding occurs without symptoms, meaning the virus may become active temporarily without the individual noticing it [4].
Scientific research has confirmed that asymptomatic viral shedding is a major reason herpes spreads unknowingly between partners. Viral particles can occasionally be detected on mucosal surfaces even when no sores are present [5].
Limitations of Conventional Treatment
Standard antiviral medications such as acyclovir, valacyclovir, and famciclovir work by inhibiting viral replication. These medicines can reduce symptoms, shorten outbreaks, and lower transmission risk. However, they do not remove the viral DNA stored in nerve ganglia.
Because these drugs only suppress viral activity temporarily, the infection often remains in the body indefinitely. This is why many patients experience recurrent outbreaks when medication is stopped or when immune stress triggers viral reactivation [3].
Ayurvedic View on Eliminating Latent Viral Disease
In Ayurveda, chronic and hidden infections are understood through the concept of Krimi, Srotorodha, and weakened Ojas, which together create an internal environment where pathogens remain dormant inside the body.
Classical Ayurvedic texts describe that when disease-causing organisms remain hidden in tissues, treatment should not only suppress symptoms but should remove the root cause and restore systemic balance.
Charaka Samhita explains the principle of eliminating deep-rooted disease through purification and rejuvenation therapy.
“संसर्गजाः क्रिमयः देहे तिष्ठन्ति दीर्घकालम्।
बलवद्भिरौषधैः शोधनैश्च विनाशयेत्।”
Charaka Samhita, Chikitsa Sthana
Translation
Pathogenic organisms may remain hidden within the body for long periods. They should be eliminated using potent medicines and purification therapies that remove disease from its root.
According to Ayurvedic clinical philosophy, treatment involves three major stages:
• Removal of accumulated toxins and pathogenic factors
• Restoration of immune strength and metabolic balance
• Rejuvenation of tissues through Rasayana therapy
This multi-layered therapeutic approach aims to change the internal environment of the body so that hidden pathogens can no longer persist.
Ayurvedic Therapeutic Principle for Viral Elimination
Ayurvedic treatment for chronic viral diseases often involves combinations of Rasayana herbs, antiviral botanicals, mineral preparations, immune-modulating therapies, and individualized dietary protocols based on a person’s constitutional type.
These therapies aim to strengthen Ojas, restore Agni, clear blocked Srotas, and normalize immune response. By correcting the internal biological environment that allows the virus to remain active, the body gradually gains the ability to eliminate latent infection.
Yes. Ayurveda aims to eliminate silent herpes infection by addressing the root biological terrain where the virus survives, rather than only suppressing symptoms.
Clinical Ayurvedic protocols therefore focus on restoring systemic equilibrium so the body can overcome chronic viral persistence.
A Deeper Guide to Viral Elimination
Understanding how chronic viral infections persist and how different treatment systems approach them is essential for long term healing.
A detailed explanation of the scientific mechanisms of herpes latency, modern antiviral limitations, and Ayurvedic therapeutic strategies for eliminating viral infection is discussed in our main guide:
Herpes Ayurvedic Treatment: Diagnosis, Symptoms, and Long-Term Viral Elimination
This article explains how personalized Ayurvedic protocols aim to restore immune strength, correct internal imbalance, and support long-term viral eradication.
Key Facts Women Should Know About Silent Herpes Infection
| Topic | Key Medical Insight | What Women Should Understand |
|---|---|---|
| Silent infection | Herpes virus can remain dormant inside nerve ganglia for long periods | Many women may carry the virus without visible symptoms |
| Viral latency | HSV hides inside sensory nerve cells after initial infection | The virus may stay inactive for years |
| Asymptomatic viral shedding | The virus can occasionally reactivate without visible sores | Transmission may occur even when symptoms are absent |
| Internal lesions | Herpes lesions may appear inside the cervix or vaginal canal | Some infections remain unnoticed without medical examination |
| Hormonal influence | Hormonal fluctuations can affect immune response and viral activity | Symptoms may appear during stress or menstrual cycle changes |
| Blood test limitations | HSV antibody tests detect past exposure rather than active infection | A positive test does not always mean a current outbreak |
| Unexpected diagnosis | Many women discover herpes during fertility or pregnancy screening | Routine testing may reveal infections that previously caused no symptoms |
| Psychological impact | Unexpected diagnosis can cause anxiety or confusion | Proper medical counseling helps patients understand the condition |
| Medical evaluation | Persistent genital discomfort or unusual symptoms require professional assessment | Early evaluation helps confirm diagnosis and guide treatment |
| Long term management | Conventional medicine suppresses outbreaks but may not eliminate viral latency | Integrative approaches aim to restore immune balance and long term health |
FAQ
Can herpes remain in the body without symptoms?
