- Ayurvedic Perspectives
- Neuroanatomy of Sexual Function
- Central Nervous System
- Spinal Cord Pathways
- Peripheral Nerves
- Lesser-Known Fact
- Neurochemistry of Sexuality
- Psychoneurobiology of Sexual Arousal
- Gender, Orientation, and Brain Differences
- Neurosexology in Clinical Disorders
- Erectile Dysfunction (ED)
- Female Sexual Dysfunction
- Orgasmic Disorders
- Paraphilias & Hypersexuality
- Neurodegenerative Disorders
- Spinal Cord Injury
- Sexual Pain Disorders and Neurobiology
- Pharmacological & Neuromodulation Approaches
- Drugs Affecting Sexual Function
- Neuromodulation Therapies
- Lesser-Known Fact: Cannabis and Sexual Neurochemistry
- Integrative Neurosexology
- Frequently Asked Questions (FAQ) on Integrative Neurosexology
- Reference
Neurosexology is a scientific discipline dedicated to exploring the intricate relationship between the nervous system and human sexuality. It examines how brain structures, neural pathways, hormones, and psychological processes converge to shape sexual function, behavior, and identity. Unlike traditional sexology, which largely focused on behavioral and physiological aspects, neurosexology integrates multiple disciplines including neuroscience, psychology, endocrinology, and clinical sexology. This multidimensional approach allows for a deeper understanding of the biological and psychological mechanisms that underlie human intimacy [1].
The historical roots of neurosexology can be traced back to early pioneers such as Alfred Kinsey and the team of Masters and Johnson, whose groundbreaking research in the mid-20th century mapped the physiology of sexual response. While their work highlighted the sequence of arousal, plateau, orgasm, and resolution, it left unanswered questions about the role of the brain in regulating these processes. With the advent of neuroimaging techniques such as fMRI and PET scans, researchers began to identify the specific brain regions activated during arousal, desire, and orgasm. This marked the evolution of sexology into a neuroscientific field, opening the door to a more precise and clinically informed understanding of sexual health [2].
In the modern era, the relevance of neurosexology has expanded dramatically. Sexual dysfunction is increasingly common, fueled by chronic stress, the widespread use of antidepressants and antipsychotics, exposure to digital pornography leading to desensitization and erectile dysfunction, and the pressures of sedentary lifestyles. Neurosexology not only offers insights into the neurological underpinnings of these conditions but also provides evidence-based strategies for therapy and prevention. It bridges gaps between physical health, mental health, and sexual well-being, making it indispensable in both clinical and wellness contexts [3].
A lesser-known fact about this field is that the term neurosexology was first coined in the late 20th century, primarily in the context of rehabilitation medicine. It emerged to address the sexual health of patients with spinal cord injuries, recognizing that sexuality is not extinguished by neurological impairment but instead reorganized through alternative neural pathways. This early clinical focus laid the foundation for a broader discipline that now informs not only sexual rehabilitation but also the holistic treatment of sexual dysfunction across diverse populations [4].
Ayurvedic Perspectives
Classical Ayurveda has long recognized the intimate connection between the nervous system (Majja Dhatu and Manovaha Srotas) and sexual vitality (Shukra Dhatu). According to Charaka Samhita, the strength of Shukra Dhatu determines not only reproductive capacity but also Ojas, the vital essence that sustains life, immunity, and mental stability [5]. The nervous system’s role in arousal, memory, and desire aligns with the Ayurvedic concept of Manas (mind) being deeply interlinked with sensory and motor functions. Thus, what neurosexology investigates through neural pathways, Ayurveda explains through the interaction of Sharirika Doshas (Vata, Pitta, Kapha) with Manasika Doshas (Rajas and Tamas).
- Majja Dhatu (Bone marrow and nervous tissue): Described as the substratum of nervous function, closely governing sensory and motor responses. Disturbances in Majja lead to disorders of perception, memory, and sexual drive [6].
- Manovaha Srotas (mental pathways): Responsible for thought, desire, and emotional balance. Dysfunction here leads to Kama-viparyaya (abnormal sexual behavior), Smriti-bhramsha (distorted memory of erotic cues), and premature loss of libido [7].
- Shukra Dhatu (reproductive tissue): The final refinement of all bodily dhatus, regulating fertility, vigor, and sexual performance. Its depletion manifests as erectile dysfunction, infertility, and weakened orgasmic capacity [8].
Ayurveda also emphasizes Vajikarana Rasayana (aphrodisiac rejuvenation), which is considered essential for maintaining both nervous and reproductive integrity. Classical texts highlight formulations such as Ashwagandha, Kapikacchu, Shatavari, and Suvarna Bhasma, which modern studies show act on dopaminergic, serotonergic, and neuroendocrine pathways, reflecting a close parallel with neurosexology’s biochemical focus [9].
The integrative view thus reveals that while modern neurosexology uses imaging and neurochemistry to understand desire and arousal, Ayurveda conceptualized the same through Dosha–Dhatu–Srotas balance centuries earlier. Together, these perspectives provide a comprehensive framework for addressing the rising epidemic of sexual dysfunction in a way that is both scientifically rigorous and philosophically holistic.
Neuroanatomy of Sexual Function
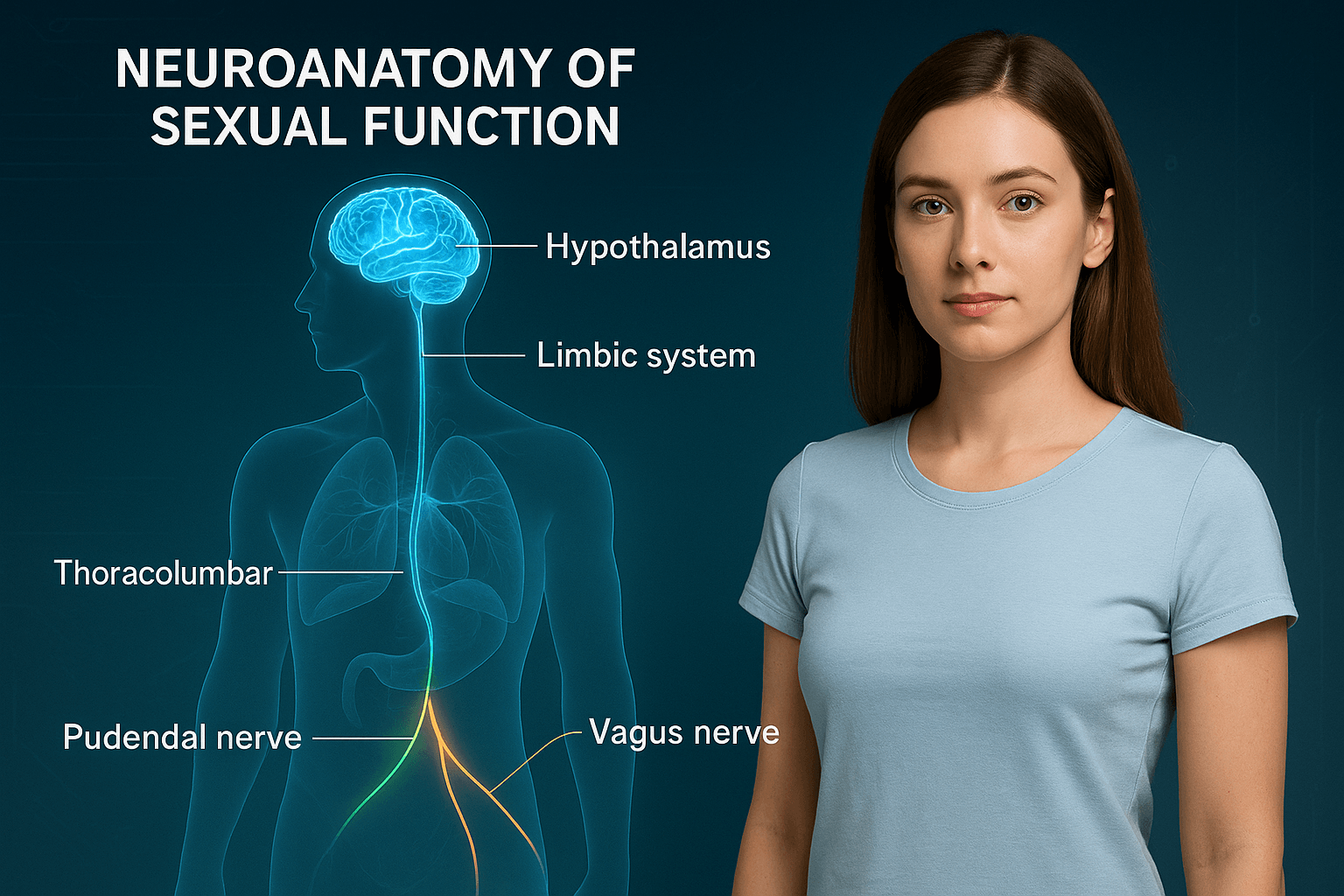
Human sexuality is a deeply integrated function of the nervous system. It is not governed by a single organ but by a network of interconnected regions within the brain, spinal cord, and peripheral nerves. This intricate system regulates desire, arousal, orgasm, and emotional bonding. Understanding the neuroanatomy of sexual function is essential for grasping how disorders arise and how therapies can be targeted effectively.
