- Anatomy and Physiology
- Pathophysiology
- Disorders of the Parathyroid
- Hyperparathyroidism
- Hypoparathyroidism
- Parathyroid Carcinoma
- Causes and Risk Factors
- Diagnostic Approaches
- Diseases and Conditions Associated With Parathyroid Disorders
- Ayurvedic Perspective on Parathyroid Disorders
- Less Common and Rare Diseases Associated With Parathyroid Disorders
- Ayurvedic Interpretation of Less Common and Rare Parathyroid Related Diseases
- Modern Medical Management
- Prognosis, Disease Progression, and Quality of Life
- Why the Condition Often Persists or Recurs
- Ayurvedic Treatment Principles
- Ayurveda Avaleha (Medicine) for Cure
- Critical Warning About Market Purchased Avaleha and Self Preparation
- Modern Scientific Research
- Diet and Lifestyle Recommendations
- Preventive Strategies
- When to Seek Medical Advice
- Guidance From NCCIH and Major Governing Bodies
- FAQs
- References
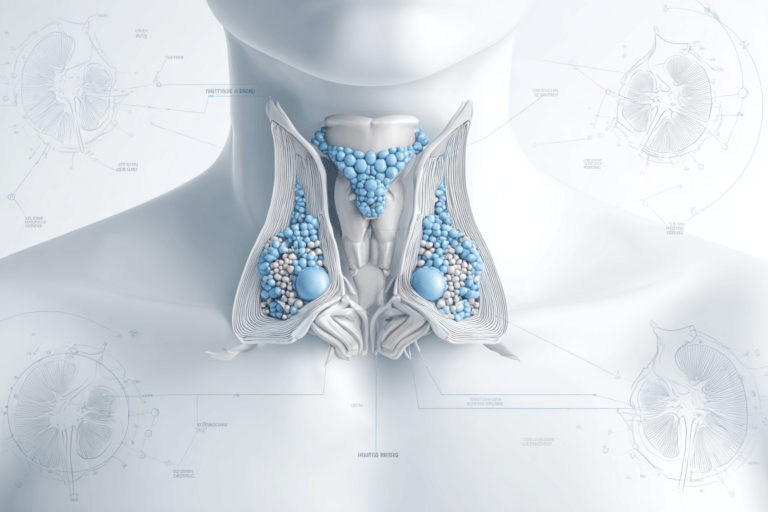
The parathyroid glands are four tiny endocrine structures located behind the thyroid gland, yet they play a crucial role in regulating calcium and phosphorus balance in the human body. Unlike the thyroid, which manages metabolism through thyroxine, the parathyroid glands secrete parathyroid hormone (PTH), a key regulator of bone strength, kidney function, and neuromuscular stability [1].
Disturbances in parathyroid function can lead to two opposite but equally dangerous conditions: hyperparathyroidism, where excess hormone causes calcium overload, kidney stones, and bone resorption, and hypoparathyroidism, where low hormone levels trigger tetany, seizures, and brittle bones [2]. Rarely, parathyroid cancer can arise, usually presenting with severe hypercalcemia and aggressive symptoms [3].
From an Ayurvedic perspective, parathyroid dysfunction may be correlated with Asthi Dhatu Kshaya (weakening of bone tissue), Majja Dhatu Dushti (marrow and nervous system imbalance), and Kapha-Pitta aggravation (stones, sluggish digestion, swelling) or Vata aggravation (tetany, cramps, dryness) [4]. Classical Ayurvedic texts emphasize maintaining calcium homeostasis through Rasayanas, mineral preparations like Praval Pishti, Mukta Sukti Bhasma, and Godanti Bhasma, and lifestyle measures such as sunlight exposure, diet, and stress regulation [5].
With rising cases of lifestyle disorders, thyroid–parathyroid surgeries, and chronic kidney disease, parathyroid disorders are becoming more prevalent worldwide. Modern medicine offers surgical and pharmacological interventions, while Ayurveda provides a holistic, root-cause–oriented approach that not only manages symptoms but also restores long-term balance [6].
Important Medical Safety Notice
Parathyroid disorders can lead to life-threatening complications if mismanaged. Symptoms such as confusion, seizures, severe muscle spasms, chest pain, extreme weakness, or dehydration require urgent medical attention. Ayurvedic support should never replace emergency care, surgery, or endocrinologist-guided treatment when clinically indicated.
Table: A Complete Clinical Overview for Patients
| Topic | Key Insight |
|---|---|
| What is a Parathyroid Disorder | A condition where glands in the neck disrupt calcium balance affecting bones, kidneys, and nerves |
| Main Types | Primary hyperparathyroidism, secondary hyperparathyroidism, hypoparathyroidism |
| Early Signs | Fatigue, weakness, constipation, mild bone pain, mood changes |
| Serious Symptoms | Kidney stones, fractures, severe cramps, confusion |
| Causes | Gland overactivity, vitamin D deficiency, kidney disease, surgery |
| Diagnosis | Blood tests calcium, PTH, vitamin D, imaging |
| Treatment | Monitoring, medication, surgery based on severity |
| Why It Persists | Metabolic imbalance, kidney involvement, delayed diagnosis |
| Ayurvedic View | Agni imbalance, Asthi Dhatu depletion, systemic dysfunction |
Anatomy and Physiology
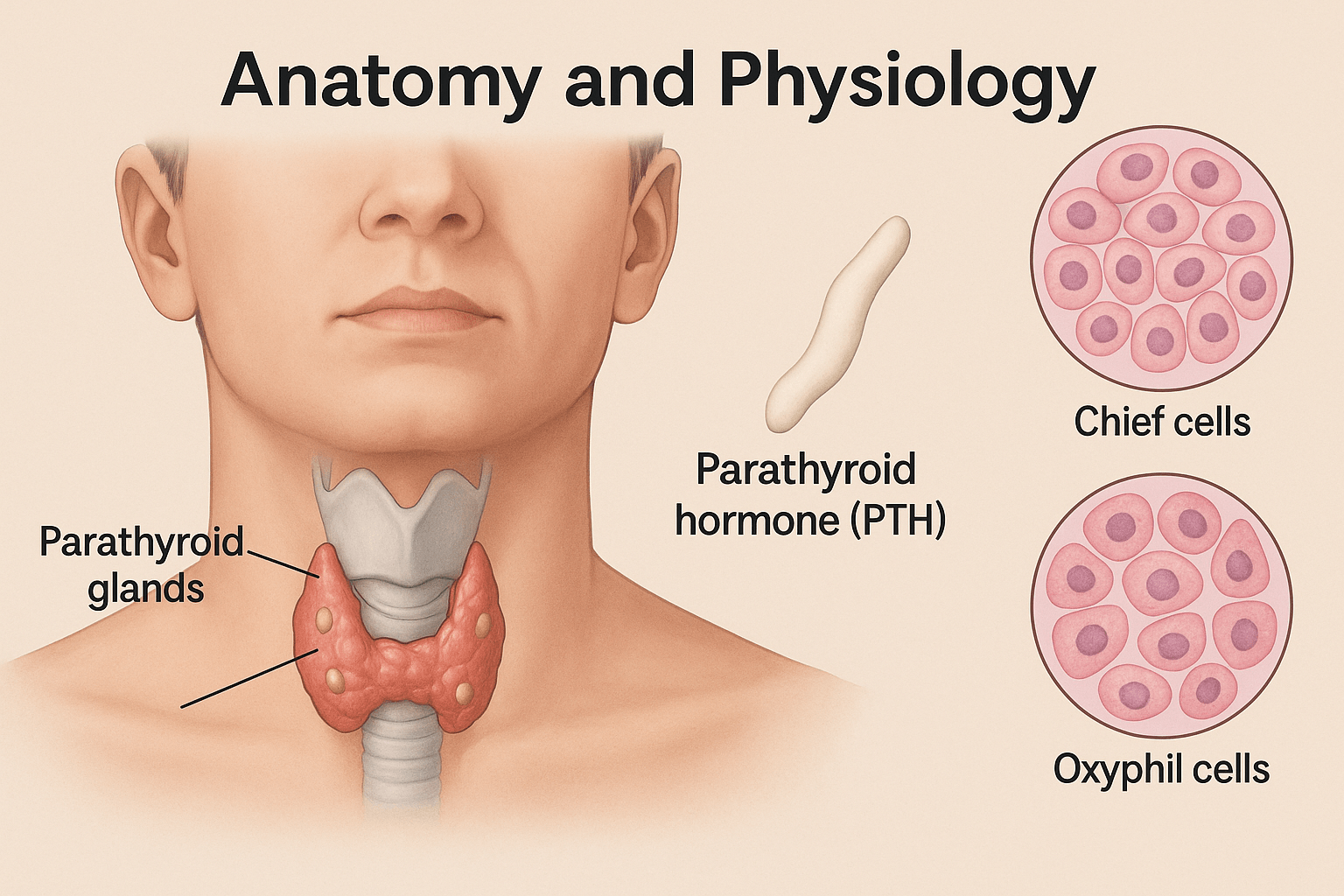
Structure of Parathyroid Glands
The parathyroid glands are typically four small, oval-shaped structures located on the posterior surface of the thyroid gland, though anatomical variations exist where individuals may have three or even five glands [1]. Each gland measures only a few millimeters in size yet carries immense importance for calcium balance. Unlike the thyroid, which is encapsulated and highly vascular, the parathyroid glands have a delicate capsule and are richly supplied with blood vessels to allow rapid hormone release into circulation [2].
Histology: Chief Cells and Oxyphil Cells
Microscopically, the parathyroid glands are composed primarily of two cell types. Chief cells are the most abundant and are responsible for the synthesis and secretion of parathyroid hormone (PTH). These cells contain numerous secretory granules, reflecting their endocrine function [3]. The second type, oxyphil cells, appear larger with an acidophilic cytoplasm rich in mitochondria. Their exact function remains less defined, though modern research suggests they may contribute to oxidative metabolism and possibly play a role in parathyroid hormone reserve [4].
Hormonal Function: Parathyroid Hormone (PTH)
The primary hormone secreted by the parathyroid glands is parathyroid hormone (PTH), a peptide consisting of 84 amino acids. PTH is a master regulator of serum calcium and phosphate levels, acting as a feedback mechanism when calcium levels drop in the bloodstream [5]. The release of PTH is tightly regulated by calcium-sensing receptors (CaSR) located on the parathyroid chief cells.
Role of PTH in Regulating Calcium, Phosphate, and Vitamin D
PTH increases serum calcium through three major mechanisms:
- Bone: Stimulates osteoclast activity indirectly via osteoblast signaling, leading to calcium release from bone matrix [6].
- Kidneys: Enhances calcium reabsorption in renal tubules while promoting phosphate excretion, preventing simultaneous hyperphosphatemia [7].
- Intestines: Indirectly increases calcium absorption by stimulating renal production of calcitriol (active vitamin D, 1,25-dihydroxycholecalciferol), which in turn promotes intestinal calcium uptake [8].
This finely tuned balance ensures adequate calcium availability for neuromuscular conduction, bone mineralization, and enzymatic functions. Disturbances in PTH secretion, therefore, have widespread systemic consequences.
From an Ayurvedic perspective, this regulation can be related to the dynamic interaction of Asthi Dhatu (bone tissue), Majja Dhatu (marrow and nervous system), and Shukra Ojas (vital essence). The parathyroid’s role in balancing calcium parallels the Ayurvedic concept of maintaining Dhatu Samya (tissue equilibrium), where disruption leads to conditions such as Asthi Kshaya (bone weakening) or Vata-related neuromuscular spasms [9].
Pathophysiology

Mechanism of Calcium Regulation
The parathyroid glands maintain calcium levels within a narrow physiological range (8.5–10.5 mg/dL). When serum calcium drops, calcium-sensing receptors (CaSR) on parathyroid chief cells are activated, stimulating the release of parathyroid hormone (PTH). PTH then works through bone, kidney, and intestines to restore calcium homeostasis [1]. Conversely, when calcium rises above normal, PTH secretion is suppressed, preventing hypercalcemia [2].
Interplay with Kidney, Bone, and Intestines
The action of PTH spans multiple organ systems:
- Bone: PTH stimulates osteoblasts to release RANKL, which activates osteoclasts, leading to the release of calcium and phosphate from bone into the blood. This ensures immediate calcium availability but contributes to bone resorption if prolonged [3].
- Kidneys: PTH promotes calcium reabsorption in the distal tubules, reduces phosphate reabsorption in the proximal tubules (preventing calcium-phosphate precipitation), and stimulates the conversion of 25-hydroxyvitamin D into active 1,25-dihydroxyvitamin D (calcitriol) [4].
- Intestines: The increase in calcitriol enhances calcium and phosphate absorption from the gut, supporting bone mineralization and systemic calcium balance [5].
Feedback Loop with Calcitonin and Vitamin D
Calcium regulation involves a delicate feedback loop. While PTH raises calcium, calcitonin, secreted by parafollicular cells (C-cells) of the thyroid, acts as a counter-regulatory hormone, lowering calcium by inhibiting osteoclast activity and increasing calcium deposition in bones [6]. In parallel, vitamin D plays a dual role: its active form, calcitriol, enhances intestinal calcium absorption but also provides negative feedback on the parathyroid gland to suppress excess PTH secretion [7].
This balance ensures that serum calcium remains stable, supporting neuromuscular conduction, cardiac rhythm, clotting mechanisms, and skeletal strength. Disturbances in any part of this axis, parathyroid glands, kidneys, bones, or vitamin D metabolism, result in clinical manifestations such as osteoporosis, kidney stones, or neuromuscular dysfunction [8].
From an Ayurvedic perspective, this dynamic interaction mirrors the Samyavastha (homeostasis) of Asthi Dhatu (bone tissue) and Majja Dhatu (nervous system and marrow). Disruption in this regulation can be correlated with Asthi Kshaya (bone weakening), Mutrashmari (urinary stones), and Vata-Pitta imbalance, where deranged fire (Agni) and obstructed channels (Srotas) disturb the equilibrium of mineral metabolism [9].
Disorders of the Parathyroid
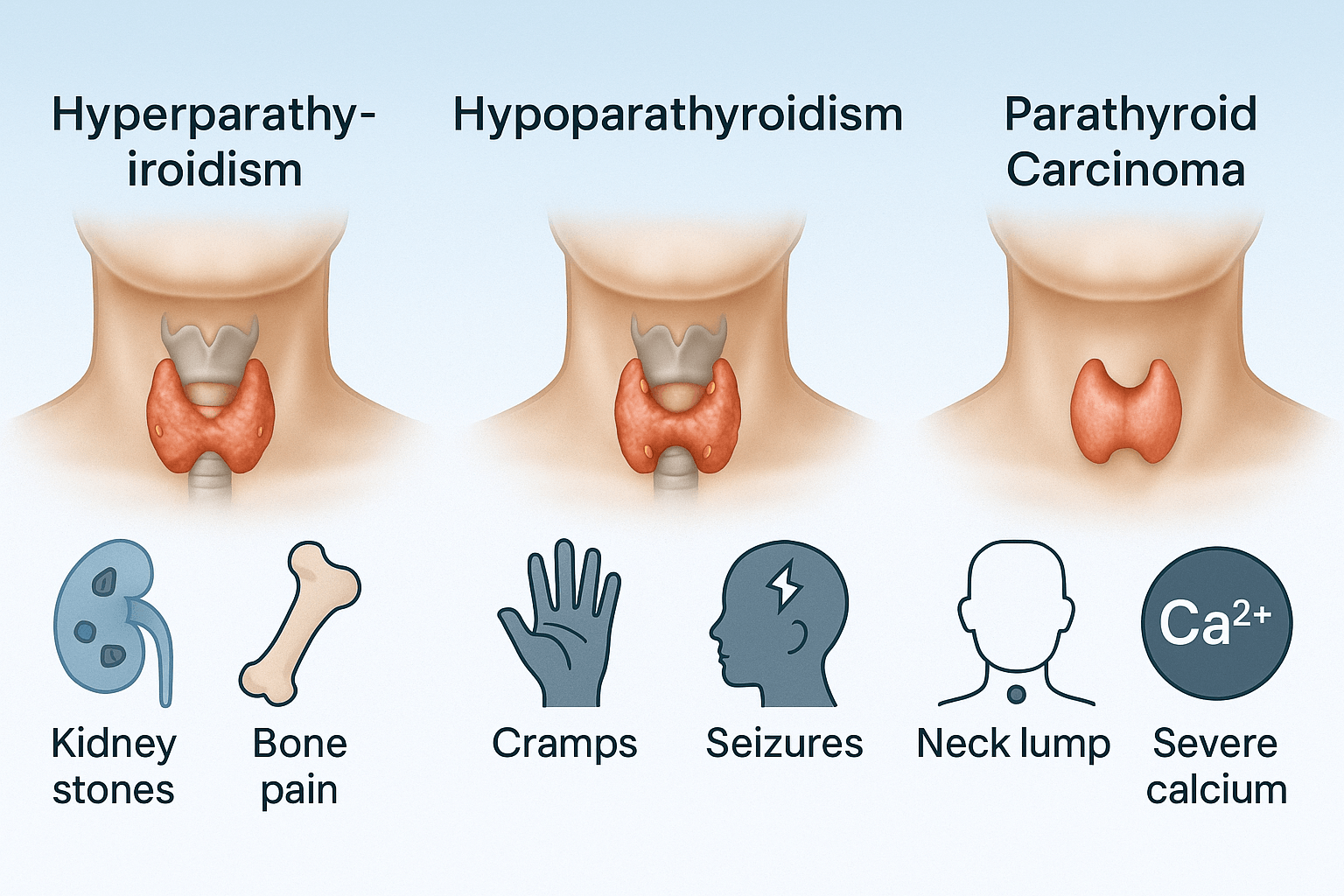
The parathyroid glands, despite their small size, are responsible for maintaining calcium-phosphate balance. Dysfunction of these glands leads to three major clinical entities: hyperparathyroidism, hypoparathyroidism, and parathyroid carcinoma. Each has distinctive causes and symptom clusters that can severely affect multiple organ systems.
Hyperparathyroidism
Hyperparathyroidism happens when the parathyroid glands make too much parathyroid hormone (PTH). This hormone normally helps regulate calcium and phosphorus levels, but when produced in excess, it disrupts the body’s mineral balance.
There are three main types:
- Primary hyperparathyroidism is most often caused by a benign growth (adenoma) on one of the parathyroid glands. Less commonly, all glands may be enlarged (hyperplasia).
- Secondary hyperparathyroidism develops as a result of another condition, most often chronic kidney disease (CKD). In CKD, the kidneys can’t properly regulate calcium and phosphate, which overstimulates the parathyroid glands.
- Tertiary hyperparathyroidism occurs when long-term secondary hyperparathyroidism becomes autonomous, with the glands continuing to release excess hormone even after the underlying problem is addressed.
Symptoms can vary widely, but the classic presentation is described as “stones, bones, groans, and psychic moans.”
- Stones: kidney stones, frequent urination, and calcium buildup in the kidneys.
- Bones: bone pain, fractures, and osteoporosis.
- Groans: abdominal discomfort, nausea, constipation, and sometimes pancreatitis.
- Psychic moans: depression, fatigue, and memory problems.
Other symptoms may include muscle weakness, hypertension, and generalized fatigue. If left untreated, complications such as severe bone loss, kidney damage, and cardiovascular problems can occur.
Hypoparathyroidism
Hypoparathyroidism is the opposite problem. It occurs when the parathyroid glands do not produce enough PTH. Without this hormone, calcium levels in the blood drop too low, while phosphate levels rise.
The most common cause is accidental damage or removal of the parathyroid glands during thyroid or neck surgery. Autoimmune conditions, genetic mutations, and certain metabolic disorders can also lead to hypoparathyroidism.