Yes. Herpes simplex virus can remain dormant inside nerve cells for long periods without causing visible symptoms. This stage is called viral latency. During this time the virus stays inactive inside nerve ganglia.
Why do some people never notice herpes symptoms?
In many individuals the immune system keeps viral activity under control. Because the virus remains hidden in nerve cells, infection may stay unnoticed for years and may only be discovered during routine medical testing.
Can herpes spread when no symptoms are present?
Yes. The virus can occasionally reactivate without visible sores. During this period, known as asymptomatic viral shedding, the virus may be present on the skin or mucosal surfaces and can potentially spread to a partner.
Do blood tests always confirm active herpes infection?
Blood tests detect antibodies produced by the immune system after exposure to the virus. A positive result usually means the body has encountered herpes at some point, but it does not always indicate an active infection.
Can silent herpes infection be eliminated?
Conventional medicine focuses mainly on suppressing viral activity. In contrast, Ayurvedic treatment aims to restore immune balance, remove internal disease-supporting factors, and strengthen the body so that the virus cannot persist. Many Ayurvedic protocols therefore aim at long-term elimination of silent infection rather than temporary suppression.
Reference
- Corey, L., & Wald, A. (1999). Maternal and neonatal herpes simplex virus infections. New England Journal of Medicine, 341(16), 1228–1235. https://doi.org/10.1056/NEJM199910143411606
Brief explanation: This landmark clinical review explains how HSV infections often remain undiagnosed and asymptomatic, especially in women. It also discusses transmission dynamics and the clinical importance of recognizing silent infection.
Suggested section use: Global prevalence of silent HSV infection, pregnancy screening discovery, asymptomatic carriers. - Looker, K. J., Magaret, A. S., May, M. T., Turner, K. M. E., Vickerman, P., Gottlieb, S. L., & Newman, L. M. (2015). Global and regional estimates of prevalent and incident herpes simplex virus type 1 infections in 2012. PLOS ONE, 10(10), e0140765. https://doi.org/10.1371/journal.pone.0140765
Brief explanation: This global epidemiological study provides estimates showing that hundreds of millions of people carry HSV infections, many without symptoms. It supports the statement that herpes is extremely common and frequently unnoticed.
Suggested section use: Hidden epidemic, prevalence statistics, silent infection. - Johnston, C., Koelle, D. M., & Wald, A. (2016). HSV-2: in pursuit of a vaccine. Journal of Clinical Investigation, 126(3), 851–858. https://doi.org/10.1172/JCI84424
Brief explanation: This virology-focused article explains HSV latency, immune response, and viral persistence in nerve cells. It supports discussions about viral dormancy and intermittent shedding.
Suggested section use: Viral latency, asymptomatic shedding, silent infection biology. - Tronstein, E., Johnston, C., Huang, M. L., Selke, S., Magaret, A., Warren, T., Corey, L., & Wald, A. (2011). Genital shedding of herpes simplex virus among symptomatic and asymptomatic persons with HSV-2 infection. JAMA, 305(14), 1441–1449. https://doi.org/10.1001/jama.2011.420
Brief explanation: This widely cited study measured HSV shedding patterns and demonstrated that people without symptoms can still shed the virus and potentially transmit infection.
Suggested section use: Asymptomatic viral shedding, silent transmission. - Wald, A., Zeh, J., Selke, S., Ashley, R. L., & Corey, L. (2000). Virologic characteristics of subclinical and symptomatic genital herpes infections. New England Journal of Medicine, 342(12), 844–850. https://doi.org/10.1056/NEJM200003233421203
Brief explanation: This clinical research paper demonstrates that HSV reactivation occurs frequently even when no lesions are visible, confirming the concept of subclinical infection.