Central Nervous System
Hypothalamus
The hypothalamus is the command center for sexual desire and autonomic control of reproductive behaviors. Within it, the medial preoptic area (MPOA) acts as a central hub for initiating sexual behavior. Animal and human studies consistently show that damage to this area diminishes sexual motivation, whereas stimulation increases sexual activity [1]. The paraventricular nucleus (PVN) of the hypothalamus is responsible for oxytocin release, which plays a pivotal role in orgasm, bonding, and trust formation. Oxytocin, often called the “cuddle hormone,” enhances pair bonding and reinforces positive sexual experiences.
Limbic System
The limbic system, particularly the amygdala and hippocampus, integrates emotional and memory components of sexuality. The amygdala processes sexual motivation and emotional salience of erotic cues, while the hippocampus encodes memory of these cues, allowing individuals to associate certain stimuli, settings, or people with sexual arousal. Dysfunction in the limbic system can lead to diminished desire, altered sexual preferences, or in some cases, compulsive behaviors.
Prefrontal Cortex
The prefrontal cortex serves as the “brake” system of sexual behavior. It is involved in inhibition, judgment, and decision-making. This region determines the appropriateness of sexual expression in social and cultural contexts. Overactivation of the prefrontal cortex may suppress natural arousal, while impaired inhibition (as seen in frontal lobe injury or dementia) may cause hypersexuality or socially inappropriate behaviors [2].
Spinal Cord Pathways
Sacral Reflex Arc
Sexual function is strongly mediated by reflexogenic pathways. The sacral parasympathetic arc, originating in the S2–S4 spinal segments, controls penile erection in men and vaginal lubrication in women. These responses can occur even in the absence of conscious arousal, highlighting the reflexive nature of genital engorgement [3].
Thoracolumbar Sympathetic Pathways
Orgasm and ejaculation are governed by the thoracolumbar sympathetic system (T11–L2). These pathways orchestrate rhythmic contractions of pelvic muscles, emission of semen, and uterine/vaginal contractions during orgasm. The coordination between parasympathetic and sympathetic systems underlies the climax phase of sexual response.
Vagal Nerve Involvement in Female Orgasm
The vagus nerve provides a remarkable bypass route. Unlike most sexual pathways that ascend through the spinal cord, the vagus nerve transmits sensory information from the cervix and uterus directly to the brainstem. This explains how women with complete spinal cord injuries can still achieve orgasm, as the vagal pathway remains intact [4].
Peripheral Nerves
Pudendal Nerve
The pudendal nerve is the principal conduit of genital sensation. It transmits tactile stimuli from the penis and clitoris to the sacral spinal cord, forming the afferent limb of orgasmic reflexes. It also controls contraction of pelvic floor muscles that intensify orgasmic pleasure.
Dorsal Nerve of the Penis/Clitoris
This branch of the pudendal nerve provides specialized innervation for erogenous sensation. It is particularly sensitive to mechanical stimulation and plays a central role in arousal and orgasmic reflex loops [5].
Lesser-Known Fact
A fascinating clinical observation is that some women with complete spinal cord transection still report orgasms. This phenomenon is explained by the vagal pathways, which connect the cervix and uterus directly to the brain without requiring spinal cord mediation. These findings highlight the redundancy and adaptability of the female sexual nervous system, and they also reinforce the importance of recognizing multiple parallel pathways in sexual function [6].
Neurochemistry of Sexuality
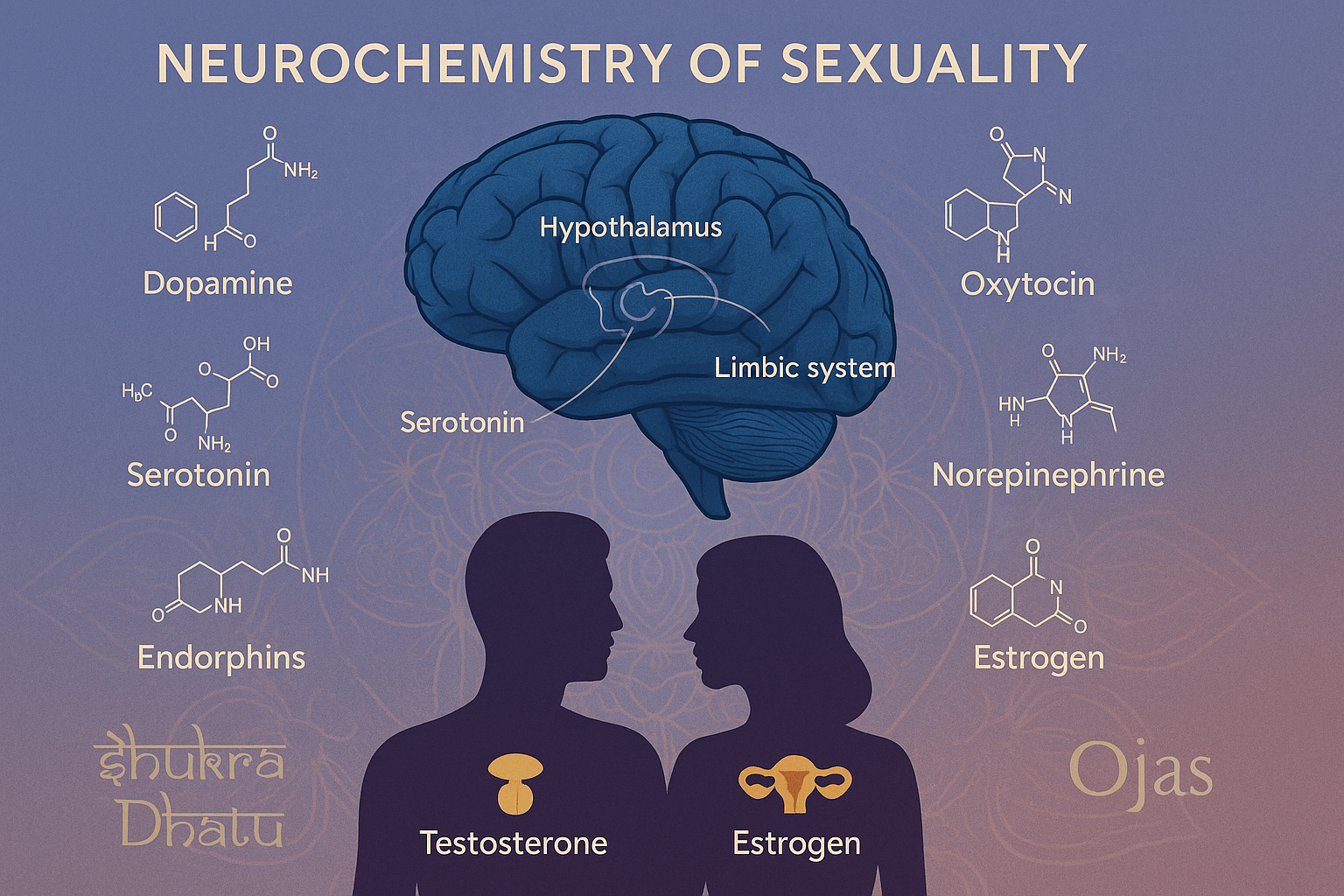
The chemistry of sexuality is orchestrated by a dynamic interplay of neurotransmitters and hormones that regulate desire, arousal, orgasm, and post-coital bonding. Modern neurosexology identifies a complex network of neurochemicals acting within the brain’s reward and emotional centers, while Ayurveda offers a parallel understanding through the balance of Doshas, Dhatus, and the flow of Manovaha Srotas.
Dopamine
Dopamine is the cornerstone of sexual desire and motivation, driving the initiation of arousal through the mesolimbic reward system. When an individual experiences attraction, erotic stimuli, or anticipates pleasure, dopamine surges within the ventral tegmental area (VTA) and nucleus accumbens, reinforcing sexual pursuit. This neurochemical “spark” explains why dopamine deficiency, as seen in Parkinson’s disease or chronic stress, leads to loss of libido and anhedonia. From an Ayurvedic standpoint, dopamine parallels the Vata dosha, especially its Prana Vata subtype, which governs sensory input, enthusiasm, and initiation of activity. When Vata is balanced, sexual curiosity and drive remain strong; when depleted, as in excessive worry or over-exertion, desire diminishes. Rasayana herbs such as Kapikacchu (Mucuna pruriens), rich in L-DOPA, directly nourish dopaminergic pathways, aligning with both neurochemical and classical frameworks. Thus, dopamine is not merely a “pleasure chemical” but a biological bridge between motivation, reward, and the Ayurvedic spark of life [1].
