- When Treatment Ends but the Disease Continues
- High-Authority Global Medical Perspective on Recurrence
- The Post-Treatment Gap Most Patients Experience
- The Hidden Phase Before Recurrence Begins
- What Happens Months Before Glioma Recurrence Is Detected
- Why Current Monitoring Often Detects Recurrence Late
- Early Functional Changes Before Recurrence
- Objective Early Warning Indicators Beyond Symptoms
- Why Gliomas Are Difficult to Cure Completely
- The Role of Cancer Stem Cells in Recurrence
- Tumor Microenvironment and Regrowth
- Why Modern Treatment Cannot Fully Prevent Recurrence
- What Changes in the Body After Treatment
- Typical Timeline of Glioma Recurrence
- Risk Factors for Faster or Aggressive Recurrence
- Why Recurrence Often Happens in the Same Location
- Symptoms Patients Often Ignore After Treatment
- Why Recurrence Feels Sudden but Is Not
- Why Patients Seek Alternative Treatment After Recurrence
- Global Healthcare Gaps in Recurrence Management
- Shift in Strategy: From Tumor Removal to Long-Term Control
- When to Consider an Integrative Approach
- Safety and Integration with Modern Oncology
- Ayurvedic Perspective on Glioma Recurrence
- Pre-Recurrence Changes (Ayurvedic View)
- Ayurvedic Management Approach
- Key Herbs and Classical Formulations
- Modern Scientific Research Supporting Integrative Approach
- Practical Guidance for Patients and Families
- Clinical Insight (Real-World Pattern)
- Prognosis and Long-Term Management
- FAQs
- Reference
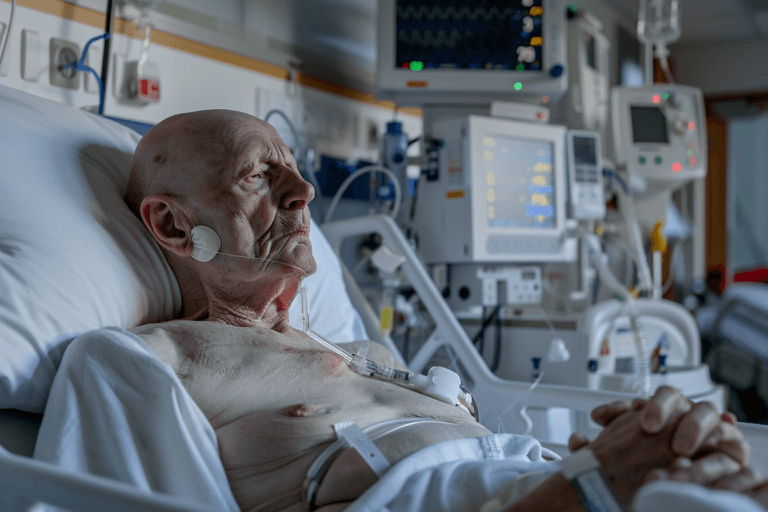
When Treatment Ends but the Disease Continues
When treatment ends, you and your family feel relief. Surgery is done. Radiation is finished. Chemotherapy is over. It feels like the disease is gone.
But with glioma recurrence, this is usually not true.
Glioma cells spread into the brain in a way that cannot be fully removed. Even after surgery, some tumor cells always remain. These cells are invisible on scans but continue to grow slowly inside the brain [2].
Radiation and chemotherapy are given to control these cells. They can slow the disease, but they also affect the patient’s health.
Radiation to the brain can cause long-term damage to normal brain tissue. Many patients develop memory loss, confusion, slow thinking, and personality changes over time. Chemotherapy can weaken immunity, reduce blood counts, cause fatigue, and make the body weaker overall. So even after treatment, the patient is often not as strong as before [1].
Now comes the reality that most families are not clearly told.
In aggressive brain tumors like glioblastoma, glioma recurrence happens in almost all patients. Even with the best treatment, average survival is about 12 to 15 months from diagnosis. After the tumor comes back, survival is often only 2 to 9 months in many cases [1], [3].
This means that a large number of patients die within 1 to 2 years, even after going through full treatment.
For caregivers, this is the most difficult phase.
At first, the patient may look stable. But slowly, changes begin.
Research on end-stage glioma patients shows very clear patterns:
- Drowsiness in about 85 to 87% of patients
- Difficulty swallowing (dysphagia) in about 70%
- Seizures in around 40 to 45%
- Severe cognitive decline in about 30 to 35%
- Headaches in about 30% [9]
This is what you may actually see at home.
The patient may forget simple things. They may not recognize family members. Speech becomes unclear. Thinking becomes very slow.
As glioma recurrence progresses, seizures can happen again and again. Headaches may increase. Vomiting can occur due to rising pressure in the brain. The patient may become physically weak and unable to walk.
In later stages, many patients cannot swallow properly. Because of this, some patients are given food through a tube. Studies show that around 10 to 15% of patients may require tube feeding in advanced stages [9].
The patient may then become very sleepy and spend most of the time in bed. Gradually, they lose awareness of surroundings.
At this stage, the brain is no longer able to control basic functions properly. This is when the disease leads to death.
For you as a caregiver, it may feel sudden. But medically, it is not sudden. Glioma recurrence usually begins months before it is seen on MRI scans. By the time symptoms become clear, the disease is already advanced [9].
This is why understanding this phase is very important.
Glioma is not a disease that ends after treatment. It continues silently. Knowing the real course of the disease helps you prepare, recognize early warning signs, and support the patient in a more informed and realistic way.
When you look at glioma recurrence from a global medical perspective, there is strong agreement across leading health organizations. The reality is clear. Even with advanced treatment, recurrence is common, especially in high-grade tumors like glioblastoma.
Table 1: Glioma Recurrence Timeline
| Phase After Treatment | What Happens Inside the Brain | What Patients/Family Notice | Insight |
|---|---|---|---|
| 0–3 Months | Residual microscopic tumor cells remain active | Patient feels stable or slightly weak | Recurrence already begins silently |
| 3–6 Months | Cellular regrowth and microenvironment changes | Mild fatigue, slight confusion | Early warning signs often ignored |
| 6–12 Months | Tumor becomes biologically active | Headaches, memory issues, mood changes | Most common recurrence window |
| 12–18 Months | Structural tumor growth detectable | Seizures, weakness, speech issues | MRI starts detecting recurrence |
| 18+ Months | Progressive neurological decline | Loss of independence, severe symptoms | Advanced stage progression |
Guidelines from the American Society of Clinical Oncology explain that current treatments such as surgery, radiation, and chemotherapy help control the tumor but do not completely eliminate it. Because of this, recurrence is expected in many patients, and long-term cure remains difficult [6].
The National Institute for Health and Care Excellence also emphasizes that care does not end after treatment. Patients require continuous monitoring because tumors can return silently. NICE further highlights that treatment options become more limited once recurrence occurs [7].
The World Health Organization classifies gliomas as aggressive and infiltrative tumors. This means they spread into normal brain tissue in a way that cannot be fully removed, which directly explains why glioma recurrence is so common [8].
Clinical frameworks such as those from the National Comprehensive Cancer Network (NCCN) further reinforce that recurrence is one of the biggest challenges in brain tumor management and that structured follow-up is essential [5].
From another important angle, the NCCIH recognizes that many patients seek supportive and integrative care during and after cancer treatment. This is especially relevant when the disease returns or when patients experience side effects from therapy. NCCIH supports evidence-based complementary approaches to improve quality of life alongside standard treatment [16].
If you are a patient or caregiver, the key takeaway is simple. Across the world, medical experts agree on one point: glioma recurrence is not rare. It is expected.
This is why long-term monitoring, early recognition of changes, and a broader, supportive care approach are essential after initial treatment ends.
The Post-Treatment Gap Most Patients Experience
After surgery, radiation, and chemotherapy are completed, you are usually told to enter a “follow-up” or “monitoring” phase. This often means periodic MRI scans every few months and short consultations. From a medical system point of view, this is standard care. But from a patient and caregiver point of view, this phase can feel confusing and uncertain.
Guidelines such as those from the National Comprehensive Cancer Network (NCCN) emphasize regular imaging and clinical follow-up after treatment [5]. Similarly, recommendations from the National Institute for Health and Care Excellence (NICE) highlight ongoing monitoring as an essential part of brain tumor care [7]. However, what these guidelines also indirectly show is that active treatment often pauses during this period, unless clear progression is detected.
This creates what many families experience as a “gap.”
You are no longer in active treatment, but the disease has not truly ended. There is often no clear strategy given to prevent glioma recurrence, only instructions to “wait and watch.” For caregivers, this can be one of the most stressful phases. You may constantly wonder if the disease is returning, but you are told everything is fine as long as scans look stable.
Another important limitation is how monitoring works. MRI scans are designed to detect structural changes in the brain, not early biological activity. According to clinical evidence, tumor cells can begin growing again long before they become visible on imaging [9]. This means that by the time recurrence is confirmed, the disease may already be progressing for months.
During this phase, many patients also continue to deal with the after-effects of treatment. Fatigue, cognitive slowing, emotional changes, and physical weakness can persist. Yet these symptoms are often attributed to “recovery” rather than being carefully monitored as possible early warning signs.
So from your perspective as a caregiver, this phase can feel like:
- The treatment has stopped, but the disease risk is still there
- There is monitoring, but no early detection of microscopic changes
- There are symptoms, but no clear explanation
- There is fear, but limited guidance
This is why the post-treatment phase is not just a recovery period. It is a critical window where glioma recurrence may already be developing silently.
Understanding this gap helps you stay more alert. It allows you to observe subtle changes, ask the right questions, and recognize that stability on a scan does not always mean the disease is inactive.
Microscopic Tumor Cells Remain After Treatment
After treatment ends, it may feel like the tumor is gone. But in reality, glioma recurrence often begins silently at a microscopic level. Surgery removes what can be seen, but glioma cells spread into surrounding brain tissue in a diffuse manner. Because of this, tiny clusters of tumor cells almost always remain, even after the most advanced surgical removal [2].
These cells are too small to be detected on MRI scans. So while reports may show “no visible tumor,” the disease has not truly disappeared.
Dormant Cells Survive and Reactivate Later
These remaining tumor cells do not always grow immediately. Many of them enter a temporary inactive state known as dormancy. During this phase, the patient may appear stable, and scans may look normal.
However, research shows that these cells can survive radiation and chemotherapy, then later reactivate and begin growing again [9]. This is one of the key reasons why glioma recurrence happens even after aggressive treatment.
Tumor Stem Cells Drive Recurrence
A major factor behind recurrence is the presence of tumor stem-like cells. These cells are highly resistant to treatment and have the ability to regenerate the tumor.
Even if most tumor cells are destroyed, a small number of these stem-like cells can survive and slowly rebuild the tumor over time [10]. This makes glioma fundamentally different from many other cancers.
Why This Phase Is Dangerous
This hidden phase is difficult to detect but clinically very important. During this time:
- The tumor is already starting to return
- There are no strong symptoms yet
- MRI scans may still appear normal
- No active treatment is usually given
From your perspective as a caregiver, this phase may look like recovery. But medically, it is often the stage where glioma recurrence is silently developing.
What This Means for Patients and Caregivers
The most important point to understand is simple. Glioma recurrence does not begin when it appears on a scan. It begins much earlier, at a microscopic level.
Recognizing this changes how you look at the disease. Instead of assuming the tumor is gone, you become more aware that ongoing vigilance is necessary, even when everything seems stable.
What Happens Months Before Glioma Recurrence Is Detected

Tumor Cells Begin Regrowing at a Microscopic Level
Months before glioma recurrence is visible on a scan, the process has already started inside the brain. After treatment, small clusters of tumor cells remain hidden within normal brain tissue. These cells slowly begin to divide and expand, but at a scale too small to be detected on MRI. During this time, the patient may feel stable and reports may appear normal, yet biologically the tumor is already regrowing and preparing for visible recurrence [2].