Symptoms are mainly related to low calcium (hypocalcemia) and include:
- Tingling or numbness in the lips, fingers, and toes.
- Muscle cramps, spasms, or painful contractions.
- Twitching of the facial muscles (Chvostek’s sign) or hand spasms when the arm is compressed (Trousseau’s sign).
- In more severe cases, seizures.
Over time, patients may also develop brittle nails, dry skin, coarse hair, and dental abnormalities. Psychological changes such as anxiety, irritability, and depression are also common. If untreated, hypoparathyroidism can cause chronic neuromuscular symptoms, calcification in soft tissues, and impaired quality of life.
Treatment usually involves calcium and vitamin D supplementation, and in some cases synthetic PTH therapy. Lifelong monitoring is typically required.
Parathyroid Carcinoma
Parathyroid carcinoma is a very rare but serious cancer of the parathyroid glands. It accounts for less than 1% of cases of primary hyperparathyroidism. Unlike benign adenomas, this tumor can invade nearby tissues and spread to other organs.
The exact cause is unknown, but certain inherited syndromes such as multiple endocrine neoplasia type 1 (MEN1) and mutations in the HRPT2 gene increase the risk.
Symptoms are usually more severe than in benign parathyroid disease because the tumor produces extremely high levels of PTH, leading to dangerous hypercalcemia. Common signs include:
- Persistent nausea, vomiting, dehydration, and confusion.
- A noticeable lump in the neck.
- Hoarseness or difficulty swallowing if the tumor presses on surrounding structures.
- Severe bone pain and fractures due to calcium loss.
Because symptoms often overlap with benign hyperparathyroidism, diagnosis can be challenging. Blood calcium and PTH levels are usually extremely elevated, and imaging may reveal a neck mass.
Treatment typically requires surgical removal of the cancerous gland along with surrounding tissue. Even with surgery, recurrence is common, and patients need close long-term monitoring.
Causes and Risk Factors
Parathyroid disorders do not emerge in a vacuum. They develop within a biological and clinical context that is often overlooked until symptoms become persistent, disruptive, or structurally damaging. For many patients, the first visible sign is not a gland problem but a consequence: a kidney stone, bone loss, unexplained fatigue, muscle cramps, mood change, or abnormal calcium levels on routine blood work. From a strategic clinical perspective, this matters greatly. When the cause is misunderstood, treatment becomes reactive. When the cause is identified clearly, management becomes more precise, credible, and potentially more effective.
A strong pillar article must therefore go beyond naming the disorder. It must help the patient understand not only what parathyroid disease is, but why it begins, what makes it more likely, and which hidden factors allow it to progress. That is where this section becomes essential.
Primary Hyperparathyroidism
The most common cause of primary hyperparathyroidism is a benign overactive parathyroid adenoma. In this situation, one of the parathyroid glands begins secreting excess parathyroid hormone independently of the body’s actual mineral needs. Less commonly, multiple glands enlarge in a process known as parathyroid hyperplasia. In rare cases, parathyroid carcinoma may be responsible. For the patient, the result is the same at first: the gland continues sending a biochemical signal that raises calcium levels, pulls calcium from bone, alters kidney handling of minerals, and gradually destabilizes the body’s internal equilibrium.
What makes this especially important is that many patients do not feel acutely ill in the beginning. They may simply notice fatigue, constipation, subtle mood changes, recurrent renal stones, or declining bone strength. Because these complaints are common and often treated separately, the underlying endocrine driver may remain hidden for years. This is one reason parathyroid disease can advance silently while damage accumulates in bone, kidney, and quality of life.
Secondary Hyperparathyroidism
Secondary hyperparathyroidism develops when the parathyroid glands are responding to a chronic stress signal elsewhere in the body rather than acting as the original problem. The most common cause is chronic kidney disease. As kidney function declines, phosphate excretion becomes impaired, vitamin D activation decreases, and calcium regulation becomes less stable. The parathyroid glands react by producing more hormone in an attempt to maintain balance.
This adaptive response may initially appear protective, but over time it becomes harmful. Persistent elevation of parathyroid hormone can lead to bone pain, skeletal weakness, muscle fatigue, vascular calcification, and a broader syndrome of mineral and metabolic disruption. In advanced disease, long standing overstimulation may cause the glands to become autonomously overactive, creating a more severe state often described as tertiary hyperparathyroidism.
For the global patient exploring natural or Ayurvedic care, this distinction is critical. A person with gland driven primary disease is not the same as a patient with kidney driven secondary disease. The terrain, the risks, the expected progression, and the therapeutic priorities are different.
Vitamin D Deficiency and Mineral Dysregulation
Vitamin D deficiency is one of the most important and frequently underestimated contributors to parathyroid dysfunction. When vitamin D is inadequate, calcium absorption from the intestine falls, even if the diet appears acceptable. The body interprets this as a threat to mineral balance, and parathyroid hormone rises in compensation. This can produce elevated parathyroid hormone with normal, low normal, or low calcium depending on the individual stage and context.
This pattern is common in patients with low sunlight exposure, indoor lifestyles, darker skin living in less sunny regions, malabsorption disorders, chronic gut inflammation, obesity, restrictive diets, or prolonged nutritional neglect. For international readers, especially those in the USA, UK, Canada, Australia, and Singapore, this is highly relevant because modern lifestyles often disconnect people from the natural environmental factors that support healthy mineral metabolism.
Post Surgical Hypoparathyroidism
One of the most important causes of hypoparathyroidism is previous thyroid or neck surgery. The parathyroid glands are very small and lie close to the thyroid. During thyroidectomy or related procedures, they may be accidentally removed, bruised, devascularized, or otherwise impaired. When this happens, parathyroid hormone levels can drop sharply, leading to low calcium and neuromuscular instability.
Patients in this category may develop tingling around the mouth, cramps, muscle spasms, anxiety, weakness, or even seizures. In some cases the dysfunction is temporary, but in others it becomes chronic. This is a major risk factor that must never be ignored, especially in patients who develop unexplained symptoms after thyroid surgery and are told only that their calcium is slightly abnormal without deeper endocrine interpretation.
Autoimmune Causes
Autoimmune mechanisms may also damage parathyroid tissue and reduce hormone production. In these patients, the body’s immune system begins attacking endocrine structures in a way that disrupts normal function. This may occur alone or as part of a broader autoimmune syndrome involving the thyroid, adrenal glands, pancreas, or mucosal immunity.
From a patient education perspective, this is a high value point. It shows that parathyroid dysfunction may not always be local. Sometimes it is part of a systemic pattern. From an Ayurvedic perspective, such cases often suggest deep seated Agni disturbance, Ojas depletion, and chronic dysregulation of internal defense mechanisms.
Genetic and Familial Risk Factors
A smaller but clinically significant group of patients develops parathyroid disorders due to inherited syndromes or familial calcium regulation abnormalities. These include familial hyperparathyroid states, multiple endocrine neoplasia syndromes, familial hypocalciuric hypercalcemia, pseudohypoparathyroidism, and developmental disorders affecting the parathyroid glands.
These conditions matter because they often present earlier, behave differently, and may be mismanaged if they are mistaken for more common forms of disease. A young patient with abnormal calcium or parathyroid hormone levels, especially with family history, requires more careful interpretation than a typical older adult with sporadic disease. In strategic terms, the diagnosis changes the treatment path and sometimes the screening needs of the entire family.
Age and Life Stage
Age is not merely a demographic detail. It changes disease behavior, risk, resilience, and treatment response. In older adults, parathyroid disorders often coexist with osteoporosis, fracture risk, polypharmacy, vascular calcification, and reduced physiological reserve. Symptoms may be less dramatic but more dangerous because the cost of delayed diagnosis is higher.
In younger adults, the disease may be overlooked because serious structural damage has not yet appeared. In postmenopausal women, parathyroid dysfunction can significantly worsen bone loss and increase fragility risk. In children and adolescents, calcium metabolism operates in the context of growth and development, making endocrine disruption especially important. Pregnancy and breastfeeding further alter calcium handling and demand careful, individualized medical judgment.
Chronic Disease Burden
Parathyroid disorders are often shaped by the broader health background of the patient. Chronic kidney disease, recurrent renal stones, liver disease, malabsorption syndromes, diabetes, autoimmune disease, inflammatory bowel conditions, osteoporosis, and long term steroid exposure all influence mineral metabolism, tissue resilience, and treatment complexity.
This is one reason a standard, one size fits all explanation often fails patients. Two individuals may both show abnormal calcium and parathyroid hormone levels, yet the deeper clinical story may be entirely different. One may have a localized adenoma. Another may have long standing kidney disease. Another may be recovering from surgery. Another may have autoimmune endocrine disruption. The visible laboratory similarity can hide very different biological realities.
Lifestyle and Metabolic Stress
Lifestyle does not always initiate the disorder directly, but it often shapes the terrain in which the disorder becomes established and harder to reverse. Poor dietary quality, low sunlight exposure, chronic dehydration, high sodium intake, sedentary behavior, chronic stress, disturbed sleep, obesity, and years of fragmented symptom based care all contribute to metabolic instability.
From a Kotler style strategic view, this matters because patients do not only want a diagnosis. They want a narrative that makes sense of why this happened to them. Lifestyle and metabolic burden often provide that missing context. They explain why mineral imbalance persists, why energy declines, and why a narrow supplement based approach may fail without broader correction.
Medication Related Factors
Medication history is another frequently neglected contributor. Some drugs affect calcium handling, vitamin D metabolism, kidney function, bone turnover, or endocrine signaling. In patients already taking calcium supplements, calcitriol, thyroid medication, diuretics, steroids, antiepileptics, or kidney related therapies, the clinical picture becomes more complicated. These interactions can amplify symptoms, distort lab interpretation, or mask the real pattern of disease progression.
This is especially important before any integrative or Ayurvedic treatment is introduced. Without a clear understanding of the patient’s medication background, even well intentioned therapy can become poorly targeted.
The Real Clinical Message
The most important takeaway is this: parathyroid disorders are rarely random events. They usually arise within a framework of glandular pathology, kidney dysfunction, vitamin D deficiency, surgical injury, autoimmune change, inherited vulnerability, age related decline, chronic disease burden, or long standing metabolic stress. If this framework is ignored, treatment becomes superficial. If it is understood, the pathway to more intelligent and individualized care becomes much clearer.
Diagnostic Approaches

Diagnosing parathyroid disorders usually starts with simple blood work and then moves on to imaging and bone testing if needed. Doctors use these tools to confirm whether the glands are working properly and to check the effects of abnormal hormone levels.
Blood tests
The first step is usually blood testing. High or low calcium levels are a key sign of parathyroid problems. Other markers include phosphate, parathyroid hormone (PTH), and vitamin D. For example, high calcium and high PTH suggest hyperparathyroidism, while low calcium and low PTH point toward hypoparathyroidism.
Imaging
If a parathyroid tumor or enlarged gland is suspected, imaging can help locate the problem. Ultrasound of the neck is commonly used because it’s safe and non-invasive. A sestamibi scan is more specific, using a small radioactive tracer to highlight overactive parathyroid tissue. In difficult cases, advanced imaging such as MRI or CT scans may be used.
Bone mineral density testing
Because parathyroid disorders can weaken the bones, doctors often recommend a bone mineral density (DEXA) scan. This test measures bone strength and can reveal early osteoporosis or fracture risk, even before symptoms appear.
Diseases and Conditions Associated With Parathyroid Disorders
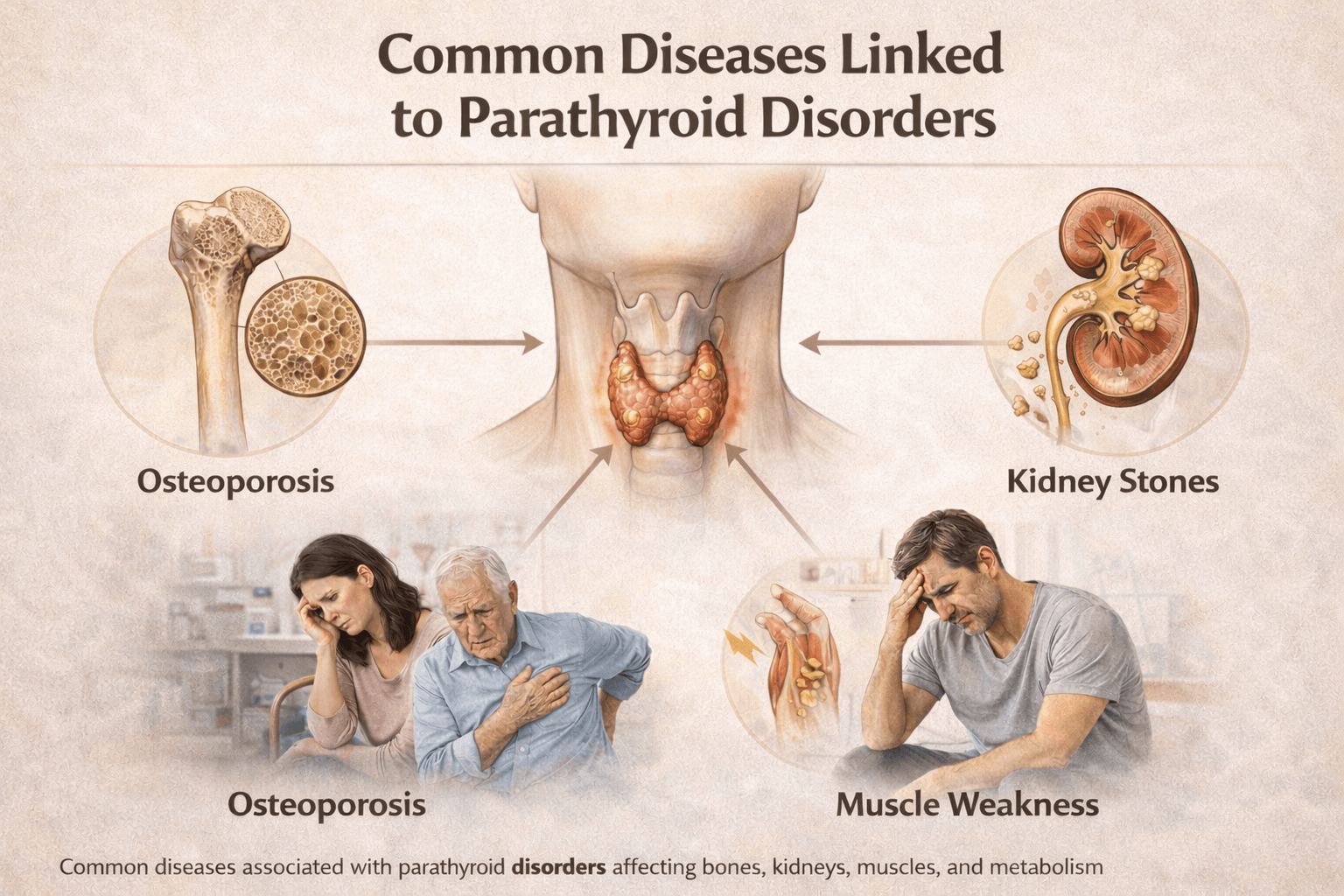
Parathyroid disorders influence far more than calcium values on a laboratory report. In my clinical experience, parathyroid hormone imbalance affects bones, kidneys, muscles, nerves, digestion, cardiovascular health, cognition, and long term metabolic stability. Many patients come with complaints such as bone pain, kidney stones, fatigue, anxiety, or seizures, while the underlying parathyroid disorder remains unrecognized. If you understand the full spectrum of associated diseases, you can identify patterns earlier and avoid years of misdirected treatment.
Bone and Skeletal Diseases
Excess parathyroid hormone accelerates bone resorption and weakens skeletal structure. Patients commonly develop osteopenia, osteoporosis, cortical bone loss, and fragility fractures. You may notice chronic back pain, height reduction, repeated fractures after minor trauma, or generalized bone discomfort. Clinicians often observe silent vertebral fractures even in patients who believe they are asymptomatic. In severe and prolonged disease, osteitis fibrosa cystica and brown tumor like lesions may appear, sometimes mimicking malignant bone disease on imaging. These skeletal manifestations represent advanced hormonal imbalance rather than isolated orthopedic problems.
Kidney and Urinary Tract Disorders
Renal involvement is one of the most frequent consequences of parathyroid dysfunction. Patients often experience recurrent kidney stones, flank pain, hematuria, or frequent urination. In many cases, nephrocalcinosis develops silently and is discovered incidentally. Over time, repeated calcium deposition and dehydration can reduce kidney function. If you have recurrent stones or unexplained decline in renal parameters, clinicians should consider parathyroid hormone excess as a contributing factor rather than treating stones as an isolated condition.
Neuromuscular and Neurological Conditions
Calcium imbalance directly alters nerve conduction and muscle excitability. In hypoparathyroidism, patients commonly experience tingling around the lips, fingers, and toes, muscle cramps, twitching, carpopedal spasm, and episodes of tetany. You may feel stiffness, restlessness, or involuntary contractions that worsen with stress. Severe hypocalcemia lowers the seizure threshold, and some patients are diagnosed with seizure disorders long before the metabolic cause is identified. Chronic cases may show basal ganglia calcification, movement disorders, or cognitive slowing, highlighting the deep neurological impact of untreated parathyroid disease.
Cardiac and Cardiovascular Associations
Parathyroid hormone and calcium balance play a critical role in cardiac conduction and vascular integrity. Patients may develop palpitations, prolonged QT interval, dizziness, syncope, or arrhythmias. Over the long term, mineral imbalance contributes to vascular calcification, arterial stiffness, hypertension, and increased cardiovascular risk. In patients with chronic kidney disease, these cardiovascular effects become more pronounced and contribute significantly to morbidity and mortality.
Gastrointestinal and Metabolic Disorders
Digestive symptoms are common but often overlooked. Patients frequently report constipation, abdominal discomfort, bloating, nausea, reduced appetite, and unexplained weight changes. Hypercalcemia can impair smooth muscle function and enzyme activity, leading to sluggish digestion. In some individuals, pancreatitis or peptic ulcer like symptoms develop in association with elevated calcium levels. If you have persistent gastrointestinal complaints along with fatigue, bone pain, or kidney stones, clinicians should evaluate parathyroid related causes.
Neuropsychiatric and Cognitive Conditions
Parathyroid disorders can significantly affect mental health and cognitive function. Patients often describe depression, anxiety, irritability, sleep disturbance, poor concentration, memory impairment, and a sense of mental clouding. I have seen patients treated for mood disorders for years without improvement until calcium and parathyroid hormone imbalance was corrected. These symptoms are biochemical in origin and not merely psychological, and they often improve when hormonal balance is restored.
Chronic Kidney Disease Related Parathyroid Disorders
In chronic kidney disease, secondary hyperparathyroidism develops due to phosphate retention and impaired vitamin D activation. Patients experience bone pain, muscle weakness, itching, fractures, and progressive vascular calcification. Over time, prolonged stimulation of the parathyroid glands can lead to tertiary hyperparathyroidism, where hormone secretion becomes autonomous and hypercalcemia persists even after kidney transplantation. If you or your patient has kidney disease, parathyroid monitoring becomes a long term necessity rather than an optional test.
Endocrine and Post Surgical Associations
Hypoparathyroidism is a well recognized complication after thyroid or neck surgery. Patients may develop early symptoms such as numbness, cramps, voice fatigue, or swallowing difficulty, followed by long term complications if calcium control remains unstable. Parathyroid disorders also coexist with other endocrine conditions such as diabetes and menopausal bone loss, where skeletal fragility and fatigue tend to be more severe. If you already have an endocrine disorder, parathyroid evaluation should not be overlooked.
Genetic and Familial Conditions
Some parathyroid disorders arise from inherited syndromes. Familial hyperparathyroidism, multiple endocrine neoplasia syndromes, familial hypocalciuric hypercalcemia, autoimmune polyglandular syndromes, pseudohypoparathyroidism, and congenital parathyroid absence are rare but clinically significant. These conditions often present earlier in life and may involve multiple organs. Recognizing them changes management not only for the patient but also for family members who may require screening.