Serotonin
Serotonin exerts an inhibitory influence on sexuality, moderating desire and delaying orgasm. Elevated serotonin levels, such as those induced by SSRIs, often result in delayed ejaculation or anorgasmia, one of the most common medication-related sexual dysfunctions. This neurotransmitter plays a protective role in mood regulation and impulse control but becomes problematic when overexpressed in sexual circuits. Ayurveda echoes this balance through Kapha dosha, which governs stability, heaviness, and retention. Just as serotonin can “hold back” orgasm, Kapha in excess causes lethargy, dullness, and diminished responsiveness to sexual stimuli. Conversely, Kapha balance provides emotional security and endurance in intimacy. Classical texts describe conditions like Klaibya (impotence) where excess heaviness and suppression dominate, reflecting serotonergic overactivity. Corrective therapies include Kapha-pacifying diets, detoxification, and Rasayanas such as Triphala and Guduchi, which restore vitality. Thus, serotonin functions as a double-edged sword, necessary for balance but detrimental when unchecked [2].
Oxytocin
Oxytocin, often called the “cuddle hormone,” is a key player in post-orgasmic bonding, trust, and intimacy. Released during sexual climax, breastfeeding, and affectionate touch, it strengthens pair-bonding and reinforces feelings of safety with a partner. Oxytocin’s role extends beyond pleasure—it is a biological glue for long-term attachment and relationship stability. In Ayurveda, this correlates with Ojas, the subtle essence of all Dhatus, which sustains vitality, immunity, and emotional harmony. Ojas is enhanced by acts of love, compassion, and Rasayana therapy, just as oxytocin rises during nurturing interactions. Low oxytocin levels are associated with detachment, lack of empathy, and even sexual dissatisfaction. Modern studies show oxytocin nasal sprays can improve arousal and intimacy, while Ayurveda emphasizes foods, meditation, and herbs like Shatavari and Ashwagandha for nurturing Ojas. Both systems converge on one truth: oxytocin is not just about reproduction, but about sustaining human connection [3].
Norepinephrine
Norepinephrine enhances the physiological arousal that precedes sexual climax. It elevates heart rate, blood pressure, and alertness, creating the heightened anticipation that characterizes erotic excitement. Released primarily from the locus coeruleus, norepinephrine activates the sympathetic nervous system, energizing the body for sexual performance. However, chronic stress and overstimulation can desensitize this system, leading to burnout and diminished responsiveness. Ayurveda parallels norepinephrine’s fiery nature with Pitta dosha, particularly its Sadhaka Pitta subtype, which governs passion, focus, and emotional intensity. Balanced Pitta ignites sexual enthusiasm, while aggravated Pitta leads to irritability, premature ejaculation, or excessive sexual drive. Herbs such as Brahmi (Bacopa monnieri) and cooling therapies help stabilize excessive sympathetic activity while preserving healthy arousal. Norepinephrine thus illustrates the delicate line between passion and agitation, showing that both modern neurochemistry and Ayurveda recognize the importance of harnessing sexual fire without allowing it to consume equilibrium [4].
Endorphins
Endorphins are natural opioids released during orgasm, producing euphoria, deep relaxation, and analgesia. They provide a neurochemical “afterglow,” often linked to post-coital satisfaction and intimacy. Endorphins also buffer pain, which explains why sexual climax can momentarily alleviate chronic pain conditions like migraine or dysmenorrhea. Ayurveda recognizes a similar bliss state in the refinement of Shukra Dhatu, where the reproductive essence is said to nourish not only fertility but also joy, mental calmness, and spiritual contentment. The experience of Shukra prasada aligns with the endorphin high—both are peak expressions of vitality transformed into delight. Practices such as yoga, chanting, and Rasayana tonics (e.g., Swarna Bhasma and Abhrak Bhasma) are said to enrich Shukra and strengthen Ojas, paralleling endorphin-driven well-being. Endorphins therefore reveal sexuality’s deeper role beyond reproduction, as a neurochemical and Ayurvedic gateway to health, happiness, and transcendence [5].
GABA
Gamma-Aminobutyric Acid (GABA) is the brain’s chief inhibitory neurotransmitter, moderating neural overactivity and promoting calm. In the sexual domain, adequate GABA tone ensures relaxation and receptivity, while deficiency may result in performance anxiety or premature climax. Conversely, excessive GABA can suppress arousal and contribute to anorgasmia. Ayurveda resonates with this duality through Tamas guna, the principle of inertia and suppression. When Tamas dominates, sexual expression becomes blocked, mirroring excess GABA inhibition. Yet in balance, Tamas provides grounding and steadiness essential for deep intimacy. Ayurvedic therapies that reduce excessive Tamas—such as Sattvavajaya chikitsa (mental purification), Satvic diet, and herbs like Tulsi and Jyotishmati—restore equilibrium. Interestingly, modern research finds that yoga and meditation naturally enhance GABA activity, paralleling ancient Ayurvedic mind-body practices. Thus, GABA demonstrates how balance, rather than extremes, defines healthy sexual expression [6].
Hormonal Regulation
Sexuality is profoundly influenced by hormones, which act as long-term regulators of libido and arousal. Testosterone, present in both men and women, enhances desire, sensitivity, and assertiveness. Estrogen facilitates vaginal lubrication and increases clitoral blood flow, heightening female arousal, while progesterone often dampens sexual interest and readiness. These hormonal rhythms are cyclical, explaining variations in desire across menstrual, seasonal, and life stages. Ayurveda parallels this with its understanding of Shukra Dhatu and Rakta Dhatu, which together form the substratum of reproductive strength and passion. Imbalances in these Dhatus manifest as Klaibya (erectile dysfunction), Yoni-vyapad (female sexual disorders), or Vandhyatva (infertility). Vajikarana therapy emphasizes restoring hormonal and Dhatu balance through Rasayanas like Ashwagandha, Shatavari, Gokshura, and mineral preparations such as Suvarna Bhasma. Both Ayurveda and modern endocrinology affirm that sexual health requires dynamic balance between stimulating and inhibitory forces [7].
Lesser-Known Fact: Prolactin and Refractory Period
A fascinating aspect of sexual neurochemistry is the role of prolactin, a hormone best known for stimulating lactation. After orgasm, men experience a sharp prolactin surge, which induces the refractory period—a temporary phase during which sexual arousal and erection are physiologically suppressed. This effect is far less pronounced in women, allowing them the capacity for multiple orgasms within short intervals. Ayurveda indirectly acknowledges this distinction in classical texts, noting that women, when endowed with abundant Shukra and Ojas, can engage in repeated sexual activity without fatigue, whereas men experience post-coital depletion. The post-orgasmic prolactin spike also explains why men often feel drowsy or experience mood changes after intercourse. Modern science validates these ancient observations, highlighting prolactin as a natural safeguard against overstimulation. This integration of neuroendocrinology and Ayurveda emphasizes that sexual recovery, like arousal, is rooted in rhythms of balance and replenishment [8].