Tumor Stem Cells Rebuild the Tumor Structure
A key reason this regrowth happens is the presence of tumor stem-like cells. These cells are more resistant to chemotherapy and radiation compared to regular tumor cells. Even when most tumor cells are destroyed, these stem-like cells can survive and gradually multiply. Over time, they begin to rebuild the tumor structure from within, acting as the core source of recurrence. This explains why the disease often returns despite aggressive treatment [10].
Formation of Tumor Niches in the Brain
As these surviving cells grow, they do not expand randomly. They settle into protective environments within the brain known as tumor niches. These niches provide a supportive space with nutrients, oxygen, and protection from the immune system. Within these microenvironments, tumor cells can grow quietly and resist further treatment. This allows early tumor expansion to continue without being easily detected [11].
Early Biological Activity Before Detection
During this hidden phase, the brain is already undergoing subtle but important changes. Tumor cells increase their activity and begin forming new blood supply to support growth. There are also early metabolic changes in the surrounding brain tissue, along with mild disruption of normal brain function. However, these changes are not yet visible on routine imaging, because MRI scans detect structural abnormalities rather than early biological activity.
Why Detection Comes Too Late
By the time glioma recurrence is finally detected on imaging, the tumor has often been growing for weeks or even months. At this point, it is no longer microscopic, and symptoms may start appearing. Treatment options may also become more limited compared to earlier stages. This delay between silent regrowth and visible detection is one of the biggest challenges in managing glioma.
What This Means for Patients and Caregivers
For patients and caregivers, the most important point to understand is that recurrence does not begin suddenly. It develops quietly over time, long before it appears on a scan. What looks like a stable phase is often a period where the disease is slowly returning. Recognizing this reality helps you stay more aware and better prepared during the months after treatment, even when everything seems under control.
Why Current Monitoring Often Detects Recurrence Late
MRI Is Designed for Structure, Not Early Biology
After treatment ends, most patients enter a monitoring phase that relies primarily on MRI scans. MRI is an excellent tool for visualizing structural changes in the brain, such as tumor size, swelling, or shifts in surrounding tissue. However, the fundamental limitation is that MRI does not detect early biological activity.
In the months following treatment, tumor cells may already be active at a microscopic level. These cells can begin dividing, altering local metabolism, and interacting with surrounding brain tissue. Yet none of these early processes are visible on standard MRI. By the time MRI shows a clear abnormality, the disease has often progressed beyond its earliest stage [9].
This creates a critical delay. From a clinical perspective, the tumor appears stable. But from a biological perspective, recurrence may already be underway.
The Challenge of Distinguishing Recurrence from Treatment Effects
One of the most complex issues in post-treatment monitoring is differentiating true tumor regrowth from treatment-related changes. Radiation and chemotherapy do not only target tumor cells. They also affect healthy brain tissue, leading to inflammation, edema, and sometimes necrosis.
These changes can appear very similar to tumor recurrence on MRI scans. This phenomenon, known as pseudoprogression, can occur within weeks to months after treatment. In some cases, scans may suggest tumor growth when the changes are actually temporary treatment effects. In other situations, real recurrence may be masked by these overlapping patterns.
This diagnostic uncertainty can delay appropriate clinical decisions. Doctors may adopt a “wait and watch” approach to see how the imaging evolves over time, which can further postpone intervention [14].
Biological Progression Continues Between Scans
Another important limitation is the interval between follow-up scans. Most patients undergo imaging every two to three months. During this period, significant biological changes can occur.
Tumor cells can multiply, establish new microenvironments, and recruit blood supply through angiogenesis. They may also adapt to the post-treatment environment, becoming more resistant and aggressive. These processes are continuous and dynamic, yet they remain invisible until they produce measurable structural changes.
This means that recurrence is not a sudden event. It is a gradual process that develops silently between monitoring intervals. By the time the next scan is performed, the disease may already be clinically significant.
Advanced Imaging Techniques Provide Partial Solutions
To overcome the limitations of conventional MRI, advanced imaging techniques such as PET scans, MR spectroscopy, and perfusion imaging have been introduced. These methods aim to detect metabolic activity, blood flow changes, and biochemical alterations within the brain.
For example, PET imaging can identify areas of increased glucose metabolism, which may indicate active tumor growth. MR spectroscopy can detect changes in chemical markers associated with tumor cells. Perfusion imaging can reveal abnormal blood vessel formation.
While these technologies provide deeper insights, they are not routinely used in all clinical settings. Their availability may be limited, and interpretation requires specialized expertise. Even with these tools, detecting very early microscopic disease remains a challenge [15].
Why Monitoring Often Feels Reassuring but Is Not Definitive
From a patient or caregiver perspective, regular scans can create a sense of reassurance. When reports say “no progression” or “stable disease,” it is natural to assume that the condition is under control.
However, it is important to understand that stability on imaging does not always mean biological inactivity. The disease may still be evolving at a level that current tools cannot detect.
This gap between what is visible and what is actually happening inside the brain is one of the key reasons why recurrence is often diagnosed at a later stage.
What This Means for Patients and Caregivers
Understanding these limitations changes how you interpret follow-up care. Monitoring is essential, but it is not a guarantee of early detection. It is a system designed to identify visible progression, not the earliest signs of disease activity.
For caregivers, this means staying attentive to subtle changes in the patient’s condition, even when scans appear normal. For patients, it highlights the importance of ongoing vigilance and a broader understanding of how the disease behaves after treatment.
In simple terms, current monitoring methods are powerful but incomplete. They show what has already happened, not always what is beginning to happen.
Early Functional Changes Before Recurrence

Subtle Changes Begin Before Any Scan Shows Abnormality
Long before any visible change appears on a scan, the brain often begins to show early functional disturbances. These changes are not dramatic at first. They are subtle, gradual, and easy to overlook. In many cases, patients are told everything is stable based on imaging, yet their day-to-day functioning begins to shift.
This phase reflects early clinical progression where tumor activity is beginning to affect surrounding brain networks, even though structural changes are not yet detectable [9].
Mild Cognitive Decline Is Often the First Signal
One of the earliest signs is a change in cognitive function. Patients may begin to experience slight memory lapses, difficulty concentrating, or slower thinking. These changes are often dismissed as fatigue, stress, or recovery from treatment.
However, in many cases, these are early indicators that brain function is being affected at a microscopic level. The tumor may be interacting with critical neural pathways responsible for memory, attention, and processing speed [13].
Behavioral and Personality Changes May Appear
Caregivers are often the first to notice subtle behavioral changes. A patient who was previously calm may become irritable. Someone who was emotionally stable may show mood swings or withdrawal.
These changes can be confusing and are often attributed to psychological stress or medication effects. But clinically, they may reflect early disruption of frontal or temporal brain regions involved in emotional regulation and behavior.
Speech, Coordination, and Daily Function Begin to Shift
In some patients, early functional decline may involve slight difficulty in speech, such as finding the right words or forming sentences. Others may notice minor coordination issues, like unsteadiness while walking or reduced precision in hand movements.
These symptoms are usually mild in the beginning and may come and go. Because they are not severe, they are often ignored. However, they can represent early neurological involvement as the disease begins to progress.
Fatigue and Neurological Slowing Increase Gradually
Another common early change is a persistent sense of fatigue that does not improve with rest. Patients may feel mentally and physically slower, taking more time to complete simple tasks.
This is not just general tiredness. It often reflects changes in brain metabolism and neural efficiency as the tumor begins to influence surrounding tissue.
Why These Changes Are Often Missed
The biggest challenge is that these symptoms are nonspecific. They can easily be explained as side effects of radiation, chemotherapy, or medications. Because scans may still appear normal, both patients and doctors may not immediately connect these changes to disease progression.
This creates a situation where early warning signs are present, but not recognized as part of the recurrence process.
How You Should Interpret These Early Changes
For caregivers, these subtle changes are important. You may notice differences before any test confirms a problem. Paying attention to small shifts in memory, behavior, speech, or coordination can provide early clues that something is changing.
For patients, it is important to understand that not all symptoms are simply part of recovery. Some may reflect early functional changes in the brain.
In simple terms, the body often shows signs before the scan does. Recognizing these early changes can help you stay more alert during the post-treatment phase, even when reports appear stable.
Objective Early Warning Indicators Beyond Symptoms
Why Symptoms Alone Are Not Enough
Relying only on symptoms can delay recognition of disease progression. Many early changes in the brain occur before noticeable symptoms appear. In some cases, patients may feel stable while biological activity is already increasing. This creates a gap where the disease is progressing silently but remains clinically undetected.
This is why objective indicators, especially those based on imaging and functional assessment, play an important role in identifying early changes that symptoms alone cannot reveal [14].
Functional Changes Can Be Measured Before Structural Changes
The brain begins to show functional disturbances before visible structural damage appears. These include alterations in metabolism, blood flow, and neural activity. While standard MRI focuses on structure, it does not capture these early functional shifts.
Advanced techniques such as functional MRI, perfusion imaging, and metabolic imaging can detect these changes earlier. They provide insight into how the brain is working, not just how it looks. This difference is critical because early tumor activity often affects function before it alters anatomy [15].
Metabolic Imaging Reveals Hidden Tumor Activity
Techniques like PET scans are designed to detect metabolic activity within tissues. Tumor cells often have higher metabolic rates compared to normal cells. This allows PET imaging to identify areas of increased activity that may indicate early tumor regrowth.
In some cases, metabolic changes can be detected before structural abnormalities appear on MRI. This makes PET a valuable tool in specific clinical situations, although it is not routinely used for all patients due to limitations in access and cost [15].
Perfusion and Blood Flow Changes Signal Early Progression
As tumor cells begin to grow, they require an increased blood supply. This leads to early changes in blood flow within the affected brain regions. Perfusion imaging can detect these changes by measuring how blood moves through brain tissue.
Increased perfusion may indicate active tumor growth even when structural imaging appears stable. These early vascular changes are often among the first objective signs of progression [14].
Challenges in Using Advanced Indicators
Although these advanced methods provide valuable insights, they are not widely used in routine follow-up for every patient. Their interpretation requires expertise, and results may vary depending on the technique and clinical context.
Additionally, very early microscopic disease may still remain beyond the detection limits of even the most advanced imaging tools. This means that while these indicators improve early detection, they do not completely eliminate the gap.
How to Understand These Indicators in Real Life
From a practical perspective, objective indicators help bridge the gap between what you feel and what imaging shows. They provide additional layers of information that can support earlier recognition of changes.
Understanding that functional and metabolic changes can occur before visible tumor growth helps you see why relying only on symptoms or routine scans may not always give the full picture.
Why Gliomas Are Difficult to Cure Completely
Diffuse Infiltration Into Surrounding Brain Tissue
Gliomas do not stay confined to one location. They spread into nearby brain tissue in a scattered and microscopic pattern. Even when scans show a defined tumor, individual cancer cells have already moved beyond that visible area.
Table : Why Glioma Recurs (Root Cause Breakdown)
| Factor | What Happens | Why Treatment Fails | Value |
|---|---|---|---|
| Infiltrative Nature | Tumor spreads into surrounding brain | Cannot be fully removed | Core reason for recurrence |
| Microscopic Residual Cells | Cells remain after surgery | Undetectable in scans | Hidden disease progression |
| Treatment Resistance | Cells adapt to chemo/radiation | Becomes harder to treat | Explains relapse |
| Tumor Microenvironment | Supports regrowth | Promotes survival of cells | Key biological driver |
| Cancer Stem Cells | Self-renewing tumor cells | Cause regrowth | Major research focus |
During surgery, only the main tumor mass can be removed. The scattered cells that mix with normal brain tissue cannot be safely taken out without damaging essential functions like speech or movement. Because of this, some tumor cells almost always remain after surgery, which later leads to regrowth [2].
Limitations Imposed by Brain Function
The brain controls every vital function of the body. Areas responsible for memory, speech, coordination, and behavior are often located very close to the tumor. This creates a major limitation during treatment.
Surgeons cannot remove large margins of surrounding tissue like they might in other cancers. Radiation must also be carefully controlled to avoid permanent brain injury. This balance between treating the tumor and protecting brain function makes complete removal extremely difficult [4].