Suggested section use: Silent viral reactivation, subclinical infection explanation. - Centers for Disease Control and Prevention. (2021). Sexually transmitted infections treatment guidelines: Genital herpes. https://www.cdc.gov/std/treatment-guidelines/herpes.htm
Brief explanation: The CDC guideline explains herpes epidemiology, testing strategies, and asymptomatic infection patterns. It is widely used in clinical practice across the United States and internationally.
Suggested section use: testing confusion, epidemiology, diagnosis. - Ashley-Morrow, R., Nollkamper, J., Robinson, N., Bishop, N., & Smith, J. (2003). Performance of focus and kalon enzyme-linked immunosorbent assays for antibodies to herpes simplex virus type 2 glycoprotein G in culture-documented cases of genital herpes. Journal of Clinical Microbiology, 41(2), 521–523. https://doi.org/10.1128/JCM.41.2.521-523.2003
Brief explanation: This study evaluates HSV antibody tests and explains how blood tests detect exposure rather than active infection, which often confuses patients receiving unexpected positive results.
Suggested section use: testing confusion section. - Gillgrass, A. E., Fernandez, S. A., Rosenthal, K. L., & Kaushic, C. (2005). Estradiol regulates susceptibility following primary exposure to genital herpes simplex virus type 2. Journal of Virology, 79(5), 3107–3116. https://doi.org/10.1128/JVI.79.5.3107-3116.2005
Brief explanation: This experimental study shows how estrogen affects immune responses to HSV infection in the female reproductive tract. It supports explanations of hormonal influence on viral activity.
Suggested section use: estrogen immune interaction section. - Cherpes, T. L., Meyn, L. A., Krohn, M. A., & Hillier, S. L. (2003). Association between acquisition of herpes simplex virus type 2 in women and bacterial vaginosis. Journal of Infectious Diseases, 187(6), 934–940. https://doi.org/10.1086/368163
Brief explanation: This study investigates the interaction between genital immune environment and HSV infection in women, highlighting how vaginal microbiome and mucosal immunity influence susceptibility and symptoms.
Suggested section use: female immune environment, genital tract explanation. - Charaka Samhita, Chikitsa Sthana, Chapter 7 (Krimi Chikitsa Adhyaya), verses describing internal pathogens and latent disease processes. Standard English translation by Sharma, P. V. (2008). Chaukhambha Orientalia.
Brief explanation: Classical Ayurvedic text describing internal pathogens (Krimi) that can remain dormant within tissues and later produce disease when bodily balance is disturbed. This concept parallels modern ideas of latent infections.
Suggested section use: Ayurvedic interpretation of silent viral infection. - Sushruta Samhita, Sutra Sthana, Chapter 24, verses describing the importance of Ojas in maintaining resistance to disease. Standard English translation by Sharma, P. V. (2008). Chaukhambha Orientalia.
Brief explanation: This classical Ayurvedic text explains how Ojas represents systemic immunity and vitality, which protects the body against disease processes. Reduced Ojas is associated with susceptibility to chronic conditions.
Suggested section use: immune strength, Ayurvedic explanation. - Bhavaprakasha, Madhyama Khanda, Krimi Rogadhikara, classical description of internal pathogenic organisms and their manifestations. Translation by Srikantha Murthy, K. R. (2001). Chaukhambha Krishnadas Academy.
Brief explanation: Bhavaprakasha describes various forms of internal pathogens affecting reproductive and systemic health, providing conceptual parallels to latent microbial infections.
Suggested section use: Ayurvedic section discussing latent pathogens.
Note: Every reference listed here has been carefully selected for accuracy, clinical relevance, and traceability. Ayurvedic formulations are cited directly from classical medical texts such as Charaka Samhita, Sushruta Samhita, and Bhavaprakasha along with specific chapters and verses. All modern scientific studies are provided with active hyperlinks in APC format. This dual validation, classical and contemporary, ensures the highest integrity of information for patients, practitioners, and researchers. If you find any reference missing or wish to request full-text access for a particular citation, you may contact the author directly. Our goal is to maintain complete transparency and academic rigor.