Psychoneurobiology of Sexual Arousal
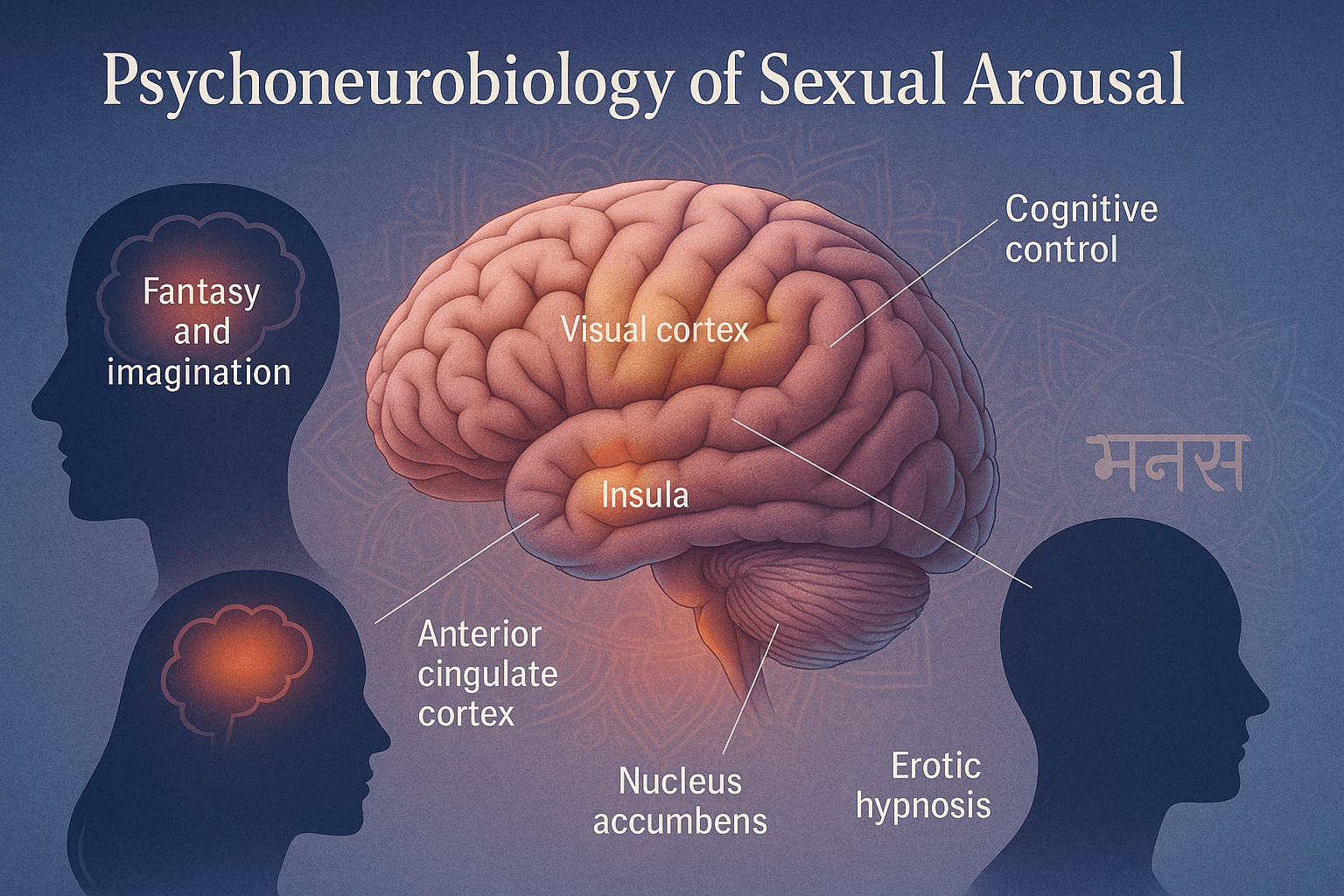
Brain Activation
Functional MRI (fMRI) studies have revealed that sexual arousal is not confined to one brain center but engages a widespread network. The visual cortex responds to erotic imagery, while the insula processes visceral sensations of arousal. The anterior cingulate cortex integrates emotional anticipation, and the nucleus accumbens registers pleasure and reward. Together, these regions orchestrate the transition from desire to physiological arousal. From an Ayurvedic lens, this multi-regional activation parallels the Manovaha Srotas (mental pathways), which coordinate sensory inputs (Indriyas) with internal responses. Arousal reflects balanced Rajas guna, the dynamic force of passion, guiding energy toward intimacy. When overstimulated or depleted, however, Vata or Pitta imbalance manifests as premature arousal, anxiety, or irritability. Thus, modern imaging validates what Ayurveda long emphasized—that sexual arousal is not purely genital but a whole-brain, whole-body experience where perception, memory, and vitality converge [1].
Fantasy and Imagination
Sexuality extends beyond physical stimuli; imagination alone can ignite the same neural circuits as actual intimacy. Studies show that fantasy-driven arousal activates the limbic system, amygdala, and sensory cortices, producing physiological changes like genital blood flow, increased heart rate, and heightened dopamine release. This demonstrates the brain’s remarkable ability to blur lines between real and imagined experiences. Ayurveda also acknowledged the power of the mind in shaping sexual vitality, describing Kama (desire) as both a mental and physical phenomenon. Excessive indulgence in fantasy is cautioned against in texts like Charaka Samhita, as it can drain Shukra Dhatu and weaken Ojas. Yet, balanced imagination—expressed through love, poetry, or daydreams—is seen as a source of rejuvenation. Thus, fantasy is neither inherently harmful nor trivial; it is a potent psychoneural force that must be moderated to sustain harmony in sexual and emotional life [2].
Cognitive Control
The prefrontal cortex (PFC) plays a regulatory role in sexual arousal, acting as both accelerator and brake. Depending on cultural conditioning, personal values, and social context, the PFC may suppress arousal (through inhibition) or enhance it by focusing attention and anticipation. This explains why guilt, shame, or fear can inhibit desire, even in the presence of strong physical stimuli, while mindfulness or intentional focus can heighten responsiveness. Ayurveda mirrors this function in the domain of Sattva guna, which governs clarity, discrimination, and self-mastery. A sattvic mind refines desire into healthy intimacy, while dominance of Rajas or Tamas distorts impulses into obsession or suppression. Classical therapies such as Satvavajaya Chikitsa (cognitive–behavioral Ayurvedic therapy) aim to realign the mind’s control over arousal, paralleling modern psychosexual interventions. Thus, cognitive control demonstrates how beliefs and culture shape biology, confirming that sexual health is inseparable from mindset [3].
Lesser-Known Fact: Erotic Hypnosis
An intriguing finding in neurosexology is that erotic hypnosis can activate deeper limbic structures and bypass conscious inhibition, creating heightened or altered sexual experiences. Under trance, the amygdala and hippocampus engage more directly with arousal pathways, while the prefrontal cortex’s critical control loosens. This explains phenomena such as enhanced orgasm, increased receptivity, and the ability to experience sensations without direct stimulation. Ayurveda described a comparable state through Tantric and meditative practices, where the dissolution of conscious filters (Avarana) allows subtle energies (Prana and Shukra) to flow freely through the Sushumna Nadi. Such practices were not meant for indulgence alone but for transforming sexual energy into spiritual vitality. Modern science thus converges with ancient wisdom in recognizing that altered states of consciousness can unlock hidden dimensions of sexuality, where inhibition gives way to deeper emotional and physiological release [4].
Gender, Orientation, and Brain Differences
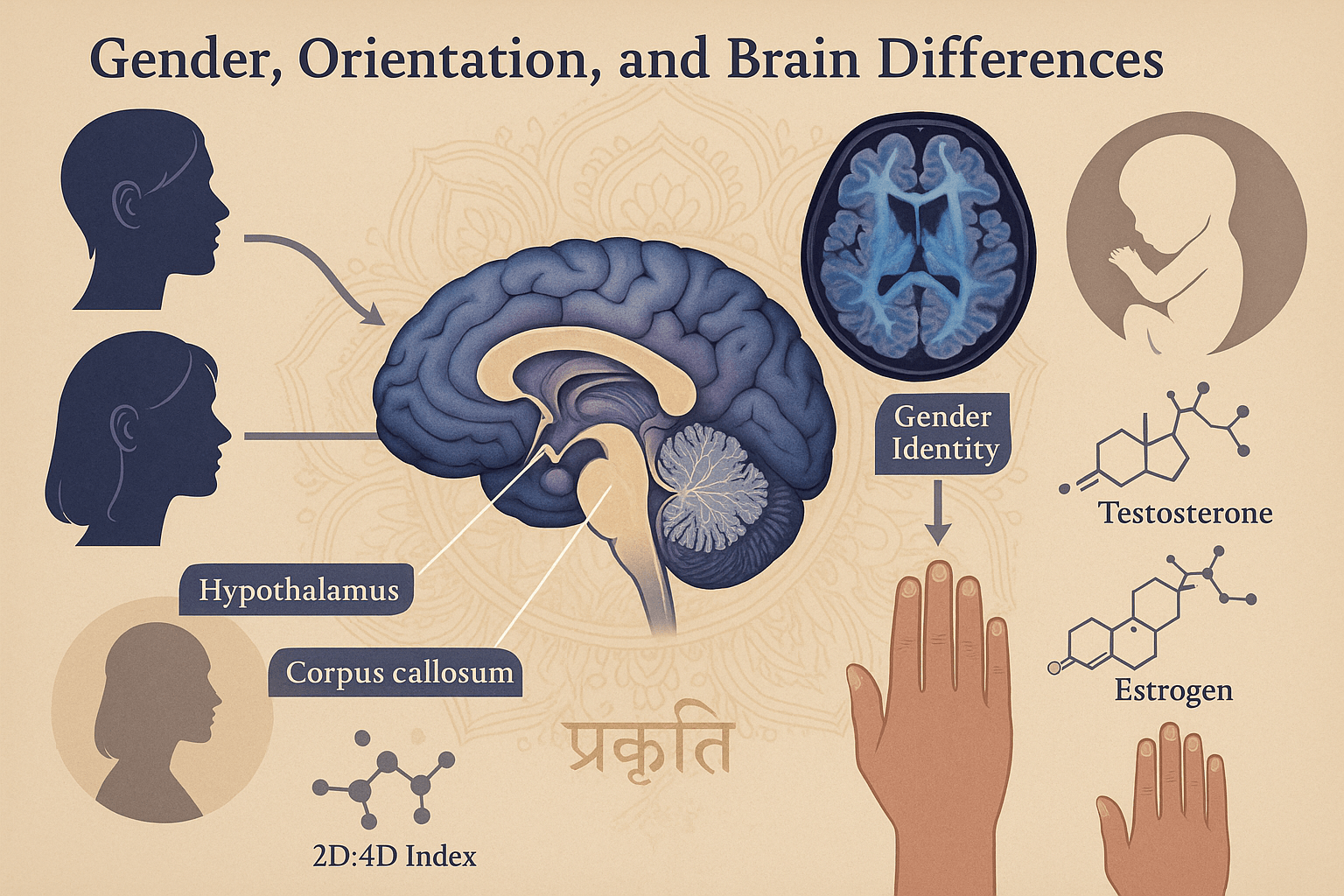
Sexual Orientation
Modern neuroimaging studies suggest that sexual orientation is associated with structural and functional brain differences. For example, certain nuclei within the hypothalamus differ in size and activity between heterosexual and homosexual individuals. The corpus callosum, which facilitates interhemispheric communication, has been found to exhibit structural variations across sexual orientations, potentially reflecting differences in emotional and sensory integration. These findings underscore that orientation is not a simple matter of choice but is rooted in neurobiology. Ayurveda, while not categorizing sexual orientation in modern terms, recognizes Kama (desire) as a natural variation among individuals. Classical texts describe conditions such as Napumsaka (third-gender individuals) and acknowledge diversity in sexual preference without condemnation. This aligns with the idea that orientation arises from Prakriti (innate constitution), molded by both biology and karmic factors. Thus, both modern science and Ayurveda point toward orientation as a naturally determined aspect of identity rather than a deviation [1].