Resistance to Standard Therapies
Glioma cells are not equally sensitive to treatment. Some respond well to radiation and chemotherapy, while others survive. These surviving cells can repair damage, adapt, and continue growing.
Over time, the remaining cells may become stronger and more resistant. This is why treatment may reduce the tumor significantly, but does not eliminate it completely. The disease often returns from these resistant cells [13].
Tumor Stem-Like Cells Sustain Regrowth
Within gliomas, there is a small group of cells known as tumor stem-like cells. These cells behave differently from regular tumor cells. They can remain inactive for some time and later restart tumor growth.
They are also more resistant to treatment, which allows them to survive even after aggressive therapy. Once conditions become favorable, they begin rebuilding the tumor, making long-term cure very challenging [13].
Ongoing Biological Adaptation
Gliomas continue to change over time. When treatment kills sensitive cells, resistant cells survive and multiply. This leads to a more aggressive tumor during recurrence.
Each cycle of treatment and regrowth can make the disease harder to control. The tumor adapts to survive in the treated environment, which reduces the effectiveness of future therapies.
Clinical Reality Patients Should Be Aware Of
The difficulty in curing gliomas is not due to lack of treatment options alone. It is mainly due to how the tumor behaves inside the brain. It spreads invisibly, survives therapy, and changes over time.
Because of this, treatment often focuses on controlling the disease rather than completely removing it. This is why recurrence is common, even after intensive treatment.
The Role of Cancer Stem Cells in Recurrence
A Small Population With a Powerful Impact
Within gliomas, there exists a small but highly influential group of cells known as cancer stem cells. These cells make up only a fraction of the tumor, yet they play a central role in why the disease returns after treatment.
Unlike regular tumor cells, these cells have the ability to self-renew and generate new tumor cells repeatedly. Even if most of the tumor is destroyed, this small population can survive and later rebuild the entire tumor structure [10].
Why These Cells Survive Treatment
Cancer stem cells are naturally more resistant to both chemotherapy and radiation. While standard treatments are effective at killing rapidly dividing tumor cells, stem-like cells can remain in a slower, protected state.
They also have enhanced repair mechanisms, allowing them to recover from treatment-induced damage. This survival advantage means that even after aggressive therapy, these cells can persist inside the brain.
Dormancy and Delayed Regrowth
One of the most concerning features of these cells is their ability to remain dormant. During this phase, they do not actively grow or cause symptoms. This makes them difficult to detect using standard imaging or clinical evaluation.
After a period of dormancy, these cells can become active again. Once reactivated, they begin dividing and gradually rebuild the tumor, leading to recurrence.
Rebuilding the Tumor From Within
Cancer stem cells act as the “starting point” for tumor regrowth. They produce new generations of tumor cells, recreate the tumor microenvironment, and support the formation of blood supply needed for growth.
This process does not happen suddenly. It develops over time, often months before recurrence becomes visible on imaging. By the time the tumor is detected again, it has already been rebuilding internally.
Why Targeting These Cells Is Difficult
These cells are difficult to target because they behave differently from typical tumor cells. Many treatments are designed to attack rapidly dividing cells, but stem-like cells can remain inactive and avoid these therapies.
Additionally, they can adapt to changes in the environment and develop resistance over time. This makes them one of the main reasons why long-term cure remains challenging.
Clinical Insight for Patients and Caregivers
The presence of cancer stem cells explains why treatment may appear successful at first, yet the disease still returns later. Even when scans show no visible tumor, these cells may still be present at a microscopic level.
This highlights an important point. The disease does not always return from what was visible. It often returns from what remained hidden.
Tumor Microenvironment and Regrowth
The Brain Environment Supports Tumor Survival
After treatment, the remaining tumor cells do not exist in isolation. They interact with the surrounding brain environment, which plays a major role in helping them survive and grow again. This surrounding space, known as the tumor microenvironment, includes blood vessels, immune cells, supporting brain cells, and chemical signals.
Even when most of the tumor is removed, this environment can still support the survival of residual cells. It provides the conditions needed for these cells to remain active and eventually regrow [11].
Hypoxia Creates a Survival Advantage
One of the key features of this environment is hypoxia, which means low oxygen levels. After treatment, parts of the tumor area may have reduced blood supply, creating a hypoxic state.
Instead of dying, tumor cells can adapt to this low-oxygen environment. In fact, hypoxia can make them more aggressive. It activates survival pathways, increases resistance to therapy, and promotes further tumor growth. This gives the remaining cells a strong advantage in rebuilding the tumor [12].
Angiogenesis Supports New Tumor Growth
As tumor cells begin to grow again, they need a steady supply of oxygen and nutrients. To achieve this, they stimulate the formation of new blood vessels, a process known as angiogenesis.
This new vascular network allows the tumor to expand and sustain itself. Angiogenesis is not just a late event. It begins early in the regrowth phase, often before the tumor becomes visible on imaging. This is one of the reasons why recurrence can progress rapidly once it starts [11].
Immune System Evasion Allows Silent Progression
Under normal conditions, the immune system can recognize and destroy abnormal cells. However, glioma cells develop mechanisms to escape immune detection.
They can suppress immune responses, alter signaling pathways, and create a local environment that protects them from immune attack. This allows tumor cells to grow silently without being eliminated by the body’s natural defenses [12].
A Self-Sustaining Cycle of Regrowth
The combination of hypoxia, angiogenesis, and immune evasion creates a powerful system that supports tumor survival. These factors work together to form a self-sustaining cycle where tumor cells continue to grow, adapt, and resist treatment.
This is why recurrence is not just about leftover cells. It is also about the environment that supports those cells.
Clinical Perspective to Keep in Mind
Regrowth is not driven by tumor cells alone. The surrounding environment actively contributes to the process. Even a small number of remaining cells can expand if the conditions are favorable.
Recognizing this helps explain why recurrence can occur even after seemingly successful treatment, and why controlling the environment is as important as targeting the tumor itself.
Why Modern Treatment Cannot Fully Prevent Recurrence
Standard Treatments Control but Do Not Eliminate the Disease
Modern treatment for gliomas typically includes surgery, radiation therapy, and chemotherapy. These approaches are effective at reducing tumor burden and slowing disease progression. Clinical trials have shown that these treatments can improve survival and temporarily control tumor growth.
However, they are not designed to eliminate every tumor cell. Due to the infiltrative nature of gliomas, microscopic disease almost always remains after treatment. This residual disease becomes the source of recurrence over time [1].
Surgery Cannot Remove Invisible Tumor Cells
Surgical removal is one of the most important steps in treatment. But even the most advanced neurosurgical techniques can only remove what is visible and safely accessible.
Glioma cells spread beyond the visible tumor margins into normal brain tissue. Removing these cells would require removing healthy brain areas, which can lead to severe neurological damage. Because of this, surgery is inherently limited, and complete removal is not possible [2].
Radiation and Chemotherapy Have Biological Limits
Radiation and chemotherapy are used to target remaining tumor cells after surgery. While they can destroy a large number of cells, they do not affect all tumor populations equally.
Some cells survive due to resistance mechanisms. Others may be in a dormant state and less affected by treatment. Over time, these surviving cells can reactivate and begin growing again. This is a major reason why recurrence is seen even after aggressive therapy [9].
Guidelines Acknowledge Recurrence as a Major Challenge
Clinical guidelines from organizations such as the National Comprehensive Cancer Network (NCCN) clearly recognize recurrence as one of the biggest challenges in glioma management. These guidelines emphasize ongoing monitoring rather than prevention, reflecting the current limitations of treatment [5].
The focus is often on detecting recurrence early rather than completely preventing it, because current therapies do not fully address microscopic disease or long-term tumor survival mechanisms.
Treatment Pressure Leads to More Resistant Tumors
Another important factor is how tumors respond to treatment over time. When therapy is applied, sensitive tumor cells are destroyed, but resistant cells survive.
These resistant cells then multiply and form a new tumor that is often more aggressive and harder to treat. This process of selection and adaptation contributes to repeated recurrence and reduced effectiveness of future treatments.
Clinical Reality Patients Should Recognize
The limitation of modern treatment is not due to lack of effort or technology. It is mainly due to the biology of gliomas. These tumors spread invisibly, resist treatment, and adapt over time.
As a result, treatment is often focused on controlling the disease rather than completely curing it. This is why recurrence remains common, even after the best available therapies.
What Changes in the Body After Treatment
Residual Tumor Cells Remain Within Brain Tissue
After treatment is completed, it may appear that the tumor has been controlled or removed. However, at a microscopic level, tumor cells often remain within the surrounding brain tissue. These cells are not visible on imaging but continue to exist in a scattered and infiltrative pattern.
Because they are embedded within normal brain structures, they cannot be completely removed without causing damage. These remaining cells form the biological base from which regrowth can begin over time [2].
The Local Brain Environment Becomes Altered
Treatment does not only affect tumor cells. It also changes the surrounding brain environment. Radiation and chemotherapy can lead to inflammation, tissue injury, and altered cellular signaling in the treated area.
These changes create a different local environment compared to normal brain tissue. Instead of returning to a fully healthy state, the treated region may remain biologically altered, which can influence how remaining tumor cells behave [11].
Low Oxygen Conditions Promote Survival
One of the key changes after treatment is the development of low oxygen conditions, known as hypoxia. Damage to blood vessels and tissue structure can reduce oxygen supply in certain areas of the brain.
Tumor cells are able to adapt to these conditions. In fact, hypoxia can activate survival pathways that make tumor cells more aggressive and resistant. This environment supports their persistence and future growth [12].
Formation of New Blood Supply
As surviving tumor cells begin to recover, they stimulate the formation of new blood vessels to supply nutrients and oxygen. This process helps create a supportive network that allows the tumor to grow again.
This vascular development does not happen suddenly. It begins early at a microscopic level and supports gradual regrowth before it becomes visible on imaging [11].
Immune Response Becomes Suppressed Locally
The immune system plays a role in identifying and removing abnormal cells. However, after treatment, the local immune environment in the brain can become altered.
Tumor cells can take advantage of this by suppressing immune activity around them. This allows them to survive without being effectively targeted by the body’s natural defenses, enabling silent progression [12].
Overall Shift Toward a Pro-Growth Environment
When these factors are combined, the treated area of the brain becomes a space where tumor cells can survive and eventually grow again. Residual cells, altered tissue, reduced oxygen, new blood vessel formation, and immune suppression all contribute to a setting that favors recurrence.
This means that recurrence is not only about leftover tumor cells. It is also about how the body and brain environment change after treatment in a way that supports those cells.
Typical Timeline of Glioma Recurrence
Early Phase After Treatment Completion
In the first few months after surgery, radiation, and chemotherapy, most patients enter what appears to be a stable phase. MRI scans may show no visible tumor, and symptoms may temporarily improve. This period often creates a sense of relief.
However, at a microscopic level, residual tumor cells are still present. These cells may remain inactive or begin slow regrowth during this time. Clinical data shows that even after aggressive treatment, complete eradication is rare, and the disease often persists in a hidden form [1].
Silent Progression Phase (3 to 9 Months)
Between three to nine months after treatment, early biological regrowth may begin. Tumor cells start dividing, forming small clusters, and interacting with the surrounding brain environment.
During this phase, there are usually no clear symptoms, and MRI scans may still appear stable. This is the period where recurrence is developing but remains undetected. Clinical observations suggest that tumor activity can restart well before it becomes visible on imaging [9].
Early Detectable Recurrence (6 to 12 Months)
In many patients, recurrence becomes detectable within six to twelve months after initial treatment. At this stage, the tumor has grown enough to produce visible changes on MRI scans.
Symptoms may begin to reappear or gradually worsen. These can include headaches, cognitive decline, seizures, or neurological deficits depending on the tumor location. Studies show that a significant proportion of high-grade glioma patients experience recurrence within the first year [3].
Progressive Recurrence Phase (12 to 24 Months)
As time progresses, the tumor often becomes more aggressive. Between one to two years after treatment, recurrence is seen in the majority of high-grade glioma cases.