Rare and Severe Complications
Parathyroid carcinoma is rare but aggressive and often presents with severe hypercalcemia, neck mass, hoarseness, dysphagia, profound bone disease, and rapid systemic decline. Calciphylaxis, particularly in patients with advanced kidney disease, represents a catastrophic form of vascular calcification associated with mineral imbalance. Chondrocalcinosis and crystal induced arthritis may occur due to altered calcium and phosphate metabolism, presenting as acute joint inflammation.
Ayurvedic Correlation of Associated Diseases
From an Ayurvedic perspective, these wide ranging disease patterns reflect Asthi Dhatu Kshaya, Majja Dhatu Dushti, Mutravaha Srotas imbalance, and Agni dysfunction. In practice, I observe that Vata aggravation aligns with degeneration, spasms, neurological instability, and weakness, while Kapha and Pitta involvement aligns with stone formation, calcification, inflammation, and metabolic overload. If you integrate this classical understanding with modern diagnostics and safety boundaries, Ayurveda can be applied responsibly to support long term correction rather than superficial symptom suppression.
Ayurvedic Perspective on Parathyroid Disorders
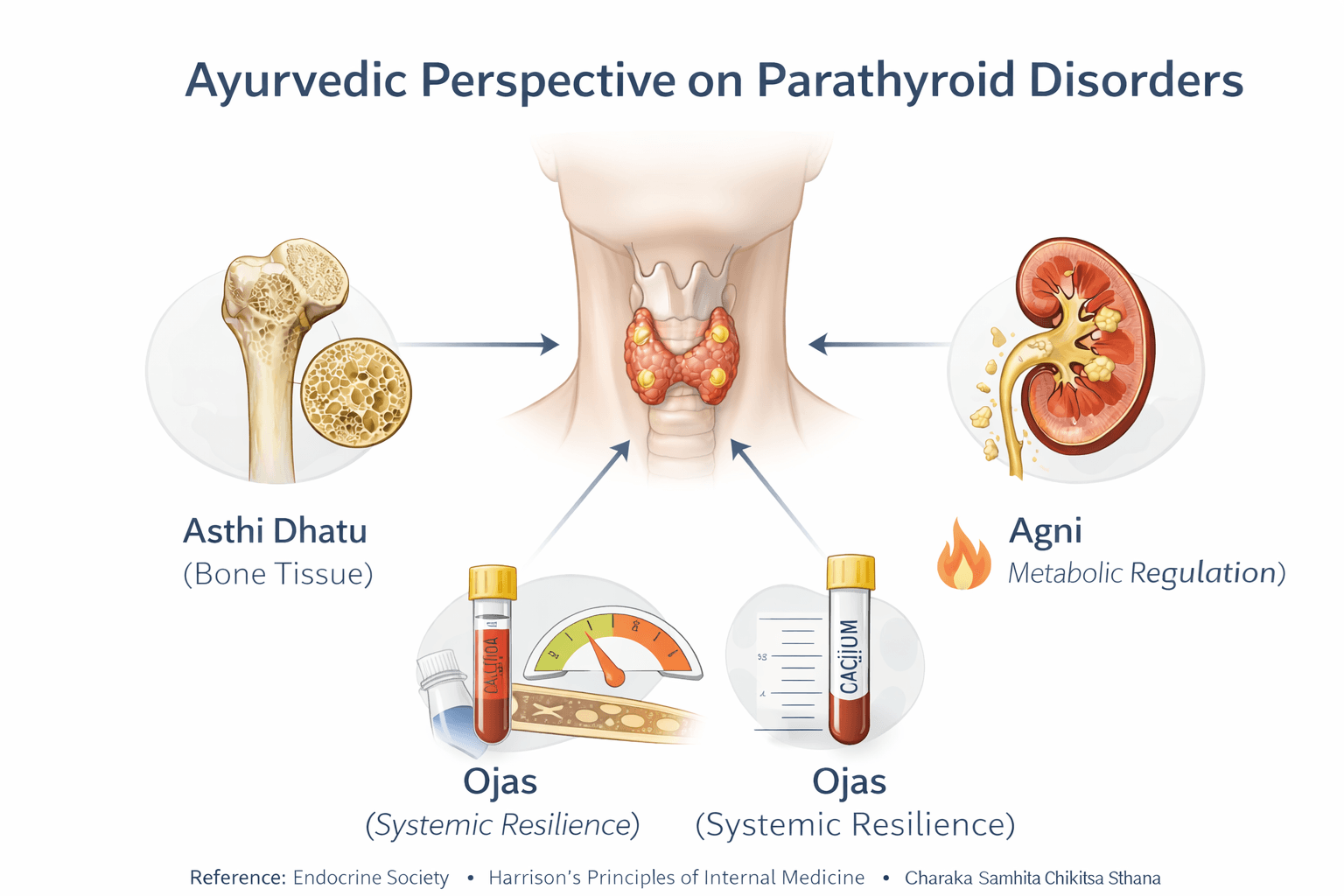
Ayurveda approaches parathyroid disorders not as isolated glandular diseases but as systemic disturbances rooted in Dhatu imbalance, Agni dysfunction, and Srotas obstruction. When I assess such patients, I do not look only at calcium levels. Ayurveda asks why the body has lost its ability to regulate minerals, nourish bone tissue, and maintain neuromuscular stability. If you understand this classical framework, the wide range of bone, kidney, neurological, and metabolic diseases associated with parathyroid disorders becomes logically connected rather than fragmented.
Asthi Dhatu Kshaya as the Foundation of Bone and Calcium Disorders
Asthi Dhatu governs bones, teeth, nails, and all mineralized structures. Classical Ayurveda clearly states that when Asthi Dhatu is depleted, degeneration, pain, and structural weakness follow.
Charaka Samhita Chikitsa Sthana Chapter 28 Asthi Pradoshaja Vikara states
“दन्तभेदः अस्थिभेदः केशरोमलोपः खलित्यम्”
Translation
Disorders arising from vitiation of bone tissue include pain in bones and teeth, loss of hair, and progressive degeneration of structural tissues.
In parathyroid disorders, especially hyperparathyroidism and chronic secondary hyperparathyroidism, excessive bone resorption mirrors this Asthi Dhatu Kshaya. Patients experience osteoporosis, fractures, and chronic bone pain. I consistently observe that calcium supplementation alone does not reverse these conditions unless Asthi Dhatu nourishment is addressed through Rasayana and Agni correction.
Majja Dhatu Dushti and Neuromuscular Instability
Majja Dhatu represents bone marrow and the nervous system. Hypocalcemia and hypoparathyroidism frequently present with spasms, tingling, seizures, anxiety, and cognitive disturbance. Ayurveda classifies these under Majja Dhatu Dushti combined with aggravated Vata Dosha.
Charaka Samhita Sutra Sthana Chapter 17 Dhatu Poshan Adhyaya explains
“मज्जा अस्थीनां पूरकः”
Translation
Majja Dhatu fills and nourishes the bones and supports neurological stability.
If Majja Dhatu is weakened, nerve conduction becomes unstable. You may see seizures or tremors treated symptomatically for years without improvement. In my clinical experience, strengthening Majja Dhatu through Vata pacifying Rasayana brings lasting neuromuscular stability rather than temporary biochemical correction.
Agni Mandya and Failure of Mineral Assimilation
Agni governs digestion, absorption, and tissue transformation. Ayurveda emphasizes that without proper Agni, nutrients cannot be utilized even if intake is sufficient.
Charaka Samhita Chikitsa Sthana Chapter 15 Grahani Chikitsa states
“अग्निमूलं बलं पुंसाम्”
Translation
Agni is the root of strength, health, and nourishment in the human body.
In parathyroid disorders, Agni Mandya leads to improper calcium absorption and erratic mineral metabolism. Patients often report adequate diet and supplements yet continue to show deficiency or imbalance. If you correct Agni, tissue uptake improves naturally and dependence on external supplementation reduces.
Mutravaha Srotas Dushti and Renal Stone Formation
Kidney stones and nephrocalcinosis are hallmark features of hyperparathyroidism. Ayurveda explains this through Mutravaha Srotas Dushti combined with Kapha and Pitta imbalance, leading to abnormal crystallization and obstruction.
Sushruta Samhita Nidana Sthana Chapter 3 Ashmari Nidana describes
“दोषाणां संमूर्छनात् अश्मरी जायते”
Translation
When Doshas accumulate and solidify, stone formation occurs.
In my practice, treating only hydration or stone removal without correcting Srotas pathology leads to recurrence. When Mutravaha Srotas are cleared and metabolism is corrected, recurrence reduces significantly.
Dosha Involvement in Parathyroid Disorders
Parathyroid disorders are rarely single Dosha diseases. Hypoparathyroidism shows dominant Vata aggravation with spasms, tremors, dryness, fear, and instability. Hyperparathyroidism shows Kapha involvement in calcification and stone formation and Pitta involvement in inflammation and tissue breakdown.
Ashtanga Hridaya Sutra Sthana Chapter 12 Dosha Bhediya explains
“वातः पित्तं कफश्चेति त्रयो दोषाः समासतः”
Translation
Vata, Pitta, and Kapha together govern all physiological and pathological processes.
If you treat only one Dosha, the disease shifts rather than resolves. Ayurveda demands individualized Dosha assessment for true cure.
Rasayana Therapy for Long Term Correction
Rasayana is central to curing parathyroid related disorders. It is not a tonic but a therapeutic discipline aimed at rebuilding Dhatus, stabilizing Agni, and restoring resilience.
Charaka Samhita Chikitsa Sthana Chapter 1 Rasayana Adhyaya states
“रसायनं नाम वयसः स्थापकं बलवर्णकरं”
Translation
Rasayana preserves vitality, strengthens tissues, and restores physiological balance.
In Asthi and Majja Dhatu disorders, Rasayana supports bone regeneration, neuromuscular stability, and metabolic correction. I emphasize to patients that Rasayana works gradually and requires discipline. It does not offer overnight biochemical correction but aims at permanent disease resolution.
Ayurvedic Mineral Preparations and Classical Safety Doctrine
Classical texts describe Praval Pishti, Mukta Sukti Bhasma, and Godanti Bhasma for bone and calcium disorders. These are processed medicines, not raw minerals.
Rasa Tarangini Chapter 13 Praval Varga describes proper purification and use of coral based formulations for Asthi related disorders.
Ayurveda strictly warns against unsupervised use. If you self medicate or ignore Agni and Dosha status, even classical medicines can aggravate disease. In my clinical approach, mineral formulations are used only after thorough assessment and always in limited duration.
Less Common and Rare Diseases Associated With Parathyroid Disorders
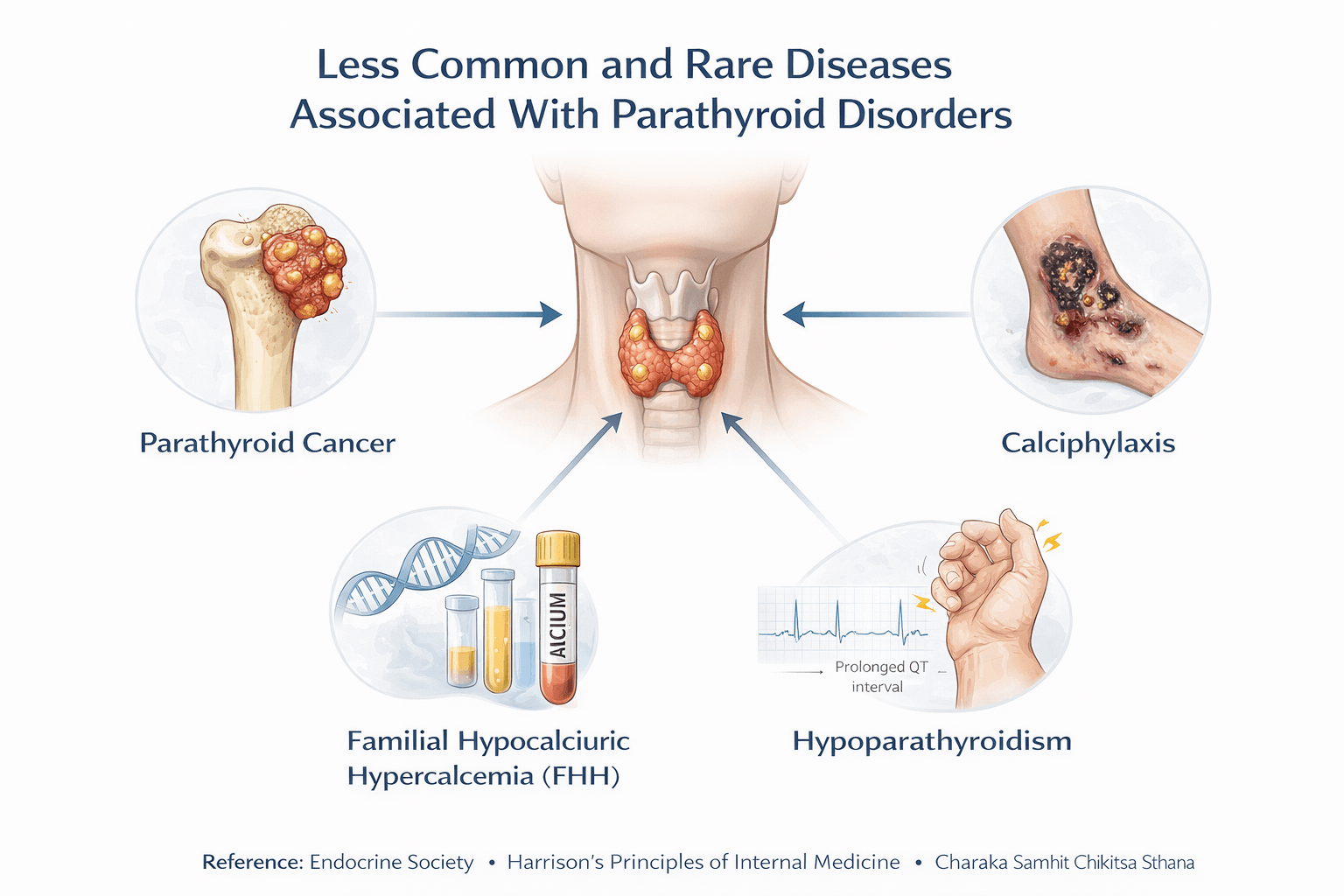
Parathyroid disorders can manifest through a wide range of less common and rare diseases that are frequently overlooked in routine clinical practice. In my experience, these conditions often appear after years of unrecognized hormonal imbalance and are mistakenly treated as isolated orthopedic, neurological, psychiatric, renal, or dermatological disorders. If you are aware of these associations, you can identify severe disease earlier and prevent irreversible damage. Clinicians also rely on these patterns to differentiate mild biochemical imbalance from advanced systemic pathology.
Advanced Skeletal Manifestations and Structural Bone Disease
In prolonged and severe hyperparathyroidism, bone disease progresses beyond osteoporosis into advanced structural damage. Patients may develop osteitis fibrosa cystica with extensive bone resorption, deformities, and pathological fractures. Radiological findings can include subperiosteal bone resorption, tapering of distal clavicles and phalanges, and a characteristic salt and pepper appearance of the skull. These changes can closely mimic malignant bone disease. I have seen patients undergo extensive cancer evaluation before parathyroid hormone excess was identified as the underlying cause. If you encounter destructive bone lesions with elevated calcium levels, parathyroid evaluation becomes mandatory.
Brown Tumors and Focal Bone Lesions
Brown tumors represent localized areas of excessive bone turnover and hemorrhage resulting from prolonged parathyroid hormone excess. They commonly affect the jaw, ribs, pelvis, spine, and long bones. Patients may present with swelling, localized pain, deformity, or fractures. These lesions are reactive rather than neoplastic, and they often regress when hormonal balance is restored. If you recognize them early, unnecessary surgical or oncologic interventions can be avoided.
Rare Neurological and Neuropsychiatric Presentations
Beyond common neuromuscular symptoms, parathyroid disorders can produce rare but severe neurological manifestations. Chronic hypoparathyroidism may lead to intracranial calcification, particularly in the basal ganglia. Patients can present with seizures, movement disorders, tremors, rigidity, gait disturbance, or progressive cognitive decline. Severe hypercalcemia in hyperparathyroidism can precipitate delirium, hallucinations, psychosis, or marked alteration in consciousness. If sudden psychiatric or neurological symptoms occur alongside calcium imbalance, they should never be considered primary psychiatric disease alone.
Raised Intracranial Pressure and Visual Complications
Chronic hypocalcemia can lead to increased intracranial pressure and papilledema. Patients may experience persistent headaches, blurred vision, visual field defects, or transient visual loss. These findings are uncommon and frequently misattributed to primary neurological conditions. If you or your patient has hypocalcemia with unexplained visual symptoms, this rare association should be actively investigated.
Cardiac and Electrical Conduction Abnormalities
Severe disturbances in calcium homeostasis can produce rare but dangerous cardiac complications. Patients may develop prolonged QT interval, ventricular arrhythmias, syncope, or sudden cardiac instability. These manifestations may occur without obvious cardiac disease and can be life threatening if unrecognized. In such cases, correcting calcium and parathyroid hormone imbalance becomes an urgent priority.
Renal and Vascular Calcification Disorders
Longstanding parathyroid dysfunction can lead to extensive soft tissue and vascular calcification. Calciphylaxis is a rare but catastrophic complication seen most often in advanced kidney disease with severe secondary hyperparathyroidism. It presents with painful skin lesions that progress to necrosis, infection, and systemic illness. Mortality remains high even with treatment. If painful skin lesions develop in a patient with kidney disease and mineral imbalance, this diagnosis requires immediate attention.
Genetic and Familial Disorders Affecting Parathyroid Function
Several rare genetic conditions alter parathyroid hormone regulation and calcium metabolism. Familial hypocalciuric hypercalcemia presents with lifelong mild hypercalcemia and low urinary calcium excretion. These patients are often misdiagnosed with primary hyperparathyroidism and may undergo unnecessary surgery. Multiple endocrine neoplasia syndromes involve parathyroid disease along with tumors of other endocrine glands. Pseudohypoparathyroidism represents hormone resistance rather than hormone deficiency and presents with hypocalcemia and characteristic skeletal features. If parathyroid disease appears at a young age or has a strong family history, genetic evaluation becomes essential.
Autoimmune and Congenital Parathyroid Disorders
Autoimmune hypoparathyroidism may occur as part of autoimmune polyendocrine syndromes. Patients can present with hypocalcemia alongside adrenal insufficiency, thyroid disease, chronic mucocutaneous candidiasis, or other immune mediated conditions. Congenital absence or underdevelopment of the parathyroid glands, as seen in DiGeorge syndrome, presents early in life with hypocalcemia, seizures, immune dysfunction, and cardiac anomalies. Early recognition is critical to prevent life threatening complications.
Dermatological, Dental, and Ocular Complications
Chronic hypocalcemia affects ectodermal tissues. Patients may develop dry scaly skin, brittle or deformed nails, hair texture changes, early onset cataracts, and dental enamel defects. These features often progress slowly and are rarely linked back to parathyroid dysfunction unless specifically evaluated. Dentists and ophthalmologists are sometimes the first to suspect an underlying metabolic disorder in such cases.
Rare Malignancy of the Parathyroid Glands
Parathyroid carcinoma is extremely rare but aggressive. It often presents with disproportionately severe hypercalcemia, profound weakness, bone destruction, kidney failure, neck mass, hoarseness, or difficulty swallowing. The severity of systemic manifestations is often greater than expected for benign disease. Early recognition and surgical management are critical for survival.