Gender Identity
Neuroimaging research reveals that transgender individuals often exhibit brain connectivity patterns that align more closely with their experienced gender rather than their sex assigned at birth. Studies of white matter tracts, cortical thickness, and resting-state connectivity show shifts toward the gender with which they identify. This provides neurobiological validation for gender dysphoria and identity affirmation, showing that gender experience is deeply embedded in the brain’s architecture. Ayurveda provides a nuanced lens, acknowledging conditions beyond binary male–female classification through the concept of Tritya Prakriti (third nature). Classical texts recognize individuals with both masculine and feminine traits or behaviors, situating gender identity within a spectrum of natural expressions. These are said to arise from dosha imbalances during conception or from karmic imprints affecting fetal development. Together, modern neurosexology and Ayurveda affirm that gender identity is neither purely psychological nor cultural, but an authentic neurobiological and constitutional reality [2].
Prenatal Hormones
Exposure to testosterone and estrogen during critical windows of fetal development plays a decisive role in shaping sexual differentiation of the brain. Elevated prenatal testosterone influences masculinization, affecting hypothalamic development and later sexual behavior patterns. Conversely, estrogen modulates neural circuits linked to nurturing and bonding. These hormonal effects persist into adulthood, influencing orientation, libido, and gender expression. Ayurveda reflects this in its understanding of Garbha Sanskara (prenatal influences), emphasizing that the state of doshas, maternal diet, and emotional balance during pregnancy profoundly shapes fetal physiology and psychology. Classical texts describe how disturbances in Shukra (reproductive tissue) and Rakta (blood tissue) during gestation can predispose the child toward variations in constitution and identity. Thus, what modern science explains through sex steroids, Ayurveda maps through the interplay of doshas and maternal environment, reinforcing that identity is seeded before birth [3].
Lesser-Known Fact: Finger Length Ratio
One intriguing and lesser-known marker of prenatal androgen exposure is the finger length ratio, specifically the 2D:4D index (the ratio of index finger to ring finger length). Research shows that a lower 2D:4D ratio (shorter index relative to ring finger) is associated with higher prenatal testosterone exposure, while a higher ratio indicates greater prenatal estrogen exposure. These ratios have been correlated with variations in sexual orientation, athletic ability, and even libido intensity. While not definitive, this subtle biometric marker underscores how deeply prenatal hormones imprint on development. Ayurveda, though not describing finger ratios, does emphasize Lakshana (bodily signs) as indicators of constitution and temperament. Ancient texts note that the shape and proportion of limbs reflect underlying doshic dominance and even tendencies in behavior. In this way, both traditions use physical markers as windows into deeper physiological and psychological predispositions [4].
Neurosexology in Clinical Disorders
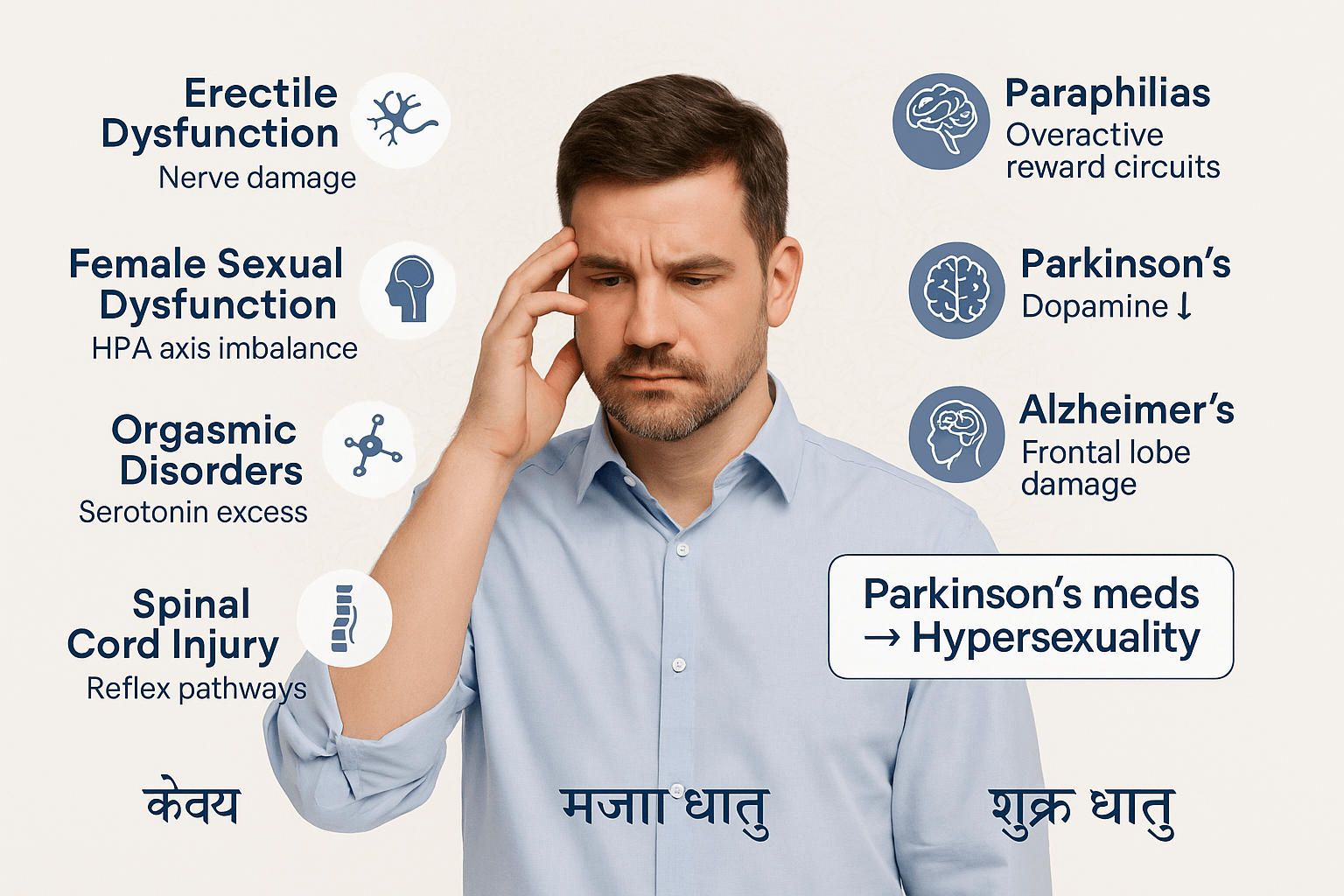
Erectile Dysfunction (ED)
Neurogenic erectile dysfunction occurs when the communication between brain, spinal cord, and penile nerves is disrupted. Conditions such as diabetes, multiple sclerosis, spinal cord injury, or pelvic nerve trauma impair nitric oxide release and neural conduction, leading to weak or absent erections. While PDE-5 inhibitors help vascular causes, they are less effective in neurogenic ED. Ayurveda describes a similar condition under Klaibya (impotence), often arising from Vata vitiation that blocks Shukra vaha srotas (reproductive channels). Rasayanas like Ashwagandha, Kapikacchu, and Suvarna Bhasma are prescribed to restore nerve vigor, while therapies such as Mardana (therapeutic massage) and Shirodhara improve neurovascular integration. Thus, both modern neurosexology and Ayurveda highlight that ED is not merely physical but a complex neurovascular condition demanding holistic rehabilitation [1].