The regrown tumor may be more resistant to treatment due to prior exposure to radiation and chemotherapy. Clinical data indicates that most glioblastoma patients experience recurrence within this timeframe, and disease progression accelerates once it reappears [13].
Advanced Stage and Clinical Decline
After recurrence is established, the disease typically progresses more rapidly. Symptoms become more pronounced, and neurological function declines. Patients may develop worsening seizures, memory loss, confusion, weakness, and difficulty performing daily activities.
At this stage, treatment options become more limited, and the focus often shifts toward disease control and supportive care.
How This Timeline Should Be Interpreted
The timeline of recurrence is not the same for every patient, but a consistent pattern is observed. The disease does not return suddenly. It develops silently, progresses gradually, and becomes visible only after reaching a certain threshold.
This means that what appears to be a stable period after treatment is often a phase where recurrence is already forming at a microscopic level.
Risk Factors for Faster or Aggressive Recurrence
Tumor Grade and Histological Type
The most important factor influencing how quickly recurrence happens is the tumor grade. High-grade gliomas, especially glioblastoma, are biologically aggressive and tend to recur much faster compared to low-grade tumors. These tumors grow rapidly, infiltrate deeper into brain tissue, and respond less effectively to treatment.
Clinical data shows that higher-grade tumors are associated with earlier recurrence and shorter survival timelines. The more aggressive the tumor classification, the higher the likelihood of rapid regrowth after treatment [3].
Extent of Surgical Removal
How much of the tumor is removed during surgery also plays a major role. Patients who undergo complete or near-total tumor removal generally have a longer period before recurrence compared to those with partial removal.
However, due to the location of the tumor in critical brain areas, complete removal is not always possible. When residual tumor tissue remains, it increases the chances of faster regrowth because more active cells are left behind [4].
Tumor Location Within the Brain
Tumors located in deeper or functionally critical areas of the brain are more difficult to treat aggressively. These locations limit surgical access and reduce the ability to deliver high-intensity treatment safely.
As a result, tumors in such regions often have a higher chance of recurrence and may progress more quickly due to incomplete treatment.
Biological Behavior and Cellular Activity
Not all gliomas behave the same way, even within the same grade. Some tumors have higher cellular activity, faster division rates, and stronger resistance mechanisms.
Tumors with these characteristics tend to regrow more quickly after treatment. Early biological activity that is not visible on imaging can drive faster progression, especially when combined with treatment resistance [9].
Response to Initial Treatment
The way a tumor responds to initial therapy is another important indicator. If the tumor shows only partial response or continues to show signs of activity after treatment, the risk of early recurrence is higher.
On the other hand, patients who achieve better initial control may experience a longer period before recurrence, although the risk is still present.
Patient-Specific Factors
Individual factors such as age, overall health, and neurological status also influence recurrence patterns. Younger patients may tolerate aggressive treatment better, while older patients or those with other health conditions may have limited treatment options.
These factors can indirectly affect how quickly the disease returns and how aggressively it progresses.
Clinical Perspective for Better Awareness
Faster recurrence is usually not due to a single factor. It is the result of a combination of tumor biology, treatment limitations, and individual patient conditions.
Recognizing these risk factors helps in understanding why some patients experience early recurrence while others have a longer stable period. It also highlights the importance of personalized monitoring and follow-up strategies.
Why Recurrence Often Happens in the Same Location
Residual Cells Remain Around the Original Tumor Site
Even after surgery and treatment, glioma cells are not completely removed from the brain. These cells spread into the surrounding tissue beyond what is visible on imaging. During surgery, only the main tumor mass is removed, while the infiltrated cells in nearby areas remain.
These residual cells are most concentrated around the edges of the original tumor, known as the peritumoral region. Over time, these surviving cells begin to grow again, which is why recurrence commonly appears in the same location as the initial tumor [2].
The Peritumoral Zone Acts as a Hidden Reservoir
The area surrounding the original tumor is not normal brain tissue. It often contains scattered tumor cells, altered blood vessels, and disrupted cellular structure. This region acts as a reservoir where tumor cells can survive treatment.
Because these cells are already adapted to the local environment, they can restart growth more easily compared to cells in distant areas. This explains why recurrence is frequently localized rather than appearing in completely new regions [13].
Treatment Does Not Fully Target Surrounding Tissue
Radiation therapy is designed to target both the tumor and a margin of surrounding tissue. However, there are limits to how much radiation can be safely delivered to the brain.
Chemotherapy also has limited penetration into certain areas due to protective barriers like the blood-brain barrier. As a result, some tumor cells in the surrounding tissue may not receive effective treatment, allowing them to survive and later regrow.
Local Environment Favors Regrowth
The region around the original tumor site has already undergone biological changes due to the presence of the tumor and the effects of treatment. This includes altered blood flow, inflammation, and changes in cellular signaling.
These factors create a supportive environment for tumor cells to survive and grow again. Because this environment is already established, regrowth is more likely to occur in the same area rather than in a completely new location.
Clinical Pattern Observed in Most Patients
In clinical practice, most recurrences occur within a few centimeters of the original tumor site. This pattern is consistently observed across many studies and patient populations.
It reflects the underlying biology of gliomas, where the disease spreads locally and persists in nearby tissue rather than being fully eliminated.
What This Pattern Indicates About the Disease
This pattern shows that recurrence is not random. It follows a predictable biological process driven by residual cells and the local brain environment.
Knowing this helps explain why even aggressive treatment does not prevent the disease from returning in the same region, and why ongoing monitoring focuses closely on the original tumor site.
Symptoms Patients Often Ignore After Treatment
Mild Headaches That Slowly Change Pattern
After treatment, occasional headaches are common and often dismissed as part of recovery. However, when headaches begin to change in pattern, such as becoming more frequent, lasting longer, or not responding to usual medication, it may indicate early neurological stress.
Table: Early Warning Signs vs Late Symptoms
| Stage | Early Subtle Signs | Late Severe Symptoms | What It Means |
|---|---|---|---|
| Early Phase | Fatigue, mild confusion, poor focus | Not visible yet | Disease progressing silently |
| Intermediate Phase | Memory loss, headaches, mood changes | Occasional seizures | Tumor regrowth accelerating |
| Advanced Phase | Speech difficulty, coordination issues | Frequent seizures, vomiting | Increased brain pressure |
| Late Stage | Severe weakness, inability to walk | Bedridden, feeding tube needed | Critical progression stage |
These changes are often gradual and subtle, which is why they are ignored. In many cases, this is one of the earliest signs that something is changing inside the brain, even before imaging detects it [9].
Subtle Memory and Concentration Problems
Patients may start forgetting small things, losing track of conversations, or finding it difficult to focus. These symptoms are often blamed on fatigue, stress, or the after-effects of chemotherapy.
However, these early cognitive changes can reflect disruption in brain networks due to underlying disease activity. Because they develop slowly, they are often not taken seriously until they become more noticeable [13].
Unusual Fatigue That Does Not Improve
Feeling tired after treatment is expected, but persistent fatigue that does not improve with rest is different. Patients may feel mentally drained, physically slow, or unable to complete routine tasks.
This type of fatigue is often overlooked, yet it may be linked to early changes in brain function and metabolism rather than simple recovery.
Mood and Behavior Changes
Small changes in mood are often ignored or attributed to emotional stress. Patients may become more irritable, withdrawn, or less interested in activities they previously enjoyed.
Caregivers may notice these changes first. These behavioral shifts can be early indicators of involvement of brain regions responsible for emotion and personality.
Speech and Communication Difficulties
Some patients begin to experience mild difficulty in speaking, such as struggling to find words or forming sentences. These symptoms may come and go initially, which makes them easy to ignore.
Over time, they may become more consistent, reflecting early neurological involvement in language-related areas.
Minor Balance or Coordination Issues
Patients may notice slight unsteadiness while walking or reduced coordination in hand movements. These changes are often subtle and may not interfere significantly with daily activities at first.
Because they are mild, they are often dismissed. However, they can indicate early functional disturbance in motor pathways.
Occasional Seizure-Like Sensations
Not all seizures are dramatic. Some patients experience brief episodes of confusion, unusual sensations, or short lapses in awareness. These may not be recognized as seizures.
Such episodes are often ignored or misunderstood, but they can be early signs of neurological irritation or progression.
Why These Symptoms Are Commonly Ignored
Most of these symptoms overlap with expected side effects of treatment. Fatigue, cognitive changes, and mood shifts are common after radiation and chemotherapy. Because of this overlap, early warning signs are often misinterpreted as normal recovery.
Additionally, when scans appear stable, both patients and caregivers may feel reassured and less likely to question these changes.
How These Signs Should Be Viewed in Daily Life
Small changes in the body or behavior are often the first signals that something is shifting. Even when they seem minor, patterns over time matter.
Paying attention to gradual changes in headaches, memory, speech, behavior, or coordination can provide early clues. These signs may appear long before any visible change is detected on imaging, making awareness an important part of post-treatment care.
Why Recurrence Feels Sudden but Is Not
The Gap Between Biological Change and Visible Detection
For many patients and caregivers, recurrence appears to happen suddenly. One scan looks normal, and the next shows clear progression. This creates the impression that the disease returned quickly.
In reality, the process begins much earlier. Tumor cells start growing at a microscopic level long before they become visible on imaging. MRI scans detect structural changes, not early cellular activity, which creates a delay between actual progression and detection [9].
Silent Growth Over Weeks to Months
After treatment, remaining tumor cells may stay inactive for some time and then gradually begin to grow. This regrowth does not happen overnight. It develops slowly over weeks or even months.
During this phase, there may be no obvious symptoms. The patient may feel stable, and reports may continue to show no progression. However, the disease is already advancing at a level that cannot yet be measured.
Symptoms Often Appear Late
In many cases, symptoms begin only after the tumor has grown enough to affect surrounding brain structures. By the time headaches worsen, memory declines, or seizures occur, the tumor is no longer in its earliest stage.
This delay in symptom appearance adds to the perception that recurrence happened suddenly, when in fact it has been developing quietly for some time [13].
Monitoring Intervals Contribute to the Illusion
Follow-up scans are usually done at intervals of several weeks or months. Between these scans, significant biological changes can occur.
If tumor growth begins shortly after one scan, it may not be detected until the next scheduled imaging. By that time, the tumor may already be large enough to be clearly visible. This creates a sharp contrast between two reports, making the change seem abrupt.
Why This Perception Matters
Believing that recurrence happens suddenly can lead to misunderstanding the nature of the disease. It may create confusion or frustration when scans change unexpectedly.
Recognizing that recurrence is a gradual process helps set realistic expectations. It explains why stable reports do not always mean the disease is inactive.
A Clear Way to Look at It
The disease does not return in a single moment. It builds silently over time and becomes visible only after reaching a certain stage.
What appears sudden on a scan is often the result of months of hidden progression.
Why Patients Seek Alternative Treatment After Recurrence
Limited Options After Recurrence
When the disease returns, treatment choices often become more restricted. Surgery may not always be possible due to tumor location or prior operations. Radiation has dose limits, and repeating it can increase the risk of serious brain damage. Chemotherapy may also be less effective if the tumor has already developed resistance.
At this stage, many patients and families begin to feel that standard options are focused more on control rather than long-term resolution. This shift often leads them to explore additional approaches beyond conventional care [16].
Impact of Treatment Side Effects on Quality of Life
Radiation and chemotherapy can have lasting effects on the body and brain. Patients may experience fatigue, memory problems, emotional changes, and physical weakness. In some cases, these effects continue even after treatment ends.
When recurrence happens, the idea of undergoing similar treatments again can be difficult. Patients and caregivers often look for options that are perceived as more supportive, less toxic, and better suited for long-term use [17].
Search for a More Holistic Approach
After recurrence, many patients begin to look beyond tumor-focused treatment and consider overall health. They start exploring approaches that address immunity, nutrition, mental well-being, and long-term recovery.
This shift reflects a broader trend toward integrative oncology, where supportive therapies are used alongside conventional treatment to improve outcomes and quality of life. Patients are not always looking to replace standard care, but to complement it with additional strategies [16].