Clinical Importance of Recognizing Rare Associations
Less common and rare diseases associated with parathyroid disorders usually indicate advanced, long standing, genetic, or systemic disease. If you recognize these patterns early, you can prevent irreversible bone damage, neurological injury, cardiovascular events, and unnecessary procedures. From a clinical standpoint, these associations reinforce that parathyroid disorders are systemic diseases rather than isolated endocrine abnormalities.
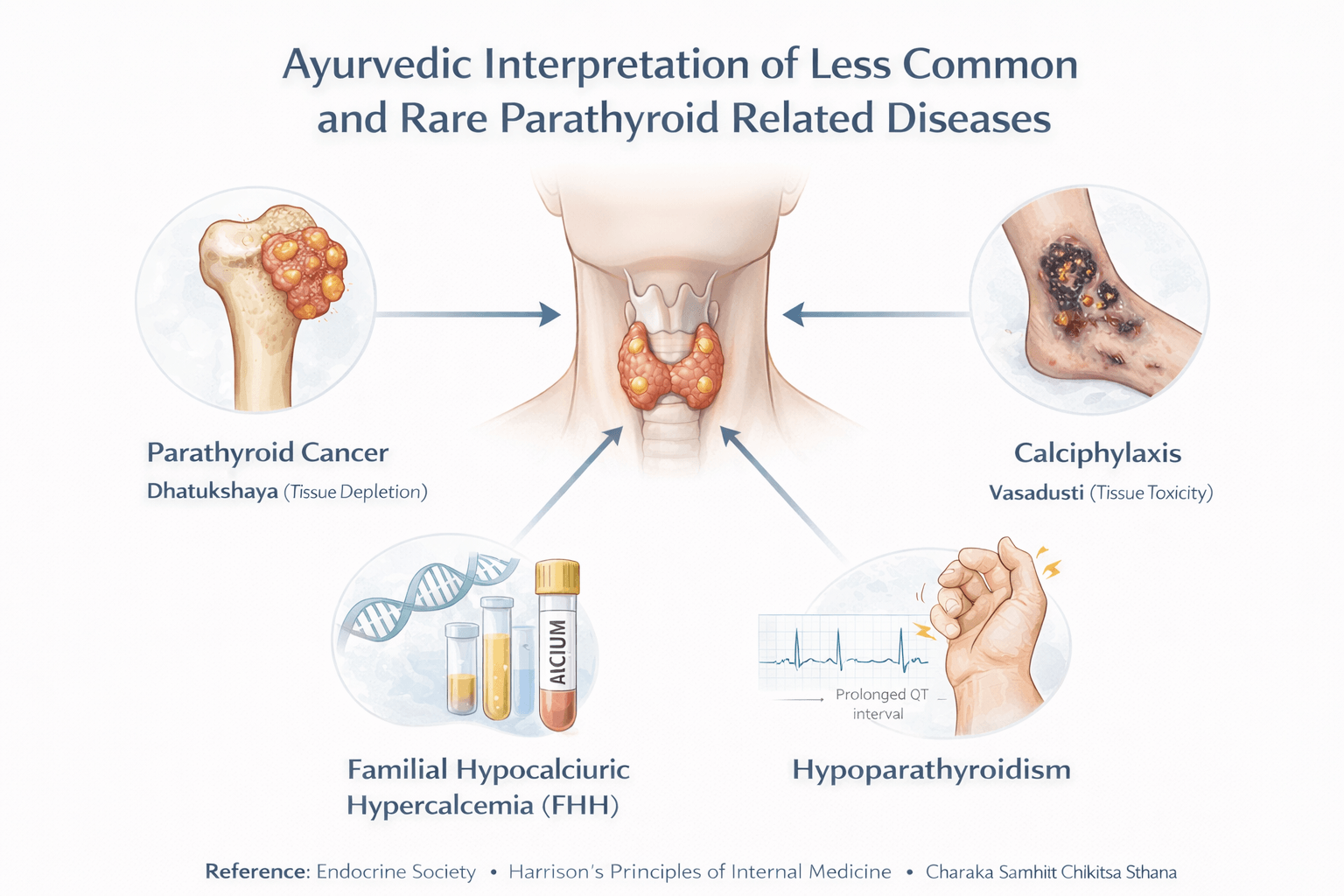
From an Ayurvedic standpoint, the appearance of rare and advanced diseases in parathyroid disorders indicates deep seated imbalance that has crossed beyond superficial metabolic disturbance. In my clinical experience, these manifestations arise when Dosha imbalance, Dhatu depletion, and Srotas obstruction remain uncorrected for prolonged periods. If you view these conditions through Ayurvedic principles, each rare complication reflects a predictable stage of systemic deterioration rather than an isolated event.
Advanced Bone Destruction and Osteitis Fibrosa Cystica
Severe bone destruction and deformities reflect profound Asthi Dhatu Kshaya combined with aggravated Vata Dosha. Ayurveda explains that when Asthi Dhatu loses nourishment, the body responds with excessive internal catabolism, leading to bone resorption, pain, deformity, and instability. Brown tumors and cystic bone changes represent localized failure of Asthi and Majja Dhatu integration. If this stage is reached, simple nourishment is insufficient. Rasayana aimed at Asthi and Majja Dhatu along with Vata pacification becomes essential for any chance of structural recovery.
Neurological Calcification and Movement Disorders
Basal ganglia calcification, seizures, tremors, and movement disorders are interpreted as Majja Dhatu Dushti with severe Vata aggravation. Ayurveda describes Majja as responsible for nerve conduction, mental stability, and motor control. When calcium metabolism fails, Majja Dhatu becomes depleted and unstable. You may see neurological symptoms that appear irreversible. In reality, Ayurvedic therapy focuses on stabilizing Vata, nourishing Majja, and restoring Agni to prevent further neurological decline.
Severe Psychiatric and Cognitive Manifestations
Delirium, hallucinations, psychosis, and profound cognitive impairment reflect combined Vata and Pitta disturbance affecting Manovaha Srotas. Ayurveda recognizes that the mind and nervous system are deeply influenced by metabolic heat and dryness. When mineral imbalance persists, mental symptoms emerge as systemic pathology rather than isolated psychiatric illness. If you treat only the mind, symptoms persist. When Dosha balance and Dhatu nourishment are restored, mental clarity often improves significantly.
Raised Intracranial Pressure and Visual Disturbance
Headache, papilledema, and visual impairment seen in chronic hypocalcemia represent obstruction of Majjavaha and Rasavaha Srotas. Ayurveda explains that improper fluid circulation combined with Vata instability leads to pressure phenomena within confined spaces such as the cranial cavity. If you ignore this stage, permanent visual damage may occur. Early correction of Agni and Srotas flow is crucial.
Cardiac Rhythm Disturbance and Sudden Instability
Arrhythmias and electrical instability of the heart reflect Prana Vata dysfunction combined with Rakta and Ojas depletion. Ayurveda considers the heart the seat of Prana and consciousness. When calcium regulation fails, Prana Vata becomes erratic, leading to rhythm disturbance. In such cases, Rasayana aimed at stabilizing Prana and strengthening Ojas is as important as biochemical correction.
Vascular Calcification and Calciphylaxis
Calciphylaxis and widespread vascular calcification indicate severe Kapha and Pitta involvement with Mutravaha and Raktavaha Srotas Dushti. Ayurveda describes this as pathological solidification where substances meant for nourishment instead obstruct circulation. Painful skin necrosis represents the final stage of tissue starvation. If you reach this stage, therapy must focus on clearing Srotas obstruction, cooling Pitta, and restoring metabolic discrimination.
Genetic and Hormone Resistance Disorders
Conditions such as pseudohypoparathyroidism and familial calcium regulation disorders reflect Beej Dushti meaning congenital or hereditary disturbance at the foundational level. Ayurveda acknowledges that such disorders require lifelong management rather than short term correction. If you identify Beej Dushti early, progression into severe Dhatu damage can be slowed through tailored Rasayana and lifestyle regulation.
Autoimmune and Congenital Gland Failure
Autoimmune hypoparathyroidism and congenital absence of parathyroid tissue reflect failure of Ojas and immune regulation. Ayurveda interprets this as deep seated Agni collapse affecting immune tolerance. Patients often show multi organ involvement. In such cases, Rasayana focused on immune balance and tissue resilience becomes the core strategy rather than symptom suppression.
Dermatological, Dental, and Ocular Manifestations
Dry skin, brittle nails, enamel defects, and early cataracts reflect Rasa and Asthi Dhatu malnourishment. Ayurveda teaches that when foundational Dhatus are weak, external tissues reveal early warning signs. If you observe these features, they should prompt evaluation of deeper metabolic imbalance rather than cosmetic treatment alone.
Rare Malignancy of the Parathyroid Glands
Parathyroid carcinoma represents uncontrolled Dhatu proliferation driven by deranged Pitta and Kapha under the influence of chronic Agni distortion. Ayurveda recognizes such growth as loss of cellular intelligence rather than random mutation. While modern surgery is mandatory, Ayurvedic intervention focuses on preventing recurrence by restoring metabolic order and tissue regulation.
Modern Medical Management
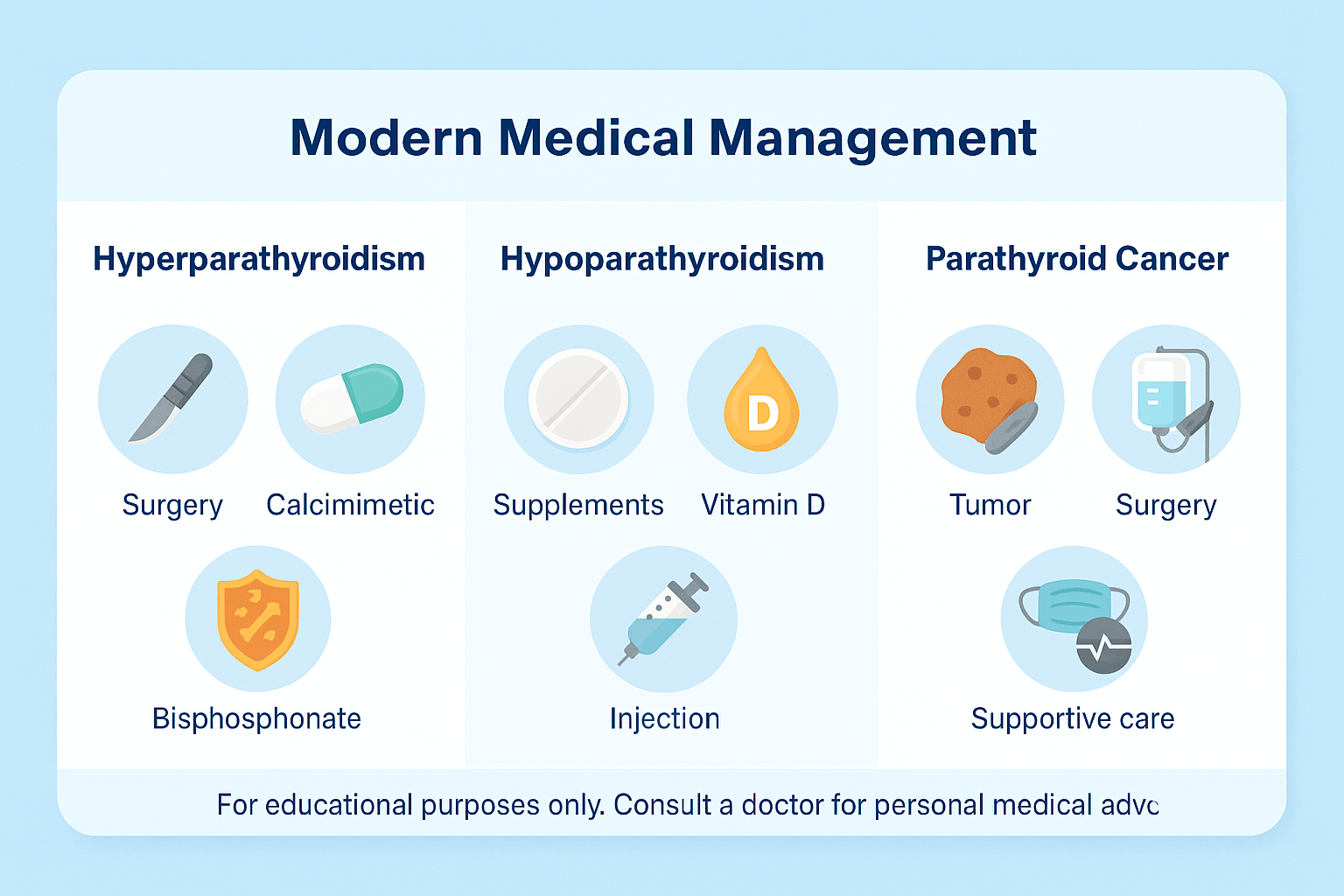
Treatment for parathyroid disorders depends on whether the glands are overactive, underactive, or affected by cancer. The main goal is to restore normal calcium balance while preventing long-term complications.
Hyperparathyroidism
The most effective treatment for primary hyperparathyroidism is surgery to remove the overactive gland. Parathyroidectomy is usually recommended if calcium levels are very high, if bone or kidney complications are present, or if the patient is young.
For people who cannot have surgery, medications may help. Calcimimetics, such as cinacalcet, reduce parathyroid hormone release and lower calcium levels. Bisphosphonates may be prescribed to protect bone strength by slowing down calcium loss from bones.
Hypoparathyroidism
Management focuses on raising calcium levels and keeping them stable. Most patients take lifelong calcium supplements along with active forms of vitamin D to improve calcium absorption. In some cases, recombinant parathyroid hormone (PTH) injections are used, particularly when standard supplements are not enough to control symptoms.
Parathyroid cancer
Treatment is more complex because the disease is rare and often aggressive. Surgery is the main option, with complete removal of the cancerous gland and sometimes surrounding tissue. After surgery, patients may still need supportive therapies to manage persistent high calcium levels, which can include hydration, bisphosphonates, or calcimimetics. Long-term monitoring is essential because the cancer often comes back.
Prognosis, Disease Progression, and Quality of Life
Parathyroid disorders are rarely static. They tend to evolve over time, sometimes slowly and silently, sometimes with a pattern of recurring symptoms, cumulative tissue damage, and progressive loss of physiological balance. From a patient perspective, this is one of the most important sections in the article because prognosis is never just about survival or lab normalization. It is about whether the person can regain strength, prevent recurrence, protect bone and kidney health, restore confidence, and return to a normal daily life without living in constant fear of the next complication.
A strong prognosis section must therefore do more than reassure. It must explain what tends to happen if the condition is recognized early, what usually worsens if treatment is delayed, how quality of life is affected, and why long term outcomes depend not only on diagnosis but also on timing, disease type, tissue damage, and the depth of correction achieved.
Prognosis Depends on the Type of Parathyroid Disorder
The outlook varies significantly depending on whether the patient has primary hyperparathyroidism, secondary hyperparathyroidism, tertiary hyperparathyroidism, hypoparathyroidism, or a rare malignant condition. In primary hyperparathyroidism, the long term outlook is often favorable when the underlying gland abnormality is recognized and managed appropriately. However, favorable does not mean harmless. Many patients live for years with silent bone loss, subtle neurocognitive decline, recurrent kidney stones, or chronic fatigue before the diagnosis is made. By the time treatment begins, the hormonal disturbance may already have left a structural footprint.
In secondary hyperparathyroidism, the prognosis is closely tied to the severity and reversibility of the underlying cause, especially chronic kidney disease. Here, the parathyroid glands are often reacting to a larger metabolic crisis. This means outcomes are shaped not only by hormone control but also by phosphate balance, vitamin D handling, vascular health, kidney reserve, and long term systemic burden. In tertiary hyperparathyroidism, the condition becomes even more complex because the glands may continue to overproduce hormone despite the original trigger having changed or partially improved.
In hypoparathyroidism, prognosis depends heavily on whether the condition is temporary or permanent, whether it follows surgery or autoimmune dysfunction, and how stable calcium control remains over time. Some patients regain function. Others require long term management and careful monitoring to prevent recurrent neuromuscular symptoms, renal complications from overtreatment, and quality of life deterioration.
Early Disease Often Looks Mild but Is Not Truly Benign
One of the most misleading aspects of parathyroid disease is that early stage illness can appear deceptively mild. A patient may feel only slightly tired, mentally dull, constipated, or irritable. Another may have a first kidney stone that is treated as a one time event. Another may show mild calcium or parathyroid hormone imbalance on routine blood work and be told it is not serious enough to matter.
This is where disease progression becomes clinically important. Mild symptoms do not always indicate mild biological consequences. Bone may continue losing density. Renal calcification may quietly develop. Mood and cognitive symptoms may deepen gradually. Muscle weakness, sleep disturbance, and loss of vitality may become normalized by the patient simply because they have adapted to feeling unwell for so long. In strategic terms, parathyroid disorders often extract their cost slowly enough to avoid urgent alarm, but steadily enough to damage long term well being.
Delayed Diagnosis Changes the Course of the Disease
Timing influences prognosis more than many patients realize. When the disorder is detected early, there is often more opportunity to prevent fractures, preserve kidney function, reduce symptom burden, and avoid the emotional exhaustion that comes from years of unanswered complaints. When diagnosis is delayed, the condition often shifts from a metabolic problem to a structural problem.
At that stage, the patient is no longer dealing only with hormone imbalance. They may now have osteoporosis, fragility fractures, recurrent stone disease, nephrocalcinosis, chronic anxiety about symptoms, sleep disruption, reduced confidence in mobility, or persistent cognitive and emotional fatigue. This is why delayed recognition is not a neutral event. It changes the disease narrative from correction to recovery from accumulated damage.
Bone Health and Skeletal Outcome
Bone is one of the most vulnerable long term targets of parathyroid dysfunction. In hyperparathyroid states, persistent hormonal excess accelerates bone resorption and may gradually erode skeletal integrity. Patients may first present with osteopenia, but progression to osteoporosis, chronic bone pain, vertebral compression, and fragility fractures is a real concern. In more advanced or neglected disease, structural deformity and severe mineral depletion may emerge.
Even when the hormonal problem is later corrected, skeletal recovery is not always immediate or complete. Bone remodeling takes time. Older age, menopause, poor nutrition, low muscle mass, chronic inflammation, and limited mobility can all slow recovery. This means prognosis for bone health depends not only on treatment of the gland or metabolic cause, but also on how much structural damage already exists when care begins.
Kidney Outcome and Risk of Recurrence
The kidney is another major determinant of prognosis. In hypercalcemic states, persistent mineral stress may lead to recurrent stones, nephrocalcinosis, dehydration related decline, and chronic renal burden. Patients who have already formed multiple stones often live with fear of recurrence, repeated imaging, dietary confusion, and anxiety about long term kidney damage.
If the underlying parathyroid disorder is corrected early, the risk of ongoing stone formation can be reduced substantially. However, if the patient has preexisting chronic kidney disease or severe longstanding mineral dysregulation, renal prognosis becomes more guarded. This is particularly relevant in secondary and tertiary hyperparathyroidism, where kidney disease is not just an associated condition but a central driver of the hormonal disturbance.
Neuromuscular Stability and Daily Function
In hypoparathyroidism and severe calcium instability, prognosis is strongly shaped by neuromuscular control. Muscle cramps, paresthesia, tetany, weakness, tremors, and seizure risk do not merely affect symptoms. They affect independence, work ability, driving confidence, sleep quality, emotional safety, and daily functioning. A patient who never knows when tingling, cramping, or instability will return does not feel truly well, even if some lab values improve.
This is why quality of life must be discussed directly. Many patients do not fear the diagnosis as much as they fear unpredictability. They want to know whether they can live normally, exercise safely, travel, think clearly, sleep well, and avoid repeated emergency care. Prognosis improves significantly when calcium control becomes more stable, triggers are reduced, and treatment is individualized rather than purely reactive.