Female Sexual Dysfunction
Female sexual dysfunction, particularly reduced arousal and difficulty achieving orgasm, is frequently associated with hypothalamic–pituitary axis imbalance and the suppressive effects of antidepressants. Serotonergic drugs blunt sexual responsiveness, while hormonal disturbances from thyroid or pituitary dysfunction further impair libido and lubrication. Ayurveda explains this through imbalance in Apana Vata (pelvic energy) and depletion of Shukra Dhatu, often aggravated by chronic stress, poor nutrition, or excessive Kapha. Therapies such as Shatavari, Guduchi, and Abhrak Bhasma restore neuroendocrine balance and nourish reproductive tissues. Panchakarma procedures like Basti (medicated enema) are also recommended to regulate pelvic neurology and hormonal rhythms. In both paradigms, female dysfunction is not a singular disease but a multidimensional disruption involving brain, hormones, and mind [2].
Orgasmic Disorders
Anorgasmia and delayed orgasm frequently stem from excess serotonin activity or overactive prefrontal inhibition, which suppresses limbic reward pathways. Antidepressants, anxiety, or rigid cognitive control can block orgasm despite adequate arousal. Neuroimaging shows reduced activity in the nucleus accumbens and limbic regions in anorgasmic patients. Ayurveda conceptualizes orgasm (Rati sukha) as a refined expression of Shukra Dhatu and Majja Dhatu (nervous tissue). When these are weakened—by chronic illness, excessive Rajas (overexcitement), or Tamas (inhibition)—orgasm is impaired. Vajikarana herbs like Kapikacchu, Safed Musli, and Swarna Makshik Bhasma are used to restore nervous excitability and reproductive vigor. Thus, orgasmic disorders reflect the intersection of neurochemistry and mind-body imbalance, requiring treatments that address both psychological release and neurophysiological flow [3].
Paraphilias & Hypersexuality
Paraphilic behaviors and hypersexuality are linked to overactivation of brain reward circuits (dopamine-driven pathways) combined with impaired frontal inhibition. Compulsive sexual behavior resembles addiction, with cravings, tolerance, and withdrawal symptoms. Neurosexology classifies this as a neuropsychiatric condition, often comorbid with obsessive-compulsive disorder or bipolar disorder. Ayurveda offers a lens through Rajas–Tamas imbalance, where excessive Rajas drives uncontrolled desire while Tamas suppresses rational control. Such disturbances result in Vyavichari Chitta (unstable mind) and abnormal expressions of Kama. Treatments include Satvavajaya Chikitsa (counseling, mindfulness, and restraint training), along with herbs such as Brahmi and Jyotishmati to stabilize cognitive control. Both systems view hypersexuality as a disorder of imbalance—whether in dopamine regulation or mental Gunas—requiring therapies that restore restraint and healthy pleasure-seeking [4].
Neurodegenerative Disorders
Parkinson’s disease causes reduced libido due to dopamine deficiency in the nigrostriatal and mesolimbic pathways. Interestingly, dopamine replacement therapy can trigger hypersexuality, impulsive behaviors, and obsessive romantic fixation, highlighting dopamine’s dual role in desire and control. Alzheimer’s disease, by contrast, often results in disinhibited sexual behaviors due to frontal lobe degeneration. Patients may display inappropriate advances, not from heightened desire but from loss of social inhibition. Ayurveda contextualizes these disorders within Majja Dhatu kshaya (degeneration of nervous tissue) and Vata vriddhi (excess Vata). Classical Rasayanas like Swarna Bhasma, Abhrak Bhasma, and Medhya herbs (Brahmi, Mandukaparni) were prescribed for degenerative neurological conditions. Thus, neurodegenerative diseases reveal how deeply sexual function is tied to the nervous system’s integrity, with both science and Ayurveda advocating nerve-nourishing therapies [5].
Spinal Cord Injury
Spinal cord injuries disrupt the neural pathways that mediate arousal, erection, and orgasm. However, many patients retain reflexogenic responses—automatic erections or lubrication triggered by direct genital stimulation, independent of brain input. Modern rehabilitation uses electrical stimulation, vacuum devices, and counseling to restore sexual function. Ayurveda identifies this as Vata vyadhi (neurological disorder) impairing Shukra vaha srotas. Treatment emphasizes Rasayanas like Ashwagandha, Shilajit, and Suvarna Bhasma for nerve regeneration, combined with Panchakarma therapies such as Abhyanga (oil massage) and Basti to strengthen pelvic and spinal function. The convergence of these approaches suggests that even after severe neural disruption, sexual vitality can be partially restored through reflex pathways and holistic rejuvenation [6].
Lesser-Known Fact
A striking clinical observation is that dopamine agonists, used to treat Parkinson’s disease, sometimes trigger compulsive sexual behaviors, gambling, and hyper-romantic obsessions. This paradox illustrates how neurochemical therapy can unleash hidden circuits of desire by overstimulating reward pathways. Ayurveda mirrors this insight with warnings against excessive Rasayana or Vajikarana use without proper balance, noting that unregulated stimulation of Shukra and Rajas can destabilize the mind. Both traditions caution that sexual energy, though therapeutic, must be channeled responsibly to avoid compulsive or destructive outcomes [7].
Sexual Pain Disorders and Neurobiology
Dyspareunia & Vulvodynia
Dyspareunia (painful intercourse) and vulvodynia (chronic vulvar pain) are increasingly recognized as neurobiological disorders rather than purely gynecological problems. Research shows that hyperactive pain pathways in the spinal cord and brain, combined with central sensitization, amplify normal sensations into pain. fMRI studies reveal increased activity in pain-processing regions such as the anterior cingulate cortex and insula, even in the absence of physical injury. Ayurveda classifies such conditions under Yonivyapad (disorders of the female reproductive tract) and attributes them to aggravated Vata dosha, which governs pain, movement, and neurosensory activity. Classical therapies such as Yoni Pichu (medicated oil tampons), Basti (enemas with oil and herbs), and Rasayanas like Ashwagandha and Bala are recommended to calm Vata and reduce hypersensitivity. This dual lens shows that vulvodynia and dyspareunia are not merely “local issues,” but disorders of the nervous system demanding both neural and holistic healing [1].
Chronic Pelvic Pain Syndromes
Chronic pelvic pain syndromes (CPPS) represent a complex interplay of gynecological, urological, gastrointestinal, and neurological disturbances. Many patients with CPPS also suffer from fibromyalgia, irritable bowel syndrome, or chronic fatigue, indicating a shared mechanism of central sensitization—where the nervous system amplifies pain perception across multiple organ systems. Neurosexology highlights how these conditions are not independent but interconnected through common neural pathways. Ayurveda conceptualizes CPPS as Apana Vata vitiation, where deranged pelvic energy disrupts the functions of Mutravaha (urinary), Artavavaha (menstrual), and Purishavaha srotas (bowel channels) simultaneously. Treatment protocols include Basti therapy, yoga postures for pelvic grounding, and Rasayanas like Gokshura, Shatavari, and Abhrak Bhasma. Both traditions affirm that chronic pelvic pain is not “all in the mind” but arises from a system-wide dysregulation of pain networks, requiring a biopsychosocial and integrative management approach [2].
Lesser-Known Fact: Vaginismus and the Brain
A fascinating discovery in neurosexology is that some cases of vaginismus—a condition where involuntary tightening of vaginal muscles prevents penetration—are not purely muscular but neurocognitive. Functional brain imaging shows hyperactivation of the amygdala (fear center) and motor cortex, suggesting the brain is “anticipating pain” and triggering muscle spasm reflexively. This explains why conventional pelvic floor therapy often fails without addressing the fear–anxiety loop. Ayurveda recognized this link long ago, describing vaginismus-like disorders under Yonivyapad caused by Chitta vikaras (mental disturbances) and aggravated Vata. Management included Sattvavajaya Chikitsa (cognitive–behavioral therapy through counseling, mantra, meditation) alongside local therapies to relax pelvic Vata. Thus, vaginismus illustrates how sexual pain can originate in the mind–brain circuits as much as in muscles, validating the need for both neurological retraining and holistic balance of body–mind energies [3].
Pharmacological & Neuromodulation Approaches
Drugs Affecting Sexual Function
Pharmacological agents profoundly influence sexual desire, arousal, and orgasm. Selective serotonin reuptake inhibitors (SSRIs), widely prescribed for depression, are notorious for suppressing libido and delaying orgasm by amplifying serotonergic inhibition of limbic circuits. In contrast, Bupropion, a norepinephrine–dopamine reuptake inhibitor, enhances sexual desire by boosting dopamine activity in the reward pathways, often prescribed to counteract SSRI-induced dysfunction. Phosphodiesterase-5 inhibitors (PDE-5i) such as sildenafil, though primarily acting peripherally to improve penile blood flow, also modulate central arousal centers by influencing nitric oxide pathways. Ayurveda acknowledges similar drug-induced sexual disturbances under Aushadha-janita Klaibya (impotence caused by medicines). The antidote is Vajikarana Rasayana therapy, using agents like Kapikacchu, Ashwagandha, and Suvarna Bhasma to restore Shukra Dhatu and balance Vata–Pitta derangements. Both systems emphasize that pharmaceutical interventions can either suppress or stimulate sexual function, underscoring the need for personalization and balance [1].