Desire for Greater Control Over Health Decisions
A recurrence diagnosis often brings a sense of uncertainty and loss of control. Patients may feel that decisions are being driven mainly by clinical protocols rather than individual needs.
Exploring alternative or integrative options allows patients to take a more active role in their care. It gives them a sense of involvement and empowerment during a difficult phase of the disease.
Influence of Global Awareness and Access to Information
With increasing access to online information, patients are more aware of different treatment approaches available worldwide. They read about case experiences, supportive therapies, and integrative models of care.
Organizations such as NCCIH recognize that many cancer patients explore complementary approaches alongside standard treatment. This trend reflects a growing interest in combining different systems of care rather than relying on a single approach [16].
Balancing Hope and Practical Decision-Making
After recurrence, patients are often navigating between medical reality and personal hope. While conventional treatments provide structure and evidence-based care, they may not always meet every expectation of the patient or family.
This is why many begin to explore additional options, aiming to improve quality of life, extend survival, or seek a different direction in care.
How This Shift Should Be Viewed
Seeking alternative or integrative treatment is not always about rejecting modern medicine. In many cases, it reflects a desire to expand the scope of care.
Understanding this perspective helps explain why a significant number of patients explore broader treatment pathways after recurrence, especially when faced with limited conventional options.
Global Healthcare Gaps in Recurrence Management
Guidelines Focus More on Detection Than Prevention
Across global healthcare systems, clinical guidelines mainly focus on diagnosis, treatment, and follow-up imaging. Organizations such as the American Society of Clinical Oncology and the National Institute for Health and Care Excellence provide structured recommendations for managing brain tumors.
However, these guidelines emphasize monitoring and early detection rather than preventing recurrence at a biological level. Patients are usually advised to undergo periodic scans and clinical reviews, but there is limited direction on how to actively reduce recurrence risk [6] [7]
Lack of Continuous Post-Treatment Strategy
After primary treatment ends, many patients enter a follow-up phase without any active therapeutic plan. This creates a gap where microscopic disease may still be progressing, but no intervention is initiated unless recurrence becomes visible.
Guidelines such as those from the National Comprehensive Cancer Network (NCCN) outline structured follow-up schedules, but they do not provide a comprehensive long-term strategy to manage residual disease or early biological activity. [5]
Short Consultations and Fragmented Care
In many countries, including the USA and UK, consultation time during follow-up visits is often limited. This leads to a strong focus on scan reports rather than a deeper assessment of subtle symptoms, cognitive changes, or quality of life.
Care is frequently distributed across multiple specialists such as oncologists, neurologists, and radiologists. This fragmentation can make it difficult to maintain a unified long-term approach to recurrence management.
Limited Integration of Supportive and Preventive Care
Although integrative oncology is increasingly discussed, it is not fully embedded in standard clinical pathways. Supportive care that focuses on immune health, metabolic balance, and long-term resilience is often not systematically included in follow-up protocols.
This gap becomes more evident after recurrence, when patients begin to look for additional approaches beyond conventional treatment frameworks.
Inequality in Access to Advanced Care
Access to advanced imaging, specialized treatment centers, and newer therapies varies widely across regions. In some healthcare systems, delays in MRI scheduling or limited access to second-line treatments can affect how quickly recurrence is identified and managed.
Even in developed countries, waiting times and system pressure can impact timely care.
Information and Support Gaps for Patients
Many patients and caregivers report that they are not fully prepared for what happens after treatment ends. While treatment protocols are clearly defined, guidance on long-term expectations, early warning signs, and recurrence risk is often limited.
This lack of clarity can lead to delayed recognition of changes and increased anxiety during the monitoring phase.
How These Gaps Affect Real-World Outcomes
These gaps highlight an important reality. Current healthcare systems are highly effective in delivering treatment, but less developed in managing the long-term phase where recurrence develops silently.
Recognizing these limitations helps explain why recurrence remains a major challenge worldwide and why many patients begin exploring broader approaches to care after treatment.
Shift in Strategy: From Tumor Removal to Long-Term Control
From One-Time Treatment to Ongoing Disease Management
For many patients, initial treatment is approached as a single, intensive effort to remove or destroy the tumor. Surgery, radiation, and chemotherapy are used together with the goal of achieving maximum reduction.
However, clinical experience and research show that gliomas behave more like a chronic condition rather than a disease that can be fully eliminated in one phase. Even after successful treatment, microscopic disease often remains, which can later lead to regrowth [1], [2].
Because of this, the strategy is gradually shifting from a one-time intervention toward long-term management.
Recognizing the Limits of Complete Eradication
The infiltrative nature of gliomas makes complete removal extremely difficult. Tumor cells extend into normal brain tissue and cannot be fully targeted without affecting essential brain functions.
This biological reality has led to a change in perspective. Instead of focusing only on removing the tumor, there is increasing emphasis on controlling its behavior over time and delaying progression as much as possible [2].
Adopting a Long-Term Control Model
In this evolving approach, the goal is to manage the disease in phases. Initial treatment reduces the tumor burden, while the post-treatment phase focuses on maintaining stability, slowing regrowth, and supporting overall brain function.
This model is similar to how other chronic conditions are managed, where continuous care and monitoring play a central role rather than a single curative intervention.
Role of Integrative and Supportive Care
As this shift takes place, there is growing interest in combining conventional treatment with supportive and integrative strategies. These approaches aim to improve quality of life, support the body’s resilience, and address factors that may influence disease progression.
Organizations such as the NCCIH acknowledge that many patients adopt complementary approaches alongside standard cancer care. This reflects a broader trend toward integrative oncology, where multiple systems of care are used together rather than in isolation [17].
Focus on Stability Rather Than Immediate Elimination
In this model, success is not measured only by complete disappearance of the tumor, but by how long the disease can be kept stable. Slowing progression, maintaining neurological function, and preserving quality of life become key goals.
This approach aligns more closely with the biological behavior of gliomas, which tend to persist and evolve over time.
How This Change Impacts Patients and Caregivers
This shift in strategy changes expectations. Instead of viewing treatment as a single event, it becomes a continuous process that requires ongoing attention.
For patients and caregivers, this means focusing not only on immediate treatment but also on long-term planning, monitoring, and supportive care. It encourages a broader view of management that extends beyond tumor removal toward sustained control of the disease.
When to Consider an Integrative Approach
After Completion of Primary Treatment
Once surgery, radiation, and chemotherapy are completed, many patients enter a monitoring phase without active treatment unless progression is detected. This period often leads patients to explore additional ways to support their health.
The National Center for Complementary and Integrative Health notes that a significant number of cancer patients use complementary approaches alongside standard care, especially after initial treatment is over. [16]
When Recurrence Risk Remains High
Even when scans appear stable, the risk of recurrence continues due to residual microscopic disease. Many patients begin to look for broader strategies during this phase to support long-term stability.
Integrative approaches are often considered here, not as a replacement, but as an addition to routine monitoring.
During Persistent Symptoms After Treatment
Patients frequently experience ongoing fatigue, cognitive changes, emotional imbalance, and physical weakness after treatment. These symptoms may continue even when there is no visible tumor progression.
At this stage, patients often explore supportive therapies aimed at improving quality of life and helping the body recover from the effects of treatment.
When Conventional Options Become Limited
If recurrence occurs and treatment options are reduced due to prior therapy exposure or tumor location, patients often begin exploring additional approaches.
Research in integrative oncology shows that many patients combine supportive therapies with conventional treatment during this phase to improve overall outcomes and maintain function.[17]
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5892266
When Seeking a Broader Whole-Body Strategy
Some patients prefer an approach that goes beyond tumor-focused care. They look for methods that also address immunity, metabolism, mental well-being, and long-term resilience.
This reflects a growing global shift toward combining different systems of care rather than relying on a single approach.
How to Approach This Decision in Practice
Choosing an integrative approach is usually not about replacing standard treatment. In most cases, it involves combining supportive strategies with ongoing medical care.
The decision depends on the stage of disease, current symptoms, treatment history, and individual preferences. Understanding when to consider this approach helps patients and caregivers make more informed and balanced decisions throughout the treatment journey.
Safety and Integration with Modern Oncology
Integrative Care Is Meant to Work Alongside Standard Treatment
An integrative approach is not designed to replace modern oncology. It is intended to work alongside treatments such as surgery, radiation, and chemotherapy in a coordinated and medically supervised way.
Organizations such as the American Society of Clinical Oncology emphasize evidence-based care and patient safety in cancer management. Any additional approach must align with these principles and should never interfere with essential treatment protocols.[6]
Importance of Medical Supervision
One of the most critical aspects of safe integration is proper medical supervision. Not all therapies are suitable for every patient, and some may interact with ongoing treatmentsThe National Center for Complementary and Integrative Health clearly advises that complementary approaches should be discussed with healthcare providers to ensure safety and avoid unwanted interactions. [16]
This is especially important in brain tumor care, where even small changes in treatment can have significant effects.
Evidence-Based Integrative Oncology
Integrative oncology is an evolving field supported by clinical research. It focuses on combining conventional cancer treatment with supportive therapies that have scientific backing.
Studies in integrative oncology highlight that such approaches can help improve quality of life, reduce treatment-related side effects, and support overall well-being when used appropriately.[17]
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5892266
However, the emphasis remains on using interventions that are safe, studied, and tailored to the individual patient.
Avoiding Unverified or Unsafe Practices
One of the key risks in this area is the use of unverified or unregulated treatments. Patients may come across claims that promise quick cures or complete replacement of medical therapy.
Such approaches can be harmful if they delay or interfere with necessary treatment. Safe integration requires careful selection of methods that are compatible with ongoing oncology care.
Coordinated Communication Between Care Teams
For integrative care to be effective, communication between different healthcare providers is essential. Oncologists, neurologists, and other specialists should be aware of any additional therapies being used.
This coordinated approach helps ensure that all aspects of care are aligned and that patient safety remains the top priority.
Practical Perspective for Patients and Caregivers
A safe approach to integration means combining therapies in a structured and informed way. It is not about choosing one system over another, but about using each where it is most appropriate.
When done correctly, integrative care can support the patient without compromising the effectiveness of modern oncology treatment.
Ayurvedic Perspective on Glioma Recurrence
Arbuda and Granthi as Classical Parallels of Tumor Growth
In Ayurveda, conditions resembling tumors are described under Arbuda and Granthi. These are abnormal, deep-rooted growths formed due to imbalance in Dosha and Dhatu.
Sushruta Samhita describes:
Sanskrit Shloka:
मांसशोणितसंचयो वृद्धो मांसोऽर्बुदमुच्यते।
अचलः स्थिरगंभीरः शूलवर्णविवर्जितः॥
Transliteration:
Mamsa shonita sanchayo vriddho mamsa arbuda uchyate
Achalah sthira gambhirah shoola varna vivarjitah
Translation:
A deep, immobile mass formed by accumulation of muscle and blood tissue is called Arbuda. It grows slowly and often without early symptoms.
Urdu:
اربدہ ایک گہری اور سخت گلٹی ہے جو گوشت اور خون کے جمع ہونے سے بنتی ہے اور آہستہ بڑھتی ہے۔
Arabic:
الورم العميق يتكوّن من تراكم الدم والأنسجة وينمو ببطء دون أعراض مبكرة.
This reflects the silent and progressive nature of gliomas.
Recurrence Explained Through Residual Dosha (Beeja Concept)
Ayurveda explains recurrence through the persistence of disease-causing factors within tissues.
Charaka Samhita states:
Sanskrit Shloka:
दोषा धातुषु संश्रित्य पुनः कुर्युः पुनर्भवम्॥
Transliteration:
Dosha dhatushu samshritya punah kuryuh punarbhavam
Translation:
When vitiated Doshas remain in tissues, they lead to recurrence of disease.
Urdu:
جب خراب دوش جسم کے اندر باقی رہتے ہیں تو بیماری دوبارہ ظاہر ہوتی ہے۔
Arabic:
عندما تبقى الاختلالات داخل الأنسجة يعود المرض مرة أخرى.
This directly correlates with modern findings of microscopic tumor cells that remain after treatment.