Cognitive and Emotional Quality of Life
Parathyroid disorders can profoundly affect how a person feels mentally and emotionally. Chronic fatigue, irritability, low mood, anxiety, poor concentration, memory difficulty, and a sense of reduced resilience are common complaints. These symptoms are often minimized because they are less visible than a fracture or a seizure, yet from a quality of life perspective they may be just as disabling.
Many patients lose trust in their own body long before they receive a diagnosis. They begin to wonder whether the problem is stress, aging, burnout, or something psychological. When the endocrine basis is finally recognized, there is often relief, but also frustration about lost time. Prognosis therefore includes more than tissue recovery. It includes emotional recovery, restoration of self trust, and the patient’s belief that lasting improvement is possible.
Prognosis in Post Surgical and Chronic Cases
Patients who develop hypoparathyroidism after thyroid surgery often ask whether the condition will resolve or remain permanent. The answer depends on the degree of gland injury, vascular compromise, and recovery potential. Some regain partial or full function over time. Others remain dependent on long term calcium and vitamin D management. The quality of that management then becomes a major determinant of prognosis.
In chronic cases, especially those involving kidney disease, recurrent stones, autoimmune dysfunction, or significant bone depletion, prognosis is more complex. The goal is not only symptom control but long term stabilization. In these patients, the concept of cure, recovery, and remission must be approached with honesty and precision. Some systems can recover fully. Others can improve substantially but still require continued vigilance.
Quality of Life Improves When Treatment Becomes Individualized
One of the strongest predictors of better long term outcome is individualized care. Patients do worse when they are treated according to generic assumptions. They do better when disease type, stage, age, kidney status, bone reserve, digestive function, medication burden, stress load, and metabolic context are all taken seriously.
This is true in both modern and Ayurvedic management. In modern medicine, individualized care determines whether the patient is observed, supplemented, surgically referred, or more closely monitored for complications. In Ayurveda, individualized care determines whether the primary focus should be on Agni correction, Vata stabilization, Rasayana support, Srotas clearance, Ojas enhancement, or staged mineral support under supervision. In both systems, personalization is not a luxury. It is the difference between surface management and meaningful recovery.
The Real Long Term Outlook
The long term outlook for parathyroid disorders is best understood as a spectrum rather than a fixed prediction. Some patients recover with minimal long term damage when the disorder is recognized early and managed intelligently. Others continue to live with complications that could have been reduced through earlier intervention. The key message is that prognosis is not determined by the diagnosis alone. It is determined by how long the disease has been active, how much damage has already occurred, whether the underlying cause has been identified correctly, and whether treatment addresses both the immediate biochemical problem and the deeper terrain in which the disorder developed.
For international patients seeking integrative care, this section matters because it reframes prognosis from passive waiting to active strategy. Better outcomes are possible, but they depend on timing, accuracy, and sustained individualized management.
Why the Condition Often Persists or Recurs
Parathyroid disorders often persist or return because the visible laboratory abnormality is only the surface expression of a deeper imbalance. Many patients focus on calcium alone, while the real drivers may include chronic kidney dysfunction, weak digestion and metabolism, recurrent inflammation, poor nutrient assimilation, ongoing stress, surgical injury, or long standing tissue depletion. In my clinical experience, recurrence is far more likely when treatment targets only the immediate number on the blood report and not the full chain of causation. If you want durable recovery, you have to understand why the terrain of the body keeps recreating the same disorder.
Table : Why Many Patients Do Not Improve Despite Treatment
| Key Factor | What Happens | What Needs Correction |
|---|---|---|
| Calcium Regulation Issues | Levels fluctuate despite treatment | Improve regulation, not just numbers |
| Weak Metabolism (Agni) | Poor absorption of nutrients | Restore digestion and metabolism |
| Bone Depletion | Ongoing weakness and fracture risk | Strengthen bone tissue |
| Kidney Stress | Stones and imbalance persist | Support renal function |
| Hormonal Imbalance | PTH remains unstable | Correct systemic regulation |
| Chronic Disease | Multiple conditions worsen outcomes | Integrated treatment approach |
Incomplete Correction of the Original Cause
One of the most common reasons for persistence is that the root trigger remains active. If a patient has primary hyperparathyroidism from a gland abnormality, the hormonal excess may continue until that source is addressed properly. If the patient has secondary hyperparathyroidism from chronic kidney disease, vitamin D deficiency, poor phosphate balance, or malabsorption, then calcium correction alone will not solve the problem. The gland is responding to an ongoing message of internal imbalance.
This is equally true in post surgical hypoparathyroidism. If the gland has been injured or its blood supply compromised, short term symptom control does not automatically restore endocrine stability. Some patients improve, while others remain vulnerable to fluctuations for months or years. In practical terms, recurrence often means the original driver was reduced but never truly corrected.
Agni Imbalance and Poor Metabolic Assimilation
Ayurveda places enormous emphasis on Agni, meaning digestive and metabolic fire, which you may explain to international readers as the body’s ability to digest, absorb, transform, and utilize nutrients. In Urdu this idea is close to hazm ki quwwat, and in Arabic a useful explanatory phrase is quwwat al hadm wa al istihalah, meaning digestive and transformative power. If Agni is disturbed, even a good diet or medicine may fail to nourish the tissues properly.
Charaka Samhita, Chikitsa Sthana, Grahani Chikitsa, Chapter 15 states:
अग्निमूलं बलं पुंसाम्
Transliteration:
Agnimoolam balam punsaam
Translation:
Agni is the root of human strength.
This brief statement carries major clinical significance. If metabolic fire is weak, calcium may be consumed but not properly assimilated, vitamin D may be prescribed but not optimally utilized, and tissue repair may remain incomplete. In such a state, the patient feels trapped in a cycle of temporary improvement followed by relapse. I often see this in individuals with chronic bloating, constipation, weak appetite, gut inflammation, erratic eating, or long standing digestive suppression. They may be taking the right medicines, but the body is not processing them efficiently enough to create durable change.
Ama Formation and Chronic Internal Toxicity
Another major reason for recurrence is Ama, which you can describe in English as toxic or pathological metabolic residue produced by incomplete digestion and incomplete tissue transformation. In Urdu, one may explain it as ghair hazm fuzlat ya zehri madda, and in Arabic as fadlat ghayr mahduma or maddah samiyyah natijah an su al hadm. Ama blocks physiological intelligence. It interferes with proper tissue nutrition, obstructs channels, disturbs immunity, and keeps disease mechanisms active beneath the surface.
Ashtanga Hridaya, Sutra Sthana, Chapter 13 gives the classical warning:
रोगाः सर्वे अपि मन्दे अग्नौ
Transliteration:
Rogaah sarve api mande agnau
Translation:
All diseases arise when Agni becomes weak.
For a parathyroid patient, this means recurrence is not only about the gland. It may also reflect a chronic internal state in which digestion is poor, tissue transformation is incomplete, and inflammatory residue keeps disturbing mineral handling. If Ama persists, then even after temporary stabilization the body may drift back into imbalance.
Dosha Instability and Failure to Rebalance the System
Parathyroid disorders often recur when the underlying Dosha pattern has not been corrected. In simple language, Doshas are the governing physiological principles of movement, transformation, and structure. Vata governs movement and nervous regulation, Pitta governs metabolism and transformation, and Kapha governs structure, fluidity, and stability. In Urdu and Arabic explanation for global patients, you may say these are functional regulatory patterns rather than mystical ideas.
In hypoparathyroid states, Vata often remains aggravated, producing tingling, spasms, fear, dryness, weakness, and instability. In hyperparathyroid states, Pitta and Kapha may combine with Vata to produce tissue breakdown, stone formation, metabolic irritation, and obstructed pathways. If the patient is treated only with a general tonic or general calcium support without correcting this pattern, the disease often shifts shape rather than resolves.
Ashtanga Hridaya, Sutra Sthana, Chapter 1 states:
वायुः पित्तं कफश्चेति त्रयो दोषाः समासतः
Transliteration:
Vaayuh pittam kaphash cha iti trayo doshaah samaasatah
Translation:
Vata, Pitta, and Kapha are the three governing Doshas in the body.
This matters because recurrence often indicates that the biochemical expression changed, but the Dosha terrain did not.
Srotas Obstruction and Poor Tissue Delivery
Ayurveda also teaches that disease persists when Srotas, meaning the channels of transport and communication in the body, remain obstructed. For global readers, you can explain Srotas as functional pathways that carry nutrients, wastes, signals, and tissue support throughout the system. In Urdu this can be related to jismi raaste ya nizaami guzargahen, and in Arabic to masarat al naql wa al tawasil al jasadi.
When these pathways are blocked, minerals may deposit in the wrong places, such as kidneys or vessels, while bones and nerves remain undernourished. This is one reason why a patient may have both calcification and weakness at the same time. The body is not simply deficient or excessive. It is distributing resources incorrectly.
Sushruta Samhita, Sutra Sthana, Chapter 15 teaches the importance of unobstructed pathways in health, and classical Ayurvedic pathology repeatedly shows that obstruction leads to misdirection of nutrition and disease progression. In clinical language, recurrence often means the channel problem was never truly addressed.
Asthi and Majja Dhatu Depletion
Many parathyroid cases persist because structural tissues have already become deeply depleted. Asthi Dhatu means bone tissue, and Majja Dhatu refers broadly to marrow and deeper neurological nourishment. In Urdu explanatory language, Asthi Dhatu can be described as haddiyon ka baft, and Majja Dhatu as haddi ka guda aur asabi ghiza. In Arabic, bone tissue may be explained as nسيج al izam and marrow nourishment as ghidha al نخاع wa al aasab.
Charaka Samhita and other classical texts repeatedly emphasize that when Dhatus are weak, disease becomes chronic. Even if the immediate trigger is reduced, relapse occurs because the tissues themselves remain too fragile to hold stability. A patient whose bones are depleted, nerves are irritable, sleep is poor, and vitality is low may appear “controlled” on paper while still being biologically vulnerable. Unless Asthi and Majja are rebuilt, recurrence remains likely.
Chronic Stress and Ojas Depletion
Stress is not a superficial lifestyle issue in endocrine disease. It changes sleep, digestion, inflammatory tone, adrenal signaling, compliance with treatment, and emotional resilience. In my experience, many relapses follow periods of prolonged worry, overwork, poor sleep, grief, or fear. For international patients, this point is very important because modern stress patterns are often constant and normalized.
Ayurveda explains long term resilience through Ojas, the refined essence of all tissues and the foundation of vitality, immunity, and stability. In Urdu it may be explained as quwwat e hayat or jismani madafati quwwat ka lutf, and in Arabic as jawhar al quwwah wa al manaa. When Ojas is depleted, recovery becomes shallow and relapse becomes easier.
Charaka Samhita, Sutra Sthana, Chapter 17 states:
ओजो हि सर्वधातूनां सारः
Transliteration:
Ojo hi sarvadhatoonaam saarhah
Translation:
Ojas is the essence of all the Dhatus.
If the patient remains exhausted, frightened, inflamed, sleep deprived, and nutritionally unstable, the endocrine system loses resilience. This is one reason a technically correct treatment may still fail in a chronically stressed person.
Wrong Diet and Lifestyle Continuation
A major reason for recurrence is simple but powerful: the patient continues the same aggravating diet and lifestyle that helped create the disorder in the first place. Irregular meals, poor hydration, excess salt, excessive processed food, sedentary living, inadequate sunlight exposure, chronic sleep disruption, and long standing neglect of digestion all make stable recovery more difficult.
Ayurveda calls the first and most essential treatment principle Nidana Parivarjana, meaning removal of the cause. In plain English, this means that cure is impossible if the causative pattern remains active. In Urdu, this idea can be explained as sabab ko door karna, and in Arabic as izalat al sabab.
Charaka Samhita, Sutra Sthana, Chapter 16 teaches that the first principle of treatment is to remove the causative factors. This becomes especially relevant in patients who want herbal or mineral support while continuing the same damaging routine. The body cannot maintain improvement if the daily environment keeps pushing it back toward imbalance.
Inadequate Personalization of Treatment
Parathyroid disorders recur when treatment is generic. One patient is older with osteoporosis and constipation. Another is post thyroidectomy with low calcium and spasms. Another has chronic kidney disease and phosphate retention. Another is stressed, depleted, and poorly nourished despite supplements. These are not the same patient. They should not receive the same formula, the same dose, the same timing, or the same dietary advice.
This is one reason market purchased Avaleha and unsupervised self treatment fail so often. They do not account for age, disease duration, severity, renal status, surgery history, medication use, Dosha pattern, digestive strength, and tissue depletion. Without personalization, the patient may feel some temporary symptomatic benefit, but the deeper drivers remain active, and recurrence follows.
Poor Follow Up and Lack of Monitoring
A disease may appear improved while still progressing silently. This is especially true in bone loss, renal calcification, and fluctuating calcium states. Patients often stop monitoring once symptoms reduce. In chronic cases, this becomes dangerous. Stability must be verified, not assumed.
From a modern perspective, recurrence persists when calcium, phosphate, kidney function, vitamin D, and sometimes urinary markers are not followed properly. From an Ayurvedic perspective, recurrence persists when visible symptom reduction is mistaken for Samprapti Vighatana, meaning full reversal of the disease process. True correction requires both internal and external confirmation.
Charaka Samhita, Chikitsa Sthana explains the principle:
सम्प्राप्तिविघटनमेव चिकित्सा
Transliteration:
Samprapti vighatanam eva chikitsa
Translation:
True treatment is the reversal of the disease process.
This is the deepest answer to persistence. A patient relapses because the disease pathway was softened, not fully reversed.
Why This Matters for Patients Seeking Ayurveda
Patients from the USA, UK, Canada, Australia, and Singapore often seek Ayurveda when they feel trapped between symptom control and long term uncertainty. This section matters because it explains that recurrence is not a personal failure and not always a treatment failure. It is often a sign that the disease was approached too narrowly, too late, or without enough personalization.
Ayurveda offers value here because it forces a broader view. It asks whether digestion is strong, whether inflammation is building, whether channels are blocked, whether bone and nerve tissues are weak, whether stress has depleted Ojas, and whether the patient’s daily routine is silently sustaining the disease. When these questions are addressed seriously, the chance of durable recovery improves.
Ayurvedic Treatment Principles

Ayurvedic treatment for parathyroid disorders is not built on a single medicine or a single symptom target. It is built on a therapeutic sequence. In my clinical view, this is where Ayurveda differs most clearly from fragmented care. It does not ask only how to suppress cramps, reduce stones, or stabilize calcium for a short time. It asks what disturbed the system, which tissues were weakened, which channels were blocked, which metabolic processes became inefficient, and how the body can be guided back toward stable function. If you explain this well to an international patient, the logic of Ayurveda becomes much easier to trust because it sounds like a coherent medical strategy rather than a collection of herbs.
For global readers, it is useful to explain that Ayurvedic treatment principles are broad therapeutic rules that guide individualized care. In Urdu, one may describe them as usool e ilaj, and in Arabic as usul al ilaj, meaning principles of treatment. These principles are not decorative theory. They determine what should be corrected first, what should be strengthened later, and what must never be ignored if cure is the goal.
Nidana Parivarjana, Removal of the Cause
The first and most important Ayurvedic principle is Nidana Parivarjana, which in English means removal of the causative factors. In Urdu, this may be explained as sabab ko door karna, and in Arabic as izalat al sabab. This principle is strategically powerful because it prevents the physician from treating effects while allowing the cause to continue.
Charaka Samhita, Sutra Sthana, Chapter 16 gives the therapeutic foundation:
संक्षेपतः क्रियायोगो निदानपरिवर्जनम्
Transliteration:
Sankshepatah kriyayogo nidana parivarjanam
Translation:
In brief, treatment begins with removal of the causative factors.
In parathyroid disorders, this means the physician must identify whether the ongoing driver is glandular overactivity, vitamin D deficiency, chronic kidney disease, post surgical gland injury, chronic metabolic strain, poor diet, sleep deprivation, emotional stress, improper supplementation, or long standing digestive weakness. If you continue the same pattern that helped create the disease, no formulation can produce lasting recovery. This is why Ayurveda insists on changing the terrain, not merely adding medicine to a harmful routine.
Dosha Balancing, Restoring Functional Regulation
The second principle is correction of the disturbed Doshas. In English, Doshas may be explained as the three governing regulatory patterns of the body. In Urdu, they may be described simply as jismani nizaam ke bunyadi mizaji usool, and in Arabic as al anmat al tanzimiyyah al asasiyyah fil badan. For practical understanding, Vata relates to movement and nerve regulation, Pitta to transformation and metabolic heat, and Kapha to structure, stability, and accumulation.
Ashtanga Hridaya, Sutra Sthana, Chapter 1 states:
वायुः पित्तं कफश्चेति त्रयो दोषाः समासतः
Transliteration:
Vaayuh pittam kaphash cha iti trayo doshaah samaasatah
Translation:
Vata, Pitta, and Kapha are the three Doshas of the body.
In hypoparathyroid patterns, Vata often dominates, producing spasms, tingling, tremulousness, anxiety, dryness, sleep disturbance, and instability. In hyperparathyroid patterns, Vata may combine with Pitta and Kapha, contributing to tissue depletion, inflammatory irritation, stone formation, calcific tendencies, sluggish distribution, and metabolic misdirection. If the physician does not identify which Dosha pattern is primary, the treatment may partially relieve one symptom while aggravating another. This is why individualized Dosha balancing is not optional. It is central to Ayurvedic precision.
Agni Deepana and Pachana, Correcting Digestion and Metabolic Processing
Before tissues can be rebuilt, the body must be able to process nutrition and medicine correctly. Ayurveda therefore places major emphasis on Agni Deepana and Pachana. In English, this means kindling digestive and metabolic fire and clearing incompletely processed residues. In Urdu, these ideas relate to hazm ko mazboot karna and ghair hazm maddon ko saaf karna. In Arabic, one may explain them as taqwiyat al hadm and tahsin al istihalah wa izalat al fadlat.
Charaka Samhita, Chikitsa Sthana, Chapter 15 states:
अग्निमूलं बलं पुंसाम्
Transliteration:
Agnimoolam balam punsaam
Translation:
Agni is the root of human strength.
This principle is especially important in parathyroid disorders because many patients have poor assimilation despite taking supplements or following apparently reasonable diets. If digestion is weak, tissues remain undernourished even when medicine is being taken. If metabolism is disordered, calcium may be present in the body but not utilized where it is needed. In clinical terms, this is one reason patients can show both deficiency and pathological deposition at the same time. Ayurveda addresses this paradox by correcting Agni before expecting durable tissue response.
Ama Pachana, Clearing Pathological Metabolic Residue
When digestion and tissue metabolism are impaired, Ama forms. In English, Ama can be described as pathological metabolic residue that blocks healthy functioning. In Urdu, a practical explanation is ghair hazm fuzlat ya zehri madda, and in Arabic fadlat ghayr mahduma. Ama contributes to sluggishness, inflammation, blocked channels, poor tissue response, and recurrence.
Ashtanga Hridaya, Sutra Sthana, Chapter 13 states:
रोगाः सर्वे अपि मन्दे अग्नौ
Transliteration:
Rogaah sarve api mande agnau
Translation:
All diseases arise when Agni becomes weak.
In parathyroid disorders, Ama may show itself through chronic heaviness, poor digestion, coated tongue, inflammatory tendencies, brain fog, poor responsiveness to treatment, and unstable recurrence. If Ama is not addressed, Rasayana therapy may not penetrate properly, and even otherwise well selected medicines may act weakly. This is why Ayurveda often begins with correction and clearance before deep nourishment.