Neuromodulation Therapies
Beyond pharmacology, neuromodulation offers innovative solutions for sexual dysfunction. Transcranial magnetic stimulation (TMS) has shown promise in treating hypoactive sexual desire disorder by activating prefrontal–limbic circuits, enhancing both mood and arousal. Similarly, vagus nerve stimulation (VNS) has been explored for female anorgasmia, leveraging its unique ability to bypass spinal pathways and directly connect pelvic organs to the brain. These approaches highlight that arousal is not purely hormonal or vascular, but deeply neurologically orchestrated. Ayurveda provides a parallel in its emphasis on Marma Chikitsa (vital point therapy) and Shirodhara (neuro-calming oil therapy), which modulate neural activity through sensory–motor gateways. Just as TMS re-tunes cortical circuits, these therapies are designed to calm Vata and enhance mind–body integration. Neuromodulation thus represents a convergence of modern brain-targeted interventions and classical neuro-energetic therapies [2].
Lesser-Known Fact: Cannabis and Sexual Neurochemistry
Cannabis use has a dual effect on sexual function. Short-term, it increases dopamine and oxytocin release, leading to heightened sensitivity, enhanced bonding, and altered erotic perception. Many report intensified orgasms or prolonged foreplay. However, chronic use has the opposite effect: lowering testosterone, impairing sperm count, and reducing fertility. Neurosexology interprets this as overstimulation of reward circuits followed by downregulation. Ayurveda, while not naming cannabis directly, describes similar outcomes under Madya (intoxicants)—temporary stimulation of Rajas, followed by depletion of Shukra Dhatu and Ojas. Prolonged use is warned against for causing infertility, nervous depletion, and lethargy. This paradoxical impact underscores the delicate balance of sexual neurochemistry, where short-lived enhancement can mask long-term harm if not moderated [3].
Integrative Neurosexology
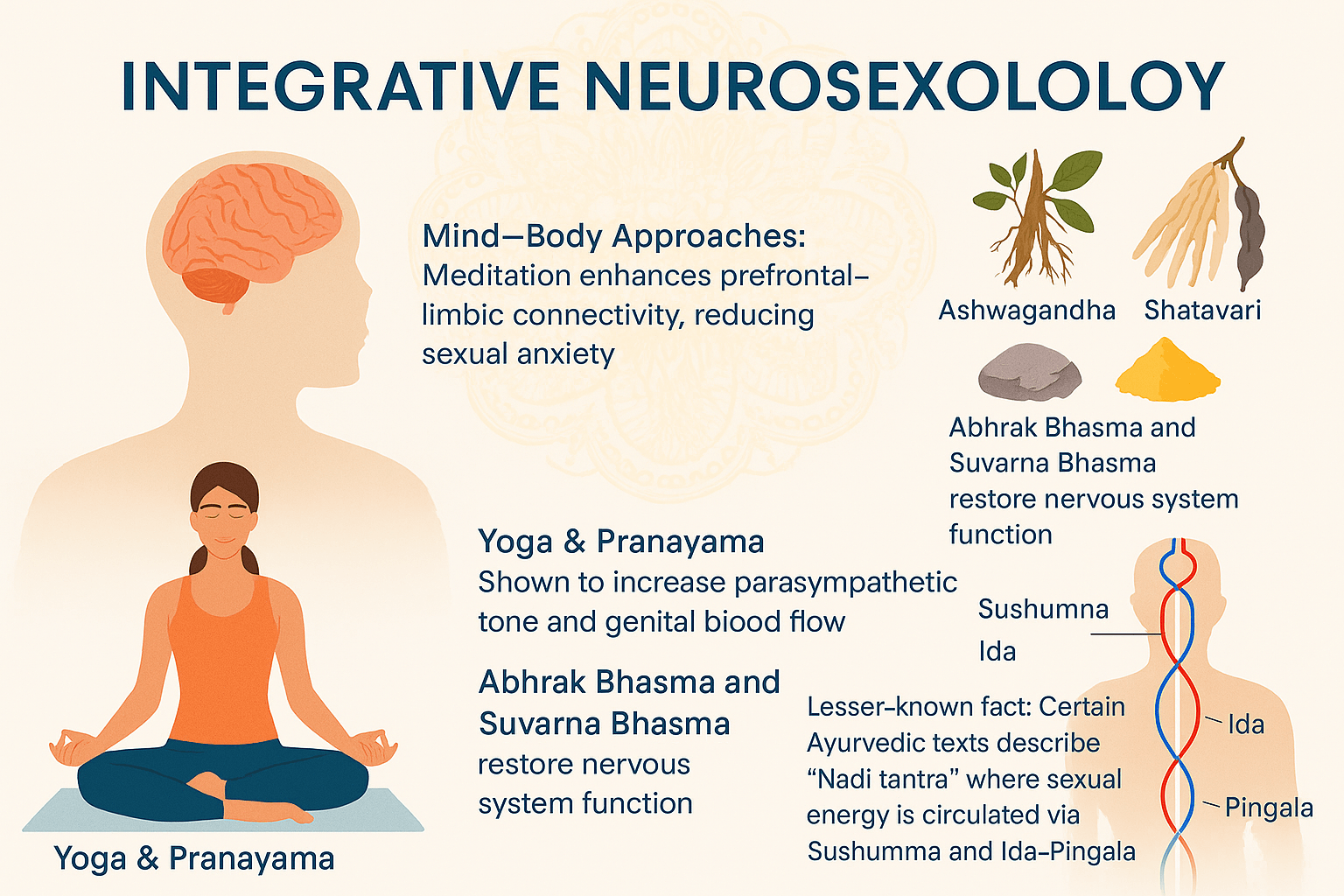
Mind–Body Approaches
Modern research shows that meditation not only calms the mind but also reshapes the brain’s sexual circuitry. Neuroimaging reveals enhanced connectivity between the prefrontal cortex and limbic system, which reduces sexual anxiety and allows arousal to flow without excessive inhibition. This “quieting” of hyperactive fear circuits, particularly the amygdala, makes sexual intimacy more fluid and natural. Ayurveda resonates with this concept, emphasizing Satvavajaya Chikitsa (mental discipline) through dhyana (meditation) and mantra therapy to stabilize Rajas and Tamas while promoting Sattva (clarity). When mind and brain are harmonized, sexual vitality becomes an expression of calm strength rather than restless pursuit. This integration underscores that sexual health is not only about hormones or nerves but also about the mental lens through which intimacy is experienced, confirming that inner balance is as critical as outer function [1].
Yoga & Pranayama
Yoga and controlled breathing (Pranayama) exert profound neurosexual benefits. Studies show that yogic practices increase parasympathetic tone, enhancing relaxation and genital blood flow, essential for both erection and vaginal lubrication. Specific postures like Bhujangasana (cobra pose) and Baddha Konasana (butterfly pose) activate pelvic circulation, while alternate-nostril breathing balances autonomic nervous system activity. Ayurveda describes these effects as pacifying aggravated Vata, grounding sexual energy, and directing Prana to the pelvic centers. Regular practice improves not only sexual performance but also emotional bonding by reducing cortisol and anxiety. Unlike pharmacological aids that provide short-term results, yoga and pranayama cultivate long-lasting resilience in the nervous system. They exemplify how physical movement, breath, and awareness synchronize to create neuroendocrine harmony, reinforcing the principle that intimacy flourishes when body and mind move in rhythm rather than conflict [2].
Ayurveda Mapping
Ayurveda offers a precise mapping of herbs and mineral formulations to neurosexual health. Vajikarana Rasayanas—such as Ashwagandha, Shatavari, and Kapikacchu—regulate dopaminergic and androgenic activity, sustaining both desire and fertility. Modern studies confirm their roles in improving testosterone, sperm quality, and neurochemical balance. Mineral preparations like Abhrak Bhasma (mica ash) and Suvarna Bhasma (gold ash) are revered for restoring Majja Dhatu (nervous tissue) and enhancing Ojas, the essence of immunity and vitality. In Ayurvedic texts, they are recommended not just as aphrodisiacs but as nervous system rejuvenators, paralleling modern neuroprotective agents. The principle of Vajikarana is that sexual strength is inseparable from nervous resilience; thus, herbs and bhasmas are not isolated “boosters” but systemic tonics. This dual framework merges with neurosexology’s vision of treating dysfunction through brain–body restoration rather than symptom suppression [3].