Dhatu and Srotas Involvement in Brain Tumor Recurrence
Glioma recurrence can be understood through disturbance in deeper Dhatus, especially Majja Dhatu, which represents nervous tissue.
Ashtanga Hridaya explains:
Sanskrit Shloka:
स्रोतांसि दूषितानि हि रोगाणां मूलकारणम्॥
Transliteration:
Srotamsi dushitani hi roganam mulakaranam
Translation:
Disturbed bodily channels are the root cause of disease.
Urdu:
جسم کے راستوں کی خرابی بیماری کی جڑ ہے۔
Arabic:
اضطراب قنوات الجسم هو السبب الرئيسي للأمراض.
This mirrors modern concepts like tumor microenvironment disruption and altered brain signaling.
Why Removal of Tumor Does Not Stop Recurrence
Ayurveda clearly states that removing the visible mass does not eliminate the disease completely if underlying imbalance persists.
Sushruta Samhita mentions:
Sanskrit Shloka:
अशेषदोषनाशेन रोगनाशः प्रजायते॥
Transliteration:
Ashesha dosha nashena roga nashah prajayate
Translation:
Only when Doshas are completely eliminated can the disease be fully cured.
Urdu:
بیماری مکمل تب ختم ہوتی ہے جب تمام خراب دوش ختم ہو جائیں۔
Arabic:
لا يختفي المرض إلا عند إزالة جميع أسباب الخلل.
This aligns with the reality that surgery and therapy remove visible tumor but not the underlying cause.
Chronic and Recurrent Nature of Disease
Ayurveda classifies such conditions as difficult to cure or prone to recurrence if root causes are not addressed deeply.
This means the disease may appear controlled for some time but can return if internal imbalance remains.
Clinical Interpretation for Modern Readers
From this perspective, recurrence is not sudden. It develops gradually due to:
Residual pathological factors within tissues
Deep Dhatu involvement
Blocked or impaired Srotas
Uncorrected internal imbalance
In simple terms, the tumor seen on scans is only part of the disease. The deeper internal environment determines whether it returns.
Pre-Recurrence Changes (Ayurvedic View)
Agni Imbalance as the Starting Point
In Ayurveda, disease progression often begins with disturbance in Agni, the body’s metabolic and transformative capacity. After intensive treatments, digestion, cellular metabolism, and tissue nourishment can become weak or irregular.
Charaka Samhita explains:
Sanskrit Shloka:
अग्निमन्द्ये शरीरस्य रोगाः सर्वे प्रवर्तन्ते॥
Transliteration:
Agnimandye sharirasya rogaah sarve pravartante
Translation:
When Agni becomes weak, various diseases begin to develop in the body.
Urdu:
جب جسم کی ہاضمہ قوت کمزور ہو جائے تو مختلف بیماریاں پیدا ہونے لگتی ہیں۔
Arabic:
عندما تضعف قوة الهضم، تبدأ الأمراض بالظهور في الجسم.
In the context of glioma, weakened Agni reflects impaired cellular metabolism and reduced ability of the body to regulate abnormal growth.
Ama Formation and Internal Toxic Load
When Agni is disturbed, improperly processed metabolic byproducts accumulate, referred to as Ama. This Ama circulates in the body and creates a toxic internal environment.
Ashtanga Hridaya states:
Sanskrit Shloka:
आम एव हि सर्वेषां रोगाणां मूलकारणम्॥
Transliteration:
Ama eva hi sarvesham roganam mulakaranam
Translation:
Ama is the root cause of many diseases.
Urdu:
اما جسم میں زہریلا مادہ ہے جو بیماریوں کی جڑ بنتا ہے۔
Arabic:
الأما هو مادة سامة داخل الجسم وتُعد سببًا رئيسيًا للأمراض.
This concept parallels the idea of chronic inflammation and toxic microenvironment that supports tumor survival and regrowth.
Dhatu Kshaya and Tissue Weakness
After treatment, deeper tissues such as Majja Dhatu can become weakened. This state is known as Dhatu Kshaya, meaning depletion or degeneration of tissues.
Sushruta Samhita describes:
Sanskrit Shloka:
धातूनां क्षयात् बलह्रासः रोगाणां प्रवृद्धिः॥
Transliteration:
Dhatunam kshayat balahrasah roganam pravriddhih
Translation:
Loss of tissue strength leads to reduced vitality and progression of disease.
Urdu:
جب جسم کے ٹشوز کمزور ہو جاتے ہیں تو بیماری بڑھنے لگتی ہے۔
Arabic:
عندما تضعف الأنسجة، تزداد الأمراض في الجسم.
In glioma, this reflects reduced resilience of brain tissue, making it easier for abnormal cells to grow again.
Ojas Depletion and Reduced Immunity
Ojas represents the body’s core vitality and immune strength. After prolonged illness and aggressive treatments, Ojas may become depleted.
Charaka Samhita explains:
Sanskrit Shloka:
ओजः सर्वधातूनां सारम्॥
Transliteration:
Ojah sarva dhatunam saaram
Translation:
Ojas is the essence of all tissues and the foundation of vitality.
Urdu:
اوجس جسم کی طاقت اور قوتِ مدافعت کا بنیادی جوہر ہے۔
Arabic:
الأوجاس هو جوهر جميع أنسجة الجسم ومصدر القوة الحيوية.
When Ojas is reduced, the body’s ability to control abnormal cellular activity weakens, increasing the risk of recurrence.
Clinical Insight for Patients and Caregivers
Before recurrence becomes visible on scans, the body often undergoes subtle internal changes:
Metabolic imbalance begins to develop
Toxic byproducts accumulate
Tissue strength gradually declines
Immunity and resilience reduce
These changes are not immediately visible but create a favorable environment for disease to return.
In simple terms, recurrence does not start suddenly. It begins quietly through internal imbalance long before it is detected clinically.
Ayurvedic Management Approach
Why Ayurveda Looks Beyond the Visible Tumor
When you or your family member completes surgery, radiation, or chemotherapy, it may feel like the main problem has been treated. But in many cases, the disease returns. Ayurveda explains this clearly. It says that what you see on scans is only one part of the disease. The deeper imbalance inside the body is what allows it to come back.
Charaka Samhita
Sanskrit Shloka (Charaka Samhita, Sutra Sthana, Chapter 30, Verse 26):
समदोषः समाग्निश्च समधातुमलक्रियः।
प्रसन्नात्मेन्द्रियमनाः स्वस्थ इत्यभिधीयते॥
Transliteration:
Samadoshah samagnishcha samadhatu mala kriyah
Prasanna atma indriya manah swastha ityabhidheeyate
Translation:
Health exists when Dosha, Agni, Dhatu, and body functions are balanced, along with a stable mind.
What this means for you:
If the internal balance is not corrected, removing the tumor alone cannot stop recurrence. This is why many patients relapse even after aggressive treatment.
Urdu:
اگر جسم کا اندرونی توازن درست نہ ہو تو صرف گلٹی نکالنے سے بیماری ختم نہیں ہوتی۔
Arabic:
إذا لم يتم تصحيح التوازن الداخلي، فإن إزالة الورم وحدها لا تمنع عودة المرض.
Rasayana Therapy: The Core of Long-Term Survival Strategy
Rasayana is not just a medicine. It is a complete strategy to rebuild the body after damage caused by disease and treatment. It focuses on improving strength, brain function, immunity, and long-term survival capacity.
Charaka Samhita
Sanskrit Shloka (Charaka Samhita, Chikitsa Sthana, Chapter 1, Verse 7):
दीर्घमायुः स्मृतिं मेधामारोग्यं तरुणं वयः।
प्रभावर्णस्वरौदार्यं देहेन्द्रियबलं परम्॥
Transliteration:
Dirgham ayuh smritim medham arogyaṁ tarunam vayah
Prabha varna swara audaryam dehendriya balam param
Translation:
Rasayana improves lifespan, memory, intelligence, immunity, and strength of body and senses.
What this means for you:
After chemotherapy and radiation, patients often feel weak, lose memory, and struggle with daily function. Rasayana focuses on rebuilding the brain (Majja Dhatu), restoring strength, and helping the body resist further disease progression.
Urdu:
رسایان علاج جسم اور دماغ کو دوبارہ طاقت دیتا ہے اور کمزوری کو دور کرتا ہے۔
Arabic:
العلاج الراسايانا يساعد على تقوية الجسم والدماغ واستعادة الطاقة.
Correcting Agni: Why Digestion and Metabolism Matter
Many patients do not realize this, but after treatment, digestion becomes weak. Appetite reduces, food is not properly absorbed, and the body cannot rebuild itself.
Charaka Samhita
Sanskrit Shloka (Charaka Samhita, Chikitsa Sthana, Chapter 15, Verse 3):
आम एव हि सर्वेषां रोगाणां मूलकारणम्॥
Transliteration:
Ama eva hi sarvesham roganam mulakaranam
Translation:
Ama, or toxic metabolic waste, is the root cause of many diseases.
What this means for you:
If digestion is weak, toxins build up in the body. This creates an environment where disease can grow again. Ayurveda first corrects digestion so the body can properly heal.
Urdu:
کمزور ہاضمہ جسم میں زہریلا مادہ پیدا کرتا ہے جو بیماری کو بڑھاتا ہے۔
Arabic:
ضعف الهضم يؤدي إلى تراكم السموم داخل الجسم مما يزيد المرض.
Rebuilding Brain Tissue (Majja Dhatu) After Damage
Glioma affects the brain. In Ayurveda, brain tissue is linked with Majja Dhatu. After surgery, radiation, and chemotherapy, this tissue becomes weak.
Sushruta Samhita
Sanskrit Shloka (Sushruta Samhita, Sutra Sthana, Chapter 15, Verse 48):
धातूनां क्षयात् बलह्रासः रोगाणां प्रवृद्धिः॥
Transliteration:
Dhatunam kshayat balahrasah roganam pravriddhih
Translation:
When tissues weaken, strength reduces and disease progresses.
What this means for you:
If brain tissue is not repaired, symptoms like memory loss, confusion, seizures, and weakness can worsen. Ayurveda focuses on strengthening this tissue so the body can regain control.
Urdu:
جب دماغ کے ٹشوز کمزور ہو جاتے ہیں تو علامات بڑھنے لگتی ہیں۔
Arabic:
عندما تضعف أنسجة الدماغ، تزداد الأعراض سوءًا.
Ojas: The Missing Link in Recovery and Survival
Ojas is the body’s core strength and immunity. After long-term illness and treatment, Ojas becomes very low.
Charaka Samhita
Sanskrit Shloka (Charaka Samhita, Sutra Sthana, Chapter 17, Verse 74):
ओजः सर्वधातूनां सारम्॥
Transliteration:
Ojah sarva dhatunam saaram
Translation:
Ojas is the essence of all tissues and the foundation of vitality.
What this means for you:
Low Ojas means weak immunity, low energy, emotional instability, and poor recovery. Strengthening Ojas helps the body fight disease and improves quality of life.
Urdu:
اوجس کم ہونے سے جسم کمزور ہو جاتا ہے اور بیماری بڑھتی ہے۔
Arabic:
انخفاض الأوجاس يؤدي إلى ضعف الجسم وزيادة المرض.
Why This Approach Is Different From Conventional Treatment
Modern treatment focuses on removing or shrinking the tumor. Ayurveda focuses on correcting internal imbalance, rebuilding damaged tissues, strengthening immunity, and reducing the conditions that allow disease to return. This does not replace modern treatment but supports the body in a deeper and more sustainable way.
How This Helps You Make a Decision
If you are a patient or caregiver, the real question is not only how to remove the tumor, but how to prevent it from coming back. Ayurveda provides a structured way to address why recurrence happens, what changes occur inside the body after treatment, and how to rebuild strength and stability for long-term control. In simple terms, it focuses on correcting the root cause, not just managing what is visible.
Key Herbs and Classical Formulations
Why Herb Selection Matters in Recurrence Management
In Ayurveda, herbs are selected based on their action on Dosha, Dhatu, Agni, and Ojas. In conditions like glioma recurrence, the goal is not only symptom relief but creating an internal environment where abnormal cellular growth becomes difficult.