Srotoshodhana, Clearing the Channels
The next treatment principle is Srotoshodhana, meaning purification and opening of the channels. In English, Srotas are the body’s functional transport pathways. In Urdu, you may explain them as jismani raaste ya guzargahen, and in Arabic as masarat al naql wa al tawasil. Their proper function is essential for delivering nutrition to the right tissues and preventing abnormal accumulation in the wrong places.
In parathyroid disorders, this principle is highly relevant. When minerals are not handled properly, stones may form, calcification may occur, tissues may remain depleted, and the body may fail to distribute nourishment intelligently. The clinical logic is simple. A blocked or distorted transport system cannot maintain stable health. Therefore, Ayurveda seeks not only to provide medicine, but to reopen the pathways through which medicine and nutrition must travel.
Classical Ayurvedic physiology repeatedly emphasizes that when Srotas are unobstructed, tissue nutrition improves, elimination becomes more efficient, and systemic balance becomes easier to restore. In a patient with recurrent stones, chronic constipation, edema, poor absorption, vascular burden, or sluggish tissue response, Srotoshodhana becomes a major therapeutic priority.
Vyadhi Pratyanika Chikitsa, Disease Specific Opposition
Ayurveda also uses Vyadhi Pratyanika Chikitsa, meaning treatment directed specifically against the disease expression. In English, this can be described as disease targeted management. In Urdu, one may call it marz ke muqabil ilaj, and in Arabic al ilaj al muwajjah didda al marad. This principle ensures that individualized constitutional treatment does not become so broad that the specific disease process is ignored.
For parathyroid disorders, this may include strategies aimed at reducing stone recurrence, calming neuromuscular irritability, protecting bone tissue, stabilizing calcium handling, supporting kidney resilience, or reducing inflammatory burden associated with chronic metabolic imbalance. This principle is important because Ayurveda is not only philosophical. It is clinically tactical. It recognizes that the patient needs both root correction and focused relief where disease is actively damaging the body.
Rasayana Chikitsa, Regeneration and Deep Tissue Rebuilding
Once the causative factors are reduced, Agni is improved, Ama is cleared, and channels begin to function better, Ayurveda moves toward Rasayana Chikitsa. In English, this means rejuvenative and restorative therapy aimed at rebuilding tissue quality, vitality, resilience, and long term stability. In Urdu, you may describe it as tajdeedi aur muqawwi ilaj, and in Arabic as al ilaj al tajdidi wa al muqawwi.
Charaka Samhita, Chikitsa Sthana, Chapter 1 states:
रसायनं नाम वयसः स्थापकं बलवर्णकरं
Transliteration:
Rasayanam naama vayasah sthaapakam balavarnakaram
Translation:
Rasayana preserves vitality and promotes strength and healthy tissue quality.
This principle is central in parathyroid disorders because many patients do not merely have a temporary imbalance. They have Asthi Dhatu depletion, Majja weakness, poor resilience, poor recovery, and fear of relapse. Rasayana is the phase in which Ayurveda tries to rebuild what chronic disease has taken away. In a global patient friendly explanation, this is the phase of structured restoration, not just symptom suppression.
Asthi and Majja Poshana, Nourishing Bone and Marrow Related Tissues
Because parathyroid disorders directly affect bone and often neuromuscular stability, a special treatment priority is Asthi and Majja Poshana, meaning nourishment of bone tissue and marrow or deeper nerve related tissues. In English, this refers to rebuilding structural integrity and internal tissue resilience. In Urdu, it can be explained as haddiyon aur guda e استخوان ki ghiza, and in Arabic as taghdhiyat al izam wa al نخاع.
Classical Ayurvedic thinking repeatedly stresses that weak tissues require nourishment suited to their nature. In patients with chronic mineral loss, fractures, thinning bones, cramping, neurological instability, or post surgical depletion, treatment must go beyond simple replacement. It must support tissue quality. This is why formulations, diet, sleep regulation, and digestive support are all coordinated together rather than prescribed independently.
Ojas Vardhana, Enhancing Vital Resilience
A patient may look biochemically better but still feel fragile, anxious, exhausted, and prone to relapse. Ayurveda explains this through weak Ojas, the refined essence of all Dhatus and the basis of resilience, immunity, stability, and recovery. In Urdu, one may explain Ojas as quwwat e hayat or jismani madafati quwwat ka lutf, and in Arabic as jawhar al manaa wa al quwwah.
Charaka Samhita, Sutra Sthana, Chapter 17 states:
ओजो हि सर्वधातूनां सारः
Transliteration:
Ojo hi sarvadhatoonaam saarhah
Translation:
Ojas is the essence of all the Dhatus.
In practical terms, Ojas enhancement means the treatment must support sleep, calm the mind, improve digestion, reduce overstrain, improve tissue nutrition, and restore confidence in the body’s capacity to heal. This is especially important in chronic cases where the patient has lived for years with fear, fatigue, and repeated setbacks.
Shamana and Shodhana, When to Calm and When to Purify
Ayurveda also distinguishes between Shamana, which means palliative or balancing treatment, and Shodhana, which means cleansing or purificatory therapy. In Urdu, these may be described as taskeen dene wala ilaj and tanqiyah ya safai ka ilaj. In Arabic, al ilaj al musakkin al muwazin and al tanqiyah al ilajiyyah can serve as explanatory phrases.
Not every parathyroid patient is a candidate for intensive cleansing. In fact, many are better suited to gentle correction, nourishment, and staged rebuilding, especially if they are older, depleted, post surgical, or living with chronic kidney disease. Therefore, the physician must judge carefully whether purification is appropriate, optional, or contraindicated. This distinction is vital for patient safety. Ayurveda is strongest when applied with judgment, not as a rigid protocol.
Chikitsa as Samprapti Vighatana, Reversal of Pathogenesis
The final guiding principle is the deepest one. Ayurveda defines true treatment not as short term symptom reduction but as Samprapti Vighatana, the breaking of the disease pathway itself. In English, this means reversal of pathogenesis. In Urdu, one may explain it as marz ke banne ke amal ko torna, and in Arabic as kasr masar takawun al marad.
Charaka Samhita, Chikitsa Sthana states:
सम्प्राप्तिविघटनमेव चिकित्सा
Transliteration:
Samprapti vighatanam eva chikitsa
Translation:
True treatment is the reversal of the disease process.
For parathyroid disorders, this means a complete Ayurvedic plan must do all of the following: remove the cause, correct digestion, reduce Ama, rebalance Doshas, clear channels, protect kidney and bone function, rebuild Asthi and Majja, strengthen Ojas, and then maintain the result through individualized follow up. Without that sequence, improvement may occur, but recurrence remains likely.
Ayurvedic Definition of Cure in Parathyroid Disorders
Ayurveda defines cure as Samprapti Vighatana, the complete breakdown of disease causation.
Charaka Samhita Chikitsa Sthana Chapter 16 states
“सम्प्राप्तिविघटनमेव चिकित्सा”
Translation
True treatment is the reversal of disease pathogenesis.
From this standpoint, Ayurveda aims to cure parathyroid disorders by restoring Agni, correcting Doshas, rebuilding Dhatus, and preventing recurrence. When applied correctly and ethically, this approach seeks long term stability rather than lifelong dependency.
Ayurveda Avaleha (Medicine) for Cure
Name: Asthi-Majja-Ojas Rasayana Avaleha (Medicine)
Ingredients
Main Herbal Interventions
- Ashwagandha (Withania somnifera) – Vata pacifying, bone/muscle strength
- Arjuna (Terminalia arjuna) – Asthi support, cardiac protection
- Shatavari (Asparagus racemosus) – Pitta pacifying, nourishes dhatus
- Guduchi (Tinospora cordifolia) – Tridosha balancing, Rasayana, immunomodulator
- Amalaki (Emblica officinalis) – Potent Rasayana, antioxidant, calcium absorption enhancer
- Bala (Sida cordifolia) – Neuromuscular support, Vata pacifier
- Gokshura (Tribulus terrestris) – Supports urinary tract, prevents stones
- Varun (Crataeva nurvala) – Specific for Mutrashmari (urinary calculi)
- Punarnava (Boerhavia diffusa) – Diuretic, balances Kapha and Pitta
- Manjistha (Rubia cordifolia) – Rakta Shodhana (blood purifier)
- Sariva (Hemidesmus indicus) – Rakta Dushti correction, cooling, Pitta pacifier
Mineral Formulations (Shuddha and classical)
- Praval Pishti (Coral calcium) – Natural calcium source, bone strengthening
- Mukta Bhasma / Mukta Sukti Bhasma (Pearl/oyster shell calx) – Calcium rich, cooling
- Godanti Bhasma (Gypsum calx) – Pitta pacifier, calcium supply
- Abhrak Bhasma (Mica calx) – Majja Rasayana, improves nerve and marrow health
- Lauh Bhasma (Iron calx) – Rakta dhatu support, strengthens Ojas
- Swarnamakshik Bhasma (Chalcopyrite calx) – Supports metabolism and endocrine functions
- Rajata Bhasma (Silver calx) – Nervine tonic, cooling, Rakta protector
- Svarna Bhasma (Gold calx) – Rasayana, enhances immunity and Ojas
- Trivanga Bhasma (Lead, Tin, Zinc compound) – Corrects metabolic imbalances
- Sphatika Bhasma (Alum calx) – Cooling, Rakta Shodhana, stone prevention
Rasayana Supports
- Amalaki Rasayana – Base Rasayana
- Gandhak Rasayan (purified sulfur Rasayana) – Tissue rejuvenator
- Chyawanprash (optional) – Classic Avaleha base if desired
Base & Carriers
- Cow’s Ghee (Go Ghrita) – Enhances Rasayana effect, pacifies Vata
- Jaggery (Guda) or Sharkara (Sugar) – Sweet base, stabilizes formulation
- Honey (Madhu) – Yogavahi (catalyst), increases tissue penetration
Dietary Powders
- Sesame seed (Tila) powder – Rich in calcium and oil, supports Asthi dhatu
- Drumstick leaf (Moringa) powder – Calcium, vitamin D, and micronutrients
Preparation Method (Avaleh Kalpana as per Bhaishajya Ratnavali)
- Prepare a decoction (Kwatha) with Ashwagandha, Arjuna, Shatavari, Guduchi, Amalaki, Bala, Gokshura, Varun, Punarnava, Manjistha, Sariva (16 parts water, reduced to 1/4th).
- Add jaggery/sugar to the decoction and boil until Avaleha consistency forms.
- Incorporate cow’s ghee slowly while stirring.
- At the final stage, add all mineral formulations (Praval, Mukta Sukti, Godanti, Abhrak, Lauh, Swarnamakshik, Rajata, Svarna, Trivanga, Sphatika Bhasma) + Amalaki Rasayana and Gandhak Rasayan.
- Allow to cool slightly, then add honey.
- Mix in sesame seed powder and drumstick leaf powder.
- Store in an airtight glass container.
Dosage & Anupana
- Dose: 10–15 g twice daily
- Anupana (vehicle): Warm milk or lukewarm water
- Course: 3–6 months under supervision
Ayurvedic Action
- Rasayana – rejuvenates tissues, restores Ojas
- Asthi Dhatu Poshaka – nourishes bone tissue (Praval, Mukta, Godanti, Sesame)
- Majja Rasayana – supports marrow and nerves (Abhrak, Ashwagandha, Shatavari)
- Rakta Shodhana – blood purification, tumor prevention (Manjistha, Sariva, Sphatika)
- Mutravaha Srotas Shuddhi – prevents stones, protects kidneys (Gokshura, Varun, Punarnava)
- Ojasvardhaka – boosts immunity and vitality (Svarna, Rajata, Gandhak Rasayan)
Indications
- Hyperparathyroidism – prevents bone resorption, balances calcium, reduces stones
- Hypoparathyroidism – relieves spasms, tetany, neuromuscular irritability
- Parathyroid cancer – Rasayana and Rakta Shodhana for recurrence prevention, immune strengthening
Critical Warning About Market Purchased Avaleha and Self Preparation

Ayurvedic Avaleha used in parathyroid related disorders is not a general health supplement and it is not meant for unsupervised use. In my clinical experience, patients who purchase Avaleha from the open market or attempt to prepare it themselves rarely achieve correction of the disease. In many cases, symptoms persist, progress slowly, or worsen due to improper formulation and lack of clinical oversight. If you are seeking cure through Ayurveda, it is essential to understand why this approach does not work.
Why Market Purchased Avaleha Fails in Parathyroid Disorders
Parathyroid disorders are endocrine conditions with significant variation between individuals. One patient may have primary hyperparathyroidism, another may have hypoparathyroidism following thyroid surgery, another may have secondary parathyroid involvement due to chronic kidney disease, while another may show parathyroid hormone elevation related to vitamin D deficiency. A fixed commercial Avaleha formula cannot address these different disease mechanisms and therefore cannot deliver cure.
Age and life stage play a decisive role. Calcium metabolism differs in children, adults, elderly individuals, and pregnant or breastfeeding women. Bone turnover, renal handling of minerals, and cardiovascular risk change with age. Market Avaleha products are not designed to adapt to these physiological differences, making them ineffective or unsafe in many situations.
Disease stage is equally important. Early stage imbalance may respond to metabolic correction and Rasayana support, whereas advanced disease with kidney stones, osteoporosis, fractures, seizures, cardiac rhythm disturbances, or vascular calcification requires staged therapy and close monitoring. Market products do not recognize disease progression and therefore fail to provide appropriate therapeutic sequencing.
Past surgical history changes endocrine stability. Patients who develop hypoparathyroidism after thyroid or neck surgery often have fragile calcium balance. In such cases, incorrect ingredients, dosing, or timing can precipitate muscle spasms, seizures, or cardiac instability. Commercial products do not account for post surgical physiology or long term risk.
Chronic medical conditions further complicate treatment response. Individuals with chronic kidney disease, recurrent kidney stones, diabetes, liver disorders, autoimmune diseases, chronic digestive disorders, osteoporosis, or long term steroid use require carefully modified formulations. Market Avaleha does not consider renal clearance, vascular calcification risk, or metabolic reserve, which leads to failure or harm.
Interactions with existing medicines are frequently overlooked. Many patients are already taking calcium supplements, vitamin D, calcitriol, thyroid hormone, diuretics, antiepileptic drugs, or dialysis related medications. Without supervision, combining these with market Avaleha can worsen hypercalcemia, trigger hypocalcemia fluctuations, or destabilize cardiac rhythm.
Individual constitution and Dosha dominance are fundamental in Ayurveda. Vata dominant individuals are prone to spasms, dryness, anxiety, and tissue depletion. Pitta dominant individuals are prone to inflammation and metabolic excess. Kapha dominant individuals are prone to sluggish metabolism and stone formation. Market Avaleha ignores these differences and often aggravates the wrong Dosha.
Digestive strength determines whether any medicine will work. Many patients have weak digestion, malabsorption, chronic constipation, or gut inflammation. Without correcting Agni and tissue metabolism, even high quality ingredients fail to act effectively. Market products do not assess or correct digestive capacity.
Quality and processing of ingredients vary widely in commercial preparations. Classical Avaleha requires precise heating stages, correct sequencing, and carefully selected raw materials. Industrial shortcuts, preservatives, excessive sweeteners, and long shelf storage reduce Rasayana potency and therapeutic depth.
Timing and Anupana are integral to treatment success. Avaleha must be taken at the correct time of day and with a specific carrier based on disease state and constitution. Market products do not provide individualized guidance, resulting in unpredictable absorption and inconsistent outcomes.
Ongoing monitoring is essential in endocrine disorders. Parathyroid related treatment requires periodic assessment of serum calcium, phosphate, vitamin D, kidney function, and sometimes urine calcium or bone density. Market use offers no follow up framework and delays detection of complications.
Why Buying Avaleha From the Market Can Be Harmful
In hyperparathyroidism, calcium levels may already be elevated. Inappropriate formulations can worsen hypercalcemia, dehydration, kidney stone formation, mental confusion, and cardiovascular risk. In hypoparathyroidism, unsupervised dosing can provoke tetany or seizures. In individuals with kidney disease, inappropriate mineral intake may accelerate vascular calcification and systemic complications.
Commercial products may not follow strict classical purification protocols, particularly when mineral ingredients are involved. Improper processing increases the risk of toxicity or therapeutic failure, creating false reassurance and delaying appropriate care.
Why Self Preparation of Avaleha Must Never Be Attempted
Patients must never attempt to prepare Avaleha at home. Avaleha preparation is a specialized pharmaceutical process that requires precise control of heat, correct identification of cooking stages, accurate sequencing of ingredients, and deep understanding of drug compatibility. Even small errors can destroy medicinal value or create harmful byproducts.
When mineral ingredients such as Bhasma or Pishti are involved, home preparation becomes dangerous. Proper purification and processing require specialized training. Without this expertise, risks include contamination, incorrect dosing, kidney strain, and worsening of calcium imbalance.
Self preparation also leads to inconsistent potency. Each batch differs in strength, making endocrine regulation unpredictable and unsafe.
Why Supervision by an Ayurvedic Physician Is Mandatory
Parathyroid disorders require individualized planning. A qualified Ayurvedic physician evaluates age, constitution, disease type, disease stage, laboratory values, kidney function, bone health, surgical history, chronic illnesses, current medications, digestive strength, and stress factors. Only then can the appropriate Avaleha composition, dosage, timing, Anupana, and duration be determined.
In clinical practice, formulations are adjusted based on response and follow up investigations. This dynamic correction is essential for safety and cure and cannot be achieved through market products or self preparation.
Final Advisory to Patients
If you are serious about curing parathyroid related disorders through Ayurveda, do not buy Avaleha from the market and do not attempt self preparation. These approaches do not work due to multiple individualized factors and may cause harm. Always follow a supervised Ayurvedic treatment plan under a qualified physician, supported by appropriate diagnostic monitoring and safety principles.
Modern Scientific Research

Modern research on parathyroid disorders is strongest in four areas: chronic kidney disease related secondary hyperparathyroidism, long term management challenges in hypoparathyroidism, bone recovery after appropriate conventional treatment, and supportive bone focused evidence for selected herbs such as Cissus quadrangularis. Direct human trials proving that Ayurvedic treatment alone reverses parathyroid gland disease remain limited, so this section should be presented as evidence informed, not overstated.
Study 1
Year: 2024
Journal: Expert Opinion on Pharmacotherapy
Study focus: Secondary hyperparathyroidism in chronic kidney disease
Key findings: This review explains that secondary hyperparathyroidism in chronic kidney disease begins as an adaptive rise in parathyroid hormone, then becomes maladaptive over time and is linked with increased morbidity and mortality. It reviews standard management strategies such as phosphate lowering, vitamin D based therapies, calcimimetics, and surgery.
Research link: https://pubmed.ncbi.nlm.nih.gov/38881200/
Brief interpretation: This is important because it confirms that elevated parathyroid hormone in kidney disease is not a minor lab abnormality. It is part of a larger mineral, bone, and cardiovascular disorder, which means any integrative plan must account for kidney function and phosphate handling.
Study 2
Year: 2024
Journal: Endocrinology and Metabolism
Study focus: Treatment limitations in hypoparathyroidism
Key findings: This review notes that conventional treatment with calcium and active vitamin D can normalize serum calcium, but many patients still experience calcium fluctuations, hypercalciuria, renal impairment, and lower quality of life. It also discusses newer long acting parathyroid hormone based therapies.
Research link: https://pubmed.ncbi.nlm.nih.gov/38572533/
Full text: https://pmc.ncbi.nlm.nih.gov/articles/PMC11066455/
Brief interpretation: This is highly relevant for patient education because it shows why many people continue looking for broader restorative care even when they are already receiving standard treatment. Biochemical control does not always mean full recovery.
Study 3
Year: 2024
Journal: Endocrine
Study focus: Quality of life in hypoparathyroidism receiving standard treatment
Key findings: This updated systematic review found that patients with hypoparathyroidism on standard therapy frequently report impaired quality of life. Almost all included studies reported statistically significant reduction in at least one quality of life domain compared with control or norm populations.