Lesser-Known Fact: Nadi Tantra
A remarkable concept preserved in certain tantric and Ayurvedic texts is Nadi Tantra, which describes how sexual energy flows through subtle channels (nadis) such as Sushumna, Ida, and Pingala. During intimacy or meditative states, energy rises through these pathways, harmonizing the sympathetic and parasympathetic systems. This idea aligns strikingly with modern neuroendocrinology, where balanced vagal tone and hypothalamic-pituitary regulation ensure healthy arousal and orgasm. Ancient texts even describe techniques for “recycling” sexual energy upward into spiritual vitality, a concept mirrored in today’s exploration of oxytocin-mediated bonding and dopamine-driven reward circuits. Ayurveda framed this as transforming Shukra (reproductive essence) into Ojas (vital essence), ensuring longevity and creativity. This convergence highlights that what neurosexology now explores with scans and neurotransmitters was intuited in Ayurveda centuries ago through metaphors of energy and consciousness—a true meeting point of science and tradition [4].
Frequently Asked Questions (FAQ) on Integrative Neurosexology
Q1. What is Integrative Neurosexology?
Integrative Neurosexology combines modern neuroscience, psychology, and pharmacology with Ayurvedic wisdom and mind–body practices to understand and heal sexual health disorders. It acknowledges both brain chemistry and subtle energy pathways like Nadis and Dhatus.
Q2. How does meditation help with sexual problems?
Meditation reduces overactivity in the fear centers of the brain (amygdala) while strengthening connectivity between the prefrontal cortex and limbic system. This leads to less sexual anxiety, smoother arousal, and deeper intimacy.
Q3. Can yoga really improve sexual function?
Yes. Yoga and Pranayama enhance parasympathetic activity, which promotes relaxation, improves genital blood flow, and balances hormones. Certain poses, like Bhujangasana and Baddha Konasana, directly support pelvic circulation.
Q4. Which Ayurvedic herbs support sexual health?
Ashwagandha improves testosterone and vitality, Shatavari nourishes female reproductive health, and Kapikacchu enhances dopamine activity. Mineral preparations like Abhrak Bhasma and Suvarna Bhasma restore nervous function and rejuvenate Shukra Dhatu.
Q5. What is Vajikarana Rasayana in Ayurveda?
Vajikarana Rasayana is the branch of Ayurveda devoted to sexual rejuvenation. It strengthens reproductive tissues, enhances fertility, and restores nervous balance through herbal and mineral formulations.
Q6. How does Ayurveda view sexual dysfunction?
Ayurveda attributes dysfunction to imbalances in Vata, Pitta, and Kapha, depletion of Shukra Dhatu, or disturbances in Manovaha Srotas (mental pathways). It treats the root cause with Rasayana therapy, Panchakarma, and mind–body healing.
Q7. What is Nadi Tantra and how does it relate to modern science?
Nadi Tantra describes how sexual energy flows through Sushumna, Ida, and Pingala channels, linking body and consciousness. This aligns with modern neuroendocrine theories of vagal tone, autonomic balance, and hypothalamic regulation.
Q8. Can integrative approaches replace medications like Viagra?
They can complement or, in some cases, reduce dependency on pharmaceuticals. Practices like yoga, meditation, and Vajikarana herbs address the root causes rather than just symptom relief, leading to longer-term results.
Q9. Is cannabis really helpful for sexual performance?
Cannabis may temporarily heighten sensitivity by boosting dopamine and oxytocin, but long-term use lowers testosterone and reduces fertility. Ayurveda warns against chronic use, as it depletes Shukra Dhatu and Ojas.
Q10. Who benefits most from Integrative Neurosexology?
Individuals with stress-related sexual dysfunction, low desire, premature ejaculation, orgasmic disorders, or couples seeking deeper intimacy benefit most. It is also useful in neurogenic and hormonal imbalances where conventional medicine has limits.
Reference
[1] Arnow, B. A., Millheiser, L., Garrett, A., Lake Polan, M., Glover, G. H., Hill, K. R., Lightbody, A., Watson, C., & Greicius, M. D. (2009). Women with hypoactive sexual desire disorder compared to normal females: A functional magnetic resonance imaging study. Neuroscience, 158(2), 484–502. https://doi.org/10.1016/j.neuroscience.2008.09.044
[2] Hu, S. H., Wei, N., Wang, Q. D., Yan, L. Q., Wei, E. Q., Zhang, M. M., & Hu, J. B. (2008). Regional brain activation during sexual arousal in healthy males: An fMRI study. Asian Journal of Andrology, 10(5), 769–775. https://doi.org/10.1111/j.1745-7262.2008.00424.x
[3] Stoléru, S., Fonteille, V., Cornélis, C., Joyal, C., & Moulier, V. (2012). Functional neuroimaging studies of sexual arousal and orgasm in healthy men and women: A review and meta-analysis. Neuroscience & Biobehavioral Reviews, 36(6), 1481–1509. https://doi.org/10.1016/j.neubiorev.2012.03.006
[4] Bancroft, J. (2005). The endocrinology of sexual arousal. Journal of Endocrinology, 186(3), 411–427. https://doi.org/10.1677/joe.1.06233
[5] Meston, C. M., & Frohlich, P. F. (2000). The neurobiology of sexual function. Archives of General Psychiatry, 57(11), 1012–1030. https://doi.org/10.1001/archpsyc.57.11.1012
[6] Bianchi-Demicheli, F., & Ortigue, S. (2007). Toward an understanding of the cerebral substrates of woman’s orgasm. Neuropsychologia, 45(12), 2645–2659. https://doi.org/10.1016/j.neuropsychologia.2007.04.015
[7] Safarinejad, M. R. (2011). Safety and efficacy of bupropion in selective serotonin reuptake inhibitor-induced sexual dysfunction: A double-blind, placebo-controlled, fixed-dose, randomized study. Journal of Clinical Psychopharmacology, 31(1), 66–74. https://doi.org/10.1097/JCP.0b013e318204c20a
[8] Wise, T. N., & Ryley, P. (2019). Sexual dysfunction and chronic pelvic pain: Neurobiological and psychosocial mechanisms. Current Pain and Headache Reports, 23(4), 25. https://doi.org/10.1007/s11916-019-0767-8
[9] Domar, A. D., & Dreher, H. (1996). Healing Mind, Healthy Woman: Using the Mind-Body Connection to Manage Stress and Take Control of Your Life. Addison-Wesley.
[10] Dhikav, V., Singh, P., Anand, K. S., & Gupta, R. (2018). Meditation and neuroplasticity in health and disease: A review of recent studies. Annals of Indian Academy of Neurology, 21(3), 187–192. https://doi.org/10.4103/aian.AIAN_36_18
[11] Chaudhary, R., & Dhankhar, J. (2020). Role of Yoga and Meditation in the management of sexual dysfunction: A comprehensive review. Journal of Clinical and Diagnostic Research, 14(9), LE01–LE06. https://doi.org/10.7860/JCDR/2020/45201.14054
[12] Khalsa, S. B. S., & Cope, S. (2006). Effects of a yoga lifestyle intervention on performance-related characteristics of musicians: A preliminary study. Medical Science Monitor, 12(8), CR325–CR331. https://pubmed.ncbi.nlm.nih.gov/16865064/
[13] Tiwari, S. (2017). Ashwagandha (Withania somnifera) and sexual health: Evidence-based review. International Journal of Research in Ayurveda and Pharmacy, 8(3), 1–6. https://doi.org/10.7897/2277-4343.083182
[14] Vyas, M., & Dikshit, N. (2021). Vajikarana Rasayana in Ayurveda: A review of classical references and modern validation. Ayu, 42(2), 89–96. https://doi.org/10.4103/ayu.ayu_85_20
[15] Mishra, L. C., Singh, B. B., & Dagenais, S. (2001). Healthcare and disease management in Ayurveda. Alternative Therapies in Health and Medicine, 7(2), 44–50. https://pubmed.ncbi.nlm.nih.gov/11253415/
[16] Patwardhan, B., Mutalik, G., & Tillu, G. (2015). Integrative approaches for health: Biomedical research, Ayurveda and Yoga. London: Academic Press. https://doi.org/10.1016/C2013-0-13094-4
[17] Singh, R. H. (2005). Exploring issues in the development of Ayurvedic research methodology. Journal of Ayurveda and Integrative Medicine, 1(1), 5–12. https://www.jaim.in/article.asp?issn=0975-9476;year=2010;volume=1;issue=1;spage=5;epage=12
[18] Shastri, A. D. (Ed.). (2012). Charaka Samhita of Agnivesha with Ayurveda Dipika Commentary of Chakrapanidatta. Varanasi: Chaukhamba Sanskrit Sansthan. (Chikitsa Sthana, Vajikarana Adhyaya).
[19] Sharma, P. V. (2013). Sushruta Samhita: With English translation of text and Dalhana’s commentary. Varanasi: Chaukhamba Visvabharati. (Chikitsa Sthana, 27th Chapter – Yonivyapad & Vajikarana).