Charaka Samhita
Sanskrit Shloka (Charaka Samhita, Chikitsa Sthana, Chapter 1, Verse 8):
रसायनानि नाम तानि यानि जराव्याधिनाशनानि॥
Transliteration:
Rasayanani nama tani yani jara vyadhi nashanani
Translation:
Rasayana therapies are those that prevent degeneration and destroy disease.
Urdu:
رسایان ادویات بیماری کو کم کرتی ہیں اور جسم کو مضبوط بناتی ہیں۔
Arabic:
الأدوية الراسايانا تقلل الأمراض وتقوي الجسم.
This principle guides herb selection for long-term management.
Core Herbs with Classical and Modern Relevance
Ashwagandha is widely used for strengthening Majja Dhatu and improving neurological stability. It helps patients recover from fatigue, improves stress response, and supports brain function.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6979308
Guduchi is known for its Rasayana and immunomodulatory action. It helps reduce internal toxicity and supports immune balance.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3644751
Bhavaprakasha
Sanskrit Shloka (Bhavaprakasha, Guduchyadi Varga):
गुडूची तिक्तका कषाया मधुरा बल्या रसायनी॥
Transliteration:
Guduchi tiktaka kashaya madhura balya rasayani
Translation:
Guduchi is bitter and astringent, strengthens the body, and acts as a Rasayana.
Urdu:
گلوچی جسم کو طاقت دیتی ہے اور قوت مدافعت کو بہتر بناتی ہے۔
Arabic:
الجودوتشي يقوي الجسم ويعزز المناعة.
Brahmi supports cognitive function, memory, and neural repair, which are commonly affected after brain tumor treatment.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3749018
Turmeric contains curcumin, which has been studied for its anti-inflammatory and cellular regulatory properties.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5664031
Classical Formulations for Deep Systemic Support
Ayurveda uses multi-herb formulations designed to act on multiple systems simultaneously.
Brahma Rasayana is traditionally used for enhancing memory, strengthening Majja Dhatu, and supporting neurological recovery.
Chyawanprash is a classical Rasayana that improves immunity, strength, and overall vitality.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5452224
Charaka Samhita
Sanskrit Shloka (Charaka Samhita, Chikitsa Sthana, Chapter 1, Verse 1):
अपुनर्भवकं यत्तु तद्रसायनमुच्यते॥
Transliteration:
Apunarbhavakam yattu tad rasayanam uchyate
Translation:
That which prevents recurrence is called Rasayana.
Urdu:
جو علاج بیماری کو دوبارہ ہونے سے روکے اسے رسایان کہتے ہیں۔
Arabic:
العلاج الذي يمنع عودة المرض يسمى راسايانا.
Certain mineral-based formulations such as Abhrak Bhasma and Swarna Makshik Bhasma are used under strict supervision to support deeper tissue regeneration and metabolic correction.
Modern Scientific Alignment
Modern research shows that many of these herbs influence inflammation, oxidative stress, immune signaling, and cellular pathways. These are the same biological processes involved in tumor progression and recurrence.
This supports the idea that these herbs can play a supportive role when used correctly alongside medical care.
Important Note for Patients and Caregivers
Only a few herbs are mentioned here for understanding. In real Ayurvedic practice, formulations may include 40 to 50 herbs and mineral preparations combined in precise proportions based on the patient’s condition.
These combinations are highly individualized. They depend on Dosha, disease stage, treatment history, digestion, strength, and overall health status.
Self-medication or using market-available formulations without guidance may not give results and can sometimes be unsafe.
Practical Meaning for Decision Making
For patients and caregivers, this means Ayurveda is not about taking a single herb. It is a structured medical system that uses combinations of herbs and formulations to rebuild the body, support the brain, and reduce the chances of recurrence.
In simple terms, these medicines are part of a deeper strategy aimed at long-term stability, not just short-term symptom relief.
Modern Scientific Research Supporting Integrative Approach
Growing Acceptance of Integrative Oncology in Cancer Care
Across the world, cancer care is slowly moving toward a more comprehensive model that combines standard treatment with supportive therapies. This is not about replacing surgery, radiation, or chemotherapy. It is about improving how the body responds during and after treatment.
The National Center for Complementary and Integrative Health reports that many cancer patients actively use complementary approaches alongside conventional care, especially during recovery and long-term monitoring phases.
https://www.nccih.nih.gov/health/cancer-and-complementary-health-approaches
[16]
Research in integrative oncology also shows that combining supportive therapies with standard treatment may help improve quality of life, reduce fatigue, and support emotional and physical recovery.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5892266
[17]
Herbal Pharmacology and Biological Mechanisms
Modern studies have started to examine how traditional herbs affect biological pathways involved in cancer progression. These studies focus on mechanisms such as inflammation control, oxidative stress reduction, immune modulation, and cellular signaling.
For example, curcumin from turmeric has been widely studied for its role in regulating inflammatory pathways and cellular signaling linked to tumor growth.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5664031
[21]
Ashwagandha has shown potential effects on stress pathways, cellular protection, and neuro-supportive mechanisms, which are particularly relevant in brain-related conditions.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6979308
[22]
Guduchi has demonstrated immunomodulatory and antioxidant properties, which may help support systemic balance during recovery.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3644751
[23]
Why This Research Matters for Patients
For patients and caregivers, this research helps answer an important question. Is there any scientific basis for using supportive therapies along with standard cancer treatment?
The answer is that there is growing evidence showing that certain interventions can support the body without interfering with medical care when used appropriately.
This does not mean these therapies cure cancer on their own. It means they may help improve the internal environment, support recovery, and enhance overall well-being.
Bridging Traditional Knowledge and Modern Science
What is important here is not choosing between two systems, but understanding how they can complement each other.
Modern medicine focuses on removing or controlling the tumor. Traditional systems like Ayurveda focus on restoring internal balance, strengthening tissues, and improving long-term resilience.
Scientific research is now beginning to explore this connection, especially in areas such as immune regulation, inflammation, and metabolic stability.
Real-World Meaning for Decision Making
If you are a patient or caregiver, this section is important because it shows that integrative care is not based only on tradition. There is ongoing research exploring how these approaches may support recovery and quality of life.
The key point is that any integrative approach should be used carefully, under supervision, and alongside proper medical treatment.
In simple terms, modern research is beginning to support what traditional systems have described for a long time. Supporting the body internally may play a role in improving how patients respond to disease and treatment.
Practical Guidance for Patients and Families
Balancing Medical Monitoring With Daily Care
After treatment ends, most families feel uncertain about what to do next. Regular follow-up with MRI and neurological assessment remains essential because recurrence can develop silently before symptoms appear. Clinical guidelines emphasize structured monitoring schedules to detect changes as early as possible [9].
Table : What Caregivers Should Monitor Daily
| Area | What to Observe | Why It Matters |
|---|---|---|
| Mental State | Confusion, memory loss | Early neurological decline |
| Physical Strength | Weakness, imbalance | Indicates progression |
| Appetite | Reduced food intake | Affects recovery |
| Sleep | Disturbed sleep patterns | Brain function impact |
| Seizures | Frequency or new onset | Critical warning sign |
| Headache | Increasing intensity | Possible pressure rise |
At the same time, daily care at home becomes equally important. Recovery is not only about scans. It is about how the patient feels, eats, sleeps, thinks, and functions each day. A balanced approach combines medical monitoring with supportive care that helps the body recover from treatment stress.
What to Watch for at Home
Caregivers often notice early changes before scans show progression. These changes may include mild confusion, slower speech, unusual fatigue, mood changes, reduced appetite, or subtle weakness. These signs should not be ignored, even if they seem small.
Tracking these changes in a simple daily record can help doctors understand patterns and take timely action. This is especially important because recurrence often develops gradually.
Supporting Recovery After Treatment
After radiation and chemotherapy, patients commonly experience weakness, poor appetite, sleep disturbance, and cognitive decline. Supporting recovery involves improving nutrition, maintaining hydration, and ensuring adequate rest.
The National Center for Complementary and Integrative Health highlights that supportive approaches such as nutrition, mind-body care, and complementary therapies may help improve quality of life when used alongside standard care.[16]
This means focusing on simple but consistent care rather than complex or aggressive interventions.
Maintaining Strength and Stability
Physical and mental strength often decline after treatment. Gentle activity, when possible, can help maintain mobility and reduce complications. Mental stimulation, conversation, and emotional support also play a role in preserving cognitive function.
Caregivers should understand that recovery is slow and varies from patient to patient. Small improvements matter and should be encouraged.
When to Seek Medical Attention
Immediate medical attention is required if the patient develops worsening headaches, repeated vomiting, seizures, sudden confusion, or weakness on one side of the body. These may indicate progression or complications that need urgent evaluation.
Delaying medical care in such situations can lead to rapid deterioration.
Making Informed Decisions About Additional Care
Many families begin to explore supportive or integrative approaches during this phase. The key is to make informed decisions rather than emotional or rushed ones.
Any additional therapy should be discussed with healthcare providers to ensure safety and compatibility with ongoing care. The goal is to support the patient, not to interfere with necessary treatment.
What This Means for You as a Caregiver
You are not just observing the patient. You are an active part of the care process. Your role includes monitoring changes, supporting recovery, and helping make informed decisions.
In simple terms, good care after treatment is a combination of medical follow-up, daily observation, and consistent supportive care. This balanced approach helps improve quality of life and allows early detection if the disease begins to progress again.
Clinical Insight (Real-World Pattern)
What Doctors Commonly Observe After Treatment
In real clinical settings, the course of disease after treatment follows a pattern that many patients and families are not fully prepared for. After surgery, radiation, and chemotherapy, there is often a short period where things appear stable. Scans may look unchanged, and symptoms may seem controlled. This phase can create a sense of reassurance.
However, clinical observations show that this stability is often temporary. Glioma is not a localized disease. It spreads microscopically into surrounding brain tissue, which cannot be fully removed or detected early. Because of this, recurrence is not an unexpected event but a known pattern seen in a large number of patients [9].
How Recurrence Typically Begins in Practice
In many cases, recurrence does not start with a sudden event. It begins gradually at a cellular level. Patients may still feel relatively stable while the disease is already progressing internally.
Over time, subtle changes begin to appear. These may include mild confusion, slower response, occasional headaches, or slight weakness. These symptoms are often overlooked or attributed to treatment side effects.
Clinical experience shows that by the time these symptoms become noticeable and persistent, the disease has usually progressed significantly [13].
The Pattern of Gradual Decline
As recurrence advances, the progression often follows a recognizable pattern. Cognitive function begins to decline. Memory becomes affected. Patients may struggle with speech, coordination, or understanding simple instructions.
Seizures may start or increase in frequency. Headaches become more persistent. Vomiting can occur due to rising intracranial pressure.
In later stages, patients may lose independence. Many become bedridden. Some require feeding support through tubes because swallowing becomes difficult. Communication may reduce significantly, and awareness may fluctuate.
This pattern is not rare. It is commonly observed in advanced cases after recurrence.
Why This Pattern Feels Sudden to Families
For families, this progression often feels sudden and unexpected. One day the patient seems stable, and within weeks or months, there is a noticeable decline.
The reason for this is that the disease progresses silently long before visible changes appear. By the time symptoms become obvious, the underlying progression is already advanced.
This creates the impression that the disease worsened suddenly, even though it had been developing quietly for a long time.
What This Means for Patients and Caregivers
Understanding this real-world pattern helps set realistic expectations. It explains why regular monitoring is important and why even small changes should be taken seriously.
It also highlights the importance of focusing not only on treatment but also on maintaining strength, function, and quality of life.
In simple terms, recurrence is not a sudden failure of treatment. It is a known pattern of disease behavior that unfolds over time, often silently at first and then more visibly as it progresses.
Prognosis and Long-Term Management
Why Prognosis Remains Challenging in High-Grade Glioma
The prognosis after treatment depends on tumor grade, location, how much tumor was removed, response to radiation and chemotherapy, and the patient’s overall neurological condition. In high-grade gliomas, especially glioblastoma, long-term cure remains difficult because the disease usually returns even after aggressive treatment.