Research link: https://pubmed.ncbi.nlm.nih.gov/38578400/
Full text: https://pmc.ncbi.nlm.nih.gov/articles/PMC11246296/
Brief interpretation: This validates a common patient experience. Many patients are told their condition is controlled, yet they still feel physically and mentally unwell. That makes a broader integrative discussion more credible and clinically relevant.
Study 4
Year: 2012
Journal: Surgery
Study focus: Bone mineral density after curative surgery for primary hyperparathyroidism
Key findings: This study found that bone mineral density improved in up to seventy five percent of patients after curative parathyroidectomy for primary hyperparathyroidism. The hip and lumbar spine both showed meaningful response.
Research link: https://pubmed.ncbi.nlm.nih.gov/23040710/
Brief interpretation: This is one of the most clinically useful studies because it shows that when the disease is driven by a structural gland abnormality, definitive treatment can significantly improve skeletal outcomes. It supports a balanced article rather than an anti medical one.
Study 5
Year: 2012
Journal: Indian Journal of Endocrinology and Metabolism
Study focus: Renal manifestations of primary hyperparathyroidism
Key findings: This review describes nephrolithiasis, nephrocalcinosis, and declining renal function as important manifestations of primary hyperparathyroidism. It also notes that progression of nephrocalcinosis is largely reversible after successful surgery, although residual risk may persist.
Research link: https://pubmed.ncbi.nlm.nih.gov/22470864/
Full text: https://pmc.ncbi.nlm.nih.gov/articles/PMC3313745/
Brief interpretation: This is useful because it helps patients understand that endocrine correction may reduce future kidney harm, but long term hydration, metabolic care, and follow up still matter.
Study 6
Year: 2015
Journal: Journal of Clinical and Diagnostic Research
Study focus: Cissus quadrangularis in fracture healing
Key findings: This pilot clinical study reported that Cissus quadrangularis helped reduce pain, swelling, and fragment mobility and accelerated healing in maxillofacial fracture patients. Serum calcium and phosphorus were also higher in the treated group during follow up.
Research link: https://pubmed.ncbi.nlm.nih.gov/27011718/
Brief interpretation: This does not prove cure of parathyroid disease itself, but it does support the bone healing relevance of a classical Ayurvedic herb, which matters in patients with parathyroid related skeletal depletion.
Study 7
Year: 2022
Journal: Phytomedicine
Study focus: Cissus quadrangularis and bone loss in postmenopausal women with osteopenia
Key findings: This randomized placebo controlled trial found that oral Cissus quadrangularis showed promise in delaying bone loss by slowing bone remodeling over twenty four weeks, although no significant short term bone mineral density gain was demonstrated.
Research link: https://pubmed.ncbi.nlm.nih.gov/35523116/
Brief interpretation: This is a realistic kind of evidence. It suggests support for bone turnover biology without exaggerating results. For your article, it helps justify bone focused adjunctive use rather than making direct gland cure claims.
What the Evidence Supports
The research strongly supports the seriousness of parathyroid disorders, especially in relation to bone loss, kidney complications, chronic kidney disease related secondary hyperparathyroidism, and reduced quality of life in hypoparathyroidism. It also offers early supportive evidence that selected herbs such as Cissus quadrangularis may have a rational adjunctive role in bone healing and bone turnover support.
What the Evidence Does Not Yet Prove
Current modern evidence does not yet prove that Ayurvedic formulations directly and independently reverse all forms of parathyroid gland disease in the same way that successful surgery can correct selected structural primary hyperparathyroidism. What it does support is an evidence informed integrative role in areas such as bone recovery, metabolic support, symptom burden, and long term quality of life, when used responsibly and alongside proper diagnosis.
Diet and Lifestyle Recommendations

Diet and lifestyle guidance in parathyroid disorders should never be reduced to a generic instruction such as take more calcium or avoid stones. That approach is too simplistic and often misleading. A more intelligent strategy begins with the type of parathyroid disorder, the current calcium pattern, kidney status, digestive strength, bone reserve, medication burden, and the patient’s stage of life. In my clinical experience, this is where many patients become confused. One source tells them to increase calcium. Another tells them to restrict it. One person warns against dairy. Another insists on supplements. The result is fear, inconsistency, and loss of confidence.
A better approach is to explain that diet and lifestyle must support physiology, not fight it blindly. In primary hyperparathyroidism, current guidance does not advise restricting dietary calcium, because low calcium intake may further stimulate parathyroid hormone secretion. Instead, calcium intake should generally remain within normal nutritional guidelines while vitamin D adequacy is maintained carefully. In chronic hypoparathyroidism, conventional guidance supports adequate dietary calcium, careful supplement timing, correction of vitamin D inadequacy, and attention to phosphorus balance and renal safety. In chronic kidney disease related secondary hyperparathyroidism, dietary phosphate management becomes especially important and should be individualized rather than handled through random internet advice.
Principles Before Food Lists
The first principle is that the patient should eat in a way that supports stability rather than extremes. Extreme restriction, erratic meals, overuse of supplements, and reactive eating patterns tend to worsen anxiety and make endocrine regulation harder. A second principle is that hydration, mineral balance, digestive efficiency, and sleep quality are all part of treatment, not background issues. A third principle is that kidney disease, kidney stones, post thyroidectomy hypoparathyroidism, and hypercalcemia all require different practical choices. If you ignore the clinical context, even well intentioned dietary advice can become harmful.
From an Ayurvedic perspective, food is not only nutrient input. It is also a regulator of Agni, meaning digestive and metabolic fire. In English, Agni may be described as the body’s capacity to digest, absorb, transform, and utilize nourishment. In Urdu, a practical explanatory phrase is hazm ki quwwat, and in Arabic quwwat al hadm wa al istihalah. When Agni is weak, the patient may consume useful nutrients but fail to utilize them properly. That is one reason why food timing, meal regularity, digestive comfort, and overburdening the gut matter so much in long term recovery.
Dietary Guidance in Primary Hyperparathyroidism
Patients with primary hyperparathyroidism often assume they should cut out calcium because blood calcium is already high. That assumption is understandable but often incorrect. Modern guidance supports maintaining normal dietary calcium intake rather than restricting it, because low calcium intake may drive parathyroid hormone even higher. Current guidance uses standard nutritional targets, roughly 800 mg daily for younger adults and 1000 mg daily for older adults, depending on age and sex. Vitamin D should also be maintained appropriately rather than ignored.
What this means practically is that the patient should avoid panic driven calcium restriction. Normal food based calcium is generally preferred over indiscriminate supplement escalation unless medical supervision indicates otherwise. Hydration becomes highly important, especially in patients with a history of kidney stones, dehydration, or constipation. A high sodium diet should be reduced because excess sodium can worsen urinary calcium losses and contribute to stone risk. Very low fluid intake, excessive processed food, and chronic dehydration should all be corrected because they increase the likelihood of renal complications and general fatigue. These practical measures align with both endocrine and Ayurvedic logic because they reduce internal strain without creating new imbalance.
Dietary Guidance in Hypoparathyroidism
In hypoparathyroidism, the dietary situation is different. These patients usually need adequate dietary calcium and often require calcium supplements and active vitamin D as part of standard treatment. Recent guidance suggests a dietary elemental calcium intake of about 800 to 1000 mg per day in adults, with supplementation added if target calcium cannot be maintained through diet and active vitamin D therapy alone.
Meal structure matters here. Calcium carbonate is generally better taken with food, and calcium supplements are often timed with meals to help limit phosphorus absorption. Adults with hypoparathyroidism may also need a lower phosphate diet when hyperphosphatemia is an issue. For patients, the practical lesson is that supplements should not be swallowed randomly. Timing, meal composition, and follow up monitoring matter. Very large and erratic calcium heavy meals may create fluctuations rather than steady balance. It is usually better to build a consistent pattern of regular meals, appropriate protein, and physician guided supplement timing than to rely on extremes.
From an Ayurvedic angle, this also means meals should be digestible, warm when appropriate, and supportive of stable Agni rather than cold, irregular, heavily processed, or gut irritating. A patient with hypocalcemia and Vata aggravation usually does poorly on erratic fasting, dry snack based eating, chronic undernourishment, or poor sleep. Regularity itself becomes therapeutic.
Dietary Guidance in Secondary Hyperparathyroidism and Chronic Kidney Disease
In secondary hyperparathyroidism related to chronic kidney disease, diet must be approached with even more caution because phosphate handling, calcium exposure, kidney reserve, and vascular calcification risk all matter. KDIGO guidance supports limiting dietary phosphate in patients with chronic kidney disease who have hyperphosphatemia, ideally considering the source of phosphate as well as the quantity. Phosphate additives and highly processed foods may create a heavier burden than many patients realize.
This is not an area for improvisation. Patients with kidney disease should not copy general calcium advice from healthy adults and should not start herbomineral self treatment casually. From both nephrology and Ayurvedic viewpoints, the patient’s terrain is already unstable. In such cases, diet must be individualized, fluid advice must reflect kidney status, and minerals must be handled with exceptional care. If you are writing for global readers, it is important to state this very clearly because many people with kidney disease search online for natural treatment and unintentionally expose themselves to unsafe advice.
Bone Supportive Nutrition
Bone health in parathyroid disorders is not supported by calcium alone. It requires a broader nutritional environment that includes adequate protein, appropriate vitamin D status, magnesium sufficiency where indicated, and overall metabolic stability. For patients with low bone density, fracture history, or postmenopausal bone vulnerability, a nutritionally sparse or chronically restrictive diet is rarely helpful. Bone is living tissue. It needs substrate, not just supplements.
A practical patient friendly message is that meals should contain real nourishment. A pattern built around protein adequacy, vegetables, balanced mineral intake, and digestible whole foods is usually more useful than dependence on isolated supplements alone. In Ayurvedic language, this supports Asthi Dhatu, meaning bone tissue, while also protecting Agni and preventing deeper depletion.
Kidney Stone Prevention Through Daily Habits
For patients with stone tendency, hydration is one of the most powerful non drug strategies. Long periods of low fluid intake, repeated dehydration, excessive salty packaged food, and high intake of ultra processed products create a physiology that favors recurrence. This does not mean every patient with stones should avoid all calcium foods. In fact, indiscriminate calcium restriction may be counterproductive in some settings. The better strategy is guided hydration, sodium moderation, and proper endocrine evaluation.
From an Ayurvedic perspective, stone prone patients often show disturbance in Mutravaha Srotas, meaning the urinary functional system. The goal is not merely washing the system with fluids, but reducing internal conditions that encourage pathological deposition. This includes improving digestion, lowering inflammatory burden, maintaining regular elimination, and avoiding long standing dietary excess.
Digestive Discipline and Agni Protection
Even the best food plan fails if digestion remains weak. This is where an Ayurvedic article can add unique value. Patients with chronic constipation, bloating, irregular appetite, or gut heaviness often have poor metabolic responsiveness. If digestion is unstable, tissue nutrition becomes unstable. If meals are erratic, endocrine resilience tends to weaken further. If the gut is chronically irritated, both conventional and Ayurvedic therapies may work less efficiently.
A practical global recommendation is simple: regular meals, moderate portions, less processed food, less late night overeating, better chewing, and reduced dependence on constant snacking. These habits support Agni and reduce the internal inconsistency that so often accompanies chronic endocrine disease. For Western readers unfamiliar with Ayurveda, this is an easy point to understand because it links digestive stability with treatment stability.
Sleep, Stress, and Recovery
Lifestyle advice is incomplete without sleep and stress. Chronic stress affects adherence, inflammation, food choices, digestion, muscle tension, and perceived symptom burden. Sleep deprivation worsens fatigue, emotional reactivity, and recovery capacity. A patient who is biologically unstable and psychologically exhausted rarely heals well.
This is where Ojas becomes clinically relevant. Ojas may be explained as the body’s deep reserve of vitality, resilience, and restorative capacity. In Urdu, you may describe it as quwwat e hayat, and in Arabic as jawhar al quwwah wa al manaa. When Ojas is weak, the patient may look functional but feel persistently depleted. Therefore, a complete lifestyle program should include fixed sleep timing, reduced overstimulation at night, mental decompression, and realistic restoration practices rather than only supplement routines.
Movement and Physical Activity
Physical activity should be supportive, not punishing. In patients with bone weakness, post fracture recovery, neuromuscular instability, or significant fatigue, aggressive exercise can be counterproductive. Gentle weight bearing movement, walking, posture focused work, supervised strengthening, and mobility support are usually more appropriate than sudden high impact regimens. Patients with severe hypocalcemia symptoms, arrhythmia risk, or active stone pain should be medically assessed before intensifying exercise.
For a pillar article, the key message is not that exercise is always good in any form. It is that appropriate movement supports bone, mood, circulation, and metabolic health when chosen according to the patient’s stage and safety profile.
Foods and Habits to Approach Carefully
A responsible article should avoid rigid food fear, but some patterns deserve caution. Excess sodium, chronic dehydration, highly processed foods, phosphate additive heavy packaged products, erratic mega dosing of supplements, and unsupervised mineral self treatment are common examples. In hypoparathyroidism, phosphorus heavy eating patterns may need attention when hyperphosphatemia is present. In chronic kidney disease, phosphate and calcium handling must be individualized carefully.
Ayurvedically, cold, heavy, stale, overly processed, and irregular eating patterns tend to weaken Agni and increase metabolic sluggishness. For many patients, the problem is not one forbidden food. It is a repeated lifestyle rhythm that keeps metabolism disorganized.
The Most Practical Message for Patients
The most useful dietary and lifestyle advice for parathyroid disorders is not extreme. It is intelligent, stable, and individualized. Eat regularly. Maintain appropriate calcium rather than restricting blindly. Correct vitamin D inadequacy under supervision. Protect hydration. Reduce sodium excess. Be careful with phosphate if kidney disease or hypoparathyroidism makes it relevant. Support digestion. Sleep consistently. Reduce chronic stress. Avoid unsupervised herbomineral treatment and supplement chaos. These simple principles often do more for long term stability than dramatic dietary rules that the patient cannot sustain.
Preventive Strategies

Prevention in parathyroid disorders is not always about stopping the disease from ever occurring. In many patients, especially those with genetic risk, prior thyroid surgery, chronic kidney disease, or established glandular pathology, true prevention may not mean total avoidance. Instead, it means reducing the chance of delayed diagnosis, limiting progression, lowering complication burden, protecting bone and kidney health, and preventing repeated metabolic destabilization. From a patient centered perspective, this is a far more useful and realistic goal. Prevention is not only about the first event. It is also about preventing the next stone, the next fracture, the next hypocalcemic spasm, the next silent decline in bone density, or the next year of living with unexplained fatigue while the disease advances quietly.
Early Identification Prevents Long Term Damage
One of the most powerful preventive strategies is early recognition. Many parathyroid disorders remain hidden because the initial symptoms are nonspecific. A patient may report weakness, constipation, poor sleep, mood changes, recurrent stones, tingling, or reduced stamina, while the underlying endocrine pattern is not investigated deeply enough. Once diagnosis is delayed, prevention becomes harder because structural consequences such as osteoporosis, renal calcification, or chronic neuromuscular instability may already be developing. Routine evaluation of calcium, parathyroid hormone, vitamin D, renal function, and in selected patients urinary calcium can help identify disease before it leaves a permanent footprint. This is particularly important in patients with kidney stones, low bone density, thyroid surgery history, chronic kidney disease, or unexplained calcium abnormalities.
Monitoring Is a Preventive Tool, Not Just a Follow Up Formality
A major mistake in long term care is assuming that once symptoms improve, monitoring can become casual. Parathyroid disorders often progress silently. Bone loss may continue without pain. Renal complications may worsen without obvious warning. Calcium may appear stable for a time while phosphorus handling, kidney function, or urinary calcium remain problematic. Preventive care therefore includes periodic monitoring, not because the patient is fragile, but because the disease can be deceptive. In primary hyperparathyroidism under observation, bone density and renal status matter. In hypoparathyroidism, calcium balance, phosphorus, kidney effects of long term treatment, and symptom stability all matter. In chronic kidney disease related secondary hyperparathyroidism, serial assessment of phosphate, calcium, vitamin D related therapy, and broader CKD mineral bone disorder parameters is essential.
Vitamin D Sufficiency Helps Prevent Secondary Escalation
Vitamin D insufficiency is one of the most modifiable contributors to parathyroid hormone elevation. When vitamin D remains low, the body struggles to absorb and regulate calcium properly, and the parathyroid glands may remain chronically stimulated. Preventive strategy therefore includes identifying and correcting deficiency thoughtfully rather than ignoring it or self prescribing erratic high dose supplements. This is especially relevant for patients with low sunlight exposure, indoor lifestyles, malabsorption, obesity, chronic kidney disease, or recurrent unexplained elevation of parathyroid hormone. For international patients, this point matters because vitamin D deficiency is common across modern urban populations and can quietly sustain endocrine imbalance.
Bone Protection Must Begin Before Fractures Occur
Fracture prevention begins long before the first fracture. In parathyroid disorders, preventive care for bone includes identifying low bone density early, ensuring adequate but not indiscriminate calcium intake, supporting vitamin D status, encouraging safe weight bearing activity where appropriate, and correcting the endocrine driver before skeletal depletion advances. Patients with menopause related bone vulnerability, previous fractures, chronic steroid use, older age, low body weight, or prolonged hyperparathyroid states need especially careful skeletal protection. Once bone weakness progresses into repeated structural injury, recovery becomes more difficult and slower.
Kidney Protection Requires Everyday Discipline
Patients with hypercalcemic patterns or stone history should understand that kidney protection is a daily preventive practice, not only a medical event during stone attacks. Appropriate hydration, reduced sodium excess, avoidance of chaotic self supplementation, and proper endocrine evaluation all matter. In patients with chronic kidney disease, prevention becomes even more delicate because calcium, phosphate, vitamin D based therapies, and vascular calcification risk are closely linked. This means that kidney protective prevention should always be individualized. A stone prone patient without CKD is different from a dialysis patient with secondary hyperparathyroidism, and both are different from a person with post surgical hypoparathyroidism. Preventive advice only works when it respects those distinctions.
Preventive Strategy After Thyroid or Neck Surgery
Patients who have undergone thyroidectomy or major neck surgery deserve a special preventive approach because post surgical hypoparathyroidism may appear early or evolve over time. Tingling, cramps, muscle tightness, anxiety, or unusual weakness after surgery should not be dismissed casually. Prevention here means early biochemical monitoring, rapid symptom recognition, adherence to prescribed calcium and vitamin D plans where needed, and careful reassessment before assuming the problem is temporary or insignificant. For these patients, education itself is preventive. When they know what to watch for, they are more likely to seek help before symptoms escalate into severe hypocalcemia or emergency presentations.
Avoiding Self Medication Prevents Many Complications
One of the most neglected preventive strategies is simply avoiding unsupervised treatment. Patients often begin calcium, vitamin D, mineral mixtures, or market purchased Ayurvedic products without understanding whether their calcium is low, high, fluctuating, kidney stressed, or surgically unstable. This can worsen hypercalcemia, promote kidney stones, increase urinary calcium losses, aggravate phosphorus imbalance, or create false reassurance while the disease continues. Prevention therefore includes not only what to take, but what not to take casually. The same principle applies strongly to herbomineral formulations and market Avaleha. Improper self treatment can turn a manageable condition into a more complex one.
Stress Regulation and Daily Rhythm Support Long Term Stability
Patients often underestimate how much stress, poor sleep, irregular meals, and chronic overwork contribute to recurrence and symptom volatility. While stress may not be the original cause of every parathyroid disorder, it strongly influences digestive function, inflammatory tone, adherence to treatment, neuromuscular sensitivity, and perceived symptom burden. A patient who is constantly sleep deprived, dehydrated, anxious, undernourished, and inconsistent with routine is more vulnerable to relapse and slower recovery. Preventive strategy therefore includes stable daily rhythm, restorative sleep, regular meals, hydration, gentle movement, and mental decompression. From an Ayurvedic viewpoint, these are not background wellness habits. They are part of preventing Vata aggravation, Agni weakening, and Ojas depletion. This is especially important in chronic and post surgical patients whose bodies already have reduced reserve.