Clinical trial data has shown that, despite combined surgery, radiation, and temozolomide chemotherapy, median survival in glioblastoma is still limited, often around 12 to 15 months from diagnosis in many patients [1]. Population-based data also shows that recurrence remains one of the main reasons survival stays poor in this disease group [3].
This does not mean every patient follows the same timeline. Some patients do better than expected, while others decline earlier. But overall, recurrence continues to shape prognosis in most cases.
Why Recurrence Changes the Long-Term Outlook
Once recurrence appears, the long-term outlook usually becomes more difficult. This is because the returning tumor is often more resistant, more diffuse, and harder to treat than the original one. At that stage, treatment options may be fewer, and the goal often shifts from cure to control.
This is a hard reality for families, but it is important to state clearly. In many patients, the disease does not end after first-line treatment. It continues as an ongoing process, and this repeated progression is what eventually leads to severe decline and, in many cases, death [9].
That is why prognosis in glioma is not based only on the first surgery or first scan. It must be viewed as a long-term pattern of disease behavior.
Why Long-Term Management Matters Even When Scans Look Stable
Many families think prognosis depends only on what the latest MRI shows. But long-term management is broader than scan results. A patient may have a stable scan and still be dealing with fatigue, memory loss, weakness, mood changes, or seizure risk. These problems affect daily life and also influence how well the patient can tolerate future treatment.
Long-term management therefore includes not only tumor monitoring but also preserving function, maintaining strength, and reducing factors that worsen decline. This becomes especially important in the months after treatment, when the disease may still be silent but the body is already under stress.
Key Goals in Long-Term Management
The first goal is regular monitoring. This helps detect structural progression as early as possible, even though microscopic changes may begin earlier. The second goal is symptom tracking. Small changes in speech, memory, coordination, mood, or appetite can be early clues that the disease is shifting. The third goal is supportive care. This includes nutrition, sleep, seizure control, emotional support, and physical assistance where needed.
For some patients, long-term management also includes integrative supportive care aimed at maintaining recovery after radiation and chemotherapy, supporting resilience, and improving quality of life.
Why Quality of Life Becomes a Central Part of Prognosis
In glioma care, prognosis is not only about how long a patient lives. It is also about how the patient lives during that time. Some patients may survive longer but with severe disability, while others may maintain better function for a shorter period. Because of this, long-term management must pay close attention to cognition, independence, communication, sleep, emotional state, and dignity of care.
This is especially important for caregivers, because they often become the first people to notice functional decline before it becomes obvious in clinical settings.
How Families Should View the Future
Families should be prepared for two realities at the same time. First, glioma often behaves aggressively and recurrence is common. Second, careful long-term management can still make a meaningful difference in comfort, function, and decision-making.
This means the aim is not only to respond when the disease worsens, but to stay alert during the quieter phases as well. A realistic and informed approach gives patients and families a better chance to act early, prepare practically, and make balanced treatment decisions.
What This Means in Simple Terms
The long-term outlook in glioma remains serious because recurrence is common and often drives the later course of the disease. But management does not stop when treatment ends. Ongoing care, close observation, supportive measures, and timely decisions remain essential throughout the journey.
In simple words, prognosis is shaped not only by the tumor itself, but by how early changes are recognized, how well the patient is supported, and how carefully the disease is managed over time.
FAQs
Does glioma always come back after treatment?
In many cases, especially high-grade gliomas like glioblastoma, the tumor returns because microscopic cells remain in the brain even after treatment.
How long does it take for glioma to recur?
Recurrence commonly happens within 6 to 18 months after treatment, but this can vary depending on the patient and tumor type.
What are the first signs of recurrence?
Early signs may include mild confusion, headaches, memory problems, speech difficulty, or seizures. These are often subtle at first.
Can MRI detect recurrence early?
MRI is the standard tool, but it usually detects changes only after the tumor has grown enough to be visible.
Why does glioma come back in the same place?
Tumor cells often remain in nearby brain tissue even after surgery, and these cells can grow again over time.
Can glioma be completely cured?
Complete cure is difficult, especially in aggressive types, because the tumor spreads into surrounding brain tissue.
What happens to patients after recurrence?
Patients may develop worsening neurological symptoms such as memory loss, seizures, weakness, and reduced independence. In advanced stages, many patients eventually die due to disease progression.
Do all patients decline quickly after recurrence?
No, progression varies. Some patients decline rapidly, while others may experience a slower course.
Is there anything that can be done after treatment ends?
Yes, regular monitoring, supportive care, and a structured recovery plan can help manage symptoms and improve quality of life.
When should families become concerned after treatment?
Seek medical attention if there are new or worsening symptoms such as persistent headaches, repeated vomiting, seizures, confusion, or weakness.
Why does recurrence feel sudden to families?
Because the disease often progresses silently before symptoms become noticeable.
Can supportive or integrative care help patients?
Supportive care may improve strength, reduce symptoms, and help patients maintain better quality of life when used alongside medical treatment.
Reference
[1] Stupp, R., Hegi, M. E., Mason, W. P., et al. (2005). Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma. New England Journal of Medicine, 352(10), 987–996.
https://www.nejm.org/doi/full/10.1056/NEJMoa043330
This landmark trial established the standard treatment for glioblastoma. It shows that even with the best available therapy, recurrence remains common, supporting the concept that treatment controls but does not eliminate tumor biology.
[2] Wen, P. Y., & Kesari, S. (2008). Malignant gliomas in adults. New England Journal of Medicine, 359(5), 492–507.
https://www.nejm.org/doi/full/10.1056/NEJMra0708126
A comprehensive clinical review explaining why gliomas are highly infiltrative and difficult to cure. It supports sections discussing tumor biology, recurrence patterns, and treatment limitations.
[3] Ostrom, Q. T., Patil, N., Cioffi, G., et al. (2020). CBTRUS statistical report: Primary brain and other central nervous system tumors. Neuro-Oncology, 22(Suppl 2), iv1–iv96.
https://academic.oup.com/neuro-oncology/article/22/Supplement_2/iv1/5874365
Provides epidemiological data showing high recurrence rates and poor prognosis, reinforcing the need for long-term management strategies.
[4] Louis, D. N., Perry, A., Reifenberger, G., et al. (2021). The 2021 WHO classification of tumors of the central nervous system. Acta Neuropathologica, 142(2), 1–36.
https://link.springer.com/article/10.1007/s00401-021-02365-1
Defines gliomas as biologically aggressive and infiltrative tumors. Supports sections explaining why recurrence is expected even after treatment.
[5] National Comprehensive Cancer Network (NCCN). (2024). Central Nervous System Cancers Guidelines.
https://www.nccn.org/guidelines/guidelines-detail?category=1&id=1425
Provides clinical guidelines for glioma treatment and follow-up, confirming that recurrence monitoring is essential and cure is rarely achieved in high-grade gliomas.
[6] American Society of Clinical Oncology (ASCO). (2022). Glioblastoma treatment and management guidelines.
https://www.asco.org
ASCO acknowledges recurrence as a major challenge and supports integrative symptom management approaches, reinforcing your integrative positioning.
[7] National Institute for Health and Care Excellence (NICE). (2021). Brain tumours (primary) and brain metastases in adults.
https://www.nice.org.uk/guidance/ng99
UK guideline highlighting limitations of treatment and need for long-term monitoring, supporting the “post-treatment gap” and recurrence sections.
[8] World Health Organization (WHO). (2021). Classification of CNS tumors.
https://www.who.int
Confirms gliomas as high-risk tumors with aggressive recurrence patterns, strengthening global authority.
[9] National Cancer Institute (NCI). (2023). Adult central nervous system tumors treatment (PDQ).
https://www.cancer.gov/types/brain/hp/adult-brain-treatment-pdq
Explains recurrence biology, treatment limitations, and monitoring approaches, supporting multiple sections including timeline and symptoms.
[10] Chen, J., Li, Y., Yu, T. S., et al. (2012). A restricted cell population propagates glioblastoma growth. Nature, 488(7412), 522–526.
https://www.nature.com/articles/nature11287
Demonstrates the role of cancer stem cells in glioma recurrence, directly supporting the section on stem-cell-driven regrowth.
[11] Hambardzumyan, D., Bergers, G. (2015). Glioblastoma: Defining tumor niches. Cancer Cell, 28(6), 707–709.
https://www.cell.com/cancer-cell/fulltext/S1535-6108(15)00463-6
Explains tumor microenvironment, hypoxia, and immune evasion, supporting regrowth and recurrence biology sections.
[12] Jain, R. K., di Tomaso, E., Duda, D. G., et al. (2007). Angiogenesis in brain tumours. Nature Reviews Neuroscience, 8(8), 610–622.
https://www.nature.com/articles/nrn2175
Shows how tumors develop new blood vessels to sustain regrowth, supporting microenvironment and angiogenesis sections.
[13] Omuro, A., DeAngelis, L. M. (2013). Glioblastoma and other malignant gliomas. JAMA, 310(17), 1842–1850.
https://jamanetwork.com/journals/jama/fullarticle/1752246
Explains clinical progression, recurrence patterns, and patient symptoms, supporting practical and symptom-based sections.
[14] Pope, W. B., Sayre, J., Perlina, A., et al. (2005). MR imaging correlates of survival in glioblastoma. AJNR American Journal of Neuroradiology.
https://www.ajnr.org/content/26/10/2466
Shows limitations of MRI in detecting early recurrence, supporting the “monitoring failure” section.
[15] Galldiks, N., Langen, K. J., Pope, W. B. (2015). From the clinician’s point of view: PET imaging in glioma. Neuro-Oncology.
https://academic.oup.com/neuro-oncology/article/17/11/1434/2402920
Explains how PET imaging detects metabolic activity earlier than MRI, supporting early detection discussion.
[16] NCCIH (National Center for Complementary and Integrative Health). (2023). Cancer and complementary health approaches.
https://www.nccih.nih.gov/health/cancer-and-complementary-health-approaches
Supports integrative care approaches for improving quality of life and symptom management alongside standard oncology.
[17] Block, K. I., et al. (2015). Integrative cancer therapies. CA: A Cancer Journal for Clinicians, 65(5), 327–340.
https://acsjournals.onlinelibrary.wiley.com/doi/full/10.3322/caac.21286
Provides strong evidence for integrative oncology, supporting combined modern and supportive approaches.
[18] Charaka Samhita, Chikitsa Sthana 30 (Arbuda Chikitsa).
https://www.easyayurveda.com/2014/08/07/arbuda-tumor-ayurveda/
Describes Arbuda (tumor pathology) and systemic imbalance, supporting Ayurvedic interpretation of glioma recurrence.
[19] Sushruta Samhita, Nidana Sthana 11 (Granthi and Arbuda Nidana).
https://www.easyayurveda.com/2014/08/08/granthi-arbuda/
Explains tumor formation, growth, and recurrence tendencies in Ayurvedic terms.
[20] Bhavaprakasha Nighantu (Guduchi, Ashwagandha, Brahmi references).
https://www.easyayurveda.com
Describes key Rasayana herbs used for immunity, neuroprotection, and tissue regeneration.
[21] Withania somnifera (Ashwagandha) anticancer study.
https://pubmed.ncbi.nlm.nih.gov/23439798/
Shows anti-tumor and neuroprotective properties, supporting Ayurvedic herb section.
[22] Tinospora cordifolia (Guduchi) immunomodulatory effects.
https://pubmed.ncbi.nlm.nih.gov/15717062/
Supports immune modulation and inflammation control.
[23] Bacopa monnieri (Brahmi) neuroprotective effects.
https://pubmed.ncbi.nlm.nih.gov/18611150/
Supports cognitive function and neural protection.
Every reference listed here has been carefully selected for accuracy, clinical relevance, and traceability. Ayurvedic concepts are cited directly from classical texts such as Charaka Samhita and Sushruta Samhita with contextual interpretation, while modern scientific studies are linked with accessible sources. This combined validation ensures reliability for both patients and medical professionals.