Ayurvedic Prevention Focuses on Terrain, Not Just Episodes
Ayurvedic prevention is valuable because it does not begin only after crisis. It tries to identify the terrain that makes crisis more likely. That includes weak Agni, Ama accumulation, disturbed sleep, erratic diet, chronic stress, poor tissue nourishment, and emerging weakness in Asthi Dhatu, Majja Dhatu, or Mutravaha Srotas. In practical terms, this means preventive Ayurvedic care may include digestive correction, staged Rasayana, constitution appropriate diet, stress reduction, and supervision rather than random use of tonics. The preventive goal is not to overwhelm the patient with lifelong medicines. It is to create internal conditions less favorable to recurrence and progression. This broader view is especially useful for patients who are not yet in severe disease but already show warning patterns.
Prevention Is Most Effective When It Is Individualized
The final preventive principle is personalization. Prevention for a postmenopausal woman with bone loss is not the same as prevention for a man with recurrent stones. Prevention for a patient with post thyroidectomy hypoparathyroidism is not the same as prevention for a dialysis patient with secondary hyperparathyroidism. Prevention for a young patient with familial calcium abnormalities is not the same as prevention for an older patient with silent glandular disease found on routine testing. The message is simple but powerful: generalized advice has limited preventive value. Individualized strategy prevents more damage because it matches the biological reality of the patient in front of you.
When to Seek Medical Advice

Parathyroid disorders should never be managed as if they are minor calcium issues that can be watched casually without context. Many patients delay consultation because the symptoms appear vague at first. They may attribute fatigue to stress, constipation to diet, cramps to weakness, stones to dehydration, or low mood to overwork. In my clinical experience, that delay is one of the main reasons why a manageable endocrine problem becomes a long standing systemic burden. A responsible article must therefore tell the reader clearly when medical advice is necessary, when urgent evaluation is needed, and when emergency care must not be postponed.
For international patients exploring natural or Ayurvedic approaches, this section is especially important. Ayurveda can be part of a broader therapeutic strategy, but it should never be used as a reason to ignore red flag symptoms, delay essential investigations, or postpone treatment in dangerous situations. The safest and most intelligent path is timely diagnosis, accurate staging, and individualized care.
Seek Medical Advice if Symptoms Persist Without Explanation
A patient should seek medical advice if there is persistent fatigue, unexplained weakness, recurrent constipation, reduced appetite, frequent urination, kidney stone history, low mood, poor concentration, tingling, cramps, muscle twitching, or abnormal calcium values on routine blood testing. These symptoms may appear ordinary when viewed one by one, but when they persist or cluster together, they deserve endocrine evaluation.
This is particularly important if the patient has a history of thyroid surgery, chronic kidney disease, repeated renal stones, osteoporosis, recurrent fractures, vitamin D deficiency, autoimmune disease, or family history of calcium related disorders. These are not minor background details. They are risk signals that should lower the threshold for proper medical assessment.
Seek Medical Advice Early if Bone or Kidney Problems Appear
Many patients first come to attention because of a fracture, bone pain, or recurrent kidney stones. By that stage, the disorder may already have moved beyond an early biochemical phase. If you develop unexplained bone loss, recurrent stone disease, slow fracture healing, nephrocalcinosis, or persistent flank discomfort, do not assume the issue is only orthopedic or urological. A parathyroid disorder should be considered and investigated.
Early assessment matters because delay can convert a reversible metabolic disturbance into a structural problem. The longer the disease remains active, the harder it may become to fully restore bone strength, kidney resilience, and quality of life.
Seek Medical Advice if Symptoms Begin After Thyroid or Neck Surgery
Any patient who develops tingling around the mouth, muscle cramps, unusual anxiety, twitching, stiffness, or weakness after thyroid or neck surgery should seek prompt medical evaluation. These symptoms may indicate post surgical hypoparathyroidism or unstable calcium balance. Even if the symptoms seem mild at first, they can progress quickly in some individuals.
This is one of the most important clinical situations in which early recognition prevents severe complications. Patients who have undergone surgery should not wait for symptoms to become dramatic before seeking help.
Seek Urgent Medical Advice if Symptoms Worsen Rapidly
Urgent medical advice is needed if symptoms are progressing over days or weeks rather than remaining stable. Rapid worsening of weakness, dehydration, repeated vomiting, increasing confusion, severe constipation, marked muscle spasms, progressive tingling, inability to eat properly, or recurrent stone pain should not be ignored.
Rapid change often means the biochemical imbalance is no longer mild or the underlying disease is becoming more active. In such cases, laboratory reassessment and medical review should not be delayed while trying home remedies alone.
Seek Emergency Care for Severe Warning Signs
Emergency medical care is necessary if the patient experiences seizures, severe muscle spasms, carpopedal spasm, chest pain, palpitations with instability, severe dehydration, persistent vomiting, marked confusion, altered consciousness, inability to swallow safely, severe weakness preventing normal movement, or symptoms suggestive of dangerous hypercalcemia or hypocalcemia.
At this stage, the priority is stabilization and immediate safety. No Ayurvedic medicine, supplement, diet change, or self prepared remedy should be used in place of emergency care. Once the patient is stabilized, integrative planning can be discussed appropriately.
Seek Advice Before Starting Supplements or Ayurvedic Medicines
A patient should also seek medical advice before starting calcium, vitamin D, herbomineral formulations, or market purchased Ayurvedic products. This is essential because the same substance can help one patient and harm another depending on whether calcium is low, high, fluctuating, kidney stressed, or poorly monitored.
In my clinical experience, many complications arise not because patients did nothing, but because they acted without enough information. They took the wrong support for the wrong stage of disease. That is why professional guidance matters so much in parathyroid disorders.
Seek Ongoing Medical Advice During Long Term Management
Parathyroid disorders should not be approached as one visit conditions. Ongoing review is important in patients with chronic kidney disease, recurrent stones, persistent symptoms, osteoporosis, prior surgery, long term calcium or vitamin D therapy, or continuing quality of life burden. Even when symptoms improve, monitoring remains valuable because silent progression can still occur.
A patient should therefore think of medical advice not as a sign of failure, but as a preventive tool. It helps ensure that treatment remains safe, relevant, and adapted to changing physiology over time.
The Most Important Patient Message
If symptoms are mild but persistent, seek evaluation. If symptoms are worsening, seek urgent medical advice. If symptoms are severe, unstable, neurological, cardiac, or disabling, seek emergency care. The earlier the condition is identified and properly classified, the better the chance of avoiding long term damage and building a more effective integrative plan.
Guidance From NCCIH and Major Governing Bodies

For international patients, guidance from recognized medical and regulatory bodies adds an important layer of clinical trust, especially in endocrine conditions involving calcium imbalance, kidney risk, long term monitoring, and possible surgery. In parathyroid disorders, this is particularly important because treatment decisions often depend on accurate diagnosis, structured follow up, medication review, and case specific risk assessment.
Link: https://kdigo.org/guidelines/ckd-mbd/
NCCIH Safety Perspective
The National Center for Complementary and Integrative Health describes Ayurveda as a traditional medical system, but it also warns that some Ayurvedic products may contain harmful levels of heavy metals and that herbs and supplements can interact with medicines. For patients with parathyroid disorders, this matters directly because many are already using calcium, vitamin D, calcitriol, thyroid medicines, diuretics, or kidney related treatments. In such cases, unsupervised use of market products may worsen calcium instability, increase renal burden, or complicate treatment.
Link: https://www.nccih.nih.gov/health/ayurvedic-medicine-in-depth
KDIGO Guidance in Kidney Related Parathyroid Disease
For patients with chronic kidney disease and secondary hyperparathyroidism, KDIGO is one of the most important international guidance bodies. Its CKD MBD guidance emphasizes structured evaluation and monitoring of calcium, phosphate, parathyroid hormone, and related mineral bone parameters rather than casual self treatment. This is highly relevant because elevated parathyroid hormone in kidney disease behaves differently from a localized gland disorder and must be interpreted within the broader context of phosphate handling, vitamin D metabolism, renal reserve, and vascular risk.
Link: https://kdigo.org/guidelines/ckd-mbd/
Endocrine Society and Evidence Based Endocrine Care
The Endocrine Society identifies primary hyperparathyroidism as a condition in which one or more parathyroid glands produce too much parathyroid hormone, often leading to high calcium levels. Its patient education and guideline resources reflect the importance of evidence based endocrine care, case classification, and specialist evaluation where appropriate. For global readers, this helps place Ayurvedic discussion within a medically informed framework where diagnostic accuracy and patient safety remain central.
Link: https://www.endocrine.org/patient-engagement/endocrine-library/primary-hyperparathyroidism
Practical Meaning for Patients Exploring Ayurveda
For patients who wish to explore Ayurvedic treatment, the practical message is clear. Ayurvedic care should be individualized, supervised, and aligned with proper medical diagnosis and monitoring. Market purchased products, self selected herbomineral preparations, or unsupervised supplementation are not appropriate substitutes for structured care in parathyroid disorders, especially when calcium levels are unstable, kidney disease is present, or surgery related endocrine changes are involved. A medically responsible Ayurvedic approach is strongest when it is applied within a safety conscious and clinically informed framework.
Link: https://www.nccih.nih.gov/health/ayurvedic-medicine-in-depth
Understanding the Full Journey Helps You Choose the Right Treatment at the Right Time
Table: From Cause to Cure A Complete Patient Pathway
| Stage | What Happens in the Body | What the Patient Feels | What Most Treatments Do | What Actually Helps |
|---|---|---|---|---|
| Early Imbalance | Calcium regulation begins to shift | Fatigue, mild weakness, constipation | Often ignored or misdiagnosed | Early detection and metabolic correction |
| Progression Phase | Hormonal imbalance increases | Bone discomfort, mood changes, frequent urination | Symptom-based treatment | Address root imbalance and absorption |
| Structural Impact | Bone and kidney involvement starts | Bone pain, stones, weakness | Medication or delayed action | Tissue strengthening and systemic support |
| Advanced Disease | Severe calcium imbalance | Fractures, severe cramps, confusion | Surgery or aggressive treatment | Integrated and stage-based care |
| Post-Treatment Phase | Body remains unstable | Recurrence, dependency, fatigue | Maintenance without correction | Long-term stabilization and restoration |
FAQs
What are the main symptoms of parathyroid disorders?
Parathyroid disorders present differently depending on hormone imbalance. Hyperparathyroidism often causes kidney stones, bone pain, fatigue, and digestive issues Hypoparathyroidism leads to muscle cramps, tetany, tingling around the mouth and extremities, and in severe cases, seizures.
How are parathyroid disorders diagnosed?
Diagnosis involves blood tests for calcium, phosphate, vitamin D, and PTH. Imaging such as ultrasound or sestamibi scans helps detect abnormal glands, while bone density scans reveal osteoporosis or bone weakening
Are parathyroid disorders common?
They are not as common as thyroid disorders but are increasingly seen due to lifestyle changes, rising cases of chronic kidney disease, and complications from thyroid surgeries affecting the parathyroid glands
What is the difference between hyperparathyroidism and hypoparathyroidism?
Hyperparathyroidism results from excess PTH, raising calcium levels in the blood. Hypoparathyroidism is due to insufficient PTH, causing low calcium and symptoms of neuromuscular irritability
Can Ayurveda help in parathyroid disorders?
Yes. Ayurveda provides holistic management by correcting dosha imbalances and nourishing dhatus. Remedies include Praval Pishti, Mukta Sukti Bhasma, Godanti Bhasma, and herbs like Ashwagandha, Guduchi, and Shatavari, which support calcium metabolism and bone strength
Is surgery always needed for parathyroid problems?
Surgery is the primary treatment for severe primary hyperparathyroidism or cancer. However, milder cases may be managed through monitoring, medication, dietary changes, and supportive Ayurvedic therapies
What diet is recommended for parathyroid disorders?
A calcium-rich diet is essential, including milk, sesame, leafy greens, and drumstick leaves. Sunlight exposure is vital for vitamin D. Ayurveda advises limiting sour and salty foods in hyperparathyroidism, while hypoparathyroidism patients benefit from warm, nourishing meals
Are Ayurvedic mineral formulations safe?
Classically prepared Bhasmas, when properly purified according to Rasashastra, are considered safe and effective. However, they must only be taken under the supervision of an Ayurvedic physician to avoid misuse or heavy metal toxicity
Can parathyroid disorders be prevented?
Complete prevention is not always possible, but lifestyle modification helps. Adequate calcium and vitamin D intake, regular sunlight exposure, and Ayurvedic Rasayana therapies strengthen bone and glandular function, reducing susceptibility
About the Doctor
Dr. Arjun Kumar is a qualified Ayurvedic physician with a focused clinical interest in chronic, metabolic, endocrine, and viral disorders. His work is grounded in the classical Ayurvedic principle that disease can be cured by identifying and correcting its root causes, rather than merely suppressing symptoms.
Dr. Kumar’s clinical approach is based on detailed assessment of Dosha imbalance, Dhatu involvement, Agni dysfunction, and Srotas pathology, with particular emphasis on Asthi Dhatu and Majja Dhatu disorders in endocrine conditions. He applies Rasayana therapy, personalized formulations, dietary regulation, and lifestyle correction as central tools aimed at long-term disease resolution and restoration of physiological balance, when applied appropriately and under medical supervision.
While firmly rooted in classical Ayurvedic medicine, Dr. Kumar recognizes the importance of modern diagnostics, laboratory monitoring, and emergency or surgical care where required. His practice follows an integrative yet Ayurveda-first philosophy, where modern medicine is used for diagnosis and stabilization, and Ayurveda is applied for curative, restorative, and preventive healing.
In addition to clinical practice, Dr. Kumar is actively involved in medical writing and research-based education. His work seeks to present Ayurveda as a complete, curative medical science, communicated responsibly and transparently for a global audience, without compromising patient safety or ethical standards.
Medical Disclaimer
This article is intended for educational and informational purposes only and is based on both modern medical literature and classical Ayurvedic medical texts. Parathyroid disorders are complex endocrine conditions, and medical evaluation, diagnosis, and monitoring by qualified healthcare professionals are essential.
Ayurveda, as a complete medical system, aims at curing disease by correcting root causes, restoring tissue balance (Dhatu Samya), regulating metabolism (Agni), and strengthening the body’s inherent healing capacity. When applied correctly, individually, and under proper medical supervision, Ayurvedic treatment is intended not merely for symptom control but for long-term resolution and disease reversal, wherever clinically feasible.
At the same time, this article recognizes that certain situations such as severe hypercalcemia, seizures, cardiac disturbances, or suspected malignancy require immediate modern medical or surgical intervention. In such cases, Ayurvedic treatment should be used integratively and sequentially, not as a replacement for emergency care.
Readers are strongly advised not to self-medicate, especially with mineral or herbomineral formulations. Ayurvedic medicines must be prescribed by a qualified Ayurvedic physician after proper assessment of diagnosis, disease stage, comorbidities, and individual constitution. Special caution is required in pregnancy, chronic kidney disease, history of kidney stones, or advanced systemic illness.
If symptoms such as confusion, seizures, severe muscle spasms, chest pain, or persistent vomiting occur, immediate medical attention is mandatory.
References
- Roumpou, A., & et al. (2025). Bone in Parathyroid Diseases Revisited. Endocrine Reviews, 46(4), 576-596. https://doi.org/10.1093/edrv/8104766
- Lee, M., & et al. (2019). Parathyroid hormone signaling in bone and kidney. Journal of Endocrinology, 241(2), R1-R14. https://doi.org/10.1530/JOE-18-0585
- Taniegra, E.D. (2004). Hyperparathyroidism. American Family Physician, 69(2), 333-339. https://www.aafp.org/pubs/afp/issues/2004/0115/p333.html
- Rejnmark, L., & et al. (2024). Treatment of hypoparathyroidism by re-establishing calcium homeostasis. Endocrinology and Metabolism, 39(1), 13-22. https://doi.org/10.3803/EnM.2024.1916
- Shankar, D., & Valiathan, M.S. (2007). Concepts and principles of Ayurveda. Ancient Science of Life, 26(3), 1-8. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3336313/
- Sharma, R.K., & Dash, B. (Eds.). (2005). Charaka Samhita (Vol. 2: Chikitsa Sthana, Asthi Dhatu Kshaya Adhyaya). Chowkhamba Sanskrit Series.
- Ureña-Torres, P., & et al. (2018). Report of The Parathyroid Day in Chronic Kidney Disease. Frontiers in Medicine, 5, 183. https://doi.org/10.3389/fmed.2018.00183
- Brandi, M.L., & et al. (2016). Management of hypoparathyroidism: summary statement and guidelines. Journal of Clinical Endocrinology & Metabolism, 101(6), 2273-2283. https://doi.org/10.1210/jc.2015-3907
- Fraser, W.D. (2009). Hyperparathyroidism. Lancet, 374(9684), 145-158. https://doi.org/10.1016/S0140-6736(09)60507-9
- Yeh, M.W., & et al. (2013). Surgery for primary hyperparathyroidism: a review. JAMA, 310(24), 2601-2610. https://doi.org/10.1001/jama.2013.282341
- Ketteler, M., & et al. (2025). Chronic kidney disease–mineral and bone disorder. Kidney International, 107(2), 192-208. https://doi.org/10.1016/j.kint.2024.11.018
- Indu, S., Kumar, P.A., Rao, S.K., & Jayaram, H. (2019). Ayurvedic perspective of calcium supplementation: A review. Vitamins & Minerals, 8, Article 185. https://www.researchgate.net/publication/341296797
- Khan, A.A., & et al. (2017). Standards of care for hypoparathyroidism in adults. Nature Reviews Endocrinology, 13, 550-561. https://doi.org/10.1038/nrendo.2017.56
- Bhadada, S.K., & et al. (2011). Dietary calcium intake and serum vitamin D in patients with primary hyperparathyroidism. Indian Journal of Endocrinology and Metabolism, 15(4), S141-S145. https://doi.org/10.4103/2230-8210.84863
- Joshi, N., & et al. (2015). Standardization and quality control parameters for Muktā (pearl) Bhasma/Pishti. Ancient Science of Life, 34(3), 138-143. https://doi.org/10.4103/0257-7941.157152
- Singh, A., Dubey, S.D., Patney, S., Kumar, V., & et al. (2010). Acute and subchronic toxicity study of calcium-based Ayurvedic Bhasmas and Pishti prepared from marine animals. Journal of Herbal Medicine & Toxicology, 4(1), 35-47. https://www.researchgate.net/publication/268432951
- Reddy, P.N., Lakshmana, M., & et al. (2003). Effect of Praval Bhasma (coral calx) in prevention of calcium and estrogen-deficient bone loss. Journal of Ethnopharmacology, 84(2-3), 259-264. https://doi.org/10.1016/S0378-8741(02)00327-2
- Kamble, S., Wanjari, A., Rathi, B., & Rajput, D. (2021). Pharmaceutico-analytical study of Muktashukti Pishti and Bhasma and comparative evaluation of oral bioavailability. Journal of Pharmaceutical Research International, 33(31B), 1-9. https://doi.org/10.9734/jpri/2021/v33i31B31680
- Patgiri, B., & Prajapati, P.K. (2015). Safety and efficacy of Ayurvedic mineral preparations. Ancient Science of Life, 34(1), 1-9. https://doi.org/10.4103/0257-7941.150771
- Valiathan, M.S. (2009). The Legacy of Charaka. Orient Blackswan.